gut health
Serotonin and Gut Health: The 90% Connection
Discover why 90% of serotonin is made in your gut, how gut bacteria control production, and evidence-based strategies to optimize serotonin for mood and digestion.
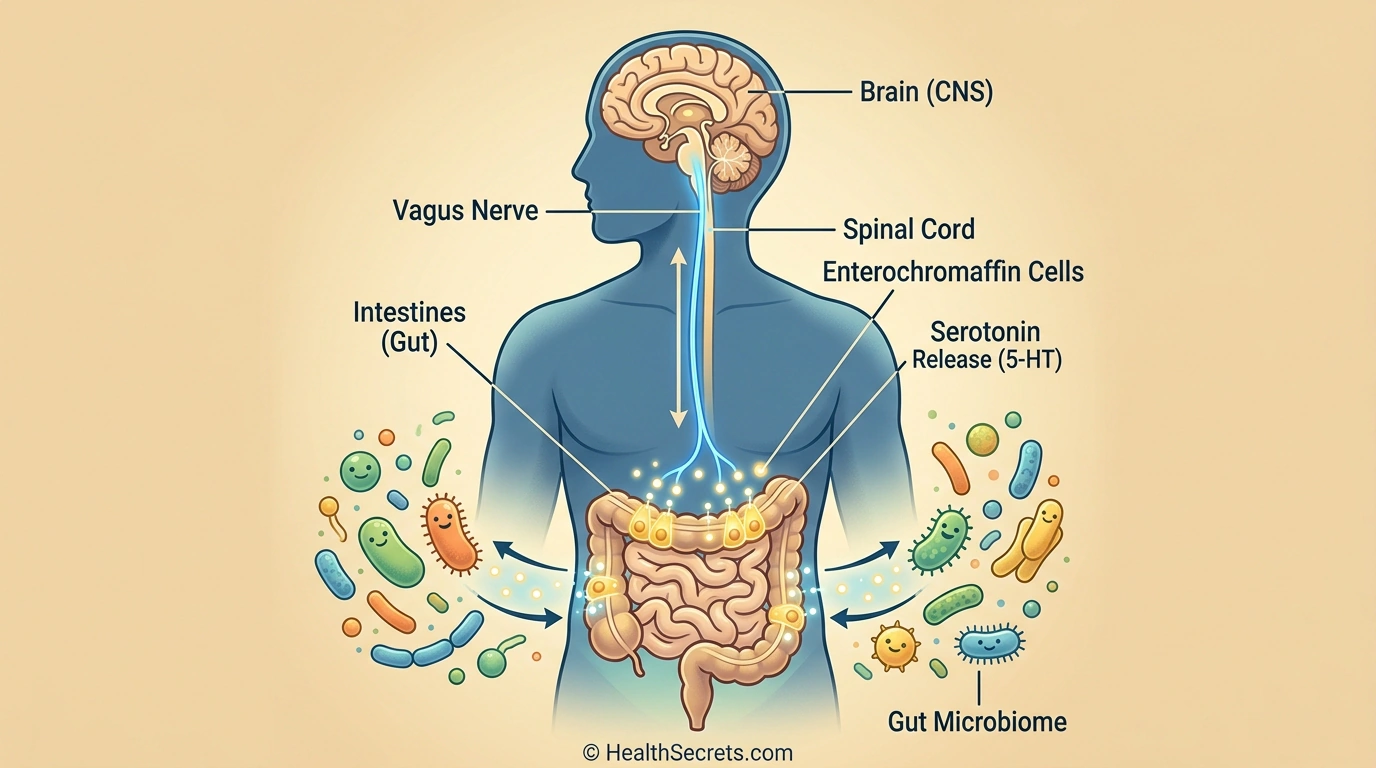
You probably think of serotonin as a brain chemical — the "happy molecule" behind your mood, sleep, and emotional balance. But here's a fact that surprises even many healthcare professionals: up to 95% of your body's serotonin is actually produced in your gut, not your brain. This revelation has transformed how researchers understand the connection between digestive health and mental wellbeing.
