gut health
Food Intolerances vs Food Allergies: Complete Guide
Learn the key differences between food intolerances and food allergies, discover the 5 most common intolerances, and follow our step-by-step elimination diet protocol.
Have you ever eaten something that left you bloated, foggy, or drained — but you could not figure out what caused it? You are not alone. An estimated 20 percent of the population experiences some form of food intolerance, and that number appears to be rising. Yet most people still confuse intolerances with true food allergies, which can lead to unnecessary fear, misdiagnosis, or — worse — ignoring symptoms that quietly erode quality of life.
The confusion is understandable. Both conditions can cause digestive distress, and the terms "allergy," "intolerance," and "sensitivity" are used interchangeably in everyday conversation. But from a biological standpoint, the difference matters enormously. A food allergy can send you to the emergency room within minutes. A food intolerance will not kill you, but it can make every single day miserable if left unmanaged.
This guide breaks down the key differences between food allergies and intolerances, walks you through the five most common types of food intolerances, explains why most at-home sensitivity tests are unreliable, and gives you a step-by-step elimination diet protocol that actually works.
If you are new to gut health, our complete gut health guide provides the broader context for understanding how food reactions connect to overall digestive wellness. For those already dealing with specific digestive conditions, our guides on IBS and food triggers and leaky gut and food sensitivities offer deeper dives into those connections.
- Food allergies involve an IgE-mediated immune response and can be life-threatening, while food intolerances are non-immune reactions that primarily affect digestion and quality of life.
- The five most common food intolerances are lactose, non-celiac gluten sensitivity, histamine, FODMAPs, and sulfites — each with distinct mechanisms and management strategies.
- Symptoms of food intolerances can be delayed by hours or even days, making them significantly harder to identify than immediate allergic reactions.
- At-home IgG food sensitivity tests lack scientific validation and are not recommended by major allergy organizations — the elimination diet remains the gold standard for diagnosis.
