gut health
The Gut-Brain Axis Explained: How Your Gut Affects Your Mind
Discover how the gut-brain axis connects your digestive system to your mental health through the vagus nerve, neurotransmitters, and microbiome signaling.
Have you ever had a "gut feeling" about something, or felt butterflies in your stomach before a big event? Those sensations are not just figures of speech — they are direct evidence of a powerful communication system between your gut and your brain that scientists are only beginning to fully understand.
Your gastrointestinal tract houses over 100 million nerve cells, produces more than 90% of your body's serotonin, and contains roughly 70% of your entire immune system. This "second brain" in your gut communicates constantly with the brain in your head through a complex network of nerves, hormones, immune molecules, and microbial metabolites known as the gut-brain axis.
For a comprehensive foundation in digestive health, start with our complete guide to gut health. If you are interested in the mental wellness side of this connection, explore our mental wellness complete guide. Those looking for practical dietary strategies can find them in our fermented foods for gut health guide.
- The gut-brain axis is a bidirectional communication network linking the enteric nervous system (100+ million neurons in your gut) to the central nervous system through neural, hormonal, immune, and metabolic pathways.
- Your gut produces approximately 90% of serotonin and 50% of dopamine — two neurotransmitters critical for mood regulation, motivation, and emotional wellbeing.
- The vagus nerve serves as the primary physical highway between gut and brain, and higher vagal tone is associated with better stress resilience and emotional regulation.
- Psychobiotics — specific probiotic strains like Lactobacillus rhamnosus and Bifidobacterium longum — show clinical promise for reducing anxiety and depression symptoms.
- Gut dysbiosis (microbial imbalance) has been linked to depression, anxiety, autism spectrum disorders, cognitive decline, and neurodegenerative diseases in emerging research.
- A diet rich in fermented foods, prebiotic fiber, omega-3 fatty acids, and polyphenols supports optimal gut-brain axis function and mental health.
- Lifestyle practices including meditation, deep breathing, regular exercise, and quality sleep directly improve vagal tone and gut-brain communication.
What Is the Gut-Brain Axis and Why Does It Matter for Mental Health?
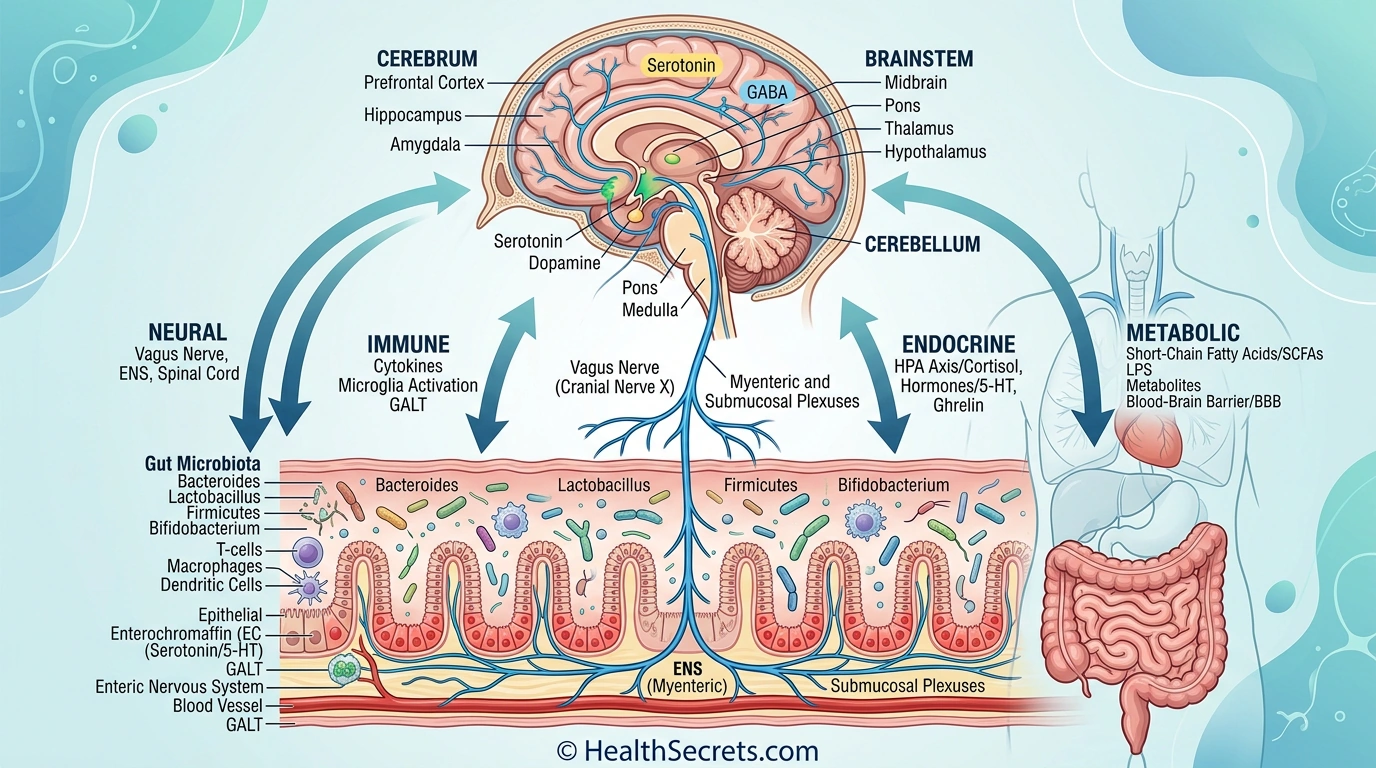
