mental wellness
Gut-Brain Axis and Mental Health: The Complete Connection
Discover how the gut-brain axis connects your microbiome to depression, anxiety, and mood. Learn about psychobiotics, vagus nerve stimulation, and the 4R gut healing protocol for better mental health.
Have you ever had a "gut feeling" about something — or felt "butterflies" before a big event? These aren't just figures of speech. They reflect a profound biological reality: your gut and brain are intimately connected through a complex communication superhighway known as the gut-brain axis.
Scientists now understand that the 100 trillion bacteria living in your digestive tract do far more than help you digest food. They produce neurotransmitters, regulate inflammation, and communicate directly with your brain through the vagus nerve. In fact, approximately 90% of your body's serotonin — the "happiness molecule" — is produced not in your brain, but in your gut [18].
This discovery has revolutionized how we think about mental health. Research shows that 70% of depression patients have significant gut dysbiosis, and targeted probiotic strains — called psychobiotics — can reduce depression and anxiety symptoms by up to 50% [4]. The gut-brain axis represents one of the most promising frontiers in mental health treatment.
In this comprehensive guide, you'll learn exactly how the gut-brain axis works, why gut health matters for conditions like depression, anxiety, ADHD, and autism, and how to use specific probiotic strains, dietary changes, vagus nerve stimulation, and lifestyle modifications to optimize your mental health from the inside out.
Related reading: mental wellness guide · gut health and inflammation · chronic inflammation · supplements guide · detox cleanse complete guide
- The gut-brain axis is a bidirectional communication network — your gut affects your brain through neurotransmitters, inflammation, and the vagus nerve, while stress and emotions alter your gut microbiome composition
- Approximately 90% of your body's serotonin is produced in the gut by enterochromaffin cells, with gut bacteria directly influencing synthesis of serotonin, GABA, and dopamine
- 70% of depression patients show significant gut dysbiosis with reduced microbial diversity and depleted Lactobacillus and Bifidobacterium populations
-
Psychobiotics — specifically Lactobacillus helveticus R0052 combined with Bifidobacterium longum
R0175 — reduced depression and anxiety scores by up to 50% in clinical trials
- Leaky gut allows bacterial endotoxins (LPS) into the bloodstream, triggering systemic inflammation and neuroinflammation that drives depressive symptoms
- The vagus nerve carries 80% of signals from gut to brain, and stimulation techniques (deep breathing, cold exposure, meditation) improve treatment-resistant depression by 40%
- The 4R gut healing protocol — Remove triggers, Repair lining, Restore microbiome, Rebalance lifestyle — provides a systematic framework for improving mental health through gut health
- A Mediterranean diet reduces depression risk by 30–50% through anti-inflammatory effects, microbiome support, and providing precursors for neurotransmitter synthesis
- Dietary fiber (25–35g daily) feeds beneficial bacteria that produce short-chain fatty acids like butyrate, which cross the blood-brain barrier and improve mood
- Lifestyle factors including stress management, 7–9 hours of sleep, and 150 minutes of weekly exercise directly influence gut microbiome diversity and mental health outcomes
What Is the Gut-Brain Axis and Why Does It Matter for Mental Health?
The gut-brain axis is a bidirectional communication network connecting the gastrointestinal tract and the central nervous system through neural, hormonal, immune, and metabolic pathways. This system enables your gut microbiome — the 100 trillion bacteria inhabiting your digestive tract — to directly influence mood, cognition, and behavior, while your brain simultaneously shapes gut function and microbial composition.
What Makes the Gut Microbiome So Important for Brain Function?
Your gut microbiome is a complex ecosystem containing over 1,000 bacterial species weighing 3–5 pounds — more microbial cells than human cells in your entire body. This community performs critical functions including digestion, immune regulation, vitamin production, neurotransmitter synthesis, and inflammation control [2].
Each person's microbiome is as unique as a fingerprint, shaped by birth method, breastfeeding, diet, environment, medications, and stress exposure. When this ecosystem becomes imbalanced — a state called dysbiosis — the consequences extend far beyond digestive discomfort.
Why Is the Gut Called the "Second Brain"?
The enteric nervous system (ENS) contains approximately 100 million neurons lining the gastrointestinal tract — more than the spinal cord. This "second brain" can function independently of the central nervous system, controlling digestion, motility, and secretion on its own [3].
Critically, the ENS produces the same neurotransmitters as the brain — serotonin, dopamine, GABA, and acetylcholine. The ENS communicates with the brain primarily through the vagus nerve, creating a continuous feedback loop that influences mood, stress response, and cognitive function.
