supplements
Probiotics for Immune Health: Strains That Actually Matter
Discover which probiotic strains actually boost immunity. Evidence-based guide to LGG, B. lactis, S. boulardii dosing, and the 9 best immune probiotic supplements.
Your gut is home to roughly 70–80% of your immune cells. This is not a wellness talking point. It is a biological reality that explains why the trillions of bacteria living in your digestive tract have such a profound influence on whether you catch that cold making its way around the office or sail through flu season relatively unscathed.
Probiotics, the live beneficial bacteria you can take as supplements or get from fermented foods, tap directly into this gut-immune connection. But here is where most people go wrong: they grab whatever probiotic is on sale and hope for the best. The science is clear that different strains do very different things, and the strains that help with digestive comfort are not necessarily the same ones that reduce respiratory infections or enhance natural killer cell activity.
In this guide, you will learn which specific probiotic strains have the strongest clinical evidence for immune support, how they work at the cellular level, evidence-based dosing protocols for different populations, and which products deliver what they promise.
Related reading: Gut Health and Immunity: The Surprising Connection · How to Boost Your Immune System Naturally · Best Probiotics for Gut Health · Immune-Boosting Foods · Fermented Foods for Gut Health · Prebiotic Foods Guide · Sleep and Immune Function · Stress and Immune Function
- Approximately 70–80% of immune cells reside in or around the gut, making the gut microbiome a central hub for immune regulation.
- Strain specificity matters enormously: Lactobacillus rhamnosus GG, L. casei Shirota, and Bifidobacterium lactis BB-12 have the strongest clinical evidence for immune support.
- Meta-analyses show probiotics reduce respiratory infection incidence by 20–30% and shorten illness duration by 1–2 days, particularly in children and the elderly.
- Effective immune dosing ranges from 10–50 billion CFU daily for adults, with strain-specific protocols for prevention versus acute support.
- Saccharomyces boulardii, a beneficial probiotic yeast, is uniquely antibiotic-resistant and reduces antibiotic-associated diarrhea risk by 50–60%.
- Combination formulas with multiple evidence-based strains may offer synergistic immune benefits that single-strain products cannot match.
- Quality markers include full strain identification, CFU guarantee through expiration, third-party testing, and appropriate delivery technology.
- Probiotics are generally very safe but immunocompromised individuals should consult a healthcare provider before use.
What Are Immune-Supporting Probiotics and Why Do Strains Matter?
Probiotics are live microorganisms that confer a health benefit when consumed in adequate amounts. For immune support, the critical distinction is that different strains within the same species can have entirely different effects. The strain designation, the letters and numbers after the species name like "GG" in Lactobacillus rhamnosus GG, determines the specific immune mechanisms that probiotic activates.
