gut health
Healing Leaky Gut Syndrome: Complete Evidence-Based Protocol
Science-based leaky gut healing guide. Learn the 5R Protocol, best supplements (L-glutamine, zinc carnosine), root causes, and proven gut barrier repair strategies.
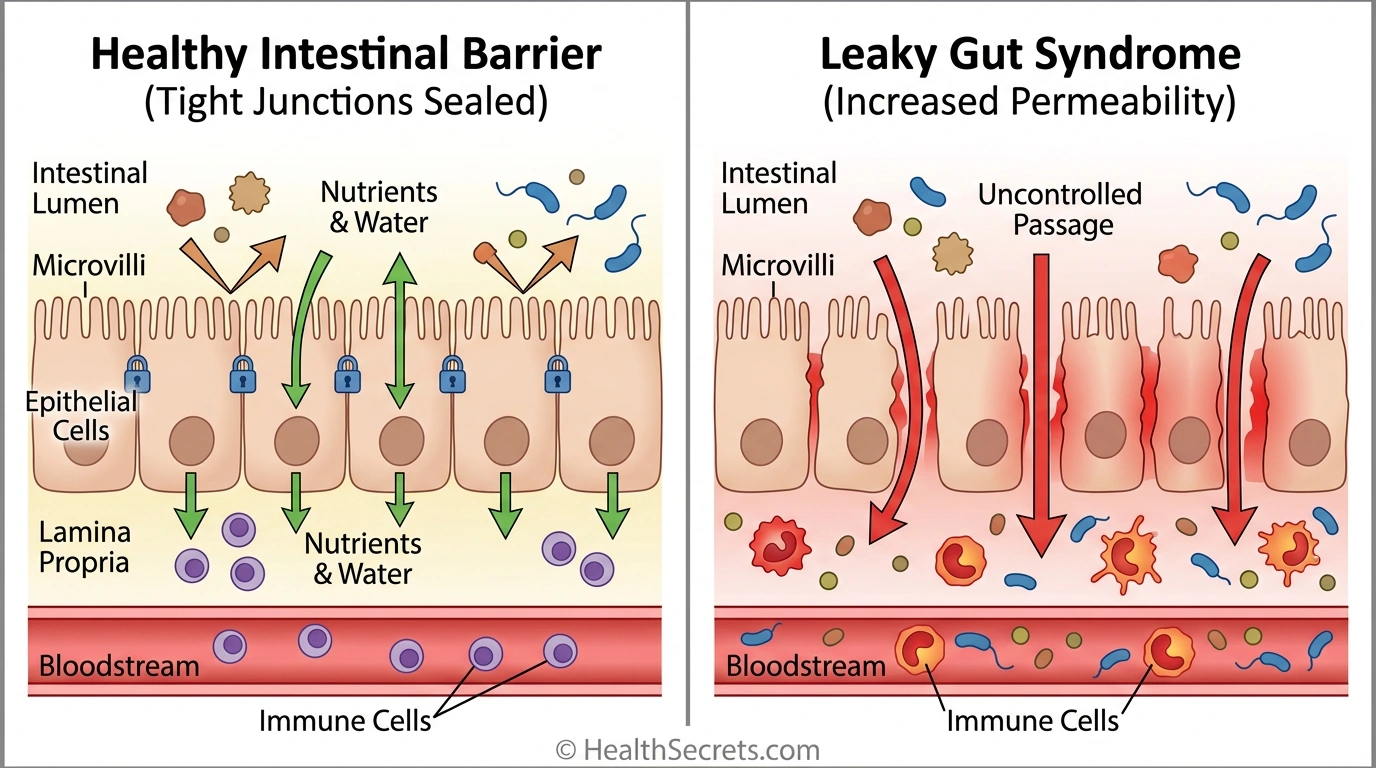
Your gut lining is just one cell thick — a single layer of epithelial cells standing between the outside world and your bloodstream. When that barrier breaks down, a condition researchers call increased intestinal permeability (commonly known as "leaky gut syndrome") allows partially digested food particles, bacterial toxins, and other molecules to slip through into your body, triggering widespread inflammation that can manifest as digestive problems, skin issues, joint pain, brain fog, and even autoimmune disease.