How Does the Gut Produce 90% of Your Serotonin?
Enterochromaffin cells in the intestinal lining produce approximately 90% of the body's total serotonin, with only about 5–10% synthesized in the brain's raphe nuclei. Gut bacteria directly influence this production by generating precursor molecules and enzymes required for serotonin synthesis [18].
While gut serotonin primarily regulates intestinal motility, secretion, and pain perception, the gut microbiome's influence on tryptophan metabolism — serotonin's amino acid precursor — directly affects how much tryptophan reaches the brain for serotonin production. This means gut bacterial composition can significantly impact your mood, sleep, and appetite regulation.
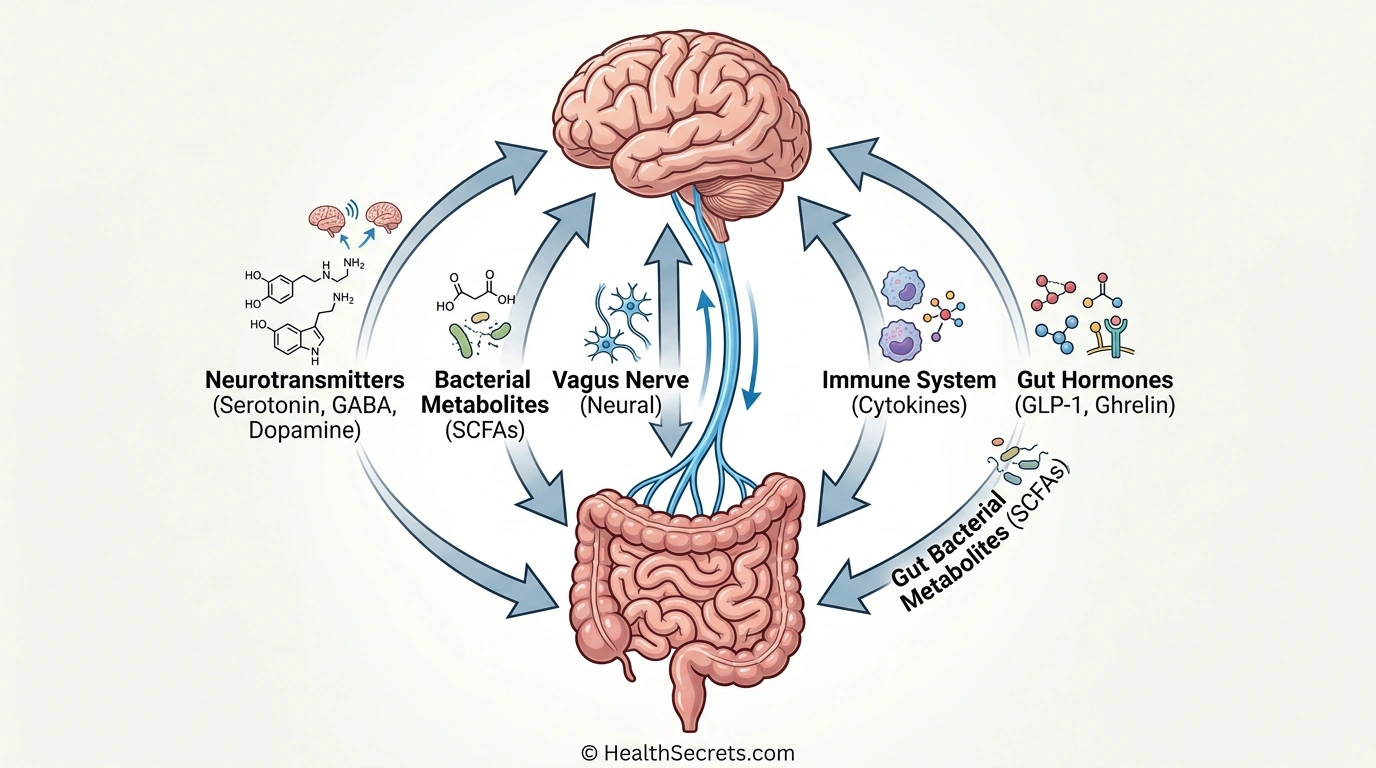
How Does the Gut Communicate With the Brain Through Five Key Pathways?
The gut-brain axis operates through five interconnected communication channels: the vagus nerve, neurotransmitter signaling, immune system activation, gut hormone signaling, and bacterial metabolite production. Understanding these pathways reveals why gut health is inseparable from mental health and how targeted interventions can improve both simultaneously.