The Gut-Immune Connection
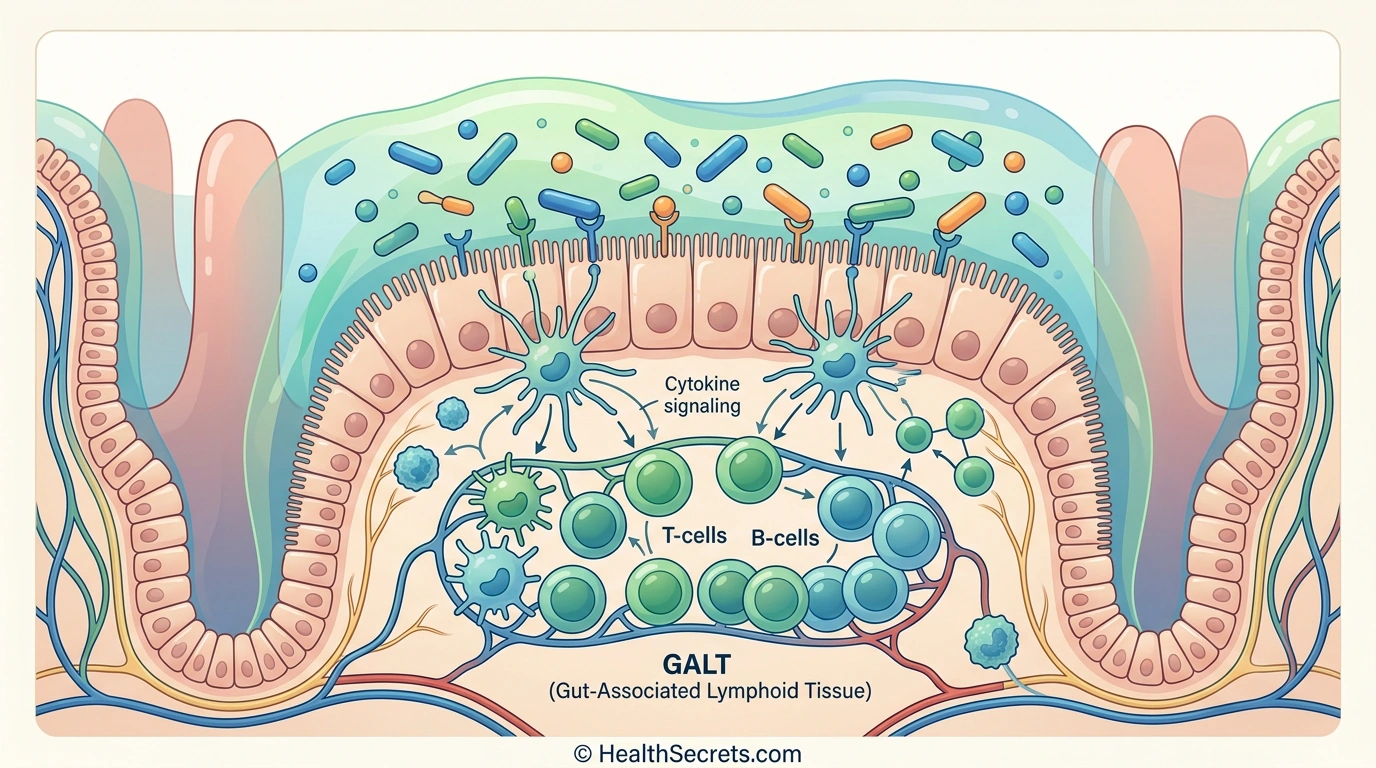
The gut-associated lymphoid tissue (GALT) is the largest immune organ in the body, containing Peyer's patches, mesenteric lymph nodes, and vast populations of immune cells including T cells, B cells, macrophages, and dendritic cells. Your gut encounters more foreign antigens than any other part of your body, making it the primary training ground where your immune system learns to distinguish pathogens from harmless substances. For a deeper exploration, see our full guide on gut health and immunity.
The Top Immune-Supporting Strains
- Lactobacillus rhamnosus GG (LGG) is the most clinically studied probiotic strain with over 1,000 publications. It consistently reduces respiratory infections in children by 20–30% and enhances natural killer cell activity, IgA production, and gut barrier function.
- Lactobacillus casei Shirota is extensively researched for enhancing NK cell activity, particularly in elderly populations and healthcare workers. Studies show reduced infection rates and improved immune markers across multiple populations.
- Bifidobacterium lactis (BB-12, HN019, Bi-07) enhances phagocytosis, NK cell activity, and vaccine antibody response. It is especially effective for elderly immune support and works synergistically when combined with L. acidophilus.
- Lactobacillus acidophilus NCFM activates dendritic cells and macrophages, increases antibody production, and reduces cold incidence and duration when paired with B. lactis Bi-07.
- Lactobacillus plantarum (299v, HEAL9) reduces upper respiratory infections in athletes and stressed individuals through antimicrobial compound production and immune modulation.
- Saccharomyces boulardii CNCM I-745 is a unique probiotic yeast that is antibiotic-resistant, making it the go-to choice during antibiotic treatment. It increases IgA production, strengthens gut barrier integrity, and reduces antibiotic-associated diarrhea by 50–60%.
- Bifidobacterium bifidum is dominant in breastfed infants and critical for early immune development. It enhances mucosal IgA production and may help reduce allergy risk in early life.
How Do Probiotics Strengthen the Immune System?
Probiotics support immunity through multiple overlapping mechanisms that work at both the gut barrier level and the systemic immune level. They strengthen the intestinal barrier, compete with pathogens for resources, produce antimicrobial compounds, and directly communicate with immune cells in the GALT to modulate both innate and adaptive immune responses.
How Do Probiotics Train and Activate Immune Cells?
Probiotics interact directly with dendritic cells and macrophages in the gut lining through pattern recognition receptors. This interaction triggers a cascade of immune activation: enhanced natural killer cell cytotoxicity, increased phagocytic activity of macrophages and neutrophils, and improved T cell and B cell function. A 2021 systematic review (PMC8320399) documented that specific probiotic strains increase production of secretory IgA, the antibody that protects mucosal surfaces throughout the body.
How Do Probiotics Balance the Inflammatory Response?
