gut health
Complete Guide to Gut Health: Transform Your Microbiome in 30 Days
Learn how to transform your gut health in 30 days with this evidence-based guide. Covers microbiome science, probiotics, prebiotics, diet, and a step-by-step protocol.
Something felt off for months—bloating after every meal, brain fog that wouldn't lift, and a general tiredness that sleep couldn't fix. Sound familiar? For millions of people, these vague, frustrating symptoms trace back to one place: the gut. And here's the thing most doctors won't tell you during a 15-minute appointment—your gut health influences practically everything, from your mood and immunity to your metabolism and skin.
The human gut microbiome is a thriving ecosystem of roughly 100 trillion microorganisms spanning over 1,000 species, collectively weighing 2–5 pounds. Recent research confirms that gut microbiota influences brain physiology through neural, immune, endocrine, and metabolic signaling pathways along the gut-brain axis [0]. Meanwhile, gut microbiota dysbiosis—characterized by loss of health-promoting bacteria and proliferation of pathogenic species—has been linked to neuroinflammation and multiple neurological disorders [1] [2].
This guide is your comprehensive roadmap to understanding and transforming your gut health. We'll walk through the science of the microbiome, the gut-brain connection, how intestinal permeability ("leaky gut") develops, which foods heal versus harm, and a practical 30-day protocol you can start this week. Whether you're dealing with digestive issues, autoimmune concerns, or just want to optimize your overall well-being, the evidence points to one place: start with your gut.
- Your gut microbiome contains 100 trillion microorganisms that influence digestion, immunity, mental health, metabolism, and skin health—roughly 70% of your immune system resides in the gut.
- The gut-brain axis is a bidirectional communication highway; your gut produces approximately 90% of serotonin and 50% of dopamine, directly shaping mood and cognitive function.
- Intestinal permeability ("leaky gut") occurs when tight junctions weaken, allowing toxins and undigested food particles into the bloodstream—triggering systemic inflammation [4].
- Dysbiosis—an imbalance favoring harmful bacteria over beneficial ones—is linked to IBS, autoimmune conditions, obesity, depression, and skin disorders [1].
- Multi-strain probiotics containing Lactobacillus and Bifidobacterium strains enhance gut barrier function and lower systemic inflammation [8].
- Prebiotic fibers—found in garlic, onions, Jerusalem artichokes, and oats—feed beneficial bacteria and boost short-chain fatty acid production [13].
- Eating 30+ different plant foods per week is one of the most impactful steps for increasing microbiome diversity and improving health outcomes.
- The 30-day gut health protocol follows four phases: Remove (irritants), Repair (gut lining), Reinoculate (beneficial bacteria), and Rebalance (prebiotic diversity).
- Short-chain fatty acids like butyrate are the primary fuel for colon cells and play a critical role in reducing inflammation and strengthening the gut barrier [13].
- Lifestyle factors—sleep quality, stress management, regular exercise, and minimizing unnecessary antibiotics—are just as important as diet for long-term gut health.
What Is Gut Health and Why Does It Matter for Your Entire Body?
Gut health refers to the balance and function of the microorganisms living in your gastrointestinal tract—collectively known as the gut microbiome. When this ecosystem is balanced, digestion runs smoothly, your immune system stays calibrated, and your brain receives the chemical signals it needs to regulate mood and cognition.
The numbers alone are staggering. Your gut houses approximately 100 trillion microorganisms—bacteria, fungi, viruses, and archaea—spanning over 1,000 distinct species. That's roughly a 1:1 ratio with your human cells. About 70% of your entire immune system (the gut-associated lymphoid tissue, or GALT) resides in and around the intestinal walls. Your gut also manufactures roughly 90% of your body's serotonin and about 50% of its dopamine, neurotransmitters that govern mood, motivation, and sleep.
