gut health
Gut Health and Mental Health: The Complete Connection Guide
Discover how your gut health affects anxiety, depression, and mood. Learn about the gut-brain axis, psychobiotics, and a 30-day protocol to improve mental wellness through gut healing.
Have you ever felt "butterflies" in your stomach before a big event, or noticed that stress sends your digestion into chaos? These aren't coincidences — they're direct evidence of the powerful communication highway between your gut and your brain. Scientists now call this the gut-brain axis, and emerging research reveals that the trillions of bacteria living in your intestines play a far greater role in your mood, anxiety levels, and cognitive function than anyone imagined just a decade ago.
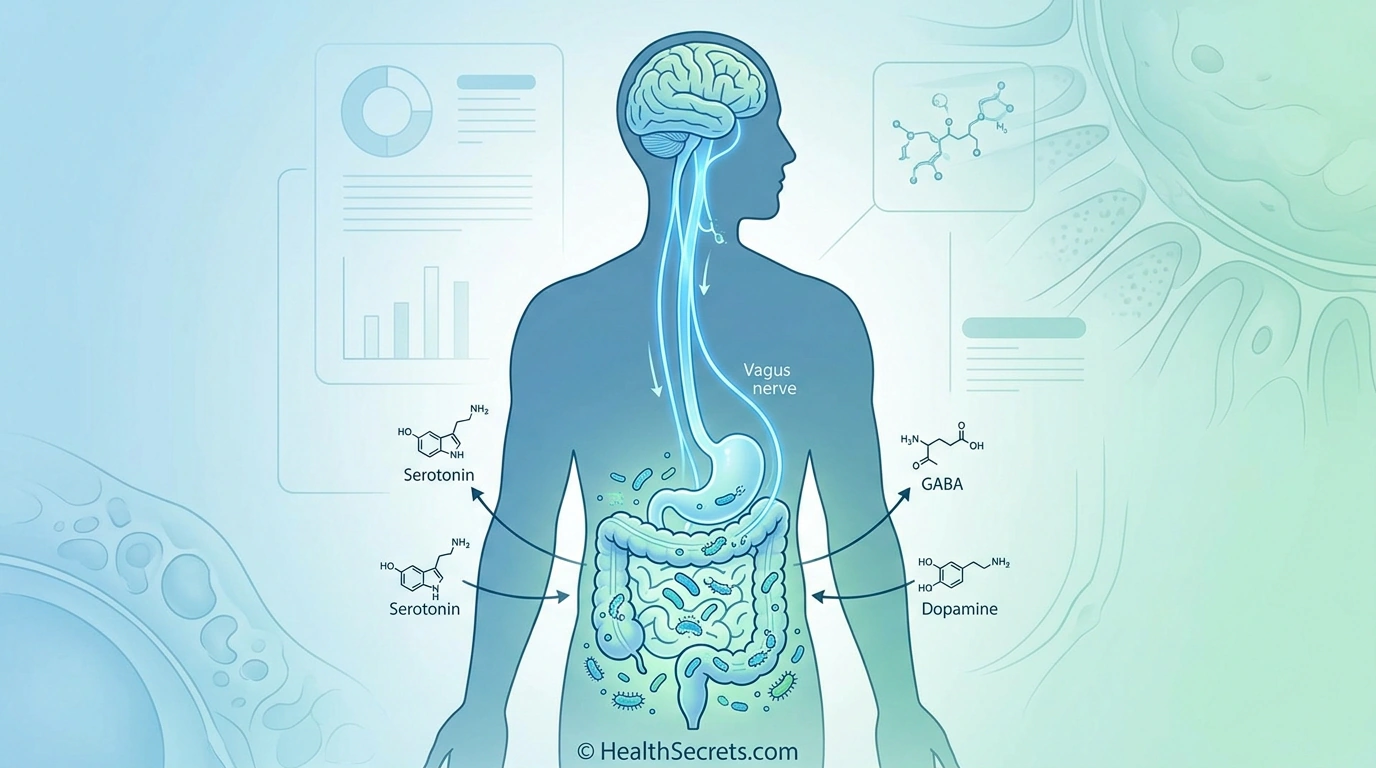
The numbers are staggering: your gut produces approximately 95% of your body's serotonin — the neurotransmitter most commonly associated with happiness and emotional stability. Your gut bacteria also manufacture GABA, dopamine, and other brain chemicals that directly influence how you feel every single day. When this microbial ecosystem falls out of balance, the consequences extend far beyond bloating and indigestion — they reach directly into your mental health.