Rather than simply "boosting" immunity, probiotics modulate the Th1/Th2 cytokine balance, promoting appropriate immune responses while preventing excessive inflammation. They increase anti-inflammatory IL-10 while regulating pro-inflammatory TNF-alpha, IL-6, and IL-8. This balancing effect is why probiotics can simultaneously help fight infections and reduce inflammatory conditions.
How Do Probiotics Protect the Gut Barrier?
Probiotics strengthen tight junction proteins between intestinal epithelial cells, reducing intestinal permeability (commonly called "leaky gut"). They also produce short-chain fatty acids like butyrate that nourish the gut lining, and they compete with pathogenic bacteria for adhesion sites and nutrients through competitive exclusion.
How Well Do Probiotics Survive to Reach the Gut?
Probiotic viability through the harsh stomach acid environment is a major factor in effectiveness. Survival rates vary dramatically by strain, formulation, and delivery technology. Spore-forming strains like Bacillus species and the yeast Saccharomyces boulardii are naturally acid-resistant, while many Lactobacillus and Bifidobacterium strains benefit from protective delivery systems.
- Enteric-coated capsules protect probiotics through stomach acid, releasing them in the more hospitable small intestine environment.
- Time-release pearls (used by Hyperbiotics) use a patented delivery that claims 15 times better survival than standard capsules.
- Freeze-dried formulations maintain viability during storage but may not improve gut survival.
- Taking probiotics with food generally improves survival by buffering stomach acid and providing nutrients for the bacteria.
For immune benefits specifically, the probiotics need to reach the small intestine and colon where the GALT is concentrated. Products that guarantee CFU counts through expiration (not just at manufacture) provide a more reliable dose of live organisms.
How Many Billion CFU Do You Need for Immune Support?
For immune support, research generally supports 10–50 billion CFU daily for adults, though effective doses are strain-specific. The minimum effective dose for most immune-studied strains is approximately 1–10 billion CFU, but higher doses within the researched range tend to produce more consistent results. Consistency of daily use matters more than any single high dose.
| Population | Recommended Strains | Daily Dose | Duration | Notes |
|---|---|---|---|---|
| Adults (prevention) | LGG, B. lactis, L. acidophilus | 10–50 billion CFU | Ongoing daily | Start before cold season |
| Children (3+) | LGG (best evidence) | 5–10 billion CFU | Ongoing daily | Powders or chewables preferred |
| Elderly | L. casei Shirota, B. lactis | 10–50 billion CFU | Ongoing daily | Counteracts immune senescence |
| During antibiotics | S. boulardii, LGG | 250–500 mg S.b. 2×/day | During + 2–4 weeks after | Take 2–3 hours apart from antibiotic |
| Athletes | L. plantarum, L. casei | 10–50 billion CFU | During heavy training | Reduces exercise-induced immunosuppression |
Timing tips: Take probiotics with food for better survival through stomach acid. During antibiotic treatment, space probiotic doses 2–3 hours apart from the antibiotic. S. boulardii is the exception since it is naturally antibiotic-resistant and can be taken at any time. For prevention, start before cold and flu season rather than waiting until you are already sick.
Can You Get Enough Immune-Supporting Probiotics from Food Alone?
Fermented foods like yogurt, kefir, sauerkraut, kimchi, miso, and kombucha provide live probiotic cultures alongside valuable nutrients. However, for targeted immune support, food sources have significant limitations: the specific strains in fermented foods are rarely identified, CFU counts are variable and generally lower than supplements, and the immune-studied strains like LGG and B. lactis BB-12 are not typically found in traditional fermented foods.
The ideal approach combines both: daily fermented foods as a foundation for microbiome diversity, plus targeted supplements with evidence-based immune strains at therapeutic doses. Kefir provides the broadest spectrum of probiotic species among foods, while yogurt labeled with specific strain information (like Activia with B. lactis) offers a middle ground between food and supplement approaches. Prebiotic foods like garlic, onions, and asparagus feed your existing beneficial bacteria and complement probiotic supplementation.
Are Probiotics Safe for Long-Term Immune Support?
Probiotics have an excellent safety record with billions of doses consumed annually worldwide. Serious adverse events are extremely rare and limited almost exclusively to severely immunocompromised individuals. Most healthy adults can take probiotics indefinitely without safety concerns, and long-term use is actually preferred for sustained immune benefits since probiotics do not permanently colonize the gut.
Common initial side effects (usually temporary, resolving within 1–2 weeks): mild gas, bloating, or digestive changes as the gut microbiome adjusts. Starting with a lower dose and gradually increasing over 1–2 weeks minimizes these effects.