Every person's microbiome is as unique as a fingerprint. Factors like birth method (vaginal vs. cesarean), breastfeeding, childhood diet, antibiotic exposure, geography, and even pet ownership shape the composition you carry into adulthood. And that composition matters—research increasingly links microbiome diversity to outcomes across virtually every organ system:
- Digestive function — nutrient absorption, motility, enzyme production
- Immune regulation — pathogen defense, allergy response, autoimmune risk
- Mental health — anxiety, depression, cognitive clarity via the gut-brain axis
- Metabolic health — weight management, insulin sensitivity, cholesterol
- Skin clarity — eczema, acne, rosacea through the gut-skin axis
- Hormonal balance — estrogen metabolism (estrobolome), thyroid function
A 2026 landmark study in Nature analyzing over 34,000 participants confirmed that specific gut microbiome species are significantly associated with dietary patterns and cardiometabolic health markers, reinforcing the microbiome's central role in disease prevention.
Put simply: your gut isn't just where food gets digested. It's a command center influencing nearly every aspect of how you feel, think, and function.
How Does the Gut-Brain Axis Actually Work?
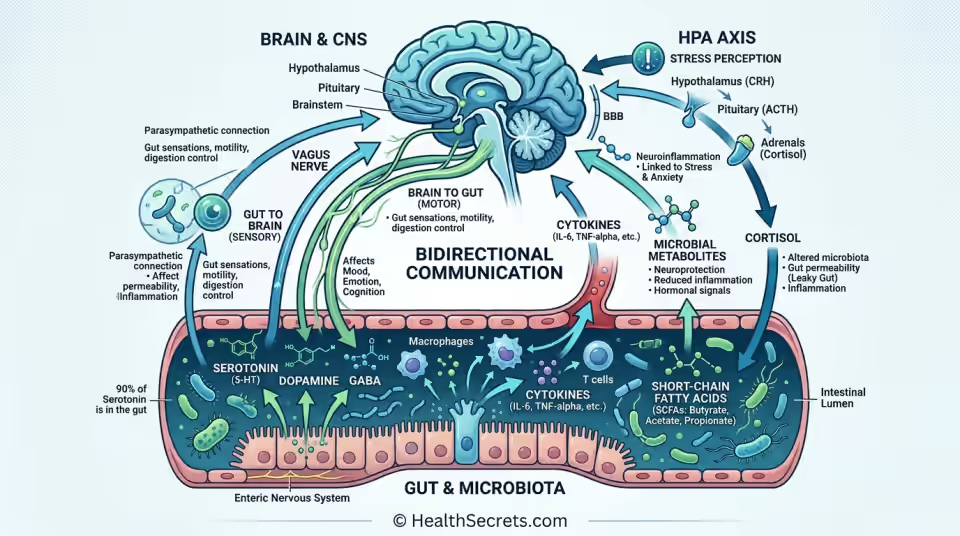
The gut-brain axis is a bidirectional communication network connecting your central nervous system to your enteric nervous system (often called your "second brain") through neural, immune, endocrine, and metabolic pathways. When this connection functions well, your gut and brain work in sync; when it's disrupted, both physical and mental health suffer.
Research published in 2026 describes the gut-brain axis as far more complex than previously understood, with emerging evidence highlighting bioelectrical signaling—ion flows and voltage gradients—as an additional communication layer between gut bacteria and neural cells [0]. Gut microbiota dysbiosis may drive neuroinflammation across multiple neurological disorders [2], while a balanced microbiome is essential for healthy brain function—perturbations contribute to cognitive deficits and mood disturbances [3].
What Are the Main Communication Pathways Between Gut and Brain?
Five primary channels carry information back and forth:
- Vagus nerve — The longest cranial nerve physically connects the brainstem to the gut. It transmits signals in both directions, and stimulating it (through deep breathing, cold exposure, or certain probiotics) can reduce inflammation and improve mood.
- Neurotransmitter production — Gut bacteria synthesize serotonin, GABA, dopamine, and norepinephrine. These chemicals cross into systemic circulation and influence everything from sleep cycles to pain perception.