The gut-brain axis is a bidirectional communication system that connects the enteric nervous system in your gastrointestinal tract with the central nervous system in your brain and spinal cord. This network operates through four distinct pathways — neural, endocrine, immune, and metabolic — allowing your gut and brain to continuously exchange information that influences digestion, mood, cognition, immunity, and stress responses.
As Hippocrates observed over 2,000 years ago, "all disease begins in the gut." Modern science is proving this intuition remarkably prescient. Research published in the Annals of Gastroenterology confirms that the gut-brain axis is not merely anatomical but extends to include endocrine, humoral, metabolic, and immune routes of communication.
The Enteric Nervous System: Your "Second Brain"
Hidden within the walls of your digestive tract lies the enteric nervous system (ENS) — a network of over 100 million nerve cells lining the gastrointestinal tract from esophagus to rectum. According to Johns Hopkins Medicine, this "brain in your gut" is revolutionizing medicine's understanding of the links between digestion, mood, health, and cognition.
The ENS can operate independently of the brain, controlling digestive processes like peristalsis, enzyme secretion, and blood flow. But its constant communication with the central nervous system is what makes the gut-brain axis so significant for mental health.
Key Communication Pathways
| Pathway | Mechanism | Brain Impact |
|---|---|---|
| Neural | Vagus nerve signaling | Mood, anxiety, stress response |
| Endocrine | HPA axis hormones | Cortisol, stress regulation |
| Immune | Cytokine signaling | Neuroinflammation, depression |
| Metabolic | SCFAs, tryptophan metabolites | Neurotransmitter production |
How Does the Gut-Brain Axis Actually Work?
The gut-brain axis works through four interconnected communication pathways that operate simultaneously: the vagus nerve provides a direct neural highway, the hypothalamic-pituitary-adrenal (HPA) axis regulates hormonal stress responses, immune cells transmit inflammatory signals, and gut microbes produce metabolites that directly influence brain chemistry. Together, these pathways create a continuous feedback loop between your digestive system and your brain.
How Does the Vagus Nerve Connect the Gut and Brain?
The vagus nerve is the longest cranial nerve in the body, running from the brainstem through the neck, chest, and abdomen to innervate the entire gastrointestinal tract. It serves as the primary physical communication highway of the gut-brain axis. Research published in Frontiers in Psychiatry demonstrates that the vagus nerve modulates the brain-gut axis in both psychiatric and inflammatory disorders.
