inflammation
Reduce Inflammation Naturally: Complete Anti-Inflammatory Guide
Learn how to reduce chronic inflammation naturally with this evidence-based guide. Covers anti-inflammatory diet, supplements, lifestyle changes, and testing.
Here's something that caught me off guard when I first started digging into health research: the same biological process that heals a paper cut can also quietly destroy your joints, clog your arteries, and fog your brain. Inflammation is your body's first responder—brilliant in short bursts, devastating when it never shuts off.
Chronic inflammation has been called the "silent killer" for good reason. Unlike the redness and swelling of a sprained ankle, systemic low-grade inflammation operates below the threshold of obvious symptoms. You might feel it as persistent fatigue, stubborn weight gain, achy joints, or digestive issues that seem to have no clear cause. According to the NIH, chronic inflammation is now recognized as a major contributor to cardiovascular disease, type 2 diabetes, cancer, Alzheimer's, autoimmune disorders, and depression.
The encouraging news? Unlike many health challenges, chronic inflammation responds powerfully to lifestyle intervention. Research consistently shows that dietary changes, targeted supplements, stress management, quality sleep, and regular exercise can measurably reduce inflammatory markers—sometimes within weeks. A 2026 breakthrough from University College London even identified the body's built-in "off switch" for inflammation: fat-derived molecules called epoxy-oxylipins that naturally rein in immune cells driving chronic disease.
This guide covers everything you need to understand and fight inflammation naturally: what inflammation actually is, how chronic inflammation develops, which diseases it drives, how to test for it, and a comprehensive anti-inflammatory protocol covering diet, supplements, lifestyle, and gut health optimization. Whether you're dealing with an autoimmune condition, chronic pain, or simply want to protect your long-term health, reducing inflammation is one of the highest-leverage steps you can take.
- Acute inflammation is protective and heals injuries; chronic inflammation is a low-grade, persistent immune response that damages healthy tissue and drives most chronic diseases.
- Chronic inflammation is linked to cardiovascular disease, type 2 diabetes, cancer, Alzheimer's, autoimmune conditions, depression, obesity, and arthritis.
- Key inflammatory biomarkers include CRP (C-reactive protein), ESR, IL-6, and TNF-alpha—simple blood tests can reveal your inflammation levels.
- The anti-inflammatory diet emphasizes omega-3 fatty acids, colorful vegetables and fruits, turmeric, ginger, olive oil, and green tea while eliminating refined sugar, processed foods, and trans fats.
- Omega-3 fatty acids (2–4g EPA/DHA daily) consistently reduce inflammatory markers like CRP in clinical meta-analyses.
- Curcumin (turmeric extract) shows positive effects on inflammatory markers, blood pressure, lipid profiles, and pain conditions across 25+ meta-analyses.
- Gut health is foundational: 70% of immune function resides in the gut, and dysbiosis directly promotes systemic inflammation.
- Lifestyle factors—sleep (7–9 hours), exercise (150 min/week moderate), stress management, and weight optimization—are as important as diet for reducing inflammation.
- Most people can measurably reduce CRP levels within 4–8 weeks of consistent anti-inflammatory dietary and lifestyle changes.
- Chronic inflammation often progresses silently for years before manifesting as disease—proactive testing and prevention are critical.
What Is Inflammation and Why Should You Care About It?
Inflammation is your immune system's response to injury, infection, or harmful stimuli—a complex cascade of white blood cells, cytokines, and other molecules that rush to the affected area to neutralize threats and begin repair. In its acute form, it's essential for survival. In its chronic form, it becomes the root driver of most modern diseases.