- Immune signaling — Cytokines (inflammatory messengers) produced in the gut can reach the brain via the bloodstream, influencing neuroinflammation. This is one mechanism linking gut inflammation to depression.
- Microbial metabolites — Short-chain fatty acids, tryptophan metabolites, and bile acid derivatives produced by gut bacteria cross the blood-brain barrier and modulate neural function.
- HPA axis (stress response) — Chronic stress activates the hypothalamic-pituitary-adrenal axis, which alters gut motility, permeability, and microbial composition. The gut, in turn, sends stress signals back to the brain.
Stanford Medicine researchers in 2026 described how this relationship affects conditions ranging from anxiety to long COVID to Parkinson's disease, noting that older mice with disrupted gut microbiomes showed dramatically higher levels of inflammation and worse neurological outcomes than younger mice with healthier guts.
What Are Psychobiotics and Can They Improve Mental Health?
Psychobiotics are specific probiotic strains that produce measurable effects on mental health. Lactobacillus rhamnosus has been shown to reduce anxiety-like behavior in animal models through vagus nerve signaling. Bifidobacterium longum demonstrates stress-reducing properties in human trials. These aren't magic pills, but they represent a genuine, evidence-based frontier in mental health support—and they work best alongside dietary and lifestyle changes that support the broader gut ecosystem.
What Causes Gut Health Problems in the First Place?
Gut health deteriorates when the delicate balance of the microbiome is disrupted by dietary, lifestyle, medical, and environmental factors—a state called dysbiosis. Most people don't develop gut issues overnight; it's a gradual erosion from multiple simultaneous stressors that eventually tips the balance.
Gut microbiota dysbiosis is defined by three hallmarks: loss of health-granting microbiota, proliferation of pathologic microbiota, and loss of overall microbial diversity [1]. Cleveland Clinic notes that dysbiosis can stem from both lifestyle choices and medical conditions, making it a multifactorial problem.
What Dietary Factors Damage Your Gut Microbiome?
- Excess sugar and refined carbohydrates — Feed harmful bacteria and yeast species like Candida, promoting dysbiosis
- Artificial sweeteners — Studies show aspartame, sucralose, and saccharin alter microbiome composition and may promote glucose intolerance
- Ultra-processed foods — Emulsifiers (polysorbate 80, carboxymethylcellulose) directly damage the intestinal mucus layer
- Excessive alcohol — Disrupts gut barrier integrity and promotes overgrowth of pathogenic species
- Low fiber intake — The average American eats only 15g of fiber daily (target: 25–35g), starving beneficial bacteria
- Excessive red meat — Produces TMAO (trimethylamine N-oxide), associated with cardiovascular disease and reduced beneficial bacteria
What Lifestyle and Medical Factors Harm the Gut?
- Antibiotics — Even a single course can devastate microbial diversity for months; broad-spectrum antibiotics are particularly destructive
- Chronic stress — Activates the HPA axis, altering gut motility, increasing permeability, and shifting microbial populations
- Poor sleep — The microbiome has its own circadian rhythm; irregular sleep patterns disrupt bacterial metabolic cycles
- Sedentary lifestyle — Lack of movement reduces microbial diversity and SCFA production
- NSAIDs (ibuprofen, aspirin) — Regular use damages the intestinal lining
- Environmental toxins — Pesticides, heavy metals, and endocrine disruptors (environmental toxins) alter microbial composition
- Over-sanitized environments — Reduced microbial exposure limits immune training and diversity development
What Are the Signs and Symptoms That Your Gut Health Is Compromised?
Gut health issues often manifest as a cluster of seemingly unrelated symptoms that span digestive, neurological, immune, and dermatological systems. Because the gut influences so many body functions, compromised gut health rarely presents as a single clear symptom—instead, it shows up as a pattern.