How Does the Vagus Nerve Serve as the Primary Gut-Brain Highway?
The vagus nerve (cranial nerve X) is the longest cranial nerve, running from the brainstem to the abdomen. It serves as the primary physical connection between gut and brain, carrying 80% of signals in the afferent direction (gut → brain) and 20% efferent (brain → gut) [19].
Gut bacteria communicate their metabolic state, inflammation status, and nutrient availability to the brain through vagal afferent fibers. Research demonstrates that cutting the vagus nerve (vagotomy) blocks the behavioral effects of probiotics in animal models, confirming this nerve as an essential conduit for microbiome-brain signaling.
Vagal tone — measured by heart rate variability (HRV) — is a biomarker for this pathway's health. Higher vagal tone correlates with better mood, stress resilience, and gut health, while low vagal tone is associated with depression, anxiety, and chronic inflammation.
Which Neurotransmitters Do Gut Bacteria Produce?
Gut bacteria synthesize or influence production of virtually every major neurotransmitter affecting mental health:
- Serotonin — 90% produced in gut; regulates mood, sleep, appetite
- GABA — the primary calming neurotransmitter; Lactobacillus and Bifidobacterium species are prolific producers
- Dopamine — gut bacteria produce precursors affecting motivation, reward, and pleasure
- Acetylcholine — influences memory and learning
- Norepinephrine — affects alertness and stress response
Research confirms that specific gut bacteria strains produce neurotransmitters that directly influence brain function and behavior. Lactobacillus and Bifidobacterium species increased GABA production and reduced anxiety-like behavior in clinical models [5].
How Does Gut Inflammation Reach the Brain?
Approximately 70% of the immune system resides in the gut-associated lymphoid tissue (GALT), making the gut the body's largest immune organ. When gut bacteria become imbalanced, immune cells produce pro-inflammatory cytokines — IL-6, TNF-alpha, and IL-1β — that travel through the bloodstream and cross the blood-brain barrier [20].
This neuroinflammation disrupts neurotransmitter metabolism, impairs neuroplasticity, and activates the HPA stress axis — directly contributing to depressive symptoms. Anti-inflammatory cytokines like IL-10, promoted by beneficial gut bacteria, provide a counterbalance.
How Do Gut Hormones and Short-Chain Fatty Acids Affect Mood?
Gut bacteria influence hormone production including GLP-1 (satiety and mood), ghrelin (hunger and stress), and leptin (satiety and inflammation). These hormones act on brain regions involved in emotional regulation and behavior [16].
Perhaps most importantly, gut bacteria ferment dietary fiber to produce short-chain fatty acids (SCFAs) — butyrate, propionate, and acetate. These metabolites cross the blood-brain barrier, exerting anti-inflammatory and neuroprotective effects. Research shows butyrate improves mood, reduces anxiety, and protects against depression, while low SCFA levels correlate with depressive symptoms. The Western diet's typical fiber intake of less than 15g daily — well below the recommended 25–35g — may contribute to insufficient SCFA production and increased mental health vulnerability.
What Are the Mental Health Benefits of a Healthy Gut-Brain Axis?
A well-functioning gut-brain axis supports mood stability, stress resilience, cognitive sharpness, and emotional regulation. Research demonstrates that optimizing gut health through diet, probiotics, and lifestyle modifications can reduce depression and anxiety symptoms by 30–50%, improve cognitive performance, enhance stress adaptation, and support healthy neurotransmitter production throughout the body.
How Does a Healthy Microbiome Protect Against Depression?
A diverse, balanced gut microbiome maintains adequate serotonin precursor availability, produces anti-inflammatory SCFAs, supports gut barrier integrity (preventing endotoxemia), and promotes healthy vagal tone. The Mediterranean diet — the gold standard for gut-brain nutrition — reduces depression risk by 30–50% through these combined mechanisms [10].
Optimal gut health also maintains healthy tryptophan metabolism, ensuring this essential amino acid is directed toward serotonin production rather than the inflammatory kynurenine pathway, which generates neurotoxic metabolites.
How Do Psychobiotics Improve Anxiety and Stress Response?
Specific probiotic strains classified as psychobiotics directly improve mental health outcomes. Lactobacillus helveticus R0052 combined with Bifidobacterium longum R0175 reduced psychological distress, anxiety-like behavior, and cortisol levels in human trials [4]. These strains bias the immune system toward an anti-inflammatory profile, increase GABA receptor expression, and improve HPA axis function — all critical for anxiety management.
How Does Gut Health Support Cognitive Function?