Approximately 80% of vagal fibers are afferent (carrying signals from gut to brain), meaning your gut sends far more information to your brain than the other way around. This explains why gut disturbances often manifest as mood changes before digestive symptoms become apparent.
Specialized enteroendocrine cells called "neuropods" in the gut lining detect nutrients, microbial metabolites, and immune signals, then transmit this information directly to the vagus nerve within milliseconds. Importantly, research shows that some beneficial gut bacteria like Lactobacillus rhamnosus do not produce anti-anxiety effects in animal models when the vagus nerve is severed — confirming the nerve's essential role.
How Do Gut Bacteria Produce Neurotransmitters?
Your gut microbiome is a neurotransmitter factory. The gut produces approximately 90% of the body's serotonin (the "happiness" neurotransmitter), about 50% of its dopamine (the "motivation" neurotransmitter), and significant quantities of GABA (the "calming" neurotransmitter). These neurochemicals are not merely confined to the gut — they signal through the vagus nerve and bloodstream to directly influence brain function.
Specific bacterial strains play distinct roles:
- Lactobacillus and Bifidobacterium species produce GABA, the primary inhibitory neurotransmitter that reduces anxiety
- Escherichia and Bacillus species produce dopamine and norepinephrine
- Enterochromaffin cells stimulated by microbial metabolites produce the majority of the body's serotonin
- Lactobacillus reuteri increases oxytocin levels, influencing social behavior and bonding
How Does the Immune System Mediate Gut-Brain Communication?
With approximately 70% of the body's immune cells residing in the gut-associated lymphoid tissue (GALT), the immune system serves as a critical intermediary in gut-brain signaling. When gut dysbiosis triggers immune activation, pro-inflammatory cytokines (like TNF-alpha, IL-6, and IL-1beta) can cross the blood-brain barrier and directly influence brain function.
This inflammatory pathway is increasingly recognized as a key mechanism in the "inflammatory subtype" of depression. A narrative review published in Science Direct confirms that the vagus nerve regulates a cholinergic anti-inflammatory pathway that attenuates inflammation and decreases intestinal permeability, which is directly relevant to depression.
What Role Do Short-Chain Fatty Acids Play?
When beneficial gut bacteria ferment dietary fiber, they produce short-chain fatty acids (SCFAs) — primarily butyrate, propionate, and acetate. These metabolites have far-reaching effects on brain health:
- Butyrate strengthens the blood-brain barrier and promotes BDNF (brain-derived neurotrophic factor) production, supporting neuroplasticity
- Propionate and acetate modulate appetite signaling and energy metabolism in the brain
- SCFAs collectively reduce neuroinflammation, support microglial function, and regulate the HPA axis stress response
Research shows that SCFA-producing bacteria like Lactobacillales and Ruminococcaceae are more abundant in individuals with better vagal function, creating a positive feedback loop between gut health and brain health.
What Are the Key Benefits of a Healthy Gut-Brain Axis?
A well-functioning gut-brain axis supports mental clarity, emotional resilience, stable mood, healthy stress responses, and cognitive performance. Research increasingly shows that optimizing gut-brain communication through diet, lifestyle, and targeted probiotics can produce measurable improvements in anxiety, depression symptoms, sleep quality, and overall psychological wellbeing.
Can a Healthy Gut Reduce Anxiety and Depression?
Emerging clinical evidence strongly suggests that gut health interventions can meaningfully reduce anxiety and depression symptoms. A 2026 article in Nature highlights that links between gut microbes and mental health could lead to large-scale clinical trials of probiotic interventions for these conditions. Multiple randomized controlled trials have shown that specific probiotic strains — particularly combinations of Lactobacillus helveticus R0052 and Bifidobacterium longum R0175 — reduce psychological distress, anxiety, and depression scores compared to placebo.