Your gut is home to specialized cells called enterochromaffin cells that manufacture this critical neurotransmitter around the clock. Even more fascinating, your gut bacteria play a direct role in regulating how much serotonin gets produced. When your microbiome is out of balance, serotonin production can suffer — and so can your mood, digestion, and overall health.
Understanding the serotonin-gut connection can help you make informed decisions about your health. In this guide, we'll explore how serotonin works in your gut, how your microbiome influences its production, and evidence-based strategies to support healthy serotonin levels. For a broader look at how your gut communicates with your brain, see our gut-brain axis explained guide. You may also want to explore our complete gut health guide for foundational strategies.
- Approximately 90–95% of the body's serotonin is produced by enterochromaffin cells in the gut, not the brain, making digestive health critical for serotonin balance.
- Gut bacteria directly influence serotonin production by metabolizing tryptophan, producing short-chain fatty acids, and stimulating enterochromaffin cells.
- Gut-produced serotonin cannot cross the blood-brain barrier, but it influences brain function indirectly through the vagus nerve, immune signaling, and metabolites.
- The amino acid tryptophan is the essential precursor to serotonin — dietary sources include turkey, eggs, salmon, pumpkin seeds, and tofu.
- SSRIs (common antidepressants) affect gut serotonin too, which explains common gastrointestinal side effects like nausea and changes in bowel habits.
- Chronic stress diverts tryptophan away from serotonin production and into the kynurenine pathway, reducing available serotonin.
- Psychobiotics — specific probiotic strains like Lactobacillus helveticus and Bifidobacterium longum — show promise for supporting mood through the gut-brain axis.
- Never combine serotonin-boosting supplements (5-HTP, L-tryptophan) with antidepressants without medical supervision due to the risk of serotonin syndrome.
What Is Serotonin and Why Does Your Gut Produce 90% of It?
Serotonin (5-hydroxytryptamine or 5-HT) is a chemical messenger that regulates mood, sleep, appetite, and digestion. While it is widely known as the "happy neurotransmitter," roughly 90–95% of the body's serotonin is synthesized by enterochromaffin cells lining the gastrointestinal tract, with only 5–10% produced in the brain.
How Does Serotonin Function Differently in the Gut Versus the Brain?
In the brain, serotonin regulates mood, emotions, the sleep-wake cycle, appetite, and cognitive function. It is the primary target of SSRI antidepressants. However, in the gut, serotonin serves entirely different purposes — it regulates intestinal motility (peristalsis), controls secretion, modulates pain perception, influences nutrient absorption, and coordinates communication between the gut and brain through the enteric nervous system.
Enterochromaffin (EC) cells are specialized enteroendocrine cells distributed throughout the GI tract, with the highest concentration in the colon. These cells function as luminal sensors, responding to nutrients, mechanical stimulation, and signals from gut bacteria to release serotonin into surrounding tissue and the bloodstream.
Does Gut Serotonin Affect Your Brain Directly?
Gut-produced serotonin cannot cross the blood-brain barrier, meaning the brain must produce its own supply. However, gut serotonin profoundly influences brain function through indirect pathways. It activates vagal afferent nerve fibers that transmit signals to the brainstem, modulates immune cells that produce brain-affecting cytokines, and influences circulating tryptophan availability. Research from Stanford Medicine confirms this bidirectional gut-brain communication plays a significant role in conditions from anxiety to neurodegenerative diseases.
How Does Your Gut Microbiome Control Serotonin Production?
Gut bacteria regulate serotonin synthesis through multiple mechanisms including tryptophan metabolism, short-chain fatty acid production, and direct stimulation of enterochromaffin cells. A 2026 study in Cell Reports identified specific human gut bacteria — Limosilactobacillus mucosae and Ligilactobacillus ruminis — that can directly synthesize bioactive serotonin.
How Does Tryptophan Become Serotonin?