For a comprehensive foundation, explore our complete guide to gut health and learn how the gut-brain axis works in detail. If you're interested in probiotics that support this connection, our best probiotics guide covers the top strains for digestive and mental wellness.
- Your gut produces approximately 95% of your body's serotonin and significant amounts of GABA and dopamine, making it a major driver of mood and emotional regulation.
- The gut-brain axis is a bidirectional communication system using the vagus nerve, immune signaling, the HPA stress axis, and microbial metabolites like short-chain fatty acids.
- Gut dysbiosis — an imbalance in intestinal bacteria — is linked to higher rates of depression, anxiety, brain fog, and stress-related disorders through systemic inflammation.
- Psychobiotics, including Lactobacillus helveticus R0052 and Bifidobacterium longum R0175, have shown clinically meaningful reductions in anxiety and depression symptoms in multiple trials.
- The inflammation-depression connection is well-established: leaky gut triggers systemic inflammation that crosses the blood-brain barrier and promotes neuroinflammation.
- A gut-brain healing protocol combines dietary changes (fermented foods, prebiotic fiber, omega-3s), targeted supplements (psychobiotics, magnesium, L-glutamine), and lifestyle practices (vagus nerve stimulation, stress management, quality sleep).
- Improvements in mood from gut-focused interventions typically begin within 2–4 weeks, with more significant changes occurring over 8–12 weeks of consistent effort.
- Professional help should be sought for severe depression or anxiety — gut healing complements but does not replace conventional mental health treatment.
What Is the Gut-Mental Health Connection and Why Does It Matter?
The gut-mental health connection refers to the bidirectional communication system between your gastrointestinal tract and your central nervous system, mediated by the vagus nerve, immune signaling, hormonal pathways, and the metabolic output of your gut microbiome. This relationship means that the state of your gut directly influences your mood, cognition, and stress resilience — and vice versa.
Your gastrointestinal tract houses the enteric nervous system (ENS), sometimes called your "second brain," which contains over 500 million neurons. These neurons communicate constantly with your brain through the vagus nerve — a superhighway where approximately 80% of signals travel from the gut to the brain, not the other direction. This means your gut is sending far more information to your brain than your brain sends to your gut.
The gut microbiome — the community of roughly 38 trillion microorganisms inhabiting your intestines — plays a central role in this communication. These bacteria produce neurotransmitters, regulate inflammation, maintain the intestinal barrier, and generate metabolites like short-chain fatty acids (SCFAs) that influence brain function at the cellular level.
Research from Harvard Medical School has identified specific bacterial species, such as Morganella morganii, that are linked to major depressive disorder through identifiable biological mechanisms. This is no longer theoretical — the gut-mental health connection is a measurable, modifiable pathway to better emotional health.
How Does Your Gut Communicate With Your Brain?
Your gut communicates with your brain through four primary pathways: the vagus nerve (neural), the immune system (inflammatory), the HPA axis (hormonal), and microbial metabolites (biochemical). These pathways operate simultaneously and bidirectionally, creating a constant feedback loop between your digestive system and your central nervous system.
How Does the Vagus Nerve Connect Your Gut and Brain?
The vagus nerve is the longest cranial nerve in your body, running from your brainstem to your abdomen. It serves as the primary communication cable between your gut and brain, carrying signals in both directions. Approximately 80% of vagal fibers are afferent (gut-to-brain), meaning your gut is constantly reporting its status to your brain. Clinical research from Feinstein Institutes and Northwell Health found that vagus nerve stimulation reduced postpartum depression symptoms in 74% of women in a clinical trial.
How Do Gut Bacteria Produce Brain Chemicals?
Your gut bacteria are neurotransmitter factories. The gut produces approximately 95% of total body serotonin, the primary mood-regulating neurotransmitter. Lactobacillus species influence serotonin and dopamine production, while Bifidobacterium and Lactobacillus rhamnosus produce GABA — the brain's primary calming neurotransmitter. Lactobacillus plantarum 299v has been shown to reduce kynurenine levels, a metabolite linked to depression when elevated.
How Does Gut Inflammation Affect Your Mood?