There are two fundamentally different types:
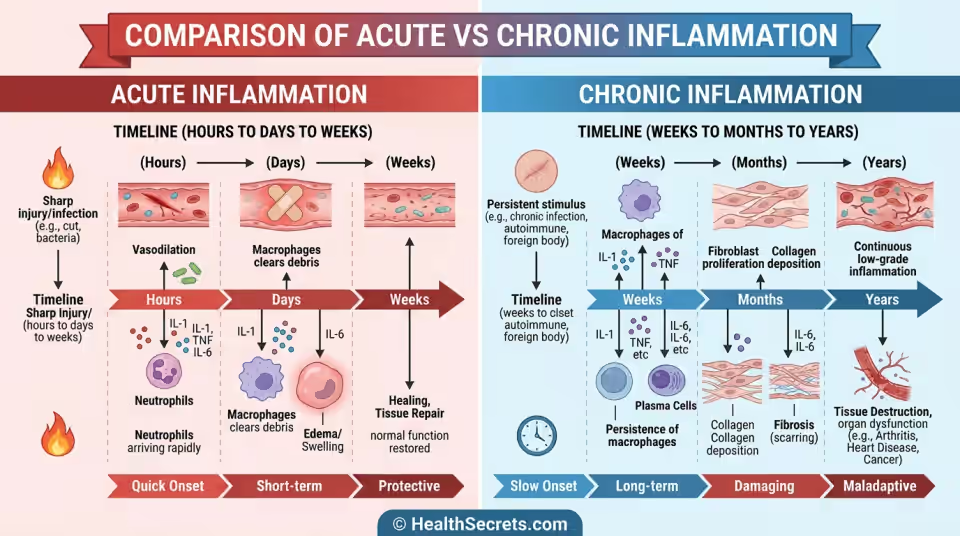
Acute inflammation is the familiar redness, warmth, swelling, and pain that follows an injury or infection. It's targeted, time-limited (days to weeks), and resolves once the threat is eliminated. This is inflammation doing exactly what it should.
Chronic inflammation is a low-grade, systemic immune activation that persists for months or years. Unlike acute inflammation, it often produces no obvious symptoms—or symptoms so vague (fatigue, brain fog, joint stiffness) that they're dismissed as "normal aging." The immune system stays partially activated, releasing inflammatory molecules like IL-6, TNF-alpha, and C-reactive protein into the bloodstream, gradually damaging blood vessels, joints, organs, and brain tissue.
| Feature | Acute Inflammation | Chronic Inflammation |
|---|---|---|
| Trigger | Injury, infection, burns | Poor diet, stress, obesity, toxins |
| Duration | Days to weeks | Months to years |
| Purpose | Protective and healing | Damaging and disease-causing |
| Symptoms | Redness, swelling, heat, pain | Fatigue, pain, brain fog, weight gain |
| Health Impact | Beneficial (resolves) | Harmful (progressive damage) |
The StatPearls medical reference notes that chronic inflammation "is the cause of most chronic diseases and presents a major threat to the health and longevity of individuals."
How Does the Inflammatory Response Actually Work in Your Body?
The inflammatory response is a coordinated immune cascade involving multiple cell types, signaling molecules, and feedback loops. Understanding these mechanisms helps explain why chronic inflammation is so damaging—and why certain interventions work to reduce it.
When tissue damage or pathogens are detected, damaged cells release chemical signals (histamine, prostaglandins, bradykinin) that trigger vasodilation—widening blood vessels to increase blood flow to the area. This causes the characteristic redness and warmth. Increased vascular permeability allows white blood cells (neutrophils first, then monocytes/macrophages) to migrate from the bloodstream into the affected tissue.
What Are the Key Inflammatory Molecules?
- Cytokines — Signaling proteins that coordinate the immune response. Pro-inflammatory cytokines (IL-1, IL-6, TNF-alpha) amplify inflammation; anti-inflammatory cytokines (IL-10, TGF-beta) resolve it.
- Prostaglandins — Lipid compounds that promote inflammation, pain, and fever. NSAIDs work by blocking prostaglandin synthesis.
- C-reactive protein (CRP) — Produced by the liver in response to IL-6. Elevated CRP is the most commonly used biomarker for systemic inflammation.