- A structured three-phase elimination diet (elimination, reintroduction, maintenance) is the most reliable method for identifying your personal trigger foods.
- Leaky gut, gut dysbiosis, chronic stress, and antibiotic overuse can all increase your susceptibility to developing new food intolerances.
- Many food intolerances can be reduced or resolved by healing the gut lining, restoring microbial balance, and supporting digestive enzyme production.
What Are Food Intolerances and How Do They Differ From Food Allergies?
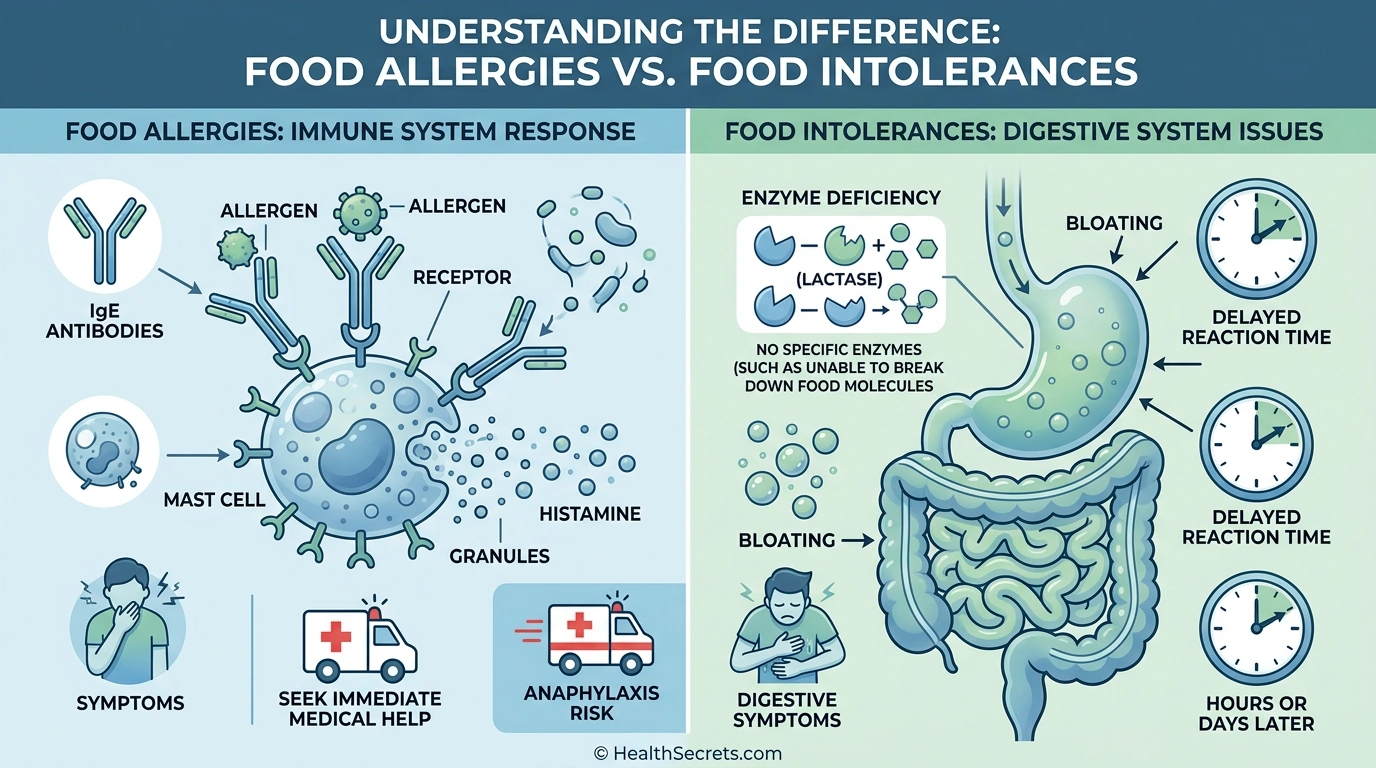
Food intolerances are adverse reactions to food that do not involve the immune system's IgE antibody pathway. Unlike true food allergies — which trigger rapid, potentially fatal immune responses — intolerances primarily affect the digestive system and produce delayed, non-life-threatening symptoms such as bloating, gas, diarrhea, headaches, and fatigue.
How Does a Food Allergy Work?
A true food allergy is an IgE-mediated immune response. When someone with a food allergy eats even a microscopic amount of the offending food, the immune system produces Immunoglobulin E (IgE) antibodies that trigger the release of histamine and other chemicals from mast cells. This cascade can cause hives, swelling, vomiting, difficulty breathing, and in severe cases, anaphylaxis — a life-threatening reaction requiring immediate epinephrine injection.
The top eight food allergens account for roughly 90 percent of all allergic reactions: milk, eggs, peanuts, tree nuts, fish, shellfish, wheat, and soy. Food allergy reactions result in an estimated 30,000 emergency room visits, 2,000 hospitalizations, and 150 deaths annually in the United States alone. Reactions typically occur within minutes to two hours and happen every time the food is consumed, regardless of amount.
How Does a Food Intolerance Work?
Food intolerances operate through entirely different mechanisms. They may result from enzyme deficiencies (like lactase deficiency in lactose intolerance), sensitivity to naturally occurring food chemicals (histamine, salicylates, sulfites), or difficulty digesting certain carbohydrates (FODMAPs). Crucially, the reaction is dose-dependent — small amounts may cause no problems at all, while larger portions trigger symptoms.
