immune system
Exercise and Immunity: How Much Is Optimal? | Guide
Discover how exercise affects your immune system. Learn the J-curve, optimal workout dose, overtraining risks, and recovery strategies for immune health.
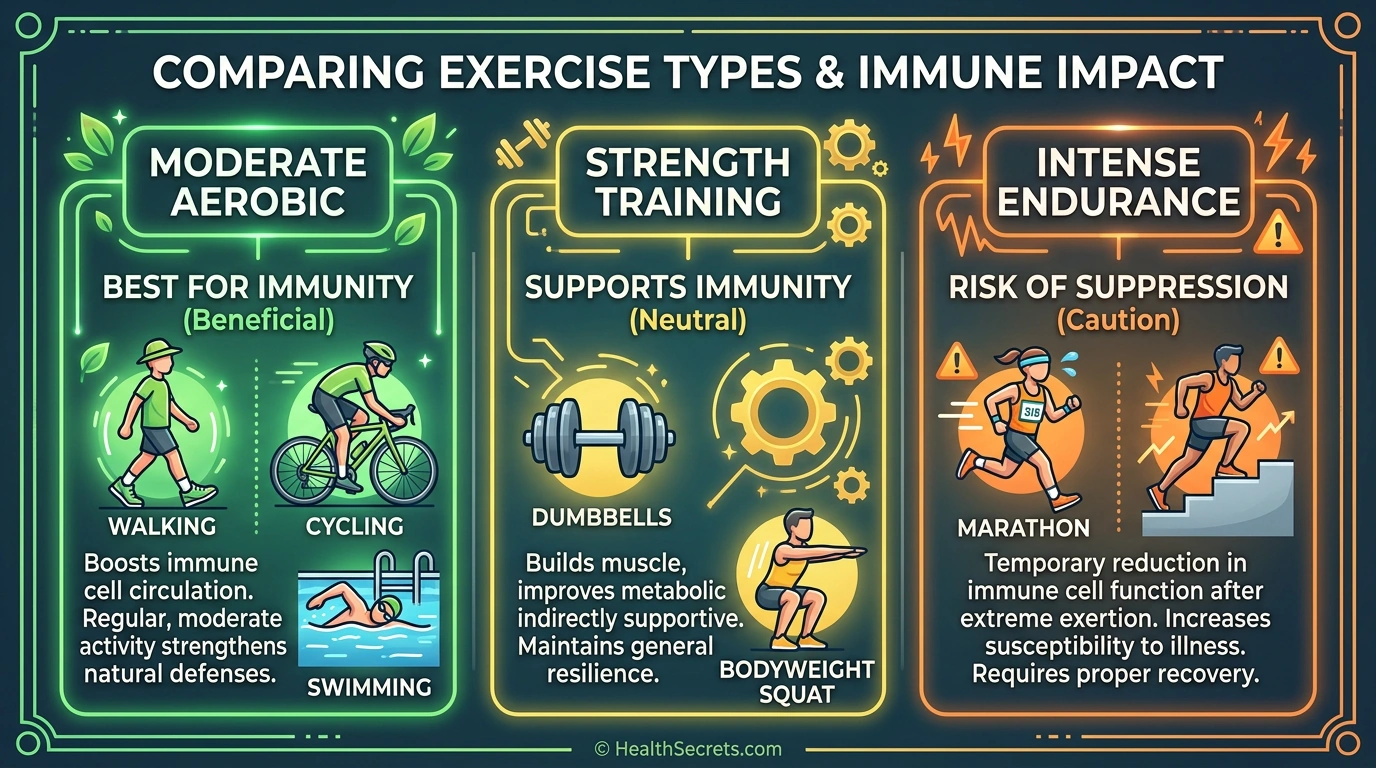
Exercise is one of the most powerful tools you have for keeping your immune system strong. People who move regularly catch fewer colds, recover faster from illness, and show better immune markers across the board. But there is a catch: more is not always better.