Digestive Symptoms
- Chronic bloating, especially after meals
- Gas (excessive flatulence or belching)
- Alternating constipation and diarrhea
- Acid reflux or heartburn
- Undigested food particles in stool
- Abdominal cramping or pain
Systemic Symptoms
- Persistent fatigue — Even after adequate sleep
- Brain fog — Difficulty concentrating, poor memory, mental sluggishness
- Mood disturbances — Unexplained anxiety, irritability, low mood
- Skin issues — Eczema flares, acne, rosacea, unexplained rashes
- Frequent infections — Colds, sinus infections, urinary tract infections (weakened immunity)
- Food sensitivities — Reacting to foods you previously tolerated
- Unexplained weight changes — Difficulty losing or gaining weight
- Joint pain — Low-grade systemic inflammation from gut permeability
- Sugar cravings — Harmful bacteria and yeast actively drive cravings for their preferred fuel
When Should You Take These Symptoms Seriously?
Occasional bloating after a heavy meal is normal. But if you're experiencing three or more of these symptoms consistently for more than 2–3 weeks, it's worth investigating your gut health—either through a structured protocol or with a healthcare provider's guidance.
What Are the Best Evidence-Based Strategies for Improving Gut Health?
The most effective gut health strategies combine dietary changes, targeted supplementation, and lifestyle modifications—no single intervention works in isolation. Research consistently shows that a multi-pronged approach yields the best results, typically within 4–8 weeks of consistent effort.
Here's a high-level overview of the five pillars of gut restoration:
- Diet optimization — Eliminating inflammatory foods while increasing fiber, fermented foods, and polyphenol-rich plants
- Probiotic replenishment — Introducing beneficial bacteria through food and supplements
- Prebiotic feeding — Providing fuel for beneficial bacteria to thrive and produce SCFAs
- Gut barrier repair — Using targeted nutrients (L-glutamine, zinc, omega-3) to heal intestinal permeability
- Lifestyle modification — Addressing sleep, stress, exercise, and medication use
Each of these pillars is covered in detail in the sections below, and they come together in the 30-Day Gut Health Transformation Protocol later in this guide.
What Should You Eat (and Avoid) for Optimal Gut Health?
The single most impactful dietary strategy for gut health is maximizing plant diversity—aiming for 30 or more different plant foods per week—while eliminating or reducing foods that damage the intestinal lining and feed pathogenic bacteria. Your daily food choices directly shape which microbial species thrive.
Which Foods Heal and Support the Gut?
Fermented foods (live probiotics):
- Yogurt (with live active cultures), kefir, sauerkraut, kimchi, kombucha, miso, tempeh
- A Stanford study found that a high-fermented-food diet increases microbiome diversity more effectively than a high-fiber diet alone
Prebiotic-rich foods (bacterial fuel):
- Garlic, onions, leeks, asparagus, Jerusalem artichokes, bananas, apples, oats, legumes
- These contain inulin, FOS, GOS, resistant starch, pectin, and beta-glucan [13] [14]
Polyphenol-rich foods:
- Berries, green tea, dark chocolate (70%+), extra-virgin olive oil, red grapes
- Polyphenols selectively feed beneficial bacteria and increase microbial diversity
Anti-inflammatory foods:
- Fatty fish (salmon, sardines, mackerel) — omega-3 fatty acids
- Turmeric and ginger — potent anti-inflammatory compounds
- Leafy greens — fiber, folate, and unique sugars that feed beneficial gut bacteria
Gut-lining support:
- Bone broth — collagen and L-glutamine support intestinal wall repair
- Aloe vera juice — soothes and supports mucosal lining
Which Foods Damage Gut Health?
| Food Category | Why It Harms the Gut | Action Step |
|---|---|---|
| Refined sugar | Feeds harmful bacteria and yeast, promotes dysbiosis | Replace with whole fruits, raw honey (small amounts) |
| Artificial sweeteners | Alters microbiome composition, may impair glucose tolerance | Switch to stevia or monk fruit if needed |
| Ultra-processed foods | Emulsifiers and additives damage mucus layer and tight junctions | Cook from whole ingredients 80% of the time |
| Excessive alcohol | Damages intestinal barrier, promotes pathogenic overgrowth | Limit to 1–2 drinks per week during gut healing |
| Gluten (if sensitive) | Increases zonulin production, raises intestinal permeability | Trial 4-week elimination to assess sensitivity |
What Lifestyle Changes Have the Biggest Impact on Gut Health?