For decades, mainstream medicine dismissed leaky gut as fringe science. That changed dramatically when Dr. Alessio Fasano's groundbreaking research identified zonulin — a protein that regulates the tight junctions between intestinal cells — and demonstrated that increased intestinal permeability precedes and contributes to autoimmune conditions, not the other way around [1]. Today, over 3,000 peer-reviewed studies reference intestinal permeability, and the evidence is clear: a compromised gut barrier is both a cause and consequence of chronic disease.
This guide walks you through everything science currently knows about healing leaky gut syndrome — from understanding the gut barrier mechanics and identifying root causes, to implementing the proven 5R Protocol (Remove, Replace, Reinoculate, Repair, Rebalance) used by functional medicine practitioners worldwide. Whether you're dealing with unexplained food sensitivities, persistent digestive issues, or autoimmune symptoms that won't resolve, restoring your gut barrier is often the missing piece.
- Leaky gut (increased intestinal permeability) occurs when tight junctions between intestinal cells break down, allowing toxins, food particles, and bacteria to enter the bloodstream
- Zonulin, discovered by Dr. Alessio Fasano, is the key protein that regulates tight junction permeability — gluten and gut bacteria are the two main triggers of zonulin release [1]
- The top causes of leaky gut are processed foods, gluten (in sensitive individuals), chronic stress, NSAIDs, antibiotics, alcohol, and gut infections like SIBO and candida overgrowth
- Leaky gut is linked to autoimmune diseases (celiac, Crohn's, type 1 diabetes, rheumatoid arthritis), allergies, eczema, depression, and chronic fatigue [2]
- L-glutamine (5–10 g/day) is the most researched gut-healing nutrient — it's the primary fuel source for intestinal epithelial cells and directly supports barrier repair [3]
- The 5R Protocol (Remove, Replace, Reinoculate, Repair, Rebalance) is the evidence-based framework used by functional medicine practitioners to heal intestinal permeability
- Healing timeline is typically 3–6 months with consistent protocol adherence, though some people notice improvement in 2–4 weeks
- Zinc carnosine (75 mg twice daily) has clinical evidence for repairing damaged gut mucosa and is used in Japan as a prescription treatment for gastric ulcers [4]
- Collagen peptides provide the amino acids (glycine, proline, glutamine) that intestinal cells need to rebuild the gut lining
- Prevention requires ongoing attention — stress management, diverse whole-food diet, and avoiding unnecessary NSAIDs and antibiotics are the cornerstones of long-term gut barrier health
What Is Leaky Gut Syndrome and Why Should You Take It Seriously?
Leaky gut syndrome — clinically known as increased intestinal permeability — is a condition where the tight junctions between cells in your intestinal lining become damaged and loose, creating microscopic gaps that allow bacteria, toxins, and undigested food particles to "leak" through the gut wall into the bloodstream. This triggers an immune response that can cause both local digestive symptoms and systemic inflammation throughout the body [1][2].
How Does the Gut Barrier Normally Work?
Your intestinal lining has a dual mission: absorb nutrients while blocking everything harmful.
It accomplishes this through:
- Epithelial cells: A single layer of cells (enterocytes) that line the entire intestinal tract — replaced every 3–5 days
- Tight junctions: Protein complexes (claudins, occludins, zonula occludens) that seal the spaces between cells, acting like molecular gatekeepers
- Mucus layer: A protective gel layer secreted by goblet cells that prevents direct contact between bacteria and the epithelial surface
- Secretory IgA (sIgA): Antibodies that neutralize pathogens before they reach the barrier
- Microbiome: Trillions of beneficial bacteria that compete with pathogens, produce short-chain fatty acids, and strengthen barrier integrity
What Is Zonulin and Why Does It Matter?