SCFA production — particularly butyrate — supports blood-brain barrier integrity, promotes BDNF (brain-derived neurotrophic factor) production, and enhances neuroplasticity. Adequate gut microbial diversity also ensures optimal production of B vitamins, which are essential cofactors in neurotransmitter synthesis and cognitive performance.
What Happens When the Gut-Brain Axis Breaks Down?
Gut dysbiosis — an imbalanced microbiome with reduced diversity and overgrowth of pathogenic bacteria — disrupts every communication pathway in the gut-brain axis. Clinical research links dysbiosis to depression, anxiety, ADHD, autism spectrum disorder, and schizophrenia through mechanisms including reduced neurotransmitter production, increased intestinal permeability, systemic inflammation, and impaired vagal signaling.
How Does Gut Dysbiosis Drive Depression?
Approximately 70% of depression patients demonstrate significant gut dysbiosis characterized by reduced microbial diversity, depleted Lactobacillus and Bifidobacterium populations, and overgrowth of pro-inflammatory bacteria [14].
The mechanisms are multifaceted: reduced serotonin precursor metabolism, leaky gut driving endotoxemia and neuroinflammation, decreased SCFA production, and HPA axis dysregulation creating a chronic stress response. Research increasingly supports the view that depression is fundamentally an inflammatory condition, with 30–50% of depression patients showing elevated inflammatory markers including CRP, IL-6, and TNF-alpha.
How Does Leaky Gut Trigger Neuroinflammation and Depression?
When intestinal tight junctions become compromised — due to poor diet, chronic stress, alcohol, NSAIDs, or dysbiosis — bacteria and their toxins translocate into the bloodstream. Lipopolysaccharide (LPS) from gram-negative bacteria triggers systemic inflammation by activating TLR4 receptors on immune cells, producing pro-inflammatory cytokines that cross the blood-brain barrier [7].
This neuroinflammation shifts tryptophan metabolism away from serotonin production toward the kynurenine pathway, generating neurotoxic quinolinic acid. Simultaneously, inflammation reduces BDNF, impairs neurogenesis, and contributes to hippocampal atrophy — hallmarks of clinical depression.
How Are Anxiety, ADHD, and Autism Connected to Gut Health?
- Anxiety: Patients show altered microbiome composition with increased Firmicutes-to-Bacteroidetes ratio, reduced GABA-producing bacteria, and elevated inflammatory markers. Impaired vagus nerve signaling and heightened amygdala reactivity compound these effects [15].
- ADHD: 50–70% of children with ADHD report gastrointestinal symptoms. Research shows distinct microbiome patterns with reduced diversity, affecting dopamine production and nutrient absorption (iron, zinc, omega-3) — all critical for executive function.
- Autism Spectrum Disorder: Approximately 70% of individuals with ASD experience GI issues and display distinct microbiome patterns. Altered bacterial metabolites and heightened neuroinflammation affect brain development and behavior.
- Schizophrenia: Patients show altered microbiome composition, elevated inflammatory markers, and evidence of leaky gut. Neuroinflammation disrupts dopamine pathways central to the condition's pathophysiology.
How Can You Heal Your Gut to Improve Mental Health Using the 4R Protocol?
The 4R gut healing protocol — Remove, Repair, Restore, Rebalance — provides a systematic, evidence-based framework for rebuilding gut health and improving mental well-being. Research shows that following this structured approach for 8–12 weeks can significantly reduce depression and anxiety symptoms while restoring microbiome diversity and gut barrier integrity.
Step 1: How Do You Remove Gut-Damaging Triggers?
Eliminate factors that promote dysbiosis and intestinal permeability:
- Processed foods — high sugar, trans fats, and additives disrupt microbiome composition
- Excess sugar — feeds pathogenic bacteria; aim for less than 25g added sugar daily
- Gluten — if sensitive, increases intestinal permeability in susceptible individuals (trial 4–6 week elimination)
- Alcohol — directly damages intestinal lining and promotes dysbiosis
- NSAIDs — aspirin and ibuprofen compromise gut barrier (use sparingly)
- Unnecessary antibiotics — devastate beneficial bacteria populations (use only when medically necessary)
Step 2: How Do You Repair the Gut Lining?
Target intestinal permeability with these evidence-based supplements:
- L-Glutamine — 5–10g daily; primary fuel for intestinal cells, heals tight junctions
- Zinc — 15–30mg daily; supports gut barrier integrity and immune function
- Collagen peptides — 10–20g daily; provides amino acids (glycine, proline) for gut lining repair
- Bone broth — 1–2 cups daily; rich in collagen, gelatin, and minerals
- Omega-3 fatty acids — 2–4g EPA+DHA daily; anti-inflammatory, supports barrier function
Step 3: How Do You Restore a Healthy Microbiome?