Serotonin production follows a two-step enzymatic pathway. First, the essential amino acid tryptophan is converted to 5-hydroxytryptophan (5-HTP) by the enzyme tryptophan hydroxylase (TPH1 in EC cells, TPH2 in the nervous system). Then, 5-HTP is converted to serotonin by aromatic L-amino acid decarboxylase. This process requires cofactors including vitamin B6, folate, iron, and magnesium. Gut bacteria influence this pathway by metabolizing dietary tryptophan, producing metabolites that stimulate or inhibit TPH1, and even producing tryptophan themselves. Species including Lactococcus, Lactobacillus, Streptococcus, and Escherichia coli have been shown to express tryptophan synthetase.
What Role Do Short-Chain Fatty Acids Play?
When gut bacteria ferment dietary fiber, they produce short-chain fatty acids (SCFAs) — butyrate, acetate, and propionate. Research published in The FASEB Journal demonstrated that these SCFAs directly stimulate enterochromaffin cells to increase serotonin production. This is one reason why a fiber-rich diet supports both gut health and mood. SCFAs also modulate TPH1 expression and influence the serotonin transporter (SERT), which regulates how serotonin is cleared from the gut.
How Does the Kynurenine Pathway Compete With Serotonin?
Tryptophan doesn't always become serotonin. Under conditions of chronic stress and inflammation, the enzyme indoleamine 2,3-dioxygenase (IDO) diverts tryptophan into the kynurenine pathway instead. This produces kynurenine metabolites rather than serotonin, effectively reducing serotonin availability. This mechanism may partly explain why chronic stress and inflammation are associated with depression — they literally redirect the raw materials away from serotonin production.
What Are the Key Benefits of Optimizing Gut-Based Serotonin?
Optimizing gut serotonin production through microbiome support offers benefits for digestion, mood, immune function, and overall wellbeing. Because serotonin influences so many systems, improving its gut-based production can have wide-ranging positive effects.
Can Improving Gut Health Reduce Anxiety and Depression?
Research increasingly supports the connection between gut health and mental wellbeing. A 2026 study in npj Mental Health Research found that probiotics can reduce negative mood over time, while meta-analyses consistently show beneficial effects of specific probiotic strains on stress, anxiety, and depressive symptoms. The concept of "psychobiotics" — probiotics that influence mental health through the gut-brain axis — has gained significant scientific traction, with strains like Lactobacillus helveticus R0052 and Bifidobacterium longum R0175 showing particular promise.
Does Gut Serotonin Improve Digestive Function?
Serotonin is the primary regulator of gut motility. It coordinates the muscle contractions (peristalsis) that move food through your digestive tract, signals feelings of fullness and satiety, and modulates secretion. Dysregulated gut serotonin is implicated in irritable bowel syndrome (IBS), with 50–90% of IBS patients experiencing co-occurring anxiety or depression. Supporting healthy serotonin production through gut-healing foods and probiotics may improve both digestive comfort and emotional wellbeing.
How Does Serotonin Support Immune Function?
Gut serotonin plays a regulatory role in intestinal immune responses. It modulates inflammation, influences immune cell activity, and helps maintain gut barrier integrity. A 2023 study in Nature Communications found that serotonin produced by mast cells contributes to pathogen clearance and immune homeostasis. When the gut barrier is compromised ("leaky gut"), endotoxins can enter the bloodstream and trigger systemic inflammation that disrupts brain serotonin production — learn more in our healing leaky gut guide.
Can Serotonin Optimization Improve Sleep Quality?
Serotonin serves as the precursor to melatonin, the hormone that regulates your sleep-wake cycle. In the pineal gland, serotonin is enzymatically converted to melatonin. By supporting healthy serotonin production during the day through adequate tryptophan intake, sunlight exposure, and gut health, you create the conditions for healthy melatonin production at night.
Are There Risks to Boosting Serotonin Levels?
While supporting healthy serotonin production through diet and lifestyle is generally safe, supplementing with serotonin precursors carries real risks, particularly when combined with medications. The most serious concern is serotonin syndrome, a potentially life-threatening condition caused by excessive serotonin activity.
What Is Serotonin Syndrome and How Do You Avoid It?