Research consistently shows that while moderate exercise reduces your risk of upper respiratory tract infections by 40–50%, prolonged intense training can temporarily weaken your defenses and leave you more vulnerable to getting sick. Scientists call this the J-curve relationship between exercise and immune system function, and understanding it could change the way you approach your workouts.
Whether you are a weekend walker, a gym regular, or a competitive athlete, finding your optimal exercise dose matters. Too little movement leaves your immune system underperforming. Too much can create an "open window" where pathogens slip through your weakened defenses.
In this guide, you will learn exactly how exercise affects your immune cells, where the sweet spot lies, and how to protect yourself during recovery. We will also cover what athletes need to know about overtraining and immune suppression, how to support immunity through nutrition and sleep, and practical strategies you can start using today to boost your immune system naturally.
- Moderate exercise (30–60 minutes most days) reduces upper respiratory infection risk by 40–50% compared to a sedentary lifestyle
- The J-curve model shows that both inactivity and excessive intense exercise increase infection risk, while moderate activity sits at the lowest point
- Each exercise session temporarily mobilizes immune cells, enhancing surveillance for pathogens and abnormal cells
- Prolonged intense exercise can create an "open window" of 3–72 hours where immune defenses are temporarily reduced
- Overtraining syndrome causes chronic immune suppression, frequent illness, persistent fatigue, and declining performance
- Recovery is when immune strengthening actually happens — sleep, nutrition, and rest days are non-negotiable
- The post-exercise immune window can be protected through proper carbohydrate and protein intake within 30–60 minutes
- Consistency matters more than intensity for long-term immune health — regular moderate movement beats occasional intense sessions
What Is the Exercise-Immunity Connection and Why Does It Matter?
The exercise-immunity connection refers to the complex, bidirectional relationship between physical activity and your body's ability to fight infections and disease. Regular moderate exercise enhances nearly every aspect of immune function, from increasing natural killer cell activity to improving antibody responses after vaccination.
Your immune system responds to exercise much like it responds to other physiological stressors — with a mobilization of immune cells, a temporary increase in inflammation followed by resolution, and long-term adaptations that make you more resilient. The key difference is that unlike chronic psychological stress, which suppresses immunity, regular moderate physical activity actually trains your immune system to work more efficiently.
Research from epidemiological studies shows that active adults experience 40–50% fewer sick days compared to their sedentary counterparts. A yearlong study of 547 adults found a 23% reduction in upper respiratory tract infection risk among those who exercised regularly at moderate intensity. These benefits extend beyond just catching fewer colds — regular exercisers also show improved vaccine responses, lower systemic inflammation, and reduced risk of chronic inflammatory diseases.
The challenge is that the relationship between exercise intensity and immune function is not linear. Scientists have modeled it as a J-shaped curve, where moderate activity provides maximum immune benefit while excessive training can actually push infection risk back up to sedentary levels or higher. Understanding this relationship is essential for anyone who wants to use exercise as an immune-boosting strategy without inadvertently undermining their defenses.
How Does Exercise Affect Your Immune System at the Cellular Level?
Exercise triggers a cascade of immune responses that begins within minutes of starting physical activity and can produce lasting benefits with consistent training. During moderate exercise, your body mobilizes immune cells into circulation, enhances their ability to detect threats, and stimulates anti-inflammatory pathways that protect against chronic disease.
How Does Moderate Exercise Enhance Immune Surveillance?
Each bout of moderate exercise causes a temporary surge in circulating immune cells. Natural killer (NK) cells, T cells, and neutrophils all increase in number and activity during and shortly after physical activity. This heightened state of immune surveillance means your body is better equipped to detect and eliminate pathogens, virus-infected cells, and even early cancer cells. Over time, repeated bouts of moderate exercise create a cumulative effect, essentially giving your immune system regular "practice runs" that keep it sharp and responsive.
What Role Do Anti-Inflammatory Cytokines Play During Exercise?