- NF-kB (Nuclear Factor kappa B) — A master transcription factor that controls expression of hundreds of inflammatory genes. Most anti-inflammatory compounds (curcumin, omega-3s, resveratrol) work partly by inhibiting NF-kB.
How Does Acute Inflammation Become Chronic?
Chronic inflammation develops when the resolution phase fails. Normally, once a threat is neutralized, the immune system switches from pro-inflammatory to pro-resolving mode, releasing specialized pro-resolving mediators (SPMs) derived from omega-3 fatty acids. The 2026 UCL discovery of epoxy-oxylipins as a natural inflammation "off switch" adds another piece to this puzzle.
When resolution fails—due to persistent triggers (poor diet, obesity, chronic stress, gut dysbiosis, environmental toxins)—the immune system remains partially activated. Macrophages continue releasing pro-inflammatory cytokines, creating a self-perpetuating cycle of tissue damage and immune activation.
What Causes Chronic Inflammation to Develop?
Chronic inflammation rarely has a single cause—it's typically the result of multiple overlapping factors that keep the immune system in a state of low-grade activation. Identifying and addressing your personal triggers is the foundation of any effective anti-inflammatory strategy.
Dietary Triggers
- Refined sugar and high-fructose corn syrup — Stimulate production of inflammatory cytokines, increase CRP levels, promote insulin resistance
- Trans fats and industrial seed oils — Promote NF-kB activation and oxidative stress; excessive omega-6 to omega-3 ratio drives inflammation
- Ultra-processed foods — Contain emulsifiers, preservatives, and artificial additives that damage the gut lining and alter the microbiome
- Refined carbohydrates — Spike blood sugar, trigger insulin release, promote advanced glycation end products (AGEs)
- Excessive alcohol — Damages gut barrier, increases endotoxin absorption, promotes liver inflammation
- Processed meats — Contain AGEs, nitrates, and saturated fats associated with elevated inflammatory markers
Lifestyle Triggers
- Chronic stress — Cortisol dysregulation eventually increases pro-inflammatory cytokine production
- Sleep deprivation — Even one night of poor sleep elevates CRP and IL-6; chronic sleep debt dramatically increases inflammatory burden
- Sedentary behavior — Lack of movement reduces anti-inflammatory myokines released by contracting muscles
- Obesity — Adipose tissue (especially visceral fat) actively secretes inflammatory cytokines (adipokines), making obesity both a cause and consequence of chronic inflammation
Medical and Environmental Triggers
- Gut dysbiosis and leaky gut — A compromised intestinal barrier allows bacterial endotoxins (LPS) into the bloodstream, triggering systemic immune activation
- Chronic infections — Low-grade viral or bacterial infections maintain immune activation
- Environmental toxins — Pesticides, heavy metals, air pollution, and endocrine disruptors promote oxidative stress and inflammation
- Autoimmune conditions — Mistaken immune targeting of healthy tissue creates persistent inflammation
What Are the Signs and Symptoms of Chronic Inflammation?
Chronic inflammation often progresses silently for years. When symptoms do appear, they're frequently vague enough to be attributed to "getting older" or "stress."
Common Symptoms
- Persistent fatigue — Feeling tired despite adequate sleep; energy that crashes mid-afternoon
- Body and joint pain — Widespread achiness, morning stiffness, joint swelling without clear injury
- Digestive issues — Bloating, gas, diarrhea, constipation, or food sensitivities
- Skin problems — Eczema, psoriasis, acne, rashes, or premature aging
- Frequent infections — Catching every cold, slow wound healing
- Mood disturbances — Depression, anxiety, irritability, brain fog, difficulty concentrating
- Weight gain — Especially visceral (belly) fat that resists diet and exercise
- Elevated blood sugar — Insulin resistance, prediabetes
Diseases Driven by Chronic Inflammation
- Cardiovascular disease — Inflammation damages arterial walls, promotes plaque formation and rupture
- Type 2 diabetes — Inflammatory cytokines impair insulin signaling
- Cancer — Chronic inflammation creates an environment that promotes tumor growth and metastasis
- Alzheimer's and dementia — Neuroinflammation accelerates cognitive decline
- Autoimmune diseases — Rheumatoid arthritis, lupus, Hashimoto's, psoriasis, MS
- Inflammatory bowel disease — Crohn's disease, ulcerative colitis
- Depression and anxiety — Inflammatory cytokines cross the blood-brain barrier and alter neurotransmitter function
- Obesity — Bidirectional: inflammation promotes weight gain, excess fat promotes inflammation
What Are the Best Evidence-Based Strategies for Reducing Inflammation?