When the intestinal barrier becomes compromised ("leaky gut"), bacterial products like lipopolysaccharides (LPS) enter the bloodstream, triggering systemic inflammation. Pro-inflammatory cytokines — particularly IL-6, TNF-alpha, and IL-1beta — can cross the blood-brain barrier and promote neuroinflammation, which is increasingly recognized as a core mechanism in depression and anxiety. This inflammation-depression pathway explains why people with chronic gut issues frequently experience mood disorders.
What Role Does the HPA Axis Play in the Gut-Brain Connection?
The hypothalamic-pituitary-adrenal (HPA) axis is your body's central stress response system. Gut dysbiosis can dysregulate HPA axis function, leading to elevated cortisol levels. Chronic cortisol elevation further damages the intestinal barrier, creating a vicious cycle: stress damages the gut, gut damage increases inflammation, inflammation worsens mood, and worsened mood increases stress. Breaking this cycle requires addressing both gut health and stress management simultaneously.
What Are the Key Benefits of Healing Your Gut for Mental Health?
Healing your gut for mental health can reduce anxiety and depression symptoms, improve stress resilience, sharpen cognitive function, and stabilize mood through multiple converging mechanisms. Clinical trials with psychobiotics and gut-healing protocols demonstrate measurable improvements in validated psychological questionnaires within 4–8 weeks.
Can Fixing Your Gut Reduce Anxiety and Depression?
Multiple randomized controlled trials demonstrate that targeted probiotic supplementation significantly reduces anxiety and depression scores. A landmark study found that the combination of Lactobacillus helveticus R0052 and Bifidobacterium longum R0175 decreased psychological distress, including depression, anxiety, and anger-hostility, in healthy volunteers compared to placebo. These strains are now classified as psychobiotics — probiotics with documented mental health benefits.
Does Gut Healing Improve Cognitive Function and Brain Fog?
Gut-driven systemic inflammation impairs cognitive function through neuroinflammation, reduced BDNF (brain-derived neurotrophic factor) production, and disrupted neurotransmitter signaling. By reducing intestinal permeability and restoring microbial balance, many people report significant improvements in mental clarity, concentration, and memory. The mechanism involves reduced inflammatory cytokine production and restored production of SCFAs like butyrate, which support brain cell health.
How Does a Healthy Gut Improve Stress Resilience?
A balanced gut microbiome helps regulate the HPA axis, preventing excessive cortisol release during stressful situations. Research shows that probiotic supplementation can lower baseline cortisol levels and reduce the cortisol awakening response. This translates to practical improvements in how you handle daily stressors, with better emotional regulation and faster recovery from stressful events.
Can Gut Health Affect Sleep Quality and Mood Stability?
Your gut microbiome influences melatonin production and circadian rhythm regulation through serotonin metabolism (serotonin is the precursor to melatonin). Gut dysbiosis disrupts this pathway, contributing to sleep disturbances that further worsen mood. Restoring gut health can improve sleep onset, sleep quality, and next-day mood stability — creating a positive feedback loop between better sleep and better mental health.
Are There Any Risks or Side Effects of Gut-Brain Interventions?
Gut-brain interventions are generally safe when approached gradually, but potential risks include initial digestive discomfort from dietary changes, die-off reactions from probiotic introduction, and the danger of substituting gut healing for necessary psychiatric treatment. Starting slowly and working with a healthcare provider minimizes these risks.
- Initial digestive adjustment: Rapidly increasing fiber, fermented foods, or probiotics can cause temporary bloating, gas, and changes in bowel habits. Start with small amounts and increase gradually over 1–2 weeks.
- Probiotic considerations: While psychobiotics show promise for subclinical and mild-to-moderate mood issues, one clinical trial found no significant benefit for patients with established major depressive disorder. Probiotics should complement, not replace, evidence-based treatments for diagnosed mental health conditions.
- Medication interactions: Some gut-healing supplements (particularly St. John's Wort, which is sometimes recommended alongside gut protocols) interact with SSRIs, MAOIs, and other psychiatric medications. Always disclose all supplements to your prescribing physician.
- Over-attribution risk: Not all mental health challenges originate in the gut. Genetic factors, trauma, social circumstances, and neurological conditions require their own targeted interventions. Gut healing is one powerful tool in a comprehensive approach — not a cure-all.
How Do You Improve Your Mental Health Through Gut Healing?