Intolerance symptoms can be delayed by 2 to 72 hours, making the connection between food and reaction much harder to identify. Symptoms are typically gastrointestinal (bloating, gas, cramping, diarrhea, constipation) but can also be systemic: headaches, migraines, brain fog, fatigue, joint pain, skin issues like eczema or acne, and even mood disturbances like anxiety and irritability.
| Feature | Food Allergy | Food Intolerance |
|---|---|---|
| Immune involvement | IgE-mediated immune response | Non-immune (digestive or enzymatic) |
| Reaction timing | Minutes to 2 hours | 2 to 72 hours (delayed) |
| Severity | Can be life-threatening (anaphylaxis) | Uncomfortable but not life-threatening |
| Dose dependency | Trace amounts can trigger reaction | Dose-dependent; small amounts often tolerated |
| Diagnosis | Skin prick test, IgE blood test, oral challenge | Elimination diet (gold standard) |
How Do Food Intolerances Develop in the Body?
Food intolerances develop through several distinct biological mechanisms, including enzyme deficiencies, chemical sensitivities, carbohydrate malabsorption, and impaired gut barrier function. Understanding these pathways helps explain why intolerances can appear suddenly in adulthood and why healing the gut often reduces or eliminates sensitivities over time.
What Role Do Enzyme Deficiencies Play in Food Intolerances?
The most well-understood mechanism is enzyme deficiency. In lactose intolerance, the body produces insufficient lactase — the enzyme needed to break down lactose (milk sugar) into absorbable glucose and galactose. Undigested lactose passes into the colon where bacteria ferment it, producing gas, bloating, cramping, and diarrhea. Primary lactase deficiency affects an estimated 68 percent of the global population, with prevalence varying significantly by ethnicity — ranging from 5 percent in Northern European populations to over 90 percent in East Asian populations.
Similar enzymatic issues underlie histamine intolerance, where insufficient diamine oxidase (DAO) enzyme allows histamine from foods like aged cheese, fermented foods, and wine to accumulate in the body. When histamine exceeds the body's capacity to break it down, it triggers headaches, flushing, hives, nasal congestion, and digestive distress.
How Does Intestinal Permeability Contribute to Food Sensitivities?
Research increasingly links food intolerances to compromised intestinal barrier function — commonly called leaky gut. When the tight junctions between intestinal epithelial cells become damaged, partially digested food proteins can cross into the bloodstream. This can trigger low-grade inflammatory responses and create new sensitivities to foods that were previously tolerated without any issues.
Factors that damage the gut barrier include chronic psychological stress, excessive NSAID use (ibuprofen, aspirin), alcohol consumption, antibiotic overuse, gut dysbiosis (microbial imbalance), and diets high in ultra-processed foods. Research from Mayo Clinic confirms that loss of intestinal barrier integrity plays a key role in the development of food sensitivities, IBS, and even autoimmune conditions. Addressing these root causes often reduces the number and severity of food intolerances over time.
How Do FODMAPs Cause Digestive Symptoms?
FODMAPs (Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols) are short-chain carbohydrates that are poorly absorbed in the small intestine. Their sensitivity mechanism involves two pathways: first, these unabsorbed carbohydrates draw water into the intestine through osmosis, causing distension; second, colonic bacteria ferment them rapidly, producing gas. The combination creates the bloating, abdominal pain, and altered bowel habits characteristic of FODMAP intolerance — particularly in people with IBS, who have heightened visceral sensitivity.
For a detailed protocol on managing FODMAP sensitivity, see our low-FODMAP diet guide.
What Are the Key Benefits of Identifying Your Food Intolerances?
Identifying and managing food intolerances can dramatically improve quality of life, resolve chronic symptoms that have persisted for years, and prevent long-term gut damage. Many people do not realize how much better they can feel until they remove their specific trigger foods and allow the digestive system to heal.
Can Identifying Food Intolerances Resolve Chronic Digestive Problems?
Absolutely. Chronic bloating, gas, abdominal pain, diarrhea, and constipation are among the most common symptoms of unidentified food intolerances. Many people spend years cycling through medications, doctor visits, and generalized dietary advice without improvement — simply because the specific trigger foods were never identified. A properly conducted elimination diet can pinpoint the exact foods causing symptoms, often delivering noticeable relief within the first two weeks of the elimination phase.