The mechanisms are multifaceted: probiotics reduce systemic inflammation, normalize HPA axis activity, increase serotonin availability, and strengthen the intestinal barrier to prevent endotoxin translocation. For those exploring natural approaches to anxiety, see our guide on mental wellness strategies.
Does Gut Health Affect Memory and Cognitive Function?
The gut-brain axis significantly influences cognitive function through several mechanisms. BDNF production — stimulated by SCFAs and certain probiotic strains — is essential for learning, memory formation, and neuroplasticity. Studies in PMC demonstrate that vagal nerve activity directly affects hippocampal-dependent memory processes. Additionally, chronic gut inflammation produces neuroinflammation that impairs executive function, attention, and processing speed — commonly experienced as "brain fog."
How Does the Gut-Brain Axis Influence Stress Resilience?
The HPA axis — the body's central stress response system — is intimately connected to gut health. Gut dysbiosis amplifies cortisol production and HPA axis reactivity, while a diverse, balanced microbiome helps modulate stress responses. Research shows that individuals with higher vagal tone (stronger vagus nerve activity) demonstrate greater emotional regulation, lower anxiety, and faster recovery from stressful events.
Can Gut Health Support Healthy Sleep Patterns?
The gut microbiome helps regulate circadian rhythm through its influence on melatonin and serotonin production. Since serotonin is the precursor to melatonin (the sleep hormone), and 90% of serotonin is produced in the gut, gut health directly impacts sleep quality. Studies show that gut dysbiosis is associated with insomnia, poor sleep architecture, and disrupted circadian rhythm. Optimizing the gut microbiome through diet and probiotics can improve sleep onset, duration, and quality.
What Happens When the Gut-Brain Axis Is Disrupted?
Gut-brain axis dysfunction occurs when gut dysbiosis, chronic inflammation, or impaired intestinal barrier function disrupts the normal communication between the gut and brain. This disruption has been linked to a range of mental health conditions including depression, anxiety disorders, autism spectrum disorders, ADHD, cognitive decline, and neurodegenerative diseases — though research is still emerging and causation is not fully established in many cases.
Mental Health Conditions Linked to Gut Dysbiosis
- Depression: Individuals with major depressive disorder consistently show altered gut microbiome composition, with reduced Lactobacillus and Bifidobacterium species and increased pro-inflammatory bacteria. A review in Frontiers in Behavioral Neuroscience confirms that specific measurable microbial markers have been identified in the feces of individuals with depression.
- Anxiety disorders: Gut dysbiosis amplifies HPA axis reactivity, increasing cortisol production and anxiety symptoms. Vagus nerve-mediated gut-brain signaling plays a central role.
- Autism spectrum disorders (ASD): Both children and adults with ASD frequently show chronic inflammation, gastrointestinal symptoms, and altered gut microbiome composition, typically with more Clostridium species and fewer Bifidobacterium.
- Cognitive decline and Alzheimer's: Gut-derived inflammation and reduced SCFA production may contribute to neurodegeneration and cognitive impairment through chronic neuroinflammation and blood-brain barrier breakdown.
Physical Symptoms of Gut-Brain Dysfunction
- Irritable bowel syndrome (IBS) and functional gastrointestinal disorders
- Chronic stress manifesting as digestive problems
- Brain fog and difficulty concentrating
- Anxiety-triggered digestive episodes
- Fatigue and low motivation
How Can You Strengthen Your Gut-Brain Axis?
Strengthening the gut-brain axis requires a multi-pronged approach targeting all four communication pathways: improving vagal tone through breathwork and meditation, diversifying the gut microbiome through diet, reducing systemic inflammation, and supporting neurotransmitter production with targeted nutrients and probiotics. A consistent 30-day protocol combining these strategies can produce noticeable improvements in both digestive and mental health.