The most effective anti-inflammatory approach combines dietary optimization, targeted supplementation, lifestyle modification, and gut health restoration. These strategies work synergistically—combining all four produces results that far exceed any single intervention.
The Five Pillars of Anti-Inflammatory Living
- Anti-inflammatory diet — Eliminate pro-inflammatory foods, emphasize omega-3s, polyphenols, fiber, and antioxidants
- Targeted supplements — Omega-3 fish oil, curcumin, ginger, boswellia, vitamin D
- Gut health optimization — Restore barrier integrity, increase microbial diversity, support beneficial bacteria
- Lifestyle modification — Regular exercise, quality sleep, stress management, weight optimization
- Toxin reduction — Clean eating, filtered water, reducing chemical exposure
Testing Your Inflammation Levels
Before starting an anti-inflammatory protocol, establish your baseline with these tests:
- hs-CRP (high-sensitivity C-reactive protein) — The gold standard marker for systemic inflammation. Optimal: <1.0 mg/L. Moderate risk: 1.0–3.0. High risk: >3.0.
- ESR (erythrocyte sedimentation rate) — Measures how quickly red blood cells settle; elevated in inflammatory conditions.
- Omega-3 Index — Measures EPA+DHA as a percentage of total red blood cell fatty acids. Target: >8% (cardioprotective).
- Fasting insulin and HbA1c — Markers of metabolic inflammation and insulin resistance.
- IL-6 and TNF-alpha — More specific inflammatory cytokine panels (specialty labs).
Retest at 8–12 weeks to track progress objectively.
What Should You Eat (and Avoid) to Fight Inflammation?
Diet is the single most impactful lever for controlling chronic inflammation. The Mediterranean diet pattern—rich in omega-3 fatty acids, colorful vegetables, olive oil, nuts, and moderate fish—has the strongest evidence base for reducing inflammatory markers and preventing inflammatory diseases.
Anti-Inflammatory Foods to Emphasize
Omega-3 rich foods:
- Fatty fish (salmon, sardines, mackerel, herring) — 2–3 servings per week minimum
- Walnuts, flaxseeds, chia seeds, hemp seeds
- Fish oil or algae-based omega-3 supplements
Colorful vegetables and fruits (antioxidants + polyphenols):
- Berries (blueberries, strawberries, cherries — rich in anthocyanins)
- Leafy greens (spinach, kale, Swiss chard — rich in lutein, zeaxanthin)
- Cruciferous vegetables (broccoli, cauliflower — sulforaphane)
- Tomatoes (lycopene), bell peppers (vitamin C)
Anti-inflammatory spices and herbs:
- Turmeric (curcumin) — Inhibits NF-kB, COX-2, and multiple inflammatory pathways
- Ginger — Reduces prostaglandin synthesis, inhibits TNF-alpha
- Rosemary, oregano, cinnamon — Potent antioxidant and anti-inflammatory compounds
Healthy fats:
- Extra-virgin olive oil — Contains oleocanthal (natural anti-inflammatory similar to ibuprofen)
- Avocados — Monounsaturated fats plus anti-inflammatory carotenoids
- Nuts (almonds, walnuts, Brazil nuts) — Vitamin E, selenium, healthy fats
Other powerful anti-inflammatory foods:
- Green tea — EGCG catechins reduce inflammatory markers
- Dark chocolate (70%+) — Flavanols with anti-inflammatory properties
- Bone broth — Glycine and proline support gut lining repair
- Fermented foods — Support gut health and reduce systemic inflammation
Pro-Inflammatory Foods to Eliminate
| Food Category | Inflammatory Mechanism | Swap With |
|---|---|---|
| Refined sugar | Spikes insulin, increases CRP and IL-6 | Whole fruits, raw honey (moderation) |
