immune system
Stress and Immune System: How Chronic Stress Weakens Immunity
Learn how chronic stress suppresses your immune system through cortisol and psychoneuroimmunology. Discover proven stress management techniques to protect immunity.
You eat well, exercise regularly, and take your vitamins — yet you still catch every cold that comes around the office. The missing piece might not be what you're putting into your body, but what's happening inside your mind. Chronic stress silently erodes your immune defenses, making you vulnerable to infections, slowing wound healing, and even reducing the effectiveness of vaccines.
The science behind this connection is called psychoneuroimmunology — the study of how your thoughts, nervous system, and immune cells communicate in a constant, bidirectional dialogue. When stress becomes chronic, this conversation turns toxic, flooding your body with cortisol and inflammatory signals that leave your immune system weakened and dysregulated.
But here's the good news: just as stress can suppress immunity, proven stress management techniques can restore it. Research shows that meditation, deep breathing, social connection, and targeted supplements can measurably improve immune markers — sometimes in as little as eight weeks.
Learn more about how lifestyle factors shape your immune defenses in our guides on boosting your immune system naturally, sleep and immune function, and exercise and immunity.
- Chronic stress suppresses immune function by elevating cortisol, reducing T cell activity, lowering antibody production, and increasing systemic inflammation
- Acute (short-term) stress can temporarily enhance immunity, but chronic stress lasting weeks or months causes progressive immune dysregulation
- Stressed individuals are 2–3 times more likely to develop upper respiratory infections and may produce up to 50% fewer antibodies in response to vaccines
- Psychoneuroimmunology research confirms that the brain, nervous system, and immune system communicate bidirectionally through the HPA axis, vagus nerve, and cytokine signaling
- Mindfulness meditation practiced for 8 weeks has been shown to increase antibody response to flu vaccines and reduce inflammatory cytokines
- Adaptogens like ashwagandha can reduce cortisol levels by up to 30% in clinical studies, supporting both stress resilience and immune function
- The gut-brain axis links stress to gut microbiome disruption, compromising the 70% of immune tissue located in the digestive tract
- Building a daily stress management practice — even 10–20 minutes of deep breathing or meditation — can measurably improve immune markers over time
What Is the Stress-Immune Connection and Why Does It Matter?