Diet gets most of the attention, but lifestyle factors—particularly sleep, stress, and exercise—exert equally powerful effects on the microbiome. You can eat perfectly and still struggle with gut issues if these foundations are neglected.
How Does Exercise Affect Your Gut Microbiome?
Moderate exercise (30 minutes most days) directly increases microbial diversity and SCFA production. A landmark study from the University of Illinois found that six weeks of exercise altered the gut microbiome composition—and those changes reversed when exercise stopped. The sweet spot appears to be consistent moderate activity: brisk walking, cycling, swimming, yoga. Intense overtraining, conversely, can temporarily increase gut permeability.
Why Is Sleep So Critical for Gut Health?
Your gut microbiome operates on its own circadian rhythm. Disrupted sleep patterns—shift work, jet lag, inconsistent bedtimes—alter bacterial metabolic cycles, reduce beneficial species, and increase inflammatory markers. Aim for 7–9 hours of consistent sleep, prioritizing sleep hygiene: dark room, cool temperature (65–68°F), no screens 60 minutes before bed, consistent wake time.
How Does Chronic Stress Destroy Gut Health?
Chronic stress activates the HPA axis, which directly alters gut motility (causing either diarrhea or constipation), increases intestinal permeability, and shifts microbial populations toward pathogenic species. Effective daily practices include:
- Meditation or deep breathing — 10 minutes daily reduces cortisol and inflammatory markers
- Time in nature — Exposure to environmental microbes increases diversity
- Yoga or tai chi — Combines movement with stress reduction
- Social connection — Shared meals and physical contact facilitate microbiome exchange
What About Medications and Gut Health?
- Avoid unnecessary antibiotics — If prescribed, take probiotics during and for 4 weeks after the course
- Minimize NSAIDs — Ibuprofen and aspirin damage the gut lining with regular use; consider alternatives like turmeric for inflammation management
- Review PPIs (proton pump inhibitors) — Long-term use alters stomach pH and microbial composition; work with your doctor on step-down protocols if appropriate
Which Supplements Actually Support Gut Health?
Targeted supplementation accelerates gut healing when combined with dietary and lifestyle changes—but supplements alone won't fix a gut damaged by poor habits. Think of them as tools that support the protocol, not replacements for the foundational work.
Probiotics
Multi-strain formulas containing Lactobacillus and Bifidobacterium strains enhance gut barrier function and lower systemic inflammation [8]. Probiotics maintain balanced gut microbiota by promoting growth of beneficial bacteria while inhibiting pathogenic species [9].
Key strains to look for:
- Lactobacillus acidophilus — immune support, digestive health
- Lactobacillus rhamnosus GG — diarrhea, IBS, immune modulation
- Lactobacillus plantarum — gut barrier strengthening, inflammation reduction
- Bifidobacterium longum — stress reduction, IBS relief
- Bifidobacterium lactis — immunity, regularity
- Saccharomyces boulardii — antibiotic-associated diarrhea, C. diff prevention
Dosing: 10–50 billion CFU daily (multi-strain formulas generally outperform single-strain). Start low and increase gradually. Allow 4–8 weeks for full effects.
Prebiotics
Prebiotic supplementation fuels beneficial bacteria when dietary intake is insufficient. Intestinal microbiota composition is shaped by fiber-rich ingredients including resistant starch [12]. NOW Foods Organic Inulin (1 lb) provides a concentrated prebiotic source.