Psychobiotics: Targeted Probiotics for Mental Health
Psychobiotics are a specific class of probiotics that have demonstrated the ability to influence brain function and mental health through the gut-brain axis. Key evidence-based strains include:
| Strain | Benefit | Mechanism |
|---|---|---|
| L. helveticus R0052 + B. longum R0175 | Anxiety and depression reduction | HPA axis modulation, cortisol reduction |
| L. rhamnosus JB-1 | Anxiety reduction, GABA production | Vagus nerve signaling, GABA receptor modulation |
| B. infantis 35624 | Depression, inflammation | Tryptophan metabolism, immune regulation |
| L. plantarum PS128 | Memory and cognition | Dopamine and serotonin modulation |
A narrative review in PMC confirms that psychobiotics have the potential to positively affect mental health by modulating the gut-brain axis, generating compounds that signal to the brain to enhance mood, cognition, and stress response.
30-Day Gut-Brain Healing Protocol
Week 1: Foundation
- Remove processed foods, refined sugar, and artificial additives
- Begin daily fermented food intake (1-2 tablespoons sauerkraut or kimchi)
- Start a symptom and mood journal
- Practice 5 minutes of deep breathing before each meal
Week 2: Rebuild
- Add prebiotic-rich foods daily (garlic, onions, asparagus, bananas)
- Begin a psychobiotic supplement
- Add 10 minutes of daily meditation or vagus nerve stimulation
- Increase omega-3 intake (fatty fish 3x weekly or supplement)
Week 3: Strengthen
- Increase fermented food variety (kefir, miso, kombucha)
- Add L-glutamine for gut lining support (5g daily)
- Increase exercise to 30 minutes of moderate activity 5 days per week
- Prioritize 7-9 hours of sleep with consistent bedtime
Week 4: Optimize
- Assess progress in mood, energy, digestion, and sleep
- Fine-tune supplement protocol based on results
- Establish long-term maintenance routine
- Consider comprehensive stool testing for personalized insights
Vagus Nerve Stimulation Techniques
- Deep diaphragmatic breathing: Slow, deep breaths with extended exhale (4 seconds in, 7 seconds out) directly stimulate the vagus nerve
- Cold water exposure: Splashing cold water on the face or ending showers with 30 seconds of cold water activates the vagal response
- Humming, singing, or gargling: Vibrations in the throat stimulate vagal fibers
- Meditation and yoga: Both increase vagal tone and are associated with improved gut-brain communication
What Diet and Lifestyle Changes Support the Gut-Brain Axis?
A Mediterranean-style diet rich in fermented foods, prebiotic fiber, omega-3 fatty acids, and polyphenol-rich plants provides the optimal nutritional foundation for gut-brain axis health. Combined with stress management, regular exercise, quality sleep, and social connection, these dietary strategies can meaningfully improve both digestive function and mental wellbeing within weeks.
Gut-Brain Axis Power Foods
- Fermented foods (daily): Raw sauerkraut, kimchi, kefir, yogurt with live cultures, miso, kombucha — increase microbial diversity and provide live beneficial bacteria. The Stanford fermented foods study showed these increase microbiome diversity and reduce inflammatory markers.
- Prebiotic fiber: Garlic, onions, leeks, asparagus, Jerusalem artichokes, under-ripe bananas, oats — feed SCFA-producing bacteria that support brain health
- Omega-3 fatty acids: Wild salmon, sardines, mackerel, walnuts, flaxseeds — reduce neuroinflammation and support both gut lining and brain cell membrane integrity
- Polyphenol-rich foods: Blueberries, dark chocolate, green tea, extra virgin olive oil, turmeric — support microbiome diversity and provide neuroprotective antioxidants
- Tryptophan-rich foods: Turkey, chicken, eggs, pumpkin seeds, tofu — provide the precursor for serotonin synthesis in the gut
- Bone broth and collagen: Support intestinal barrier integrity, reducing the "leaky gut" that drives neuroinflammation
Lifestyle Practices for Optimal Gut-Brain Health
- Stress management: Chronic stress damages the gut microbiome, increases intestinal permeability, and amplifies HPA axis reactivity. Daily meditation, yoga, or breathwork practice directly improves vagal tone and gut-brain communication.