The stress-immune connection refers to the scientifically documented relationship between psychological stress and immune system function, mediated by hormones, neurotransmitters, and inflammatory signaling molecules. Chronic stress activates the hypothalamic-pituitary-adrenal (HPA) axis, elevating cortisol levels that directly suppress immune cell production and function. This connection explains why people under prolonged stress get sick more often and recover more slowly.
How Does Your Body Respond to Stress?
When your brain perceives a threat — whether a charging predator or a looming work deadline — the amygdala triggers a cascade of physiological changes designed for short-term survival:
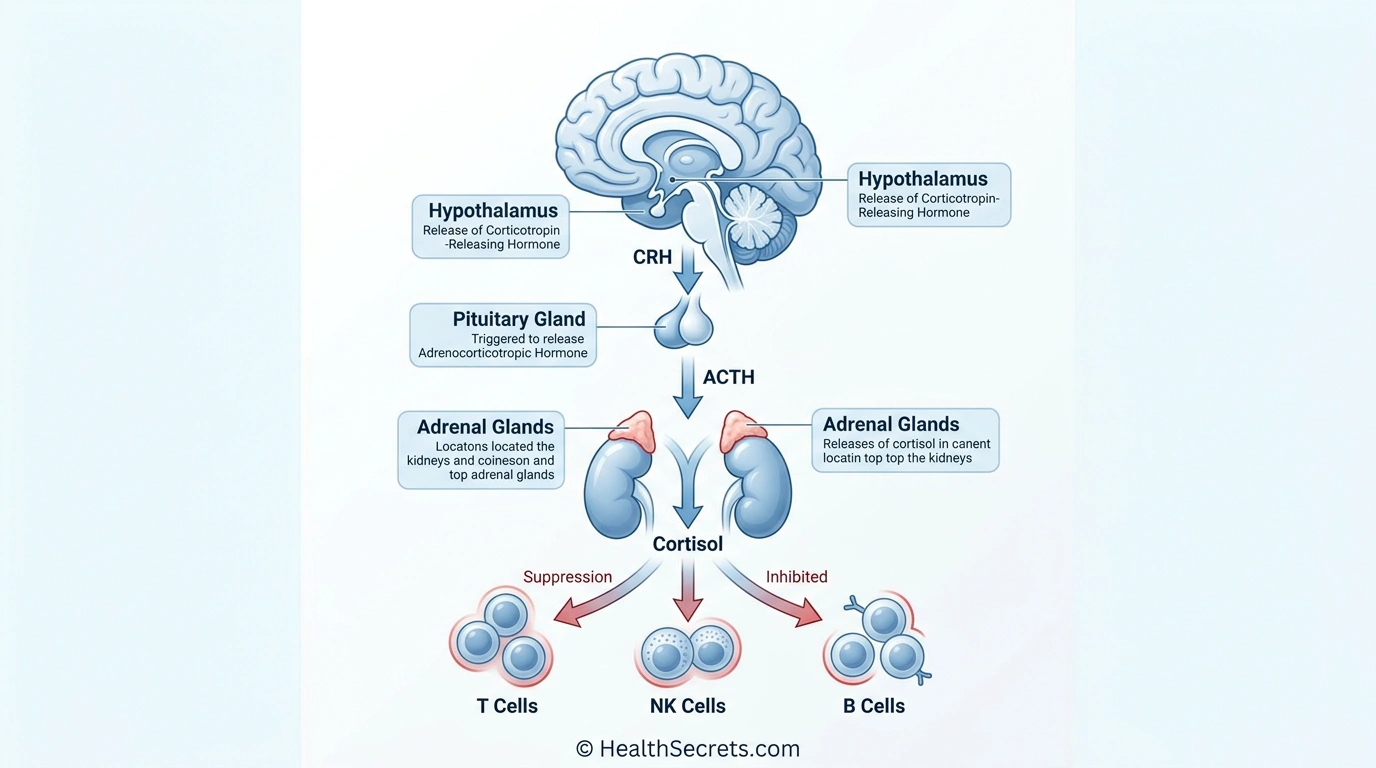
- Hypothalamus releases corticotropin-releasing hormone (CRH)
- Pituitary gland releases adrenocorticotropic hormone (ACTH)
- Adrenal glands release cortisol and adrenaline
- Heart rate, blood pressure, and alertness increase
- Energy is mobilized, digestion slows, and immune function shifts
This "fight-or-flight" response evolved for acute threats lasting minutes to hours. The problem arises when modern stressors — financial worries, relationship problems, work pressure, information overload — keep this system activated for weeks, months, or years.
What Is Psychoneuroimmunology?
Psychoneuroimmunology (PNI) is the interdisciplinary field studying the interactions between psychological processes, the nervous system, and the immune system. PNI research has revealed that immune cells carry receptors for stress hormones, neurotransmitters communicate directly with immune organs, and psychological interventions can measurably change immune biomarkers. The field demonstrates that mind and body are not separate systems but deeply interconnected networks.
| Factor | Acute Stress | Chronic Stress | Immune Impact |
|---|---|---|---|
| Duration | Minutes to hours | Weeks to years | Short vs. prolonged immune changes |
| Cortisol | Brief spike, returns to baseline | Persistently elevated | Temporary enhancement vs. chronic suppression |
| Immune Cells | Mobilized to tissues | Production reduced | Enhanced surveillance vs. depleted defenses |
| Inflammation | Controlled, protective | Chronic low-grade | Healing response vs. tissue damage |
| Overall Effect | Can enhance immunity | Suppresses immunity | Adaptive vs. maladaptive |
How Does Chronic Stress Suppress Your Immune System?
Chronic stress suppresses immunity primarily through sustained cortisol elevation, which reduces lymphocyte production, impairs T cell and Natural Killer cell function, decreases antibody output, and disrupts the balance between pro-inflammatory and anti-inflammatory cytokines. The HPA axis, sympathetic nervous system, and vagus nerve serve as the communication highways between your brain and immune organs.
What Does Cortisol Do to Immune Cells?