Zonulin is the only known physiological regulator of intestinal tight junctions in humans. When zonulin is released, it reversibly opens the tight junctions — a normal process for nutrient absorption. The problem occurs when zonulin production becomes chronically elevated, keeping the gates permanently open [1].
The two primary triggers of zonulin release:
- Gliadin (a component of gluten) — triggers zonulin in genetically susceptible individuals
- Small intestinal bacterial overgrowth (SIBO) — bacteria in the wrong location triggers zonulin as a flushing mechanism
How Prevalent Is Leaky Gut?
While exact prevalence is difficult to establish (no universal diagnostic standard), research suggests increased intestinal permeability is present in:
- 40–60% of people with IBS [5]
- Nearly all people with celiac disease
- A significant portion of people with autoimmune conditions
- An increasing number of people eating a standard Western diet
What Causes Leaky Gut Syndrome?
Leaky gut develops from a combination of dietary, lifestyle, medical, and environmental factors that damage the intestinal barrier over time. In most cases, it's not a single cause but a cumulative assault from multiple triggers acting simultaneously — processed food damages the mucus layer, stress suppresses repair, NSAIDs dissolve protective barriers, and dysbiosis shifts the microbiome toward inflammation [2][6].
Dietary Causes
- Gluten (in genetically susceptible individuals): Triggers zonulin release, opens tight junctions [1]
- Processed foods: Emulsifiers (polysorbate 80, carboxymethylcellulose) directly damage the mucus layer [7]
- Excess sugar and fructose: Feed pathogenic bacteria, increase inflammation, impair barrier function
- Alcohol: Directly damages intestinal cells and disrupts tight junction proteins
- Industrial seed oils: High omega-6 promotes intestinal inflammation
- Food additives: Artificial sweeteners, preservatives, and colors alter microbiome composition
Medication-Related Causes
- NSAIDs (ibuprofen, naproxen, aspirin): Directly increase intestinal permeability within hours of use — one of the most common and underrecognized causes [8]
- Antibiotics: Devastate beneficial bacteria, allowing opportunistic pathogens to dominate
- Proton pump inhibitors (PPIs): Reduce stomach acid, allowing bacterial overgrowth and altering microbiome
- Oral contraceptives and corticosteroids: Disrupt gut flora and immune regulation
Lifestyle and Environmental Causes
- Chronic stress: Activates the HPA axis, increases cortisol, directly increases intestinal permeability through mast cell activation [9]
- Sleep deprivation: Even 2 nights of poor sleep measurably increases intestinal permeability
- Excessive exercise: Intense endurance exercise temporarily increases gut permeability ("runner's gut")
- Environmental toxins: Pesticides (glyphosate), heavy metals, BPA disrupt gut barrier function
Infection-Related Causes
- SIBO (Small Intestinal Bacterial Overgrowth): Bacteria in the wrong location triggers chronic zonulin elevation
- Candida overgrowth: Fungal hyphae physically penetrate the intestinal lining
- Parasites: Direct mechanical damage to epithelial cells
- H. pylori and other pathogens: Chronic infection maintains inflammatory state
What Are the Symptoms of Leaky Gut Syndrome?
Leaky gut symptoms extend far beyond the digestive tract because the inflammatory response triggered by gut barrier breakdown is systemic — affecting virtually every organ system. The hallmark pattern is a combination of digestive complaints (bloating, food sensitivities, irregular bowel habits) alongside seemingly unrelated systemic symptoms (joint pain, brain fog, skin issues, fatigue) that conventional testing can't fully explain [2][10].