| Trans fats / seed oils | Activates NF-kB, promotes oxidative stress | Extra-virgin olive oil, avocado oil |
| Processed meats | AGEs, nitrates, saturated fats increase inflammation | Wild-caught fish, organic poultry |
| Refined carbs | Blood sugar spikes, AGE formation | Whole grains, sweet potatoes, legumes |
| Excessive alcohol | Damages gut barrier, liver inflammation | Green tea, sparkling water with lemon |
Anti-Inflammatory Supplements: What the Evidence Shows
| Supplement | Active Compounds | Evidence Level | Dosage | Best For |
|---|---|---|---|---|
| Omega-3 Fish Oil | EPA + DHA | Strong (multiple meta-analyses) | 2–4g EPA/DHA daily | Systemic inflammation, cardiovascular |
| Curcumin | Curcuminoids | Strong (25+ meta-analyses) | 500–1,000mg with piperine | Joint pain, inflammatory markers |
| Ginger | Gingerols, shogaols | Moderate-Strong | 1–2g daily | Pain, nausea, digestive inflammation |
| Boswellia | Boswellic acids (AKBA) | Moderate (RCTs for joints) | 300–500mg daily | Joint pain, arthritis, IBD |
| Vitamin D | Cholecalciferol | Strong (immune regulation) | 2,000–4,000 IU daily | Immune balance, deficiency |
What Lifestyle Changes Most Effectively Reduce Inflammation?
Diet gets the most attention, but lifestyle factors—particularly exercise, sleep, stress management, and weight optimization—are equally powerful anti-inflammatory interventions. Neglecting these while perfecting your diet is like building half a bridge.
How Does Exercise Reduce Inflammation?
Contracting muscles release anti-inflammatory molecules called myokines (particularly IL-6 in its anti-inflammatory form and IL-10) that counterbalance chronic inflammation. Regular moderate exercise:
- Reduces CRP levels by 20–30% within 8–12 weeks
- Decreases visceral fat (a major source of inflammatory cytokines)
- Improves insulin sensitivity
- Enhances immune regulation
Recommended protocol: 150 minutes moderate aerobic activity per week + 2 strength training sessions. Zone 2 cardio (conversational pace) is particularly effective for reducing inflammatory markers without the transient inflammation spike of extreme exercise.
Why Is Sleep the Most Underrated Anti-Inflammatory?
Even a single night of sleep deprivation (less than 6 hours) significantly elevates CRP and IL-6. Chronic sleep debt creates a compounding inflammatory burden.
Anti-inflammatory sleep protocol:
- 7–9 hours consistently (same wake time daily)
- Dark, cool room (65–68°F)
- No screens 60 minutes before bed
- Avoid caffeine after 2 PM
- Consider magnesium glycinate (200–400mg) before bed
How Does Stress Management Lower Inflammation?
Chronic psychological stress dysregulates the HPA axis, eventually leading to cortisol resistance and increased pro-inflammatory cytokine production. Effective practices:
- Meditation or breathwork — 10–20 minutes daily reduces CRP and cortisol
- Yoga — Combines movement with stress reduction; reduces IL-6 and TNF-alpha
- Nature exposure — Forest bathing (shinrin-yoku) measurably reduces inflammatory markers
- Social connection — Loneliness increases inflammation; meaningful relationships reduce it
Weight Optimization
Visceral adipose tissue is an active endocrine organ that secretes inflammatory adipokines (leptin, resistin, TNF-alpha). Losing even 5–10% of body weight significantly reduces systemic inflammatory markers. The anti-inflammatory diet and exercise protocol naturally supports healthy weight loss.