Do Food Intolerances Cause Symptoms Beyond Digestion?
Yes — and this is one of the most underappreciated aspects of food intolerances. Research confirms that food sensitivities can trigger a wide range of extra-intestinal symptoms including chronic headaches and migraines, persistent fatigue and brain fog, joint pain and muscle aches, skin conditions (eczema, acne, rashes), and mood disturbances like anxiety, depression, and irritability. The gut-brain axis — the bidirectional communication pathway between your digestive system and brain — helps explain why foods that irritate the gut can affect mental clarity and emotional wellbeing. Our gut health and mental health guide explores this connection in depth.
Can You Reduce the Number of Foods You React To?
This is perhaps the most empowering benefit. Unlike food allergies, which tend to be permanent, many food intolerances can be reduced or even eliminated by addressing root causes. Healing the gut lining, restoring healthy microbial balance with probiotics, reducing chronic stress, and supporting digestive enzyme production can all expand your tolerance over time. Some people find that foods they could not tolerate during a period of gut dysfunction become perfectly manageable once the gut has healed.
Does Managing Intolerances Prevent Long-Term Health Consequences?
Continuously eating foods your body cannot properly process maintains a state of chronic low-grade inflammation in the gut. Over time, this ongoing irritation can worsen intestinal permeability, deplete nutrient absorption, contribute to dysbiosis, and increase the risk of developing additional food sensitivities. Early identification and management of intolerances breaks this cycle and supports long-term digestive health.
Are There Any Risks of Ignoring Food Intolerances?
Ignoring food intolerances carries real risks including progressive gut damage, nutrient deficiencies, worsening symptoms over time, and reduced quality of life. While food intolerances are not immediately dangerous like allergies, their cumulative effects can significantly undermine health when left unaddressed for months or years.
The most significant risk is the self-reinforcing cycle of gut damage. Repeatedly consuming foods that cause inflammation in the digestive tract can progressively worsen intestinal permeability. As the gut barrier becomes more compromised, additional food proteins leak through, creating new sensitivities — a pattern that expands the list of reactive foods over time.
Nutrient deficiencies are another concern. Chronic diarrhea and intestinal inflammation impair the absorption of key nutrients including iron, calcium, B vitamins, magnesium, and zinc. These deficiencies can contribute to fatigue, weakened bones, poor immune function, and cognitive difficulties.
There is also a risk of misdiagnosis. Symptoms of food intolerance overlap significantly with conditions like IBS, celiac disease, inflammatory bowel disease, and even certain cancers. If you are experiencing persistent digestive symptoms, it is essential to work with a healthcare provider to rule out serious conditions before attributing everything to food intolerance.
When to see a doctor immediately: severe abdominal pain, blood in stool, unexplained weight loss, difficulty swallowing, persistent vomiting, or any symptoms of anaphylaxis (throat swelling, difficulty breathing, rapid pulse).
How Do You Identify and Test for Food Intolerances?
The most reliable method for identifying food intolerances is a structured elimination diet supervised by a healthcare provider or registered dietitian. While medical tests exist for specific conditions like lactose intolerance and celiac disease, there is no single validated test that identifies all food intolerances — making the elimination diet the gold standard diagnostic tool.
What Medical Tests Are Available?
- Hydrogen breath tests can diagnose lactose intolerance and fructose malabsorption by measuring hydrogen gas produced when undigested sugars are fermented by gut bacteria. These tests are accurate, non-invasive, and widely available through gastroenterology clinics.
- Celiac disease testing (tTG-IgA and EMA blood tests, confirmed by intestinal biopsy) should be performed before starting any gluten-free diet, as removing gluten first can produce false negative results.
- IgE allergy testing (skin prick tests or specific IgE blood tests) accurately identifies true food allergies but does not diagnose food intolerances.
Are At-Home Food Sensitivity Tests Accurate?