Cortisol — your primary stress hormone — has profound effects on virtually every immune cell type:
- T cells: Reduced proliferation and impaired cellular immunity, weakening defense against viruses and intracellular pathogens
- B cells: Decreased antibody production, particularly secretory IgA that protects mucosal surfaces in the respiratory and GI tracts
- Natural Killer cells: Suppressed activity, reducing the body's ability to kill virus-infected cells and early cancer cells
- Macrophages: Impaired phagocytosis (ability to engulf and destroy pathogens)
- Neutrophils: Reduced pathogen-killing capability
Research published in PMC confirms that prolonged cortisol exposure reduces T cell proliferation and activity, diminishing the body's ability to mount effective immune responses. At the same time, chronic cortisol elevation paradoxically increases inflammatory markers like IL-6, TNF-alpha, and C-reactive protein — creating a state where the immune system is simultaneously suppressed in some functions and overactivated in others.
How Do the Communication Pathways Work?
- HPA Axis: Stress triggers cortisol release, which directly binds receptors on immune cells, suppressing their function and altering gene expression.
- Sympathetic Nervous System: Adrenaline and noradrenaline affect immune cell distribution and function, redirecting resources away from immune surveillance during chronic activation.
- Vagus Nerve: This critical anti-inflammatory pathway connects the brain to immune organs. Chronic stress reduces vagal tone, weakening the body's natural brake on inflammation. Meditation and deep breathing activate this pathway.
- Cytokine Signaling: Immune cells communicate back to the brain through inflammatory cytokines, creating "sickness behavior" — fatigue, low mood, social withdrawal — that further compounds stress.
| Mechanism | Effect on Immune System | Result |
|---|---|---|
| Reduced lymphocyte production | Fewer T cells, B cells, NK cells available | Weakened defense against pathogens |
| Impaired immune cell function | Reduced phagocytosis, cytotoxicity | Slower pathogen clearance |
| Decreased IgA production | Weakened mucosal barriers | Increased respiratory/GI infections |
| Chronic inflammation | Elevated IL-6, CRP, TNF-alpha | Tissue damage, chronic disease risk |
| Gut microbiome disruption | Reduced beneficial bacteria, leaky gut | Compromised gut-associated immunity |
What Are the Benefits of Managing Stress for Immune Health?
Effective stress management can reverse many of the immune-suppressing effects of chronic stress, including increasing Natural Killer cell activity, improving antibody responses to vaccines, reducing inflammatory markers, and restoring healthy gut microbiome composition. Studies show that regular meditation practice can produce measurable immune improvements within eight weeks.
Can Meditation Actually Boost Your Immune System?
A systematic review of 20 randomized controlled trials involving more than 1,600 participants found that mindfulness meditation is associated with reductions in pro-inflammatory processes, increases in cell-mediated defense parameters, and increases in enzyme activity that guards against cell aging. Specific findings include:
- Increased antibody response: Eight weeks of mindfulness meditation improved antibody response to influenza vaccination
- Reduced cortisol: Regular meditation practice significantly lowers cortisol levels
- Enhanced NK cell activity: Meditation increases Natural Killer cell function
- Reduced inflammatory cytokines: Lower levels of IL-6 and CRP
- Increased telomerase activity: Protects immune cell chromosomes from premature aging
A landmark PNAS study on advanced meditation practitioners found robust activation of immune system genes, with up-regulation of pathways related to both innate and adaptive immunity and down-regulation of oxidative stress genes.
What Other Stress Management Techniques Support Immunity?
- Deep breathing exercises activate the parasympathetic nervous system and increase vagal tone, directly counteracting the inflammatory effects of chronic stress
- Yoga reduces cortisol and inflammatory markers while combining movement, breath work, and mindfulness
- Social connection buffers against stress-induced immune suppression — loneliness is as harmful to immunity as smoking is to lung health
- Nature exposure ("forest bathing") reduces cortisol, lowers blood pressure, and enhances NK cell activity
- Regular moderate exercise reduces stress hormones and increases endorphins while enhancing immune surveillance
- Cognitive behavioral therapy reduces chronic stress patterns and may improve immune biomarkers
What Are the Real-World Risks of Unmanaged Chronic Stress?
Unmanaged chronic stress significantly increases infection risk by 2–3 times, reduces vaccine effectiveness by up to 50%, delays wound healing by 25–40%, and may trigger or worsen autoimmune conditions. Chronic stress also accelerates cellular aging through telomere shortening and disrupts the gut microbiome, further compromising immune function.
How Does Stress Affect Your Risk of Getting Sick?