Who should exercise caution:
- Severely immunocompromised individuals (organ transplant recipients, advanced HIV/AIDS, active chemotherapy) face a rare but real risk of probiotic bacteremia or fungemia
- People with central venous catheters have theoretical infection risk
- Critically ill patients in intensive care should consult their medical team
- Premature infants require strain-specific safety evaluation
Drug interactions are minimal. The primary consideration is timing with antibiotics: space bacterial probiotics 2–3 hours apart from antibiotic doses, but S. boulardii can be taken concurrently since antibiotics do not affect yeast. Immunosuppressant medications warrant a conversation with your prescribing physician before starting probiotics.
What Can Probiotics Actually Do for Your Immune Health?
Probiotics provide meaningful but not miraculous immune benefits based on strong clinical evidence. Meta-analyses consistently show a 20–30% reduction in respiratory infection incidence and a 1–2 day reduction in illness duration. These effects are most pronounced in children, the elderly, athletes, and people recovering from antibiotic treatment.
- What probiotics can do: reduce the frequency of colds and upper respiratory infections, shorten illness duration when infections occur, reduce antibiotic-associated diarrhea risk by 50–60%, enhance natural killer cell and macrophage activity, improve vaccine antibody response, and support recovery after antibiotic treatment.
- What probiotics cannot do: prevent all infections, replace adequate sleep, nutrition, and stress management, cure active serious infections, or substitute for medical treatment when needed.
- Realistic timeline: Initial digestive adjustment takes 1–2 weeks. Measurable immune benefits typically emerge after 2–4 weeks of consistent daily use. Maximum benefit requires ongoing supplementation since probiotics are transient and do not permanently colonize the gut. Individual responses vary based on baseline microbiome composition, overall health, diet quality, and the specific strains used.
What Should You Do First to Support Your Immune System with Probiotics?
The most effective approach is selecting the right strain-specific product for your situation, establishing consistent daily use, and supporting probiotic effectiveness with diet and lifestyle measures. Here is a phased plan to optimize your probiotic immune strategy.
Phase 1 — Select and Start (Week 1):
- [ ] Identify your primary goal (general prevention, child health, antibiotic recovery, athletic performance, elderly support)
- [ ] Choose a product with evidence-based immune strains (see recommendations below)
- [ ] Start at half dose for 3–5 days to minimize digestive adjustment
- [ ] Take with food for optimal survival
Phase 2 — Establish Daily Protocol (Weeks 2–4):
- [ ] Increase to full dose and maintain consistent daily timing
- [ ] Add fermented foods daily (yogurt, kefir, sauerkraut) as a microbiome foundation
- [ ] Include prebiotic-rich foods to feed beneficial bacteria (garlic, onions, bananas, asparagus)
- [ ] Support with adequate sleep, stress management, and a nutrient-dense diet
Phase 3 — Optimize and Maintain (Month 2+):
- [ ] Track illness frequency and duration compared to previous seasons
- [ ] If taking antibiotics, add S. boulardii during treatment and for 2–4 weeks after
- [ ] Continue daily probiotic through cold and flu season at minimum
- [ ] Consider year-round use for sustained immune support
References
- Hao Q, Dong BR, Wu T. "Probiotics for preventing acute upper respiratory tract infections." Cochrane Database of Systematic Reviews. 2015;(2):CD006895. Source
- King S, Glanville J, Sanders ME, Fitzgerald A, Varley D. "Effectiveness of probiotics on the duration of illness in healthy children and adults." British Journal of Nutrition. 2014;112(1):41-54. Source
- Yan F, Polk DB. "Probiotics and immune health." Current Opinion in Gastroenterology. 2011;27(6):496-501. Source
- Gill HS, Rutherfurd KJ, Cross ML. "Dietary probiotic supplementation enhances natural killer cell activity in the elderly." Journal of Clinical Immunology. 2001;21(4):264-271. Source
- de Vrese M, Winkler P, Rautenberg P, et al. "Probiotic bacteria reduced duration and severity but not the incidence of common cold episodes." Vaccine. 2006;24(44-46):6670-6674. Source
- Leyer GJ, Li S, Mubasher ME, Reifer C, Ouwehand AC. "Probiotic effects on cold and influenza-like symptom incidence and duration in children." Pediatrics. 2009;124(2):e172-e179. Source
- Shida K, Sato T, Iizuka R, et al. "Daily intake of fermented milk with Lactobacillus casei strain Shirota reduces the incidence and duration of upper respiratory tract infections." European Journal of Nutrition. 2017;56(1):45-53. Source
- Makino S, Ikegami S, Kume A, Horiuchi H, Sasaki H, Orii N. "Reducing the risk of infection in the elderly by dietary intake of yoghurt fermented with Lactobacillus delbrueckii ssp. bulgaricus OLL1073R-1." British Journal of Nutrition. 2010;104(7):998-1006. Source
- McFarland LV. "Meta-analysis of probiotics for the prevention of antibiotic associated diarrhea." American Journal of Gastroenterology. 2006;101(4):812-822. Source
- Goldenberg JZ, Yap C, Lytvyn L, et al. "Probiotics for the prevention of Clostridium difficile-associated diarrhea." Cochrane Database of Systematic Reviews. 2017;12:CD006095. Source
- West NP, Pyne DB, Cripps AW, et al. "Lactobacillus fermentum VRI-003 and mucosal immunity in endurance athletes." British Journal of Sports Medicine. 2011;45(4):303-309. Source
- Waki N, Matsumoto M, Fukui Y, Suganuma H. "Effects of probiotic Lactobacillus brevis KB290 on incidence of influenza infection among schoolchildren." Letters in Applied Microbiology. 2014;59(6):565-571. Source
Frequently asked questions
Do probiotics really help prevent colds and flu?