Most at-home food sensitivity test kits use IgG antibody testing, which has not been scientifically validated for diagnosing food intolerances. The American Academy of Allergy, Asthma & Immunology (AAAAI), the Canadian Society of Allergy and Clinical Immunology, and the European Academy of Allergy and Clinical Immunology have all recommended against using IgG testing for this purpose. IgG antibodies to food simply indicate exposure — not intolerance. In fact, higher IgG4 levels may actually indicate better tolerance to a food.
The Mayo Clinic confirms: "No single test is available for food sensitivity or intolerances," and the advertised kits can lead to unnecessary dietary restrictions and potential nutrient deficiencies.
How Do You Conduct an Elimination Diet? (Step-by-Step Protocol)
:::info[Phase 1: Elimination (2–4 weeks)] Remove these common trigger food categories simultaneously: :::
| Food Category | Examples | Why Eliminate | Alternatives |
|---|---|---|---|
| Dairy | Milk, cheese, yogurt, butter, cream | Lactose and casein reactions | Coconut milk, almond milk, oat milk |
| Gluten grains | Wheat, barley, rye, spelt | Gluten sensitivity | Rice, quinoa, buckwheat, millet |
| Eggs | Whole eggs, baked goods with eggs | Common intolerance trigger | Flax eggs, chia eggs in baking |
| Soy | Tofu, soy sauce, edamame, soy milk | Phytoestrogen and digestive issues | Coconut aminos, other legumes |
| Processed foods | Packaged snacks, fast food, additives | Artificial additives, preservatives | Whole, single-ingredient foods |
During the elimination phase, focus on foods that rarely cause reactions: most vegetables, most fruits (except citrus if suspected), rice, sweet potatoes, chicken, turkey, fish, olive oil, and most herbs and spices.
:::info[Phase 2: Reintroduction (6–8 weeks)] Reintroduce one food category at a time, eating a normal serving for three consecutive days while monitoring symptoms for the full 72-hour window. Keep a detailed food and symptom diary. Wait 3–4 days between introducing new foods. :::
| Week | Food to Test | Amount | What to Watch For |
|---|---|---|---|
| Week 1 | Dairy (start with yogurt) | 1 serving daily for 3 days | Bloating, gas, diarrhea, skin changes |
| Week 2 | Gluten (bread or pasta) | 1–2 servings daily for 3 days | Bloating, fatigue, brain fog, joint pain |
| Week 3 | Eggs | 1–2 eggs daily for 3 days | Digestive distress, skin reactions |
| Week 4 | Soy | 1 serving daily for 3 days | Bloating, hormonal symptoms |
| Week 5 | Corn | 1 serving daily for 3 days | Digestive symptoms, headaches |
| Week 6–8 | Additional suspected foods | 1 serving daily for 3 days each | Any symptom recurrence |
:::warning[Phase 3: Maintenance] Once you have identified your trigger foods, create a personalized long-term eating plan that avoids or limits those foods. Rotate tolerated foods to prevent developing new sensitivities. Periodically re-test reactive foods (every 3–6 months) as gut healing may improve tolerance over time. :::
What Diet and Lifestyle Changes Help Manage Food Intolerances?
Managing food intolerances goes beyond simply avoiding trigger foods. Supporting gut healing through targeted nutrition, stress management, and digestive support can reduce existing sensitivities and prevent new ones from developing. A comprehensive approach addresses root causes rather than just managing symptoms.
Gut-healing nutrition strategies:
- Include gut-healing foods like bone broth (rich in collagen and L-glutamine), fermented vegetables, and prebiotic-rich foods to support intestinal barrier repair
- Take a high-quality probiotic with diverse strains to restore microbial balance — our probiotic strains guide can help you choose the right one
- Consider L-glutamine supplementation (5–10g daily), which research shows supports intestinal lining repair
- Eat a diverse, whole-foods-based diet rich in colorful vegetables, healthy fats (olive oil, avocado, fatty fish), and adequate protein
- Support digestive enzyme production by eating mindfully, chewing thoroughly, and considering enzyme supplements with meals
Lifestyle factors that impact food intolerances:
- Stress management: Chronic stress directly increases intestinal permeability and reduces digestive enzyme production. Regular stress-reduction practices (meditation, deep breathing, walking in nature) support gut healing.