L-Glutamine
The most abundant amino acid in the body, L-glutamine is the preferred fuel source for intestinal cells (enterocytes). It supports repair of the intestinal lining and has been studied for reducing permeability.
Dosing: 5g twice daily during gut healing phases.
Zinc Carnosine
Specifically studied for gut barrier repair, zinc carnosine protects the gastric and intestinal lining.
Dosing: 75mg daily (typically split into two doses).
Omega-3 Fatty Acids
Anti-inflammatory omega-3s (EPA and DHA) from fish oil reduce intestinal inflammation and support barrier integrity.
Dosing: 2–3g combined EPA/DHA daily.
Digestive Enzymes
Useful during the initial healing phase for people with significant maldigestion symptoms. Broad-spectrum formulas containing protease, lipase, amylase, and lactase can improve nutrient absorption while the gut heals.
How Do You Start a Gut Health Transformation Protocol?
The 30-day gut health protocol follows four sequential phases—Remove, Repair, Reinoculate, and Rebalance—each building on the previous one. This isn't about perfection; it's about progressive improvement. Most people notice meaningful differences by the end of Week 2, with substantial changes by Week 4.
Week 1: REMOVE — Eliminate Gut Irritants
Goal: Reduce inflammation and identify food sensitivities.
- [ ] Remove refined sugar, artificial sweeteners, and ultra-processed foods
- [ ] Eliminate or sharply reduce alcohol
- [ ] Trial elimination of gluten and conventional dairy (reintroduce one at a time in Week 5)
- [ ] Switch to whole foods: vegetables, fruits, lean proteins, healthy fats
- [ ] Start a food diary — track meals, symptoms, energy, and bowel habits
- [ ] Hydration: 8+ glasses of filtered water daily
- [ ] Begin 10 minutes daily stress management (deep breathing, walking meditation)
Week 2: REPAIR — Support the Gut Lining
Goal: Heal intestinal barrier integrity and reduce permeability.
- [ ] Continue all Week 1 eliminations
- [ ] Start L-glutamine: 5g twice daily (morning and evening)
- [ ] Start zinc carnosine: 75mg daily (split AM/PM)
- [ ] Start omega-3 fish oil: 2–3g EPA/DHA daily
- [ ] Add bone broth: 1 cup daily (or collagen peptides: 10–20g daily)
- [ ] Optional: aloe vera juice — ¼ cup daily before meals
- [ ] Prioritize sleep: 7–9 hours, consistent schedule
- [ ] Increase stress management to 15–20 minutes daily
Week 3: REINOCULATE — Introduce Beneficial Bacteria
Goal: Restore beneficial bacteria and improve diversity.
- [ ] Continue Weeks 1–2 protocols
- [ ] Start multi-strain probiotic: 20–50 billion CFU daily
- [ ] OR add fermented foods: 1–2 servings daily (yogurt, kefir, sauerkraut, kimchi, kombucha)
- [ ] Rotate different fermented foods throughout the week for strain diversity
- [ ] Consider Saccharomyces boulardii if you have history of antibiotic use or Candida issues
- [ ] If you experience temporary gas or bloating from probiotics, reduce dose and increase gradually
Week 4: REBALANCE — Feed Your Beneficial Bacteria
Goal: Maximize diversity, increase SCFA production, establish sustainable habits.
- [ ] Continue all previous protocols
- [ ] Diversity challenge: Eat 30+ different plant foods this week (vegetables, fruits, whole grains, legumes, nuts, seeds, herbs, spices)
- [ ] Increase resistant starch: cooked-and-cooled potatoes, cooked-and-cooled rice, green bananas, oats
- [ ] Add polyphenol-rich foods: berries, green tea, dark chocolate, extra-virgin olive oil
- [ ] Increase prebiotic foods: garlic, onions, leeks, asparagus, Jerusalem artichokes
- [ ] 30 minutes moderate exercise most days
- [ ] Evaluate progress: compare food diary from Week 1 to now
Ongoing Maintenance (Week 5+)
- 80/20 rule: 80% gut-healthy foods, 20% flexibility
- Continue daily probiotics (food or supplement)
- Eat 30+ plant foods weekly as a baseline
- Include fermented foods regularly
- Maintain sleep hygiene and stress management practices
- Limit antibiotics to when genuinely necessary
- Regular exercise: 150 minutes moderate activity per week minimum
What Should You Do First to Start Improving Your Gut Health?