Digestive Symptoms
- Chronic bloating and gas (especially after meals)
- Food sensitivities that seem to multiply over time
- Alternating constipation and diarrhea
- Abdominal pain or cramping
- Heartburn or acid reflux
- Nausea after eating
Systemic Symptoms
- Brain fog and cognitive issues: Difficulty concentrating, memory problems, mental fatigue
- Skin problems: Eczema, psoriasis, acne, rosacea, unexplained rashes
- Joint pain: Migratory joint pain, stiffness, inflammation without injury
- Chronic fatigue: Exhaustion that doesn't improve with rest
- Mood disturbances: Anxiety, depression, irritability (gut-brain axis disruption)
- Autoimmune flares: Worsening of existing autoimmune symptoms
Immune System Symptoms
- Frequent infections (lowered immune function)
- New-onset allergies or worsening of existing allergies
- Histamine intolerance symptoms (headaches, flushing, hives)
- Chemical and environmental sensitivities
The "Multiplying Food Sensitivity" Pattern
:::warning[Key warning sign] If you notice that the number of foods you react to keeps growing over time, this strongly suggests leaky gut. When undigested food particles cross the barrier, your immune system creates antibodies against them — each new "leak" can create a new sensitivity. Healing the barrier stops this cycle. :::
How Is Leaky Gut Diagnosed?
There is no single gold-standard diagnostic test for leaky gut, but several clinical tools can assess intestinal permeability. The most validated test is the lactulose-mannitol test, which measures the ratio of two sugar molecules that cross the gut barrier differently. Elevated serum zonulin is another emerging biomarker, though interpretation varies between labs [1][11].
Available Testing Methods
| Test | What It Measures | Reliability |
|---|---|---|
| Lactulose-Mannitol Test | Ratio of sugar molecules crossing gut barrier | Most validated research tool |
| Serum Zonulin | Tight junction regulator protein levels | Emerging biomarker, variable accuracy |
| Intestinal Fatty Acid Binding Protein (I-FABP) | Marker of intestinal cell damage | Good for acute damage assessment |
| Stool Secretory IgA (sIgA) | Gut immune defense capacity | Indirect indicator of barrier stress |
| Comprehensive Stool Analysis | Microbiome composition, inflammation markers | Helpful for identifying root causes |
What to Ask Your Doctor
- Request a comprehensive metabolic panel and inflammatory markers (CRP, ESR)
- Ask about lactulose-mannitol testing or zonulin testing
- Consider comprehensive stool analysis through a functional medicine practitioner
- Rule out celiac disease (tissue transglutaminase antibodies) and inflammatory bowel disease
- Consider SIBO breath testing if bacterial overgrowth is suspected
What Are the Conventional Treatment Options for Leaky Gut?
Conventional medicine has been slower to adopt leaky gut as a standalone diagnosis, so treatment typically focuses on managing the conditions associated with increased intestinal permeability rather than targeting the barrier itself. Gastroenterologists may prescribe anti-inflammatory medications for IBD, antibiotics for SIBO, immunosuppressants for autoimmune conditions, and dietary modifications — particularly a gluten-free diet for celiac disease [12].
Standard Medical Approaches
- Dietary modification: Elimination of known triggers (gluten for celiac, FODMAPs for IBS)
- Anti-inflammatory medications: For IBD-associated permeability
- Antibiotics: Rifaximin for SIBO treatment
- Immunosuppressants: For autoimmune conditions linked to permeability
- Prokinetics: To improve gut motility and prevent bacterial overgrowth recurrence
Limitations of Conventional Approaches
- Often treat downstream symptoms rather than the barrier dysfunction itself
- May not address root causes (diet, stress, microbiome imbalance)
- Some medications (NSAIDs, PPIs, antibiotics) can worsen permeability
- Limited focus on nutritional support for barrier repair
:::tip[Integrative approach recommended] The most effective strategy combines conventional medical evaluation (to rule out serious conditions and identify root causes) with the functional medicine 5R Protocol (to actively repair the gut barrier). Work with both a gastroenterologist and a functional medicine practitioner when possible. :::
What Natural Approaches Support Leaky Gut Healing?
The most effective evidence-based framework for healing leaky gut is the 5R Protocol — a systematic approach developed by the Institute for Functional Medicine that addresses root causes, restores digestive capacity, repopulates beneficial bacteria, repairs the intestinal lining, and rebalances lifestyle factors. Clinical experience shows this protocol, when followed consistently for 3–6 months, can measurably improve intestinal permeability in most patients [13].
Step 1 (Remove): What Foods and Triggers Should You Eliminate First?