- Exercise: Moderate exercise (30 minutes, 5 days weekly) increases microbiome diversity, boosts SCFA production, and stimulates BDNF release. Both aerobic exercise and resistance training show benefits.
- Sleep optimization: Aim for 7-9 hours of consistent sleep. The gut microbiome follows circadian patterns, and disrupted sleep leads to dysbiosis and impaired gut-brain signaling.
- Social connection: Emerging research suggests that social interaction positively influences the gut microbiome. Isolation and loneliness are associated with reduced microbial diversity.
- Nature exposure: Time spent in natural environments exposes you to environmental microbes that support microbiome diversity.
What Should You Do First to Improve Your Gut-Brain Connection?
Start with the two highest-impact, lowest-effort changes: add one serving of fermented food daily and practice 5 minutes of deep diaphragmatic breathing before your largest meal. These two habits address both the microbial and neural components of the gut-brain axis and can be implemented today with no special equipment or supplements.
Phase 1: Quick Wins (This Week)
- [ ] Add 1-2 tablespoons of raw sauerkraut or kimchi to one meal daily
- [ ] Practice 5 minutes of deep breathing before dinner (4 seconds in, 7 seconds out)
- [ ] Remove or reduce processed foods and refined sugar
- [ ] Start a brief daily mood and digestion journal
Phase 2: Build the Foundation (Weeks 2-3)
- [ ] Increase prebiotic food intake (garlic, onions, asparagus daily)
- [ ] Begin a psychobiotic probiotic supplement
- [ ] Add omega-3 rich foods 3 times per week (or begin supplementation)
- [ ] Establish a consistent sleep schedule (same bedtime and wake time)
- [ ] Begin 10-15 minutes of daily meditation or yoga
Phase 3: Optimize and Maintain (Weeks 4+)
- [ ] Diversify fermented food intake (rotate between different types)
- [ ] Add L-glutamine for gut lining support if needed
- [ ] Exercise 30 minutes, 5 days per week
- [ ] Review journal for patterns and adjust protocol accordingly
- [ ] Consider stool testing for personalized microbiome insights
References
- Carabotti, M., et al. (2015). The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems. Annals of Gastroenterology, 28(2), 203-209. Source
- Breit, S., et al. (2018). Vagus nerve as modulator of the brain-gut axis in psychiatric and inflammatory disorders. Frontiers in Psychiatry, 9, 44. Source
- Bonaz, B., et al. (2018). The vagus nerve at the interface of the microbiota-gut-brain axis. Frontiers in Neuroscience, 12, 49. Source
- Yano, J.M., et al. (2015). Indigenous bacteria from the gut microbiota regulate host serotonin biosynthesis. Cell, 161(2), 264-276. Source
- Cryan, J.F., et al. (2019). The microbiota-gut-brain axis. Physiological Reviews, 99(4), 1877-2013. Source
- Dinan, T.G. & Cryan, J.F. (2017). The microbiome-gut-brain axis in health and disease. Gastroenterology Clinics of North America, 46(1), 77-89. Source
- Messaoudi, M., et al. (2011). Assessment of psychotropic-like properties of a probiotic formulation (Lactobacillus helveticus R0052 and Bifidobacterium longum R0175) in rats and human subjects. British Journal of Nutrition, 105(5), 755-764. Source
- Bravo, J.A., et al. (2011). Ingestion of Lactobacillus strain regulates emotional behavior and central GABA receptor expression in a mouse via the vagus nerve. Proceedings of the National Academy of Sciences, 108(38), 16050-16055. Source
- Zheng, P., et al. (2016). Gut microbiome remodeling induces depressive-like behaviors through a pathway mediated by the host's metabolism. Molecular Psychiatry, 21(6), 786-796. Source
- Kelly, J.R., et al. (2016). Transferring the blues: Depression-associated gut microbiota induces neurobehavioural changes in the rat. Journal of Psychiatric Research, 82, 109-118. Source
- Wastyk, H.C., et al. (2021). Gut-microbiota-targeted diets modulate human immune status. Cell, 184(16), 4137-4153. Source
- Dalile, B., et al. (2019). The role of short-chain fatty acids in microbiota-gut-brain communication. Nature Reviews Gastroenterology & Hepatology, 16(8), 461-478. Source
Frequently asked questions
What is the gut-brain axis in simple terms?