Start with the highest-impact, lowest-effort changes during your first week, then layer in more targeted interventions. Trying to do everything at once leads to overwhelm and abandonment—progressive implementation is the key to lasting results.
Phase 1 — This Week (Days 1–7):
- [ ] Remove refined sugar and ultra-processed foods from your kitchen
- [ ] Start a food and symptom diary
- [ ] Drink 8+ glasses of filtered water daily
- [ ] Add one fermented food daily (yogurt, kefir, or sauerkraut)
- [ ] Begin 10 minutes of daily deep breathing or meditation
Phase 2 — Next Week (Days 8–14):
- [ ] Start L-glutamine (5g 2x daily) and omega-3 fish oil (2–3g daily)
- [ ] Add 1 cup bone broth or collagen supplement daily
- [ ] Increase vegetable intake to 5+ servings daily
- [ ] Prioritize 7–9 hours of sleep with consistent timing
Phase 3 — Weeks 3–4:
- [ ] Start multi-strain probiotic (20–50 billion CFU)
- [ ] Complete the 30+ plant diversity challenge
- [ ] Increase prebiotic foods (garlic, onions, asparagus, oats)
- [ ] Add 30 minutes moderate exercise most days
Phase 4 — Ongoing:
- [ ] Maintain 80/20 approach to diet
- [ ] Continue probiotics and fermented foods
- [ ] Reassess symptoms monthly and adjust protocol
- [ ] Consider comprehensive stool testing at 3 months if symptoms persist
References
- Cryan, J.F. et al., 2025. The Microbiota-Gut-Brain Connection: A New Horizon in Neurological and Neuropsychiatric Disorders. PMC. Source
- Hrncir, T., 2022. Gut Microbiota Dysbiosis: Triggers, Consequences, Diagnostic and Therapeutic Options. PMC. Source
- AAMC, 2024. Follow Your Gut: How Research into the Gut-Brain Axis Could Unlock New Therapies. Source
- Fasano, A., 2020. All Disease Begins in the (Leaky) Gut: Role of Zonulin-Mediated Gut Permeability. Frontiers in Immunology. Source
- Kowalski, K. et al., 2025. Reinforcing Gut Integrity: A Systematic Review and Meta-Analysis of Clinical Trials Assessing Probiotics, Synbiotics, and Prebiotics on Intestinal Permeability Markers. Pharmacological Research. Source
- Sturgeon, C. & Fasano, A., 2021. Blurring the Picture in Leaky Gut Research: How Shortcomings of Zonulin as a Biomarker Mislead the Field. Gut. Source
- Sezgin, B. et al., 2025. Intestinal Permeability Assessed by Serum Zonulin in Liver Cirrhosis. Medicine. Source
- ScienceDirect, 2025. New Insights in the Gut-Brain Axis: The Role of Bioelectrical Microbiome. Source
- Cani, P.D. et al., 2024. Microbiome 2.0: Lessons from the 2024 Gut Microbiota for Health World Summit. PMC. Source
- Ogunrinola, G.A. et al., 2024. Intestinal Permeability Disturbances: Causes, Diseases and Therapy. PMC. Source
- Stanford Medicine, 2025. The Gut-Brain Connection: What the Science Says. Source
- Frontiers in Microbiology, 2025. Studies on Changes in Rectal Permeability and Intestinal Microbiota with Developmental Age. Source
Frequently asked questions
How long does it take to heal your gut?