Which Supplements Have the Strongest Evidence for Reducing Inflammation?
Targeted supplementation can significantly accelerate inflammation reduction when combined with dietary and lifestyle changes. These are the supplements with the most robust clinical evidence.
Omega-3 Fatty Acids (EPA + DHA)
The most well-studied anti-inflammatory supplement. EPA and DHA reduce pro-inflammatory cytokine production, inhibit NF-kB, and serve as precursors for specialized pro-resolving mediators (SPMs)—the molecules your body uses to actively resolve inflammation. Doses of 2–4g/day EPA/DHA show CRP reductions in multiple meta-analyses.
Curcumin (Turmeric Extract)
A 2026 umbrella review of 25 meta-analyses found curcumin has positive effects on inflammatory markers, blood pressure, lipid profiles, musculoskeletal conditions, and cognitive function. Curcumin inhibits NF-kB, COX-2, and LOX pathways simultaneously.
:::warning[Safety Warning] Standard curcumin has poor bioavailability—use formulations with piperine (black pepper extract), phospholipid complexes (Meriva), or nano-formulations for effective absorption. :::
Boswellia Serrata
Boswellic acids (particularly AKBA) inhibit 5-lipoxygenase, reducing leukotriene production. A 2026 randomized, double-blind, placebo-controlled trial demonstrated that Boswellia extract with enhanced bioavailability, combined with curcumin, significantly reduced pain and stiffness in spondylitis patients. Particularly effective for joint inflammation, arthritis, and inflammatory bowel conditions.
Ginger
Gingerols and shogaols inhibit prostaglandin synthesis and TNF-alpha production. Clinical trials support ginger for osteoarthritis pain, exercise-induced inflammation, and digestive inflammation. Well-tolerated at 1–2g daily.
Vitamin D
Vitamin D deficiency is strongly associated with elevated inflammatory markers. Vitamin D modulates immune function, shifting T-cells toward anti-inflammatory regulatory phenotypes.
Dosing: 2,000–4,000 IU daily to maintain blood levels of 40–60 ng/mL. Test levels before supplementing.
Resveratrol
Polyphenol found in red grapes, berries, and peanuts. Activates SIRT1 (sirtuin pathway), inhibits NF-kB, and reduces oxidative stress.
Dosing: 150–500mg trans-resveratrol daily. Bioavailability is limited—pterostilbene may be a more bioavailable alternative.
How Do You Start an Anti-Inflammatory Protocol?
This phased approach allows your body to adapt gradually while maximizing results. Most people notice measurable improvements in energy, pain levels, and cognitive clarity within 2–4 weeks, with significant biomarker improvements by 8–12 weeks.