Serotonin syndrome occurs when serotonin levels become dangerously high, typically from combining multiple serotonin-boosting substances. Symptoms include agitation, rapid heart rate, high blood pressure, dilated pupils, muscle rigidity, tremors, sweating, fever, and in severe cases, seizures. The most common cause is combining SSRIs with supplements like 5-HTP or L-tryptophan.
Never combine these supplements with antidepressants without explicit medical supervision.
Can Too Much Gut Serotonin Cause Problems?
Excess serotonin in the gut can accelerate motility, causing diarrhea, nausea, and cramping. This is why SSRIs — which increase serotonin availability in both the brain and gut — commonly cause gastrointestinal side effects, especially when starting treatment. Emerging research also shows that SSRIs may alter gut microbiome composition, potentially affecting their therapeutic efficacy.
Who Should Be Cautious With Serotonin Supplements?
People taking SSRIs, SNRIs, MAOIs, or tricyclic antidepressants should avoid 5-HTP and L-tryptophan supplements unless directed by their physician. Those with carcinoid syndrome (serotonin-producing tumors) must also avoid these supplements. Pregnant or breastfeeding individuals should consult a healthcare provider before using any serotonin-targeting supplements.
How Do You Optimize Serotonin Production Through Your Gut?
Optimizing gut-based serotonin involves a multi-pronged approach: nourishing your microbiome with diverse fiber and fermented foods, ensuring adequate tryptophan and cofactor intake, managing stress, and considering targeted supplementation when appropriate. These strategies work synergistically.
What Supplements Support Healthy Serotonin Levels?
- L-Tryptophan (500–2,000 mg daily on an empty stomach) is the direct dietary precursor to serotonin. 5-HTP (50–300 mg daily) is one step closer to serotonin and crosses the blood-brain barrier more easily.
- Psychobiotic probiotics containing L. helveticus and B. longum support gut-brain communication.
- Omega-3 fatty acids (1–2 g EPA+DHA daily) support brain serotonin receptor function.
- Vitamin D (2,000–5,000 IU daily) activates tryptophan hydroxylase.
- Magnesium (300–400 mg glycinate daily) is a required cofactor for serotonin synthesis.
- B vitamins (especially B6, folate, B12) are essential for the enzymatic conversion of tryptophan to serotonin.
What Lifestyle Habits Boost Serotonin Naturally?
Sunlight exposure (10–30 minutes daily) directly stimulates brain serotonin production and supports vitamin D synthesis. Aerobic exercise (30 minutes most days) increases tryptophan availability to the brain. Stress management through meditation, yoga, or deep breathing prevents tryptophan diversion to the kynurenine pathway. Quality sleep (7–9 hours) supports the serotonin-melatonin cycle. Social connection and positive interactions have also been shown to influence serotonergic activity. For more on supporting the vagus nerve pathway, see our vagus nerve stimulation guide.
What Foods and Habits Best Support Gut Serotonin Production?
The most effective dietary strategy combines tryptophan-rich protein sources with complex carbohydrates (which help tryptophan cross the blood-brain barrier), prebiotic fiber to fuel serotonin-promoting bacteria, and fermented foods to diversify the microbiome. Supporting cofactor nutrients completes the picture.
Which Foods Are Highest in Tryptophan?
| Food | Tryptophan (mg) | Serving Size | Additional Benefits |
|---|---|---|---|
| Turkey breast | 250–350 | 3 oz | Complete protein, B vitamins |
| Salmon | 200–250 | 3 oz | Omega-3s, vitamin D |
| Pumpkin seeds | 110 | 1 oz | Magnesium, zinc |
| Tofu | 100–150 | 3 oz | Plant protein, isoflavones |
| Eggs | 75 | 1 large | Choline, B12 |
| Oats | 60 | 1 cup | Prebiotic fiber, B vitamins |
The carbohydrate connection: Eating complex carbs alongside tryptophan-rich foods triggers insulin release, which clears competing amino acids from the bloodstream and allows more tryptophan to reach the brain. Optimal pairings include turkey with sweet potato, salmon with brown rice, or oatmeal with pumpkin seeds.
Which Gut-Supporting Foods Promote Serotonin?