- Probiotics: 10–50 billion CFU daily with psychobiotic strains (L. helveticus R0052 + B. longum R0175). Minimum 4–8 weeks consistent use for mental health benefits.
- Prebiotics: 5–10g daily of inulin, FOS, or GOS to feed beneficial bacteria. Food sources include onions, garlic, leeks, asparagus, bananas, and oats.
- Fermented foods: 1–2 daily servings of yogurt, kefir, sauerkraut, kimchi, or kombucha with verified live cultures.
- Diversity: Aim for 30+ different plant foods weekly to maximize microbial diversity.
Step 4: How Do You Rebalance Your Lifestyle for Gut-Brain Health?
- Anti-inflammatory diet — Mediterranean pattern with abundant vegetables, fruits, whole grains, legumes, olive oil, and fatty fish
- Stress management — meditation 20 minutes daily; yoga 2–3 times weekly; nature exposure
- Sleep optimization — 7–9 hours nightly; consistent schedule; gut microbiome repairs during sleep
- Regular exercise — 150 minutes weekly moderate activity; increases microbial diversity and SCFA production
What Are the Best Psychobiotic Strains for Mental Health?
Research identifies these specific strains with clinical evidence:
- Lactobacillus helveticus R0052 + Bifidobacterium longum R0175 — reduced depression and anxiety scores by 50% after 30 days; reduced cortisol; dose: 3 billion CFU daily [4]
- Lactobacillus rhamnosus JB-1 — increased GABA receptor expression in brain via vagus nerve; reduced anxiety and stress behavior [8]
- Bifidobacterium infantis 35624 — reduced depression symptoms and inflammatory markers (IL-6, TNF-alpha); increased tryptophan availability; dose: 1–10 billion CFU daily
- Lactobacillus plantarum PS128 — improved anxiety, cognition, and emotional regulation; affects dopamine and serotonin pathways; dose: 10 billion CFU daily [12]
- Bifidobacterium longum 1714 — reduced stress and improved memory in healthy adults; reduced cortisol via HPA axis modulation; dose: 1 billion CFU daily
Dosing guidance: 10–50 billion CFU daily; specific researched strains matter more than total CFU count; allow minimum 4–8 weeks for mental health benefits with consistent daily use.
What Should You Eat and How Should You Live for Optimal Gut-Brain Health?
A Mediterranean-style diet combined with targeted lifestyle modifications provides the strongest evidence-based foundation for gut-brain health. The Mediterranean diet reduces depression by 30–50%, while regular exercise increases microbial diversity, adequate sleep supports microbiome repair, and stress management protects gut barrier integrity — creating a synergistic effect greater than any single intervention alone.
Which Diet Best Supports the Gut-Brain Axis?
Mediterranean Diet (Best Evidence):
- Vegetables (5–9 servings daily, colorful variety)
- Fruits (2–3 servings daily, especially berries)
- Whole grains (3–5 servings daily — oats, quinoa, brown rice)
- Legumes (3–4 times weekly — beans, lentils, chickpeas)
- Nuts and seeds (1–2 oz daily — walnuts, flaxseeds, chia)
- Extra virgin olive oil (2–3 tbsp daily)
- Fatty fish (2–3 times weekly — salmon, sardines, mackerel)
- Fiber (25–35g Daily): Feeds beneficial bacteria that produce mood-enhancing SCFAs. Sources include vegetables, fruits, whole grains, legumes, nuts, and seeds. Most Western diets provide less than 15g — well below optimal levels [10].
- Fermented Foods: 1–2 daily servings of yogurt, kefir, sauerkraut, kimchi, kombucha, miso, or tempeh. Look for "live and active cultures" on labels.
- Omega-3 Fatty Acids: 2–4g EPA+DHA daily from fatty fish or supplements. Anti-inflammatory, supports both gut barrier and brain health.
- Polyphenols: Berries daily, green tea (2–3 cups), dark chocolate (70%+ cocoa, 1–2 oz) — these act as prebiotics feeding beneficial bacteria.
- Tryptophan-Rich Foods: Turkey, chicken, eggs, cheese, nuts, seeds, tofu — provide the serotonin precursor. Requires B vitamins, magnesium, and zinc for conversion.