Phase 1: Foundation (Weeks 1–2) — Remove Inflammatory Triggers
- [ ] Eliminate refined sugar, processed foods, trans fats, and excessive alcohol
- [ ] Switch cooking oils to extra-virgin olive oil and avocado oil
- [ ] Replace processed meats with wild-caught fish (2–3x/week)
- [ ] Increase vegetable intake to 5+ servings daily (emphasize colorful variety)
- [ ] Begin daily turmeric use (cooking or golden milk)
- [ ] Start sleep optimization: consistent schedule, dark room, no late screens
- [ ] Begin 10 minutes daily stress management (meditation, breathwork)
Phase 2: Rebuild (Weeks 3–4) — Add Anti-Inflammatory Support
- [ ] Start omega-3 fish oil: 2–3g EPA/DHA daily with meals
- [ ] Start curcumin: 500–1,000mg daily with piperine or enhanced bioavailability formula
- [ ] Start vitamin D: 2,000–4,000 IU daily (test levels first if possible)
- [ ] Add fermented foods daily for gut health support
- [ ] Begin exercise protocol: 30 minutes moderate activity most days
- [ ] Increase hydration: 8+ glasses filtered water daily
Phase 3: Optimize (Weeks 5–8) — Fine-Tune and Track
- [ ] Add boswellia if joint pain is a primary concern: 300–500mg daily
- [ ] Add ginger: 1–2g daily or fresh ginger in cooking/tea
- [ ] Increase exercise to 150+ minutes moderate aerobic + 2 strength sessions weekly
- [ ] Deepen stress management: 20 minutes daily, add yoga or nature walks
- [ ] Consider adding magnesium glycinate (200–400mg) for sleep and muscle relaxation
- [ ] Track symptoms: energy, pain levels, sleep quality, digestion, mood
Phase 4: Maintain and Monitor (Week 9+)
- [ ] Retest hs-CRP and other biomarkers at 12 weeks
- [ ] Maintain anti-inflammatory diet (80/20 approach)
- [ ] Continue core supplements (omega-3, curcumin, vitamin D)
- [ ] Adjust protocol based on biomarker results
- [ ] Annual inflammation panel for ongoing monitoring
What Should You Do First to Start Reducing Inflammation?
Start with the changes that have the highest impact for the least effort, then build from there. Trying to overhaul everything simultaneously leads to burnout.
This Week (Days 1–7):
- [ ] Remove refined sugar, processed foods, and seed oils from your kitchen
- [ ] Stock up on anti-inflammatory staples: olive oil, salmon, berries, leafy greens, turmeric
- [ ] Start 10 minutes daily breathwork or meditation
- [ ] Set a consistent sleep schedule (same wake time every day)
- [ ] Schedule hs-CRP and vitamin D blood tests with your doctor
Next Week (Days 8–14):
- [ ] Start omega-3 fish oil (2–3g EPA/DHA daily)
- [ ] Start curcumin supplement (500mg with piperine)
- [ ] Begin 30 minutes moderate exercise 4–5 days per week
- [ ] Add 2–3 servings of fatty fish per week
Weeks 3–4:
- [ ] Start vitamin D if levels are below 40 ng/mL
- [ ] Add fermented foods daily for gut health
- [ ] Increase plant diversity to 30+ different plants per week
- [ ] Evaluate progress: symptoms, energy, pain levels
Ongoing:
- [ ] Maintain 80/20 anti-inflammatory diet
- [ ] Continue core supplement stack
- [ ] Retest biomarkers every 3–6 months
- [ ] Adjust based on results and symptoms
References
- Cleveland Clinic, 2024. What Is Inflammation? Types, Causes & Treatment. Source
- StatPearls (NCBI Bookshelf), 2024. Chronic Inflammation. Source
- University College London / ScienceDaily, 2026. Scientists Discover the Body's Hidden "Off Switch" for Inflammation. Source
- Mayo Clinic Press, 2024. Chronic Inflammation: What It Is, Why It's Bad, and How You Can Reduce It. Source
- Ruscio, M., 2025. The 11 Best Anti-Inflammatory Supplements. Dr. Ruscio. Source
- Ayub, A. et al., 2024. On the Health Effects of Curcumin and Its Derivatives. Food Science & Nutrition. Source
- PMC, 2025. Curcumin and Multiple Health Outcomes: Critical Umbrella Review of Intervention Meta-Analyses. Source
- Mamatha, K. et al., 2025. Boswellia Serrata Extract with Enhanced Bioavailability Alleviates Pain and Stiffness in Spondylitis. Frontiers in Pharmacology. Source
- NIH Office of Dietary Supplements, 2024. Omega-3 Fatty Acids—Health Professional Fact Sheet. Source
- Hopkins Medicine, 2024. Anti-Inflammatory Diet. Source
- Healthline, 2024. 10 Supplements That Fight Inflammation. Source
- Frontiers in Nutrition, 2024. Turmeric: From Spice to Cure—Anti-Cancer, Radioprotective and Anti-Inflammatory Effects. Source
Frequently asked questions
How long does it take to reduce chronic inflammation?