The first and most impactful step is removing everything that damages the gut barrier. This typically involves a 4–6 week elimination phase:
Foods to remove:
- Gluten and wheat products (primary zonulin trigger)
- Processed foods, refined sugar, and artificial additives
- Alcohol (directly damages intestinal cells)
- Dairy (casein is inflammatory for many people with leaky gut)
- Industrial seed oils (soybean, corn, canola)
- Known personal food sensitivities
Other triggers to remove:
- NSAIDs — switch to acetaminophen (short-term) or natural anti-inflammatories
- Unnecessary antibiotics
- Environmental toxins where possible
For a structured approach to identifying trigger foods, see our elimination diet guide. For understanding food intolerances and leaky gut, see our companion guide.
Step 2 (Replace): How Do You Restore Proper Digestive Function?
Many people with leaky gut have inadequate digestive capacity — low stomach acid, insufficient enzymes, or poor bile flow — which leaves food partially digested, increasing the inflammatory load on the gut barrier.
Key replacements:
- Digestive enzymes: Broad-spectrum with meals (protease, lipase, amylase) — see our digestive enzymes guide
- Betaine HCl: If low stomach acid is suspected (burning sensation after supplementation means you don't need it)
- Bile salts: If fat malabsorption is present (light-colored stools, fatty food intolerance)
- Apple cider vinegar: 1 tablespoon in water before meals to stimulate digestive juices
Step 3 (Reinoculate): Which Probiotics Help Restore Gut Barrier Function?
Restoring a healthy microbiome is essential because beneficial bacteria produce short-chain fatty acids (especially butyrate) that directly fuel intestinal cell repair and strengthen tight junctions.
Evidence-based probiotic strains for gut barrier repair:
- Lactobacillus rhamnosus GG — most studied strain for barrier function [14]
- Saccharomyces boulardii — yeast-based probiotic, protects against antibiotic damage
- Bifidobacterium infantis — reduces inflammation markers, improves IBS symptoms
- Lactobacillus plantarum — strengthens tight junctions in clinical studies
Dosing: 25–100 billion CFU daily from a multi-strain formula. For detailed guidance, see our best probiotics for gut repair review.
Prebiotic foods (feed beneficial bacteria): garlic, onions, leeks, asparagus, bananas, oats, flaxseed.
Step 4 (Repair): What Nutrients Directly Heal the Gut Lining?
This is where targeted supplementation makes the biggest difference. The gut lining replaces itself every 3–5 days, and these nutrients provide the raw materials for repair:
L-Glutamine (Primary gut-healing nutrient):
- The #1 fuel source for intestinal epithelial cells (enterocytes)
- Directly supports tight junction protein expression
- Clinically studied dose: 5–10 g/day in divided doses (2.5–5 g twice daily)
- Start with 2.5 g and increase gradually [3]
- For our complete guide, see L-glutamine for leaky gut
Zinc Carnosine:
- Protects and repairs gastric and intestinal mucosa
- Used in Japan as prescription treatment for gastric ulcers
- Dose: 75 mg twice daily with meals [4]
Collagen Peptides:
- Provides glycine, proline, and glutamine — the amino acids intestinal cells need for repair
- Dose: 10–20 g/day
- See our collagen for gut health guide
Additional repair nutrients:
- DGL (Deglycyrrhizinated licorice): 400 mg before meals — soothes and protects mucosa
- Slippery elm: 400–800 mg before meals — coats and protects intestinal lining
- Marshmallow root: 300–500 mg — mucilaginous herb that soothes inflammation
- Bone broth: Rich in gelatin, glycine, and glutamine — see our bone broth for gut repair guide
- Omega-3 fatty acids: 2–3 g EPA/DHA daily — reduce intestinal inflammation
Step 5 (Rebalance): What Lifestyle Changes Support Long-Term Gut Healing?