- Sleep optimization: Poor sleep disrupts the gut microbiome and impairs immune regulation. Aim for 7–9 hours of quality sleep nightly.
- Minimize unnecessary medications: NSAIDs, proton pump inhibitors, and antibiotics can all damage the gut barrier. Use them only when medically necessary and discuss alternatives with your doctor.
- Food diary practice: Even after the formal elimination diet, maintaining a simple food and symptom diary helps you catch new patterns early and track improvements over time.
Reading food labels: Learn to identify hidden sources of common trigger ingredients. Dairy can appear as casein, whey, or lactose. Gluten hides in soy sauce, malt flavoring, and modified food starch. Sulfites appear in dried fruits, wine, and processed meats.
What Should You Do First If You Suspect a Food Intolerance?
Start by ruling out serious conditions with your doctor, then implement a structured elimination diet while supporting overall gut health. A phased approach prevents overwhelm and produces the clearest results. Most people begin noticing symptom improvements within the first two weeks of eliminating trigger foods.
Phase 1 — Medical Evaluation (Week 1):
- [ ] Schedule an appointment with your primary care provider or gastroenterologist
- [ ] Request celiac disease blood testing (tTG-IgA) before removing gluten
- [ ] Request hydrogen breath test if lactose or fructose intolerance is suspected
- [ ] Rule out IBD, SIBO, and other conditions with overlapping symptoms
- [ ] Begin a food and symptom diary immediately
Phase 2 — Elimination Diet (Weeks 2–5):
- [ ] Remove dairy, gluten, eggs, soy, corn, and processed foods simultaneously
- [ ] Stock your kitchen with safe alternatives and plan meals for the week
- [ ] Record all foods eaten and any symptoms (type, severity, timing) daily
- [ ] Note energy levels, sleep quality, skin condition, and mood changes
- [ ] Continue for a full 2–4 weeks minimum before reintroduction
Phase 3 — Reintroduction and Gut Healing (Weeks 6–14):
- [ ] Reintroduce one food category every 3–4 days while monitoring symptoms
- [ ] Begin gut-healing support: L-glutamine, probiotics, bone broth
- [ ] Work with a registered dietitian to ensure nutritional adequacy
- [ ] Create your personalized long-term eating plan based on results
- [ ] Re-test reactive foods every 3–6 months as gut health improves
References
- Mayo Clinic. "Food allergy vs. food intolerance: What's the difference?" Mayo Clinic Expert Answers. Source
- American Academy of Allergy, Asthma & Immunology. "Food Intolerance Versus Food Allergy." AAAAI Conditions Library. Source
- Noga O, et al. "IgE and non-IgE food allergy: A review of immunological mechanisms." PMC. 2024. Source
- Shaoul R, et al. "Food Intolerances, Food Allergies and IBS: Lights and Shadows." PMC. 2024. Source
- American Academy of Family Physicians. "Food Intolerance vs Food Allergy: US Burden and Role of IgE." AAFP. Source
- Cleveland Clinic. "Food Allergy vs. Intolerance: What's the Difference?" Cleveland Clinic Health Essentials. Source
- UChicago Medicine. "Food allergy or food intolerance? A Q&A for parents." 2023. Source
- Vanner S, et al. "Mechanisms Underlying Food-Triggered Symptoms in Disorders of Gut-Brain Interactions." Gastroenterology. 2022. Source
- StatPearls. "Elimination Diets." NCBI Bookshelf. Source
- Vandenplas Y, et al. "Elimination diet in food allergy: friend or foe?" PMC. 2024. Source
- Mayo Clinic. "Food sensitivities may affect gut barrier function." Mayo Clinic Professional Resources. Source
- American Academy of Allergy, Asthma & Immunology. "The Myth of IgG Food Panel Testing." AAAAI. Source
Frequently asked questions
What is the difference between a food allergy and a food intolerance?