Most people see measurable improvements in energy and symptoms within 2–4 weeks of consistent anti-inflammatory dietary and lifestyle changes. CRP levels typically begin dropping within 4–8 weeks, with significant reductions by 12 weeks. However, long-standing inflammation from autoimmune conditions or obesity may take 3–6 months for meaningful biomarker improvements.
What is the best test for measuring inflammation?
High-sensitivity C-reactive protein (hs-CRP) is the gold standard blood test for systemic inflammation. It's inexpensive, widely available, and correlates well with cardiovascular risk. Optimal is below 1.0 mg/L. For a more complete picture, combine hs-CRP with ESR, fasting insulin, and an omega-3 index test. Your doctor can order these as part of routine bloodwork.
Can you completely cure chronic inflammation?
In many cases, yes—if the underlying triggers are identified and addressed. Diet-driven and lifestyle-driven chronic inflammation can often be fully resolved with sustained changes. Inflammation from autoimmune conditions may not be "cured" but can be significantly reduced and managed. The goal is to remove triggers, support resolution pathways, and maintain anti-inflammatory habits long-term.
Is ibuprofen good for chronic inflammation?
NSAIDs like ibuprofen effectively reduce acute inflammation but are not recommended for chronic use. Regular NSAID use damages the gut lining, increases intestinal permeability (which actually promotes more inflammation), and carries cardiovascular and kidney risks. Natural alternatives like curcumin, omega-3s, and boswellia address chronic inflammation without these side effects.
Which diet is best for reducing inflammation?
The Mediterranean diet has the strongest evidence for reducing inflammatory markers. It emphasizes fatty fish, olive oil, vegetables, fruits, nuts, legumes, and whole grains while minimizing processed foods, sugar, and red meat. Studies consistently show Mediterranean diet adherence reduces CRP, IL-6, and other inflammatory biomarkers.
Does sugar really cause inflammation?
Yes. Refined sugar and high-fructose corn syrup directly stimulate production of pro-inflammatory cytokines, increase CRP levels, promote insulin resistance, and feed pathogenic gut bacteria that drive further inflammation. Reducing added sugar is one of the single most impactful anti-inflammatory dietary changes you can make.
Can exercise reduce inflammation?
Absolutely. Regular moderate exercise reduces CRP by 20–30% within 8–12 weeks. Contracting muscles release anti-inflammatory myokines (IL-6 in its anti-inflammatory form, IL-10) that counterbalance chronic inflammation. Exercise also reduces visceral fat (a major inflammation source), improves insulin sensitivity, and enhances immune regulation. The key is consistency—150 minutes of moderate activity per week.
Is gut health connected to inflammation?
Profoundly. About 70% of immune function resides in the gut. A compromised intestinal barrier ("leaky gut") allows bacterial endotoxins into the bloodstream, triggering systemic immune activation. Gut dysbiosis—an imbalance favoring harmful bacteria—directly promotes inflammatory cytokine production. Restoring gut health through probiotics, prebiotics, and barrier repair is one of the most effective anti-inflammatory strategies.
Can stress cause inflammation?
Yes. Chronic psychological stress dysregulates the hypothalamic-pituitary-adrenal (HPA) axis, eventually leading to cortisol resistance. When cortisol can no longer suppress inflammation effectively, pro-inflammatory cytokine production increases. Studies show that chronic stress significantly elevates CRP, IL-6, and TNF-alpha. Meditation, breathwork, yoga, and nature exposure measurably reduce stress-driven inflammation.
How much omega-3 do you need to reduce inflammation?
Clinical meta-analyses show that 2–4g combined EPA/DHA daily produces significant reductions in inflammatory markers including CRP. For general maintenance, 1–2g daily is sufficient. For active inflammation reduction, aim for the higher end (3–4g). Triglyceride-form fish oil is approximately 50% better absorbed than ethyl ester forms.