- Increased infection susceptibility: Chronically stressed individuals are 2–3 times more likely to develop colds and upper respiratory infections. Stress can also reactivate latent viruses like herpes simplex.
- Reduced vaccine effectiveness: Studies show chronically stressed caregivers may produce up to 50% fewer antibodies in response to influenza vaccination, with protection lasting a shorter duration.
- Slower wound healing: Stress delays healing by 25–40%, affecting surgical recovery, chronic wound management, and everyday tissue repair.
- Autoimmune disease risk: Chronic stress may trigger or worsen autoimmune conditions by disrupting immune self-tolerance, with documented links to rheumatoid arthritis, lupus, and multiple sclerosis.
- Chronic disease acceleration: The persistent inflammation from chronic stress is linked to cardiovascular disease, type 2 diabetes, certain cancers, Alzheimer's disease, and depression.
- Gut microbiome disruption: Stress alters gut bacteria composition, reduces beneficial species, and increases intestinal permeability ("leaky gut") — compromising the approximately 70% of immune tissue located in the gut. Learn more about this critical connection in our guide to gut health and immunity.
How Can You Build a Stress-Immune Protection Plan That Works?
An effective stress-immune protection plan combines daily mindfulness practices (10–20 minutes), regular moderate exercise, optimized sleep, social connection, and targeted supplementation with adaptogens like ashwagandha. Start with two to three techniques that appeal to you, practice consistently for at least eight weeks, and gradually expand your toolkit based on what works.
Which Breathing Techniques Reduce Stress Fastest?
4-7-8 Breathing (Best for Acute Stress):
- Inhale through nose for 4 counts
- Hold for 7 counts
- Exhale through mouth for 8 counts
- Repeat 4–8 cycles
Box Breathing (Best for Focus and Calm):
- Inhale for 4 counts
- Hold for 4 counts
- Exhale for 4 counts
- Hold for 4 counts
- Repeat for 5–10 minutes
Diaphragmatic Breathing (Best for Daily Practice):
- Place one hand on chest, one on belly
- Breathe deeply so belly rises (not chest)
- Slow, steady breaths for 5–10 minutes
- Practice 2–3 times daily
What Does a Daily Stress-Immune Practice Look Like?
- Morning (10 minutes): Meditation or deep breathing — activates the parasympathetic nervous system and sets a calm baseline for the day
- Midday (5–10 minutes): Brief walk in nature or stretching break — interrupts stress accumulation and resets cortisol
- Evening (10–15 minutes): Yoga, progressive muscle relaxation, or gratitude journaling — promotes recovery and prepares the body for restorative sleep
- Throughout the day: Mindful moments during stressful situations — three deep breaths before responding to triggers
| Technique | How It Works | Time Needed | Best For |
|---|---|---|---|
| Mindfulness meditation | Reduces cortisol, increases vagal tone | 10–20 min/day | Long-term immune resilience |
| Deep breathing | Activates parasympathetic response | 5–10 min, 2–3x/day | Acute stress relief |
| Yoga | Combines movement, breath, mindfulness | 20–60 min, 2–3x/week | Stress + flexibility + calm |
| Nature exposure | Reduces cortisol, enhances NK cells | 20–30 min/day | Mood + immune support |
| Social connection | Buffers stress, enhances immune function | Regular quality time | Emotional resilience |
Which Foods and Lifestyle Changes Best Support Stress and Immunity?
A stress-immune supportive lifestyle centers on nutrient-dense whole foods rich in magnesium, omega-3 fatty acids, B vitamins, and vitamin C, combined with consistent sleep of 7–9 hours, moderate daily exercise, limited caffeine and alcohol, and regular social connection. Adaptogens like ashwagandha and rhodiola can provide additional support.
What Should You Eat to Combat Stress and Support Immunity?
Nutrients depleted by stress:
- Magnesium — "nature's relaxant," rapidly depleted during stress; found in dark leafy greens, nuts, seeds, dark chocolate
- B vitamins — support nervous system and energy production; found in whole grains, eggs, legumes
- Vitamin C — powerful antioxidant depleted by cortisol; found in citrus fruits, bell peppers, berries
- Omega-3 fatty acids — anti-inflammatory, support mood and brain health; found in fatty fish, walnuts, flaxseed
Gut-supporting foods are especially important because stress disrupts the gut microbiome where 70% of your immune system resides. Learn more in our gut health and immunity guide. Include fermented foods (yogurt, kefir, sauerkraut), prebiotic fiber (garlic, onions, asparagus), and bone broth.