- Prebiotic foods fuel the bacteria that stimulate serotonin production: garlic, onions, bananas, oats, apples, and asparagus.
- Fermented foods diversify your microbiome: yogurt, kefir, sauerkraut, kimchi, and kombucha.
- Polyphenol-rich foods support beneficial bacteria — learn more in our polyphenols for gut health guide.
- Anti-inflammatory foods including fatty fish, olive oil, turmeric, and berries reduce the inflammation that diverts tryptophan to the kynurenine pathway. For more on how postbiotics and metabolites influence serotonin signaling, see our dedicated guide.
What Foods Should You Limit?
Highly processed foods disrupt gut bacteria composition and increase inflammation. Excess sugar feeds harmful bacteria at the expense of serotonin-promoting species. Artificial sweeteners may alter the microbiome. Excessive alcohol irritates the gut lining and disrupts serotonin production. Trans fats increase systemic inflammation. For broader dietary strategies, see our anti-inflammatory lifestyle guide.
What Should You Do First to Support Healthy Serotonin Levels?
Start with dietary foundations before adding supplements. A phased approach ensures you build sustainable habits that support long-term serotonin production. Most people notice improvements in mood, digestion, and sleep within 4–8 weeks of consistent effort.
Phase 1 — Foundation (Weeks 1–2):
- [ ] Include a tryptophan-rich protein source at every meal paired with complex carbohydrates
- [ ] Add one serving of fermented food daily (yogurt, kefir, sauerkraut)
- [ ] Get 10–30 minutes of morning sunlight exposure
- [ ] Begin a daily 10-minute stress management practice (meditation, deep breathing)
Phase 2 — Optimization (Weeks 3–4):
- [ ] Increase dietary fiber to 30+ grams daily from diverse plant sources
- [ ] Add prebiotic-rich foods (garlic, onions, bananas, oats)
- [ ] Start 30 minutes of aerobic exercise most days
- [ ] Consider a psychobiotic probiotic supplement
Phase 3 — Advanced Support (Weeks 5–8):
- [ ] Add targeted supplements if needed (omega-3s, vitamin D, magnesium)
- [ ] Track mood, sleep, and digestive patterns to identify improvements
- [ ] Consult a healthcare provider about 5-HTP or L-tryptophan if mood support is needed
- [ ] Aim for 30+ different plant foods per week to maximize microbiome diversity
References
- Yano, J.M., et al. (2015). Indigenous bacteria from the gut microbiota regulate host serotonin biosynthesis. Cell, 161(2), 264–276. Source
- Reigstad, C.S., et al. (2015). Gut microbes promote colonic serotonin production through an effect of short-chain fatty acids on enterochromaffin cells. The FASEB Journal, 29(4), 1395–1403. Source
- Martin, C.R., et al. (2018). The brain-gut-microbiome axis. Cellular and Molecular Gastroenterology and Hepatology, 6(2), 133–148. Source
- O'Mahony, S.M., et al. (2015). Serotonin, tryptophan metabolism and the brain-gut-microbiome axis. Behavioural Brain Research, 277, 32–48. Source
- Agus, A., Planchais, J., & Sokol, H. (2018). Gut microbiota regulation of tryptophan metabolism in health and disease. Cell Host & Microbe, 23(6), 716–724. Source
- Margolis, K.G., et al. (2021). The gut-brain axis: from serotonin to new therapies. Trends in Pharmacological Sciences, 42(1), 45–55. Source
- Lv, J., & Liu, F. (2021). The mechanism of secretion and metabolism of gut-derived 5-hydroxytryptamine. International Journal of Molecular Sciences, 22(15), 7931. Source
- Strandwitz, P. (2018). Neurotransmitter modulation by the gut microbiota. Brain Research, 1693, 128–133. Source
- Carabotti, M., et al. (2015). The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems. Annals of Gastroenterology, 28(2), 203–209. Source
- Wallace, C.J.K., & Milev, R. (2017). The effects of probiotics on depressive symptoms in humans: a systematic review. Annals of General Psychiatry, 16, 14. Source
- Liu, R.T., et al. (2019). Prebiotics and probiotics for depression and anxiety: a systematic review and meta-analysis. BMJ, 365, l1906. Source
- Boehme, M., et al. (2025). Identification of human gut bacteria that produce bioactive serotonin and promote colonic innervation. Cell Reports, 44(3).)01205-7 Source
Frequently asked questions
Is it true that 90% of serotonin is made in the gut?