Moderate exercise triggers the release of anti-inflammatory cytokines, particularly IL-6 from contracting muscles, which in turn stimulates the production of IL-10 and IL-1 receptor antagonist. This anti-inflammatory cascade helps counteract chronic low-grade inflammation — a condition linked to weakened immunity, cardiovascular disease, type 2 diabetes, and other chronic conditions. Regular exercisers typically show lower baseline levels of C-reactive protein (CRP) and other inflammatory markers, indicating a healthier, more balanced immune environment.
How Does Exercise Improve Gut and Mucosal Immunity?
Regular moderate exercise increases gut microbiome diversity and supports gut barrier function. Since approximately 70% of your immune system resides in the gut, this matters enormously. Exercise also supports the production of secretory immunoglobulin A (sIgA) in mucosal surfaces — your first line of defense against respiratory and gastrointestinal pathogens. However, prolonged intense exercise can temporarily reduce sIgA levels, which partly explains why endurance athletes sometimes experience more upper respiratory infections during heavy training periods.
What Are the Key Benefits of Exercise for Immune Health?
The immune benefits of regular moderate exercise extend far beyond simply catching fewer colds. Physical activity influences virtually every branch of your immune system, from innate defenses to adaptive immunity, creating a more robust and responsive defense network.
Does Regular Exercise Reduce Your Risk of Respiratory Infections?
Yes, and the evidence is strong. Epidemiological studies and randomized controlled trials consistently report a reduction in upper respiratory tract infection incidence of 18–67% among regular moderate exercisers. A meta-analysis of exercise intervention studies found that people who maintained moderate activity had significantly fewer sick days, shorter illness duration, and less severe symptoms when they did get sick. These benefits are particularly pronounced in older adults and individuals under psychological stress, populations where immune function tends to decline.
Can Exercise Improve Your Vaccine Response?
Emerging research suggests that regular exercisers may mount stronger antibody responses to vaccinations, including influenza and COVID-19 vaccines. The mechanism likely involves exercise-enhanced immune cell trafficking and improved antigen presentation. For older adults whose vaccine responses tend to be weaker, maintaining an active lifestyle may help bridge the gap between vaccination and effective protection.
How Does Exercise Reduce Chronic Inflammation?
Chronic low-grade inflammation is a hallmark of aging (sometimes called "inflammaging") and is associated with weakened immune function. Regular moderate exercise acts as a natural anti-inflammatory intervention, reducing circulating levels of pro-inflammatory cytokines like TNF-alpha and IL-1beta while increasing anti-inflammatory mediators. This rebalancing helps preserve immune function as you age and reduces the risk of inflammation-driven chronic diseases.
Does Physical Activity Support Immune Cell Renewal?
Regular exercise appears to promote the turnover and renewal of immune cells, helping to maintain a diverse and functional immune repertoire. Studies show that physically active older adults have immune cell profiles that more closely resemble those of much younger individuals, with higher proportions of naive T cells and lower levels of senescent (worn-out) immune cells. This suggests that lifelong moderate exercise may help slow immune aging.
Are There Risks of Exercise for Immune Function?
While moderate exercise is overwhelmingly beneficial, there is a clear threshold beyond which the immune benefits diminish and risks emerge. Understanding these risks is critical for athletes and anyone who trains at high intensity.
What Is the "Open Window" of Immune Suppression After Intense Exercise?
The "open window" hypothesis describes a period of 3–72 hours after prolonged, intense exercise during which certain immune functions are temporarily suppressed. During this window, NK cell activity declines, neutrophil function may be impaired, sIgA levels drop, and lymphocyte counts fall as immune cells redistribute from the blood to peripheral tissues like the lungs and gut. Some researchers have challenged this model, suggesting that the apparent drop in blood immune cells actually represents beneficial redistribution rather than true suppression. However, the clinical observation that illness symptoms cluster around competitions and heavy training blocks remains well-documented.
What Is Overtraining Syndrome and How Does It Affect Immunity?