A food allergy is an IgE-mediated immune system response that can be life-threatening, while a food intolerance is a non-immune digestive reaction that is uncomfortable but not dangerous. Allergies react to trace amounts within minutes; intolerances are dose-dependent and symptoms can be delayed by hours or days. The distinction matters because management and risk levels differ significantly.
How long does it take for food intolerance symptoms to appear?
Food intolerance symptoms can appear anywhere from 2 to 72 hours after eating the trigger food. This delayed response is one of the main reasons intolerances are difficult to identify without a structured elimination diet. Keeping a detailed food and symptom diary with timestamps helps identify patterns that might otherwise go unnoticed.
Are at-home food sensitivity tests accurate?
Most at-home food sensitivity tests use IgG antibody testing, which has not been validated for diagnosing food intolerances. Major organizations including the AAAAI and the Canadian Society of Allergy and Clinical Immunology recommend against IgG testing. IgG antibodies indicate food exposure, not intolerance. The elimination diet remains the gold standard for identifying food intolerances.
Can you develop food intolerances later in life?
Yes, food intolerances can develop at any age. Primary lactase deficiency naturally progresses in adulthood as lactase production declines. Additionally, gut barrier damage from stress, medications, infections, or dysbiosis can create new sensitivities to previously tolerated foods. This is why some people suddenly react to foods they have eaten their entire lives.
How long should an elimination diet last?
The elimination phase should last 2 to 4 weeks, followed by a 6 to 8 week reintroduction phase. The full protocol takes approximately 8 to 12 weeks. Rushing the process — particularly the reintroduction phase — can produce unreliable results. Each food category should be tested for at least 3 days with a 3–4 day gap before testing the next food.
What are the most common food intolerances?
The five most common food intolerances are lactose intolerance, non-celiac gluten sensitivity, histamine intolerance, FODMAP sensitivity, and sulfite sensitivity. Lactose intolerance is the most prevalent worldwide, affecting an estimated 68 percent of the global population. FODMAP sensitivity is particularly common among people with IBS.
Can food intolerances be cured?
Many food intolerances can be significantly reduced or resolved by addressing root causes like leaky gut, dysbiosis, and enzyme deficiencies. Gut-healing protocols that include L-glutamine, probiotics, stress management, and anti-inflammatory nutrition often improve tolerance over time. However, some intolerances — particularly genetic enzyme deficiencies like primary lactose intolerance — are permanent and require ongoing management.
Is non-celiac gluten sensitivity a real condition?
Yes, non-celiac gluten sensitivity (NCGS) is recognized as a real clinical entity, though its mechanisms are not fully understood. Unlike celiac disease, NCGS does not involve autoimmune intestinal damage or IgE-mediated allergy. Diagnosis is made by exclusion — ruling out celiac disease and wheat allergy first, then confirming symptom improvement on a gluten-free diet and symptom return upon reintroduction.
What is histamine intolerance and how do you manage it?
Histamine intolerance occurs when the body cannot adequately break down histamine from foods due to insufficient diamine oxidase (DAO) enzyme activity. Management involves following a low-histamine diet (avoiding aged cheeses, fermented foods, cured meats, wine, and vinegar), eating fresh foods prepared quickly, and potentially supplementing with DAO enzymes before meals.
Should children follow an elimination diet for suspected food intolerances?
Children can follow modified elimination diets, but only under the supervision of a pediatrician and registered dietitian. Growing children have specific nutritional requirements, and overly restrictive diets can impair growth and development. The elimination phase is typically shorter for children (2 weeks), and careful attention must be paid to ensuring adequate calcium, iron, protein, and caloric intake throughout the process.