Yes, research consistently shows that 90–95% of the body's serotonin is produced by enterochromaffin cells in the gastrointestinal tract. These specialized cells synthesize serotonin from the amino acid tryptophan using the enzyme tryptophan hydroxylase 1 (TPH1). The remaining 5–10% is produced in the brain by neurons using TPH2.
If most serotonin is in the gut, why do antidepressants target the brain?
Gut and brain serotonin are separate pools because gut-produced serotonin cannot cross the blood-brain barrier. SSRIs target serotonin reuptake in brain synapses specifically. However, because SERT (the serotonin transporter) is also expressed in the gut, SSRIs affect gut serotonin too, which explains common GI side effects like nausea, diarrhea, and appetite changes.
Can probiotics really improve mood and anxiety?
Growing evidence supports specific probiotic strains — called psychobiotics — for mood benefits. Meta-analyses show beneficial effects on stress, anxiety, and depressive symptoms, particularly with Lactobacillus helveticus R0052 and Bifidobacterium longum R0175. However, results vary by strain and individual, and probiotics should complement, not replace, professional mental health treatment.
What foods increase serotonin levels the fastest?
Combining tryptophan-rich foods (turkey, salmon, eggs, pumpkin seeds) with complex carbohydrates is the most effective dietary strategy. Carbohydrates trigger insulin release, which clears competing amino acids and allows more tryptophan to reach the brain. A meal like salmon with brown rice or oatmeal with pumpkin seeds supports serotonin production within hours.
Is 5-HTP safe to take daily for mood support?
5-HTP (50–300 mg daily) is generally safe for short-to-medium-term use in people not taking serotonergic medications. However, it should never be combined with SSRIs, SNRIs, MAOIs, or other antidepressants due to the risk of serotonin syndrome. Long-term use should be discussed with a healthcare provider, as it may deplete other neurotransmitter precursors.
How does stress affect gut serotonin production?
Chronic stress activates the enzyme indoleamine 2,3-dioxygenase (IDO), which diverts tryptophan into the kynurenine pathway instead of the serotonin pathway. This reduces available tryptophan for serotonin synthesis. Stress also increases gut inflammation, disrupts the microbiome, and can compromise gut barrier integrity — all of which further impair serotonin production.
Can healing your gut help with depression?
Improving gut health may support mood as part of a comprehensive approach, but it should not replace professional treatment for clinical depression. Research shows that gut inflammation, dysbiosis, and leaky gut are associated with depressive symptoms. Addressing these issues through diet, probiotics, and lifestyle changes may improve mood, particularly when combined with conventional treatment.
What are the symptoms of serotonin syndrome?
Serotonin syndrome symptoms include agitation, confusion, rapid heart rate, high blood pressure, dilated pupils, muscle rigidity, tremors, sweating, fever, and diarrhea. Severe cases can involve seizures and can be life-threatening. It typically occurs from combining multiple serotonin-boosting medications or supplements. Seek immediate medical attention if you suspect serotonin syndrome.
Do SSRIs damage your gut microbiome?
Emerging research suggests SSRIs may alter gut microbiome composition. Some SSRIs, particularly sertraline, fluoxetine, and paroxetine, exhibit antimicrobial properties that can affect certain bacterial populations. However, the clinical significance is still being studied, and SSRIs remain important medications for depression. Discuss any gut-related concerns with your prescribing physician.
How long does it take to notice improvements in mood from gut health changes?
Most people notice subtle improvements in mood, energy, and digestion within 2–4 weeks of consistent dietary and lifestyle changes. Probiotic supplementation typically requires 4–8 weeks for noticeable mood effects. Full microbiome remodeling through dietary changes can take 3–6 months. Consistency is more important than intensity.