Overtraining syndrome occurs when excessive training volume and intensity are combined with insufficient recovery, leading to a chronic state of immune suppression, fatigue, and declining performance. Signs include persistent fatigue, frequent upper respiratory infections, elevated resting heart rate, mood disturbances, sleep problems, and inability to maintain training loads. Immune effects include decreased NK cell activity, reduced sIgA levels, suppressed neutrophil function, and increased susceptibility to reactivation of latent viruses. Recovery from overtraining syndrome can take weeks to months and requires significant training reduction.
Who Is Most at Risk for Exercise-Induced Immune Suppression?
Endurance athletes training at high volumes (marathon runners, triathletes, professional cyclists) face the highest risk. Other vulnerable groups include athletes who combine intense training with caloric restriction, individuals training in extreme environments (heat, cold, altitude), those experiencing high psychological stress alongside heavy training, and athletes who neglect sleep and recovery. The risk compounds when multiple factors overlap.
How Much Exercise Is Optimal for Immune Health?
Finding the right exercise dose requires balancing intensity, duration, frequency, and recovery. The goal is to land in the sweet spot of the J-curve — enough activity to enhance immune function without pushing into the zone of diminishing returns.
What Is the Optimal Exercise Prescription for Most People?
For general immune health, the evidence points to 150–300 minutes per week of moderate-intensity aerobic exercise (50–70% of maximum heart rate), spread across 5–7 days. A practical target is 30–60 minutes of moderate activity most days — brisk walking, cycling, swimming, dancing, or recreational sports. Add 2–3 sessions of moderate strength training per week for additional immune and metabolic benefits. The "talk test" is a simple intensity guide: you should be able to carry on a conversation but not sing during moderate exercise.
What Should Athletes Do to Protect Their Immunity?
Athletes pursuing performance goals should periodize training (alternating hard and easy weeks), ensure at least 1–2 complete rest days per week, prioritize 8–10 hours of sleep during heavy training blocks, and fuel adequately with sufficient calories, protein, and micronutrients. Monitoring resting heart rate, mood, energy levels, and illness frequency can help catch early signs of overtraining before immune function deteriorates significantly.
When Should You Skip a Workout? The Neck Check Rule
If you are feeling unwell, use the "neck check" as a guide. Symptoms above the neck only (mild runny nose, slight sore throat) may be compatible with light exercise. Symptoms below the neck (chest congestion, body aches, gastrointestinal issues) or any fever mean you should rest completely. After illness, return to exercise gradually — start at 50% of your normal intensity and volume, then increase over several days as you feel better. Rushing back risks relapse and prolonged recovery.
What Diet and Lifestyle Changes Support Exercise and Immunity?
Exercise does not work in isolation. Your immune response to training is heavily influenced by what you eat, how you sleep, and how you manage stress. Optimizing these factors amplifies the immune benefits of exercise and protects you during recovery.
What Should You Eat to Support Post-Exercise Immune Recovery?
Consuming carbohydrates (0.5–0.7g per pound of body weight) and protein (20–40g) within 30–60 minutes after exercise helps blunt the cortisol response, replenish glycogen, and support immune cell recovery. Include antioxidant-rich foods like berries, dark leafy greens, and colorful vegetables to combat exercise-induced oxidative stress. Adequate daily intake of immune-critical micronutrients is essential: vitamin D (2,000–5,000 IU if deficient), zinc (15–30mg), vitamin C (200–1,000mg), and iron (especially for female athletes). Staying well-hydrated supports mucosal immunity and all immune cell functions.
How Important Is Sleep for Exercise-Related Immune Function?
Sleep is arguably the single most important recovery tool for immunity. During deep sleep, your body releases growth hormone, repairs tissues, and consolidates immune memory. Athletes who sleep fewer than 7 hours per night are significantly more likely to develop upper respiratory infections. Aim for 7–9 hours (8–10 during heavy training blocks), maintain a consistent sleep schedule, and optimize your sleep environment. Learn more about how sleep affects your immune system.