The gut barrier is exquisitely sensitive to stress, sleep, and lifestyle — no supplement protocol will succeed without addressing these foundations:
- Stress management: Chronic stress directly increases permeability through cortisol and mast cell activation. Daily meditation, yoga, deep breathing, or nature exposure [9]
- Sleep 7–9 hours: Gut repair peaks during sleep. Consistent sleep schedule, dark room, no eating 3 hours before bed
- Moderate exercise: Walking, yoga, swimming support gut motility and reduce inflammation. Avoid overtraining (excessive endurance exercise increases permeability)
- Mindful eating: Chew thoroughly (30+ chews per bite), eat in a relaxed state, don't rush meals
- Social connection: The gut-brain axis responds to emotional wellbeing
For a comprehensive overview of all gut health strategies, see our complete gut health guide.
Can You Prevent Leaky Gut from Returning?
Yes — once you've healed the gut barrier, prevention requires maintaining the dietary and lifestyle foundations that supported repair, while being vigilant about the triggers that caused the problem originally. The gut lining replaces itself every 3–5 days, which means both damage and repair happen quickly. Most relapses occur when people return to their pre-protocol diet and lifestyle after feeling better [2].
Long-Term Prevention Strategies
- Maintain a diverse whole-food diet rich in fiber, polyphenols, and fermented foods
- Avoid unnecessary NSAIDs — use natural anti-inflammatories (turmeric, omega-3s) when possible
- Limit alcohol to occasional use or eliminate entirely
- Continue daily probiotics or regularly consume fermented foods (sauerkraut, kimchi, kefir, yogurt)
- Manage stress proactively — don't wait for symptoms to return
- Maintain L-glutamine at a lower maintenance dose (2.5–5 g/day) long-term
- Reintroduce foods carefully using a structured reintroduction protocol after the elimination phase
- Monitor for warning signs — if bloating, food sensitivities, or fatigue return, tighten the protocol immediately
Leaky Gut Healing Foods vs. Foods to Avoid
| Healing Foods (Eat Freely) | Moderate Carefully | Avoid During Healing |
|---|---|---|
| Bone broth, collagen | Eggs (reintroduce after 4 weeks) | Gluten and wheat |
| Wild-caught fish (salmon, sardines) | Nightshades (tomatoes, peppers) | Processed foods, additives |
| Fermented vegetables (sauerkraut, kimchi) | Nuts and seeds (soak first) | Refined sugar, HFCS |
| Cooked vegetables (squash, sweet potato, zucchini) | Dairy (ghee usually tolerated first) | Alcohol |
| Healthy fats (olive oil, coconut oil, avocado) | Legumes (well-cooked, start small) | Industrial seed oils |
When Should You See a Doctor About Leaky Gut?
You should see a gastroenterologist if you experience persistent digestive symptoms lasting more than 4 weeks, unexplained weight loss, blood in your stool, severe abdominal pain, or symptoms that worsen despite dietary changes. These could indicate conditions like inflammatory bowel disease, celiac disease, or other serious gastrointestinal disorders that require medical diagnosis and treatment — not just supplementation [12].
Red Flags Requiring Immediate Medical Attention
:::warning[See a doctor immediately if you experience]
- Blood in stool or black tarry stools
- Severe or worsening abdominal pain
- Unexplained weight loss (more than 5% in a month)
- Persistent vomiting
- High fever with digestive symptoms
- Signs of severe dehydration
:::
When to Schedule an Appointment
- Digestive symptoms lasting more than 4 weeks without improvement
- Symptoms that don't respond to dietary and lifestyle changes after 6–8 weeks
- Suspected autoimmune condition (joint pain, rashes, fatigue pattern)
- Family history of celiac disease, IBD, or autoimmune conditions
- Need for proper SIBO testing or comprehensive stool analysis
- Currently taking medications that may affect gut permeability
Specialist Recommendations
- Gastroenterologist: For ruling out IBD, celiac disease, and other structural GI conditions
- Functional medicine practitioner: For comprehensive gut health assessment, advanced stool testing, and 5R Protocol guidance
- Registered dietitian (GI-specialized): For structured elimination diets and food reintroduction planning
What Should You Do First to Start Healing Leaky Gut?