Foods to limit: Excess caffeine increases cortisol and anxiety; alcohol disrupts sleep and increases inflammation; refined sugar triggers inflammatory cascades and feeds harmful gut bacteria.
Which Adaptogens Help With Stress and Immune Function?
- Ashwagandha (Withania somnifera): A systematic review and meta-analysis of 9 studies (558 patients) found ashwagandha significantly reduced perceived stress (−4.72), anxiety (−2.19), and serum cortisol (−2.58) compared to placebo. A separate randomized, double-blind trial showed ashwagandha extract significantly improved immune profiles by modulating both innate and adaptive immunity, increasing immunoglobulins, cytokines, and TBNK cells. Typical dose: 300–600 mg daily of standardized root extract.
- Rhodiola rosea: Reduces fatigue and stress, improves mental performance under pressure, and supports immune function. Typical dose: 200–600 mg daily standardized to 3% rosavins.
- L-Theanine: An amino acid from tea that promotes relaxation without sedation, reduces stress and anxiety, and may support immune function. Typical dose: 200–400 mg daily.
Additional targeted supplements:
- Magnesium glycinate: 300–400 mg daily for stress and sleep support
- Vitamin D: 2,000–5,000 IU daily if deficient (supports mood and immunity)
- Probiotics: 10–50 billion CFU daily to support the gut-brain-immune axis
Always consult a healthcare provider before starting supplements, especially if taking medications. Learn about the gut-brain axis and how medicinal mushrooms can further support stress resilience and immune modulation.
What Is the Best Step-by-Step Action Plan for Protecting Your Immunity From Stress?
The most effective approach is a phased plan that starts with foundational stress awareness and basic breathing techniques, then builds to daily mindfulness practice, lifestyle optimization, and targeted supplementation. Consistency matters more than intensity — even 10 minutes of daily practice produces measurable immune benefits within eight weeks.
Phase 1: Foundation (Weeks 1–2)
- [ ] Assess your current stress level (rate 1–10 daily, note main stressors)
- [ ] Learn one breathing technique (4-7-8 or box breathing) and practice twice daily
- [ ] Prioritize sleep: set consistent bedtime, 7–9 hours per night
- [ ] Reduce caffeine after noon and limit alcohol to support sleep and reduce cortisol
Phase 2: Build Your Practice (Weeks 3–6)
- [ ] Start daily mindfulness meditation (begin with 5–10 minutes, build to 20)
- [ ] Add moderate exercise 30–60 minutes on most days (walking, yoga, swimming)
- [ ] Schedule time with supportive people — social connection buffers stress
- [ ] Begin an adaptogen like ashwagandha (300–600 mg daily) and magnesium glycinate (300–400 mg)
- [ ] Optimize nutrition: increase omega-3s, leafy greens, fermented foods; reduce sugar
Phase 3: Sustain and Expand (Weeks 7+)
- [ ] Maintain daily meditation and breathing practice
- [ ] Add weekly nature exposure (20–30 minutes outdoors)
- [ ] Consider yoga or progressive muscle relaxation 2–3 times per week
- [ ] Track progress: energy levels, sleep quality, mood, illness frequency
- [ ] Seek professional support if stress remains overwhelming (therapy, support groups)
- [ ] Adjust and personalize based on what works best for you
References
- Dhabhar, F.S. (2014). Effects of stress on immune function: the good, the bad, and the beautiful. Immunologic Research, 58(2-3), 193-210. Source
- Immunology of Stress: A Review Article (2024). PMC. Source
- The multifaceted impact of stress on immune function (2025). PMC. Source
- Black, D.S. & Slavich, G.M. (2016). Mindfulness meditation and the immune system: a systematic review of randomized controlled trials. Annals of the New York Academy of Sciences, 1373(1), 13-24. Source
- Investigating the Relationship Between Cortisol, a Stress Marker, and Immune Function Across Age and Gender (2025). PMC. Source
- Nisha, S. et al. (2025). A Comprehensive Review of Experimental Models of Stress: Pragmatic Insight Into Psychoneuroimmunology. Health Care Science. Source
- Dangers of the chronic stress response in the context of the microbiota-gut-immune-brain axis and mental health (2024). Frontiers in Immunology. Source
- Lopresti, A.L. et al. (2019). An investigation into the stress-relieving and pharmacological actions of an ashwagandha extract. Medicine, 98(37). Source
- Effects of Ashwagandha on stress and anxiety: A systematic review and meta-analysis (2024). Explore. Source
- Tharakan, A. et al. (2021). Immunomodulatory Effect of Withania somnifera Extract—A Randomized, Double-Blind, Placebo Controlled Trial. Medicines, 8(1), 1. Source
- Pharmacological Insights Into Ashwagandha: Immunomodulatory and Neuroprotective Properties (2025). PMC. Source
- The immunomodulatory role of Withania somnifera in inflammatory diseases (2023). Frontiers in Pharmacology. Source
Frequently asked questions
How quickly does chronic stress weaken the immune system?