Improving mental health through gut healing follows a structured 30-day protocol: remove inflammatory triggers in week one, rebuild with gut-healing foods in week two, reinoculate with targeted psychobiotics in week three, and optimize lifestyle factors in week four. Consistency across all four phases produces the strongest results.
Week 1: What Foods Should You Remove First?
Eliminate the most common gut disruptors: refined sugar, artificial sweeteners (which alter gut bacteria composition), processed foods with emulsifiers, excessive alcohol, and any known food sensitivities. These substances damage the intestinal barrier, feed pathogenic bacteria, and promote the inflammatory cascade that impacts mood. Replace them with whole, unprocessed foods and increase water intake.
Week 2: What Gut-Healing Foods Should You Add?
Introduce gut-repairing foods systematically: bone broth for L-glutamine and collagen, cooked vegetables for gentle fiber, and small portions of fermented foods like sauerkraut, kimchi, or kefir (start with 1–2 tablespoons daily). Add prebiotic-rich foods — garlic, onions, asparagus, and green bananas — to feed beneficial bacteria. Include omega-3-rich fatty fish (salmon, sardines) at least twice weekly.
Week 3: Which Psychobiotic Supplements Should You Start?
Begin targeted supplementation with clinically studied psychobiotic strains: L. helveticus R0052 + B. longum R0175 (the most researched combination for mood), along with supportive supplements like magnesium glycinate (200–400mg before bed for calming), L-glutamine (5g daily for intestinal barrier repair), and a high-quality omega-3 fish oil (1000–2000mg EPA+DHA daily).
Week 4: What Lifestyle Changes Strengthen the Gut-Brain Axis?
Optimize lifestyle factors that directly impact the gut-brain axis: practice vagus nerve stimulation techniques (deep diaphragmatic breathing, cold water face immersion, humming, and gargling), exercise aerobically for 30 minutes at least 4 times per week (shown to increase microbiome diversity), prioritize 7–9 hours of sleep, and establish a daily stress management practice (meditation, yoga, or time in nature).
What Diet and Lifestyle Changes Best Support the Gut-Brain Connection?
The most impactful dietary changes for gut-brain health include daily fermented foods, prebiotic fiber from diverse plant sources, omega-3 fatty acids, and polyphenol-rich foods — combined with regular exercise, quality sleep, stress management, and vagus nerve activation techniques. This combination addresses all four communication pathways of the gut-brain axis.
Which Foods Strengthen the Gut-Brain Connection?
- Fermented foods (kimchi, sauerkraut, kefir, yogurt, miso) deliver live beneficial bacteria directly to the gut. A Stanford study found that a diet high in fermented foods increased microbiome diversity and reduced inflammatory markers.
- Prebiotic foods (garlic, onions, leeks, asparagus, bananas, oats) feed existing beneficial bacteria.
- Omega-3 fatty acids (fatty fish, walnuts, flaxseeds) reduce neuroinflammation and support brain cell membrane integrity.
- Polyphenol-rich foods (berries, dark chocolate, green tea) act as fuel for beneficial gut bacteria and provide antioxidant protection.
- Tryptophan-rich foods (turkey, eggs, nuts, seeds, tofu) provide the raw material for serotonin production. Since most serotonin is produced in the gut, ensuring adequate tryptophan intake supports both digestive and mental health.
Which Foods Harm the Gut-Brain Connection?
Avoid or minimize: refined sugar (feeds pathogenic bacteria and causes mood-destabilizing blood sugar swings), artificial sweeteners (aspartame and sucralose alter gut bacteria composition), ultra-processed foods (emulsifiers like polysorbate 80 damage the mucus layer), excessive alcohol (increases intestinal permeability), and trans fats (promote systemic inflammation).
How Does Exercise Support the Gut-Brain Axis?
Regular aerobic exercise increases microbiome diversity — one of the strongest predictors of gut and mental health. Exercise also stimulates the vagus nerve, reduces cortisol, increases BDNF production, and promotes motility that supports healthy bacterial distribution. Even 30 minutes of moderate walking significantly impacts the gut-brain axis.
How Can You Stimulate the Vagus Nerve at Home?
At-home vagus nerve stimulation techniques include: deep diaphragmatic breathing (slow exhales activate the vagal brake), cold exposure (cold water on the face or cold showers), humming or singing (vibrates the vagus nerve through the larynx), meditation (activates parasympathetic pathways), and aerobic exercise. UCLA Health recommends these as evidence-based approaches to strengthen vagal tone and improve the gut-brain connection.