Can Stress Management Improve Your Exercise-Immune Response?
Absolutely. Training is a physical stressor, and when combined with high psychological stress, the immune burden multiplies. Chronic stress elevates cortisol, suppresses immune function, and disrupts sleep — all of which compound the immune costs of intense exercise. Daily stress management practices (meditation, yoga, deep breathing, time in nature) can meaningfully reduce illness risk for active individuals.
Which Supplements May Support Immune Function in Active People?
For athletes and regular exercisers, targeted supplementation may help close nutritional gaps. Key candidates include vitamin D (if blood levels are below 40 ng/mL), probiotics (to support gut immune function), zinc (for immune cell function), and vitamin C (especially around heavy training periods). Adequate electrolyte intake also supports hydration and overall immune function during exercise.
What Should You Do First to Optimize Exercise for Immune Health?
Building an immune-supportive exercise routine does not require dramatic changes. Start with these phased steps and build gradually.
Phase 1: Establish Your Foundation (Weeks 1–2)
- [ ] Assess your current activity level and identify where you fall on the J-curve
- [ ] Set a target of 30 minutes moderate exercise on 5 days per week
- [ ] Choose activities you enjoy — walking, cycling, swimming, dancing
- [ ] Commit to 7–9 hours of sleep per night
- [ ] Stock up on post-workout recovery foods (protein, carbohydrates, fruits)
Phase 2: Build and Optimize (Weeks 3–6)
- [ ] Gradually increase session duration to 45–60 minutes as fitness improves
- [ ] Add 2 moderate strength training sessions per week
- [ ] Begin tracking resting heart rate each morning to monitor recovery
- [ ] Incorporate one daily stress management practice (10 minutes meditation or deep breathing)
- [ ] Ensure daily intake of vitamin D, zinc, and vitamin C through food or supplements
Phase 3: Sustain and Protect (Ongoing)
- [ ] Maintain 150–300 minutes moderate exercise per week with 1–2 rest days
- [ ] Periodize training if pursuing athletic goals (alternate hard and easy weeks)
- [ ] Use the neck check rule when feeling unwell — rest when symptoms are below the neck
- [ ] Monitor for overtraining signs: persistent fatigue, frequent illness, declining performance
- [ ] Reassess and adjust quarterly based on how you feel, illness frequency, and energy levels
References
- Nieman, D.C. & Wentz, L.M. (2019). The compelling link between physical activity and the body's defense system. Journal of Sport and Health Science, 8(3), 201–217. Source
- Kang, D. et al. (2021). Effect of Exercise Intensity on Cell-Mediated Immunity. Sports, 9(1), 8. Source
- Gleeson, M. (2007). Immune function in sport and exercise. Journal of Applied Physiology, 103(2), 693–699. Source
- Gleeson, M. (2015). Effects of Exercise on Immune Function. Gatorade Sports Science Institute. Source
- Peake, J.M. et al. (2017). Recovery of the immune system after exercise. Journal of Applied Physiology, 122(5), 1077–1087. Source
- Campbell, J.P. & Turner, J.E. (2018). Debunking the myth of exercise-induced immune suppression. Frontiers in Immunology, 9, 648. Source
- MacKinnon, L.T. (2000). Overtraining effects on immunity and performance in athletes. Immunology and Cell Biology, 78(5), 502–509. Source
- Arazi, H. et al. (2025). Beyond physical exhaustion: Understanding overtraining syndrome through the lens of molecular mechanisms and clinical manifestation. PMC. Source
- Kakanis, M.W. et al. (2010). The open window of susceptibility to infection after acute exercise in healthy young male elite athletes. Exercise Immunology Review, 16, 119–137. Source
- García-Giménez, R. et al. (2024). Sports and Immunity, from the recreational to the elite athlete. Journal of Science and Medicine in Sport. Source
- Romeo, J. et al. (2010). Physical activity, immunity and infection. Proceedings of the Nutrition Society, 69(3), 390–399. Source
- Pedersen, B.K. & Saltin, B. (2015). Exercise as medicine – evidence for prescribing exercise. Scandinavian Journal of Medicine & Science in Sports, 25(S3), 1–72. Source
Frequently asked questions
How much exercise per day is best for your immune system?