Most people notice initial improvements within 2–3 weeks and significant changes within 4–8 weeks of consistent dietary and lifestyle changes. However, severe dysbiosis or conditions like leaky gut may take 3–6 months of sustained effort. The timeline depends on the severity of your starting point, consistency with the protocol, and whether underlying medical conditions are involved. Patience and consistency matter more than perfection.
Can you heal your gut without supplements?
Yes, many people can improve gut health through diet and lifestyle changes alone. Fermented foods (yogurt, kefir, sauerkraut, kimchi) provide probiotics, while garlic, onions, and oats provide prebiotics. Bone broth supplies glutamine naturally. Supplements accelerate the process and are particularly useful for people with significant dysbiosis, but they're not strictly required if your diet is comprehensive.
What is the difference between probiotics and prebiotics?
Probiotics are live beneficial microorganisms (bacteria and yeast) that you introduce into your gut through food or supplements. Prebiotics are non-digestible fibers that feed the beneficial bacteria already in your gut. Think of it this way: probiotics are the seeds, and prebiotics are the fertilizer. Both are important, and combining them (called synbiotics) creates a synergistic effect.
Do probiotic supplements actually survive stomach acid?
Many standard probiotic capsules lose significant viability in stomach acid. Look for delayed-release or enteric-coated capsules, which are designed to survive the acidic stomach environment and release in the intestines. Spore-based probiotics (Bacillus species) naturally survive stomach acid. Taking probiotics with food (which buffers stomach pH) also improves survival rates.
Is leaky gut a real medical condition?
Increased intestinal permeability is well-documented in medical research—gastrointestinal barrier dysfunction has been shown to contribute to systemic inflammation and several diseases. However, "leaky gut syndrome" as a standalone diagnosis remains controversial in conventional medicine. Many gastroenterologists acknowledge the mechanism but debate its role as a primary cause versus consequence of disease. The research is rapidly evolving.
How do you know if you have gut dysbiosis?
Common signs include chronic bloating, irregular bowel habits, food sensitivities, frequent infections, fatigue, brain fog, skin issues, and mood disturbances. A comprehensive stool test (from providers like Viome, Thorne, or Genova Diagnostics) can measure bacterial diversity, beneficial-to-pathogenic ratios, and inflammation markers. However, many people can identify dysbiosis through symptoms and successfully improve gut health without formal testing.
What kills good gut bacteria?
The biggest disruptors are broad-spectrum antibiotics (even a single course can devastate diversity for months), chronic stress, poor sleep, excess sugar and processed foods, excessive alcohol, NSAIDs (ibuprofen, aspirin) with regular use, and environmental toxins (pesticides, heavy metals). Of these, unnecessary antibiotic use is the single most destructive factor for the microbiome.
How many probiotic CFU do you need daily?
For general maintenance, 10–20 billion CFU daily is sufficient. For active gut restoration (during the 30-day protocol), 20–50 billion CFU daily from a multi-strain formula is recommended. More is not always better—strain diversity matters more than raw CFU count. Start at a lower dose and increase gradually to minimize temporary gas and bloating.
Can exercise really change your gut microbiome?
Yes. Research from the University of Illinois demonstrated that six weeks of moderate exercise (30 minutes, 3 times weekly) significantly altered gut microbiome composition, increasing SCFA-producing bacteria. These changes reversed when exercise stopped, confirming that consistent activity is needed for sustained benefits. Even daily walking improves microbial diversity.
What foods are highest in prebiotics?
The richest prebiotic food sources include chicory root (highest inulin content), Jerusalem artichokes, raw garlic, raw onions, leeks, asparagus, dandelion greens, bananas (especially slightly green), oats, and legumes (beans, lentils, chickpeas). Cooked-and-cooled potatoes and rice are excellent sources of resistant starch, another important prebiotic. Aim for 25–35g of total fiber daily from diverse sources.