What Should You Do First to Improve Your Gut-Mental Health Connection?
Start with a two-week elimination of refined sugar, processed foods, and artificial sweeteners while simultaneously adding one serving of fermented food daily and beginning a 10-minute daily breathing practice. These three changes address the most impactful gut-brain pathways — microbial balance, intestinal permeability, and vagal tone — without requiring supplements or major lifestyle overhauls.
Phase 1 — Days 1–7: Remove and Replace
- [ ] Eliminate refined sugar, artificial sweeteners, and ultra-processed foods
- [ ] Replace with whole foods, vegetables, and clean protein sources
- [ ] Start eating one fermented food daily (sauerkraut, kimchi, or kefir)
- [ ] Begin 10-minute morning diaphragmatic breathing practice
- [ ] Increase water intake to 8+ glasses daily
Phase 2 — Days 8–14: Rebuild and Feed
- [ ] Add prebiotic-rich foods daily (garlic, onions, asparagus, bananas)
- [ ] Include omega-3 sources at least 3 times per week
- [ ] Start bone broth or L-glutamine supplementation
- [ ] Add 30 minutes of aerobic exercise 4+ days per week
- [ ] Establish consistent sleep schedule (7–9 hours)
Phase 3 — Days 15–21: Reinoculate
- [ ] Begin psychobiotic supplementation (L. helveticus + B. longum)
- [ ] Add magnesium glycinate (200mg before bed)
- [ ] Increase fermented food variety (2–3 different types weekly)
- [ ] Practice vagus nerve stimulation daily (cold exposure, humming)
Phase 4 — Days 22–30: Optimize and Maintain
- [ ] Assess mood and digestive improvements (journal tracking)
- [ ] Fine-tune supplement doses based on response
- [ ] Establish sustainable long-term dietary habits
- [ ] Consider gut testing if symptoms persist
- [ ] Consult healthcare provider for persistent mental health concerns
References
- Yano, J. M., et al. (2015). Indigenous bacteria from the gut microbiota regulate host serotonin biosynthesis. Cell, 161(2), 264-276. Source
- Carabotti, M., et al. (2015). The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems. Annals of Gastroenterology, 28(2), 203-209. Source
- Messaoudi, M., et al. (2011). Assessment of psychotropic-like properties of a probiotic formulation (Lactobacillus helveticus R0052 and Bifidobacterium longum R0175). British Journal of Nutrition, 105(5), 755-764. Source
- Bravo, J. A., et al. (2011). Ingestion of Lactobacillus strain regulates emotional behavior and central GABA receptor expression via the vagus nerve. PNAS, 108(38), 16050-16055. Source
- Rudzki, L., et al. (2019). Probiotic Lactobacillus Plantarum 299v decreases kynurenine concentration and improves cognitive functions in patients with major depression. Psychoneuroendocrinology, 100, 213-222. Source
- Cryan, J. F., & Dinan, T. G. (2012). Mind-altering microorganisms: the impact of the gut microbiota on brain and behaviour. Nature Reviews Neuroscience, 13(10), 701-712. Source
- Kelly, J. R., et al. (2017). Lost in translation? The potential psychobiotic Lactobacillus rhamnosus (JB-1) fails to modulate stress or cognitive performance in healthy male subjects. Brain, Behavior, and Immunity, 61, 50-59. Source
- Romijn, A. R., et al. (2017). A double-blind, randomized, placebo-controlled trial of Lactobacillus helveticus and Bifidobacterium longum for the symptoms of depression. Australian & New Zealand Journal of Psychiatry, 51(8), 810-821. Source
- Dinan, T. G., & Cryan, J. F. (2017). The Microbiome-Gut-Brain Axis in Health and Disease. Gastroenterology Clinics of North America, 46(1), 77-89. Source
- Foster, J. A., & McVey Neufeld, K. A. (2013). Gut-brain axis: how the microbiome influences anxiety and depression. Trends in Neurosciences, 36(5), 305-312. Source
- Clapp, M., et al. (2017). Gut microbiota's effect on mental health: The gut-brain axis. Clinics and Practice, 7(4), 987. Source
- Zhu, F., et al. (2020). Metagenome-wide association of gut microbiome features for schizophrenia. Nature Communications, 11, 1612. Source
Frequently asked questions
How long does it take for gut healing to improve mental health?