Immune changes can begin within days of sustained stress, but significant immune suppression typically develops over weeks to months of chronic stress exposure. Research shows measurable reductions in NK cell activity and IgA levels within 2–4 weeks of persistent stress. The longer stress continues, the more pronounced the immune dysfunction becomes.
Can short-term stress actually help your immune system?
Yes, acute stress lasting minutes to hours can temporarily enhance immunity by mobilizing immune cells into circulation and increasing their readiness to respond to threats. This is an evolved survival mechanism. However, this beneficial effect reverses when stress becomes chronic, leading to immune suppression instead of enhancement.
How much does cortisol affect vaccine effectiveness?
Chronic stress can reduce antibody production in response to vaccines by up to 50%. Studies on caregivers of chronically ill family members showed significantly lower antibody responses to influenza vaccines compared to non-stressed controls. The protection from vaccines may also last a shorter duration in chronically stressed individuals.
Does meditation really improve immune function or is it just placebo?
Multiple randomized controlled trials demonstrate that meditation produces measurable biological changes in immune markers, beyond placebo effects. A systematic review of 20 RCTs found meditation reduces pro-inflammatory cytokines, increases cell-mediated defense parameters, and boosts telomerase activity. A PNAS genomic study showed meditation robustly activates immune system genes.
How long do you need to meditate to see immune benefits?
Research suggests immune benefits begin appearing after about 8 weeks of consistent daily meditation practice of 10–20 minutes. However, acute stress reduction from a single meditation session can provide immediate cortisol-lowering effects. For lasting immune improvements, consistency over months is more important than session length.
Is ashwagandha safe to take long-term for stress and immunity?
Clinical trials have studied ashwagandha use for 30–90 days with good safety profiles and mild side effects. However, a recent case report documented HPA axis suppression with chronic use, suggesting periodic breaks may be prudent. Consult your healthcare provider for long-term use, especially if you have thyroid conditions or take medications.
Can stress cause autoimmune diseases?
Research suggests chronic stress may trigger or worsen autoimmune conditions by disrupting immune regulation and self-tolerance mechanisms. Stress-induced immune dysregulation has been linked to the onset of rheumatoid arthritis, lupus, and multiple sclerosis. However, autoimmune diseases involve complex genetic and environmental factors, and stress is just one contributing element.
How does stress affect gut health and immunity?
Stress alters gut microbiome composition, reduces beneficial bacteria like Lactobacillus and Bifidobacterium, and increases intestinal permeability ("leaky gut"). Since approximately 70% of immune tissue is located in the gut, this disruption significantly compromises immune function. The gut-brain axis means stress directly communicates with gut immune cells through the vagus nerve and HPA axis.
What are the warning signs that stress is affecting your immune system?
Key warning signs include catching colds more than 3 times per year, slow recovery from illness, persistent fatigue despite adequate sleep, frequent cold sores or herpes outbreaks, slow wound healing, and recurring infections. If you experience these alongside high stress levels, your immune system may be compromised by chronic stress.
Can you take adaptogens and prescription medications together?
Some adaptogens may interact with prescription medications, particularly psychiatric medications, thyroid drugs, and immunosuppressants. Ashwagandha may affect thyroid hormone levels, and rhodiola may interact with antidepressants. Always consult your healthcare provider or pharmacist before combining adaptogens with any prescription medications.