Start with the Remove phase this week — eliminate the top gut barrier destroyers (gluten, processed foods, alcohol, sugar, and NSAIDs) while adding bone broth daily. This single step reduces the inflammatory assault on your gut lining and creates the conditions for healing to begin. Most people notice reduced bloating within the first 1–2 weeks.
Phase 1: This Week (Remove)
- [ ] Eliminate gluten, processed foods, refined sugar, and alcohol
- [ ] Stop NSAIDs — consult doctor about alternatives
- [ ] Start drinking bone broth daily (1–2 cups)
- [ ] Begin a food diary to identify trigger foods
- [ ] Schedule appointment with gastroenterologist or functional medicine practitioner
Phase 2: Weeks 2–4 (Replace + Reinoculate)
- [ ] Start digestive enzymes with meals
- [ ] Begin probiotic supplementation (25–50 billion CFU multi-strain)
- [ ] Add fermented foods daily (sauerkraut, kimchi, kefir)
- [ ] Increase prebiotic-rich foods (garlic, onions, asparagus)
- [ ] Start L-glutamine at 2.5 g twice daily
Phase 3: Months 2–3 (Repair)
- [ ] Increase L-glutamine to 5 g twice daily if tolerated
- [ ] Add zinc carnosine (75 mg twice daily)
- [ ] Add collagen peptides (10–20 g daily)
- [ ] Consider DGL and slippery elm before meals
- [ ] Add omega-3 supplementation (2–3 g EPA/DHA)
Phase 4: Months 3–6 (Rebalance + Maintenance)
- [ ] Begin structured food reintroduction (one food every 3–4 days)
- [ ] Establish consistent stress management practice
- [ ] Optimize sleep (7–9 hours consistently)
- [ ] Consider retesting (zonulin, stool analysis) to measure progress
- [ ] Transition to maintenance supplement doses
References
- Fasano A. Zonulin and its regulation of intestinal barrier function: the biological door to inflammation, autoimmunity, and cancer. Physiol Rev. 2011;91(1):151-175. Source
- Camilleri M. Leaky gut: mechanisms, measurement and clinical implications in humans. Gut. 2019;68(8):1516-1526. Source
- Rao R, Samak G. Role of Glutamine in Protection of Intestinal Epithelial Tight Junctions. J Epithel Biol Pharmacol. 2012;5(Suppl 1-M7):47-54. Source
- Mahmood A, et al. Zinc carnosine, a health food supplement that stabilises small bowel integrity and stimulates gut repair processes. Gut. 2007;56(2):168-175. Source
- Camilleri M, et al. Intestinal barrier function in health and gastrointestinal disease. Neurogastroenterol Motil. 2012;24(6):503-512. Source
- Mu Q, et al. Leaky Gut As a Danger Signal for Autoimmune Diseases. Front Immunol. 2017;8:598. Source
- Chassaing B, et al. Dietary emulsifiers impact the mouse gut microbiota promoting colitis and metabolic syndrome. Nature. 2015;519(7541):92-96. Source
- Bjarnason I, et al. Mechanisms of Damage to the Gastrointestinal Tract From Nonsteroidal Anti-Inflammatory Drugs. Gastroenterology. 2018;154(3):500-514. Source
- Vanuytsel T, et al. Psychological stress and corticotropin-releasing hormone increase intestinal permeability in humans by a mast cell-dependent mechanism. Gut. 2014;63(8):1293-1299. Source
- Obrenovich MEM. Leaky Gut, Leaky Brain? Microorganisms. 2018;6(4):107. Source
- Vojdani A. For the Assessment of Intestinal Permeability, Size Matters. Altern Ther Health Med. 2013;19(1):12-24. Source
- Bischoff SC, et al. Intestinal permeability — a new target for disease prevention and therapy. BMC Gastroenterol. 2014;14:189. Source
Frequently asked questions
Is leaky gut a real medical condition?