Foods to Avoid:
- Processed foods — disrupt microbiome, promote inflammation
- Added sugar — feeds pathogenic bacteria, promotes dysbiosis
- Artificial sweeteners (saccharin, aspartame, sucralose) — alter microbiome composition
- Trans fats — pro-inflammatory
- Excess alcohol — damages gut lining
How Do Vagus Nerve Stimulation Techniques Improve Mental Health?
Vagus nerve stimulation (VNS) improves depression by approximately 40% in treatment-resistant cases. While medical VNS uses an implanted device (FDA-approved for treatment-resistant depression), several non-invasive methods effectively boost vagal tone [17]:
- Deep diaphragmatic breathing — 5–6 breaths per minute, 10–20 minutes daily; activates parasympathetic response
- Cold exposure — cold water on face (diving reflex) or 30–60 second cold shower; stimulates vagus nerve
- Singing, humming, and gargling — vocal cord vibration directly stimulates vagal fibers; 5–10 minutes daily
- Loving-kindness meditation — 20 minutes daily; research shows significant improvements in HRV and vagal tone
- Moderate aerobic exercise — walking, cycling, swimming, yoga; improves HRV and mood
- Psychobiotics — specific probiotic strains signal through the vagus nerve (L. rhamnosus JB-1 effects are blocked by vagotomy)
How Do Stress, Sleep, and Exercise Directly Impact Your Gut Microbiome?
- Stress: Chronic stress damages the gut barrier through cortisol, alters microbiome composition, and reduces beneficial bacteria populations. The relationship is bidirectional — gut dysbiosis itself amplifies the stress response through HPA axis dysregulation [15].
- Sleep: The gut microbiome produces GABA and serotonin (a melatonin precursor), directly influencing sleep quality. Circadian rhythm regulates gut bacteria composition, and the microbiome repairs during sleep. Poor sleep disrupts this cycle, promoting dysbiosis and depression.
- Exercise: Regular moderate exercise (150 minutes weekly) increases beneficial bacteria, enhances microbial diversity, and boosts SCFA production through improved gut motility and fiber fermentation. Exercise also improves mood through direct brain effects and enhanced gut-brain axis function.
- Antibiotics: While sometimes medically necessary, antibiotics devastate beneficial bacteria populations, with recovery taking months. Antibiotic-associated dysbiosis is linked to increased depression and anxiety risk. When required, take probiotics during and after treatment (separated by 2–3 hours).
What Is Your Step-by-Step Gut-Brain Health Action Plan?
Follow this phased 12-week protocol to systematically improve your mental health through gut healing. Each phase builds on the previous one, and most people notice meaningful improvements in mood and cognitive function within 4–8 weeks of consistent implementation.
Phase 1 — Assess and Remove (Weeks 1–2):
- [ ] Track GI symptoms: bloating, gas, diarrhea, constipation, abdominal pain
- [ ] Assess mental health: depression, anxiety, brain fog, mood swings
- [ ] Evaluate diet quality: processed food intake, sugar, fiber levels
- [ ] Eliminate processed foods, added sugars (below 25g daily), and excess alcohol
- [ ] Consider elimination trial: gluten-free for 4–6 weeks if sensitive
- [ ] Minimize NSAID use; discuss antibiotic alternatives with doctor
Phase 2 — Repair and Restore (Weeks 2–6):
- [ ] Start L-glutamine: 5–10g daily (powder in water, empty stomach)
- [ ] Add zinc: 15–30mg daily for gut barrier support
- [ ] Begin collagen peptides: 10–20g daily or bone broth 1–2 cups
- [ ] Start omega-3: 2–4g EPA+DHA daily
- [ ] Introduce psychobiotic probiotic: L. helveticus R0052 + B. longum R0175 (3+ billion CFU daily)
- [ ] Add prebiotic fiber: 5–10g inulin/FOS daily or food sources (onions, garlic, asparagus)
- [ ] Incorporate 1–2 servings fermented foods daily
Phase 3 — Optimize Diet and Lifestyle (Weeks 4–12+):
- [ ] Adopt Mediterranean eating pattern: 5–9 servings vegetables, 2–3 fruits, whole grains, legumes, olive oil, fatty fish
- [ ] Reach 25–35g fiber daily from diverse plant sources
- [ ] Practice vagus nerve stimulation daily: deep breathing (10–20 min), cold exposure, humming
- [ ] Exercise 150 minutes weekly: walking, cycling, swimming, or yoga
- [ ] Meditate 20 minutes daily (loving-kindness for vagal tone)
- [ ] Prioritize 7–9 hours sleep with consistent schedule
Phase 4 — Monitor and Adjust (Weeks 8–12):
- [ ] Track depression symptoms (PHQ-9) and anxiety (GAD-7) scores
- [ ] Monitor GI symptom improvement
- [ ] Assess energy, focus, and mood stability changes
- [ ] Consider comprehensive stool test for microbiome composition
- [ ] Optional: test inflammatory markers (CRP, IL-6) and HRV
Expected Timeline:
- Weeks 1–2: Adjustment period; possible temporary detox symptoms
- Weeks 2–4: GI symptoms improving; energy slightly increased; mood beginning to stabilize
- Weeks 4–8: Depression/anxiety symptoms reduced 20–30%; gut health significantly improved
- Weeks 8–12: Symptoms reduced 40–50%; mood stable; cognitive function improved
- Months 3–6+: Sustained improvements; lifestyle habits ingrained; stress resilience
When to see a doctor: Severe depression or suicidal thoughts (seek immediate help); no improvement after 12 weeks; persistent GI symptoms; before stopping psychiatric medications.