For optimal immune function, aim for 30–60 minutes of moderate-intensity exercise most days of the week, totaling 150–300 minutes per week. Moderate intensity means you can carry on a conversation but not sing. This dose consistently shows the greatest reduction in upper respiratory infection risk — around 40–50% compared to being sedentary. Going significantly beyond this without adequate recovery can diminish immune benefits.
Can too much exercise weaken your immune system?
Yes, prolonged intense exercise can temporarily suppress immune function for 3–72 hours after a session — a phenomenon called the "open window." Chronic overtraining can lead to sustained immune suppression, increased infection frequency, and overtraining syndrome. The key is balancing training intensity with adequate recovery, nutrition, and sleep.
What is the J-curve relationship between exercise and immunity?
The J-curve is a model showing that sedentary individuals have elevated infection risk, moderate exercisers have the lowest risk, and people doing excessive intense exercise see their risk rise again — forming a J shape on a graph. It illustrates that moderate, consistent exercise provides the greatest immune benefit, while both inactivity and extreme training increase vulnerability.
Should you exercise when you have a cold or the flu?
Use the "neck check" rule. If symptoms are only above the neck (runny nose, mild sore throat), light exercise may be acceptable. If symptoms are below the neck (chest congestion, body aches, fever, gastrointestinal issues), rest completely. Never exercise with a fever — it can be dangerous. When returning from illness, start at 50% intensity and build back gradually.
What are the signs of overtraining syndrome?
Key signs include persistent fatigue despite adequate rest, declining performance despite continued training, frequent illness (more than 3 upper respiratory infections per year), elevated resting heart rate, mood disturbances (irritability, depression), sleep problems, chronic muscle soreness, and loss of appetite. If you notice several of these signs together, reduce training significantly and consult a healthcare provider.
How long does the immune system take to recover after intense exercise?
After a single intense exercise session, most immune parameters return to baseline within 24–72 hours with adequate rest, nutrition, and sleep. Chronic overtraining can take weeks to months for full immune recovery. The recovery timeline depends on exercise intensity, individual fitness level, nutritional status, sleep quality, and overall stress load.
Does strength training affect immunity differently than cardio?
Strength training generally carries a lower risk of immune suppression than prolonged endurance exercise because sessions are typically shorter and involve more rest intervals. However, very heavy resistance training can temporarily suppress immune function. Both forms of exercise provide immune benefits when performed at moderate intensity with adequate recovery. A combination of aerobic and strength training appears optimal for overall immune health.
What should you eat after exercise to support your immune system?
Within 30–60 minutes post-exercise, consume carbohydrates (0.5–0.7g per pound body weight) to replenish glycogen and reduce cortisol, along with 20–40g of protein to support recovery. Include antioxidant-rich foods like berries and dark leafy greens. Stay hydrated and ensure daily intake of immune-critical nutrients like vitamin D, zinc, and vitamin C through food or supplementation.
Does exercise help or hurt your immune system as you age?
Regular moderate exercise is one of the most powerful tools for maintaining immune function with age. Physically active older adults show immune cell profiles that more closely resemble those of younger people, with higher proportions of naive T cells and lower levels of senescent immune cells. The key is maintaining consistency with moderate activity while allowing for slightly longer recovery periods as you age.
Can exercise improve your response to vaccines?
Emerging research suggests that regular moderate exercisers may mount stronger antibody responses to vaccinations, including influenza and COVID-19 vaccines. The enhanced immune cell trafficking and improved antigen presentation associated with regular exercise likely contribute to this benefit. Some studies have also explored acute exercise before vaccination as a strategy to boost response, though results are mixed.