Most people notice initial mood improvements within 2–4 weeks of starting a gut-healing protocol, with more significant and stable changes occurring over 8–12 weeks. The timeline depends on the severity of gut dysbiosis, dietary consistency, and whether you're using targeted psychobiotic supplements. Neurotransmitter production shifts relatively quickly once beneficial bacteria colonize, but reducing systemic inflammation takes longer.
What are the best probiotic strains for anxiety and depression?
The most clinically studied strains for mood are Lactobacillus helveticus R0052 and Bifidobacterium longum R0175, which showed significant reductions in depression, anxiety, and psychological distress in multiple trials. Lactobacillus rhamnosus JB-1 influences GABA receptors and reduces anxiety-like behavior, while Lactobacillus plantarum 299v has been shown to reduce kynurenine levels linked to depression.
Can gut bacteria really produce serotonin and other brain chemicals?
Yes — your gut produces approximately 95% of your body's total serotonin through enterochromaffin cells that are directly influenced by gut bacteria. Gut microbes also produce GABA, dopamine, norepinephrine, and acetylcholine. While gut-produced serotonin doesn't directly cross the blood-brain barrier, it influences brain function through vagus nerve signaling and immune pathways.
Is there a connection between IBS and anxiety or depression?
Yes, the comorbidity between IBS and anxiety/depression is extremely high — studies show that 50–90% of IBS patients have co-occurring mood disorders. This bidirectional relationship means that gut inflammation and dysbiosis worsen anxiety, while anxiety and stress increase gut sensitivity and motility disruption. Treating both conditions simultaneously produces better outcomes than addressing either alone.
Can antibiotics cause depression by damaging gut bacteria?
Research supports a link between antibiotic use and increased risk of depression and anxiety. Antibiotics indiscriminately reduce beneficial bacteria, including species that produce serotonin and GABA. The impact depends on the antibiotic type, duration, and individual microbiome resilience. If you must take antibiotics, following up with psychobiotic supplementation and fermented foods helps restore mood-supporting bacteria.
What is the vagus nerve and how do you stimulate it naturally?
The vagus nerve is the longest cranial nerve connecting your brain to your gut, and strengthening its tone improves gut-brain communication. Natural vagus nerve stimulation techniques include deep diaphragmatic breathing with extended exhales, cold water face immersion, humming or gargling vigorously, meditation, and regular aerobic exercise. These practices activate the parasympathetic nervous system and improve both digestive function and emotional regulation.
Should you take psychobiotics instead of antidepressants?
No — psychobiotics should not replace prescribed psychiatric medication without medical supervision. Psychobiotics show the most promise for subclinical mood issues and mild-to-moderate symptoms, and they work well as complementary support alongside conventional treatment. One clinical trial found that psychobiotics did not significantly improve established major depressive disorder, underscoring the importance of professional psychiatric care for diagnosed conditions.
Does sugar really affect gut bacteria and mood?
Yes — high sugar intake promotes the growth of pathogenic bacteria and yeast (like Candida) while reducing beneficial species like Bifidobacterium and Lactobacillus. This shift increases intestinal permeability, drives inflammation, and disrupts neurotransmitter production. Sugar also causes rapid blood glucose fluctuations that independently trigger anxiety, irritability, and depressive symptoms.
How does leaky gut cause brain fog and cognitive problems?
When the intestinal barrier becomes compromised, bacterial endotoxins (lipopolysaccharides) enter the bloodstream, triggering systemic inflammation. Inflammatory cytokines cross the blood-brain barrier and cause neuroinflammation, which impairs synaptic function, reduces BDNF production, and disrupts neurotransmitter signaling. This manifests as brain fog, difficulty concentrating, memory problems, and mental fatigue. Healing the gut lining with L-glutamine, collagen, and anti-inflammatory foods can significantly improve cognitive function.
What gut tests can reveal mental health connections?
A comprehensive stool analysis (like GI-MAP) reveals bacterial diversity, pathogenic organisms, and inflammatory markers like calprotectin and zonulin. An organic acids test (OAT) measures microbial metabolites that indicate neurotransmitter production capacity. Food sensitivity testing (IgG panels) identifies immune-triggering foods that drive inflammation. While these tests aren't required to start a gut-brain protocol, they can help personalize your approach if initial efforts don't produce expected improvements.