References
- Yano, J.M. et al. (2015). Indigenous bacteria from the gut microbiota regulate host serotonin biosynthesis. Cell, 161(2), 264-276. Source
- Cryan, J.F. et al. (2019). The microbiota-gut-brain axis. Physiological Reviews, 99(4), 1877-2013. Source
- Carabotti, M. et al. (2015). The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems. Annals of Gastroenterology, 28(2), 203-209.)00268-7/fulltext Source
- Messaoudi, M. et al. (2011). Assessment of psychotropic-like properties of a probiotic formulation (Lactobacillus helveticus R0052 and Bifidobacterium longum R0175). British Journal of Nutrition, 105(5), 755-764. Source
- Strandwitz, P. (2018). Neurotransmitter modulation by the gut microbiota. Brain Research, 1693(Pt B), 128-133. Source
- Evrensel, A. & Ceylan, M.E. (2019). Neuroinflammation, gut-brain axis and depression. Psychiatry Investigation, 16(1), 1-7. Source
- Ohlsson, L. et al. (2019). Leaky gut biomarkers in depression and suicidal behavior. Acta Psychiatrica Scandinavica, 139(2), 185-193. Source
- Bravo, J.A. et al. (2011). Ingestion of Lactobacillus strain regulates emotional behavior and central GABA receptor expression in a mouse via the vagus nerve. PNAS, 108(38), 16050-16055. Source
- Madison, A. & Kiecolt-Glaser, J.K. (2019). Stress, depression, diet, and the gut microbiota. Current Opinion in Behavioral Sciences, 28, 105-110. Source
- Jacka, F.N. et al. (2017). A randomised controlled trial of dietary improvement for adults with major depression. BMC Medicine, 15(1), 23. Source
- Berding, K. et al. (2021). Diet and the microbiota-gut-brain axis: Sowing the seeds of good mental health. Advances in Nutrition, 12(4), 1239-1285. Source
- Liu, Y.W. et al. (2019). Psychotropic effects of Lactobacillus plantarum PS128 in early life-stressed and naïve adult mice. Brain Research, 1631, 1-12. Source
Frequently asked questions
How does the gut-brain axis work, and why is it important for mental health?
The gut-brain axis is a bidirectional communication network connecting the gastrointestinal tract and the brain through five pathways: the vagus nerve, neurotransmitter signaling, immune activation, gut hormones, and bacterial metabolites. It matters for mental health because 90% of serotonin is produced in the gut, gut bacteria manufacture GABA and dopamine precursors, and intestinal inflammation can cross the blood-brain barrier to cause neuroinflammation linked to depression and anxiety. Disruptions in any of these pathways — caused by poor diet, stress, or dysbiosis — can directly impair mood, cognition, and emotional regulation.
Can improving gut health really help with depression and anxiety?
Yes, substantial clinical evidence supports this connection. Research shows that 70% of depression patients have gut dysbiosis, and targeted interventions can meaningfully reduce symptoms. Psychobiotic strains (L. helveticus R0052 + B. longum R0175) reduced depression and anxiety scores by up to 50% in clinical trials. The Mediterranean diet reduces depression risk by 30–50%. Addressing gut health through the 4R protocol (Remove, Repair, Restore, Rebalance) typically produces noticeable mood improvements within 4–8 weeks.
What are psychobiotics and which strains have the best evidence for mental health?