Yes, multiple meta-analyses show probiotics reduce respiratory infection incidence by 20–30% and shorten illness duration by 1–2 days. The effect is most consistent with strains like LGG, L. casei Shirota, and B. lactis when taken daily at adequate doses. Probiotics are not a guarantee against infection, but they meaningfully reduce your risk.
Which probiotic strain is best for immune support?
Lactobacillus rhamnosus GG (LGG) has the most extensive clinical evidence for immune benefits, with over 1,000 published studies. For elderly populations, L. casei Shirota shows particularly strong results. For multi-strain benefits, combinations of L. acidophilus NCFM with B. lactis Bi-07 demonstrate synergistic immune effects. The best choice depends on your age, health status, and specific goals.
How many billion CFU do you need for immune benefits?
For immune support, research generally supports 10–50 billion CFU daily for adults, though effective doses are strain-specific. Children typically need 5–10 billion CFU. The key is consistency: taking an adequate dose daily is more important than occasional mega-doses. Products should guarantee CFU through expiration, not just at manufacture.
Can you take probiotics during antibiotic treatment?
Yes, and you should. Probiotics reduce antibiotic-associated diarrhea risk by 50–60%. Saccharomyces boulardii is the preferred choice since it is a yeast that antibiotics cannot kill. Bacterial probiotics like LGG should be taken 2–3 hours apart from antibiotic doses. Continue probiotics for 2–4 weeks after completing the antibiotic course.
Are probiotics safe for children?
Probiotics, particularly LGG, have an excellent safety record in children ages 1 and older. Clinical studies consistently show benefits for reducing respiratory and gastrointestinal infections in daycare and school settings. Use age-appropriate forms (powders, drops, or chewables) and strains with pediatric research. Consult a pediatrician before giving probiotics to infants under 1 year.
How long does it take for probiotics to improve immune function?
Most people experience initial digestive adjustment within 1–2 weeks. Measurable immune benefits typically emerge after 2–4 weeks of consistent daily use. For seasonal protection, start probiotics at least 2–4 weeks before cold and flu season. Maximum benefit requires ongoing daily supplementation since most probiotics do not permanently colonize the gut.
Should you refrigerate probiotics?
It depends on the product. Many modern probiotics are shelf-stable and maintain potency at room temperature when stored in a cool, dry place. Some higher-potency products still recommend refrigeration for optimal viability. Always check the product label. The most important factor is that the product guarantees CFU through the expiration date, not just at manufacture.
Are multi-strain probiotics better than single-strain for immunity?
Research suggests multi-strain formulas may offer broader immune benefits because different strains activate different immune pathways. The combination of L. acidophilus NCFM with B. lactis Bi-07, for example, shows synergistic effects on cold reduction. However, a single well-studied strain like LGG at an adequate dose can be equally effective for specific outcomes.
Can probiotics improve vaccine response?
Some studies show that certain probiotic strains, particularly B. lactis and L. casei, can enhance antibody production after vaccination, especially the flu vaccine. The effect is modest but meaningful, particularly in elderly populations with weaker vaccine responses. This is a promising area of research, though not yet a standard recommendation.
Is it better to get probiotics from food or supplements?
The ideal approach is both. Fermented foods provide diverse bacterial species plus valuable nutrients, but specific immune-studied strains like LGG are rarely found in food. Supplements deliver standardized, research-backed strains at therapeutic doses. Use daily fermented foods as a microbiome foundation and targeted supplements for specific immune benefits.