The gut-brain axis is the two-way communication system between your digestive tract and your brain. It uses the vagus nerve, hormones, immune signals, and chemical messengers produced by gut bacteria to send information back and forth. This connection explains why digestive problems often accompany anxiety or depression, and why stress can cause stomach issues.
Is it true that 90% of serotonin is produced in the gut?
Yes, approximately 90% of the body's serotonin is produced by enterochromaffin cells in the gastrointestinal tract, stimulated in part by gut microbiome activity. While gut-produced serotonin does not directly cross the blood-brain barrier, it signals through the vagus nerve and influences brain serotonin systems indirectly through tryptophan metabolism and immune signaling.
Can probiotics really help with anxiety and depression?
Emerging clinical research shows promising results. Specific strains called "psychobiotics" — particularly Lactobacillus helveticus and Bifidobacterium longum — have reduced anxiety and depression scores in randomized controlled trials. However, probiotics should complement, not replace, professional mental health treatment, and not all probiotic strains have mental health benefits.
What is the vagus nerve and why is it important for gut-brain health?
The vagus nerve is the longest cranial nerve in the body, running from the brainstem to the abdomen. It serves as the primary physical highway of the gut-brain axis, carrying information bidirectionally between your gut and brain. About 80% of its fibers carry signals from gut to brain, which is why gut health has such a profound influence on mood, stress response, and cognition.
How long does it take to improve the gut-brain connection?
Dietary changes can begin shifting gut microbiome composition within 24-48 hours, and many people notice improvements in mood and digestion within 2-4 weeks of implementing gut-brain supportive habits. However, meaningful, lasting changes in microbiome diversity and mental health outcomes typically require 8-12 weeks of consistent dietary, supplement, and lifestyle interventions.
What foods are worst for the gut-brain axis?
Processed foods high in refined sugar, artificial sweeteners, emulsifiers, and industrial seed oils are the most damaging to gut-brain axis function. These foods promote gut dysbiosis, increase intestinal permeability, trigger systemic inflammation, and reduce microbial diversity — all of which impair gut-brain communication and have been associated with increased depression and anxiety risk.
Can gut problems cause brain fog?
Yes, brain fog is one of the most common symptoms of gut-brain axis dysfunction. When the intestinal barrier is compromised ("leaky gut"), inflammatory molecules enter the bloodstream and can cross the blood-brain barrier, causing neuroinflammation that impairs cognitive function, concentration, and mental clarity. Healing the gut often resolves brain fog within weeks.
What is the difference between probiotics and psychobiotics?
All psychobiotics are probiotics, but not all probiotics are psychobiotics. Psychobiotics are a specific subset of probiotic strains that have demonstrated the ability to influence brain function and mental health through the gut-brain axis. Examples include Lactobacillus rhamnosus JB-1 for anxiety and Bifidobacterium longum R0175 for depression.
Does exercise improve the gut-brain connection?
Yes, regular moderate exercise is one of the most effective ways to improve gut-brain axis function. Exercise increases gut microbiome diversity, boosts SCFA production, stimulates BDNF release for neuroplasticity, improves vagal tone, and reduces systemic inflammation. Even 30 minutes of moderate walking five times per week produces measurable benefits.
Can children benefit from gut-brain axis optimization?
Yes, the gut-brain axis is active from birth, and early microbiome development has lasting impacts on mental health. However, children's supplementation should always be guided by a pediatrician. Focus on whole foods — fermented foods, prebiotic fiber, omega-3s — and limiting processed foods and sugar, rather than supplements, for children.