Psychobiotics are specific probiotic strains that produce measurable mental health benefits through the gut-brain axis. The strongest evidence exists for: Lactobacillus helveticus R0052 + Bifidobacterium longum R0175 (reduced depression/anxiety by 50%), Lactobacillus rhamnosus JB-1 (increased brain GABA via vagus nerve), Bifidobacterium infantis 35624 (reduced inflammation and improved serotonin precursor availability), and Lactobacillus plantarum PS128 (improved anxiety and cognition). Effective doses range from 10–50 billion CFU daily, with minimum 4–8 weeks consistent use needed.
How does leaky gut contribute to depression and brain fog?
Leaky gut (increased intestinal permeability) allows bacterial toxins — particularly LPS from gram-negative bacteria — to enter the bloodstream. This triggers systemic inflammation, producing pro-inflammatory cytokines (IL-6, TNF-alpha, IL-1β) that cross the blood-brain barrier. In the brain, these cytokines disrupt serotonin production by shifting tryptophan toward the neurotoxic kynurenine pathway, reduce BDNF (impairing neuroplasticity), and activate the chronic stress response. The resulting neuroinflammation manifests as depression, brain fog, fatigue, and cognitive dysfunction.
How long does it take to improve mental health by healing the gut?
Most people following a comprehensive gut-brain protocol notice initial improvements within 2–4 weeks, with significant benefits by 8–12 weeks. The typical timeline: weeks 1–2 bring GI symptom relief and slightly increased energy; weeks 4–8 show 20–30% reduction in depression/anxiety symptoms; weeks 8–12 yield 40–50% symptom improvement with stable mood and improved cognition. Full microbiome restoration may take 3–6 months of consistent effort. Individual results vary based on baseline health, adherence, and the severity of dysbiosis.
What is the best diet for gut-brain health?
The Mediterranean diet has the strongest evidence, reducing depression by 30–50% in clinical trials. Key components include: 5–9 daily servings of colorful vegetables, 2–3 fruits (especially berries), whole grains, legumes 3–4 times weekly, extra virgin olive oil, and fatty fish 2–3 times weekly. Fiber intake of 25–35g daily is critical for feeding bacteria that produce mood-enhancing SCFAs. Daily fermented foods (yogurt, kefir, sauerkraut) provide live probiotic cultures. Avoid processed foods, added sugars, artificial sweeteners, and excess alcohol.
How does the vagus nerve connect the gut and brain, and can you stimulate it naturally?
The vagus nerve is the longest cranial nerve, running from brainstem to abdomen, carrying 80% of signals from gut to brain. It transmits information about microbiome status, inflammation, and nutrients, directly influencing mood and cognition. Natural stimulation methods include: deep diaphragmatic breathing (5–6 breaths/minute, 10–20 minutes daily), cold exposure (30–60 second cold showers), singing and humming (vocal cord vibration), loving-kindness meditation, moderate exercise, and gargling vigorously. Medical VNS improves treatment-resistant depression by approximately 40%.
Does stress directly damage the gut microbiome?
Yes, chronic stress significantly damages gut health through multiple mechanisms. Cortisol increases intestinal permeability (leaky gut), alters microbiome composition by reducing beneficial Lactobacillus and Bifidobacterium species, and promotes overgrowth of pathogenic bacteria. The relationship is bidirectional — gut dysbiosis itself amplifies the stress response through HPA axis dysregulation, creating a vicious cycle. Stress management practices like meditation, yoga, deep breathing, and nature exposure have been shown to improve both gut microbiome composition and mental health outcomes.
What supplements help repair leaky gut for better mental health?
The most evidence-based supplements for gut barrier repair include: L-glutamine (5–10g daily, the primary fuel for intestinal cells that directly heals tight junctions), zinc picolinate (15–30mg daily for gut barrier integrity), collagen peptides (10–20g daily providing glycine and proline for lining repair), omega-3 fatty acids (2–4g EPA+DHA daily for anti-inflammatory support), and a multi-strain probiotic with psychobiotic strains (10–50 billion CFU daily). Prebiotic fiber (5–10g inulin or FOS) supports SCFA production that maintains barrier health.
How do antibiotics affect mental health through the gut?
Antibiotics can devastate beneficial gut bacteria populations, with full recovery sometimes taking months. This antibiotic-induced dysbiosis has been linked to increased risk of depression and anxiety through reduced neurotransmitter production, impaired SCFA generation, and compromised gut barrier function. When antibiotics are medically necessary, mitigate damage by taking a multi-strain probiotic during and after treatment (separated by 2–3 hours from antibiotic doses), consuming fermented foods daily, and increasing prebiotic fiber intake to support microbiome recovery.