Yes — increased intestinal permeability is a well-documented physiological phenomenon supported by thousands of peer-reviewed studies. While "leaky gut syndrome" isn't an official medical diagnosis in conventional gastroenterology, the underlying mechanism (compromised tight junctions, increased zonulin, barrier dysfunction) is scientifically established and recognized as a contributing factor to multiple chronic diseases including autoimmune conditions, IBS, and metabolic disorders.
How long does it take to heal leaky gut?
Most people following a consistent 5R Protocol notice initial symptom improvement (reduced bloating, better digestion) within 2–4 weeks. Significant barrier repair typically takes 3–6 months of consistent protocol adherence. The intestinal lining replaces itself every 3–5 days, so the tissue can heal relatively quickly once you remove the triggers and provide the right nutrients. Severe cases or those with underlying autoimmune conditions may take 6–12 months.
Can you test for leaky gut at home?
There is no reliable at-home test for leaky gut. The most validated assessment is the lactulose-mannitol test, which requires a clinical lab. Some companies offer at-home zonulin tests through mail-order stool or blood kits, but accuracy varies. The most practical approach is to work with a functional medicine practitioner who can order comprehensive stool analysis and appropriate permeability markers.
Does gluten cause leaky gut in everyone?
No — gluten triggers zonulin release and increases intestinal permeability primarily in genetically susceptible individuals. Research by Dr. Fasano shows that gliadin (a component of gluten) triggers zonulin in people with certain HLA genotypes, particularly those with celiac disease or non-celiac gluten sensitivity. However, not everyone reacts to gluten, and a trial elimination (4–6 weeks gluten-free) is the best way to determine your individual response.
What is the best single supplement for leaky gut?
L-glutamine is the most evidence-based single supplement for leaky gut repair. It is the primary fuel source for intestinal epithelial cells and directly supports tight junction protein expression. The therapeutic dose is 5–10 g per day in divided doses. While a comprehensive protocol works best, if you can only take one supplement, L-glutamine should be your choice.
Can stress alone cause leaky gut?
Yes — chronic psychological stress is a well-documented cause of increased intestinal permeability, independent of diet. Stress activates the HPA axis, increases cortisol, triggers mast cell degranulation in the gut wall, and directly loosens tight junctions. Animal and human studies confirm that stress-induced permeability changes are measurable and can persist for weeks after the stressor resolves. This is why the "Rebalance" phase of the 5R Protocol is essential.
Do NSAIDs really damage the gut lining?
Yes, significantly. NSAIDs (ibuprofen, naproxen, aspirin) increase intestinal permeability within hours of a single dose by inhibiting prostaglandin synthesis, which is needed for mucosal protection. Chronic NSAID use is one of the most common and underrecognized causes of leaky gut. If you're healing leaky gut, eliminating NSAIDs is a critical first step. Discuss alternatives with your doctor.
Is bone broth really helpful for leaky gut?
Bone broth provides gelatin (cooked collagen), glycine, glutamine, and other amino acids that support intestinal repair — making it a gentle, food-based complement to a leaky gut protocol. While there are no direct clinical trials on bone broth and intestinal permeability specifically, the individual nutrients it contains are well-researched for gut barrier support. Aim for 1–2 cups of quality bone broth daily.
Can leaky gut cause autoimmune disease?
Research strongly suggests that increased intestinal permeability is a prerequisite for the development of autoimmune disease in genetically susceptible individuals. Dr. Fasano's research proposed that autoimmunity requires three factors: genetic susceptibility, an environmental trigger, and increased intestinal permeability. Studies have documented leaky gut preceding the onset of type 1 diabetes, celiac disease, and other autoimmune conditions. Healing the barrier may help reduce autoimmune activity.
Should you take probiotics on an empty stomach for leaky gut?
It depends on the formulation. Standard probiotic capsules generally survive better when taken 30 minutes before a meal or first thing in the morning on an empty stomach — stomach acid is lowest at these times. However, delayed-release capsules (like the Renew Life formula we recommend) are designed to survive stomach acid and can be taken with or without food. Spore-based probiotics are naturally acid-resistant and can be taken anytime.