gut health
How to Improve Gut Motility: 6 Evidence-Based Steps
Learn how to improve gut motility naturally with meal spacing, prokinetic foods and supplements, exercise, and vagus nerve stimulation. Evidence-based guide.
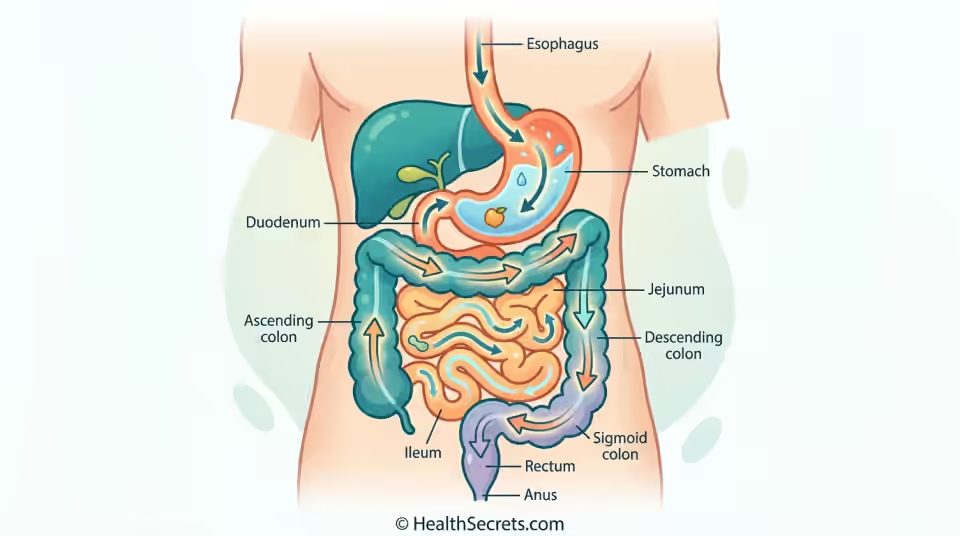
If you have ever felt uncomfortably bloated hours after a meal, struggled with chronic constipation, or been told you might have SIBO, there is a good chance your gut motility needs attention. Gut motility is the rhythmic, wave-like muscular activity that moves food from your mouth all the way to elimination — and when it stalls, problems pile up fast.
The good news? You do not need prescription drugs to get things moving again. Research shows that targeted diet changes, specific supplements, exercise, and simple vagus nerve techniques can measurably improve digestive transit. In this guide, you will learn a step-by-step protocol grounded in current gastroenterology research so you can take action today.
If you are new to digestive health, start with our complete gut health guide for foundational knowledge. For those dealing with bacterial overgrowth, our SIBO treatment guide covers the motility connection in depth.
- The migrating motor complex (MMC) is your gut's built-in housekeeper — it only activates during fasting, so spacing meals 4–5 hours apart is critical for preventing bacterial overgrowth.
- Ginger (1–2 g daily) is one of the most well-studied natural prokinetics, shown to accelerate gastric emptying by nearly 50% compared to placebo.
- Fiber intake of 25–35 g per day from whole foods adds bulk and stimulates intestinal contractions, but must be increased gradually with adequate water.
- Moderate aerobic exercise for 30 minutes most days directly stimulates colonic contractions and reduces transit time.
- Vagus nerve stimulation through deep breathing, cold exposure, and humming activates the parasympathetic "rest and digest" response essential for motility.
- Magnesium citrate (300–500 mg daily) draws water into the intestines and is well-established for improving constipation and colonic transit time.
- Stress is one of the most overlooked motility disruptors — chronic stress inhibits the parasympathetic nervous system and slows the MMC.
- Most natural motility strategies take 1–4 weeks for noticeable improvement, so consistency matters more than intensity.
What Do You Need to Know Before Improving Gut Motility?
Gut motility involves coordinated muscle contractions — peristalsis, segmentation, and mass movements — controlled by your enteric nervous system, often called the "second brain." Total digestive transit time ranges from 24 to 72 hours depending on diet, hydration, stress, and individual physiology. Understanding these basics helps you target the right interventions.
Your digestive tract uses three main types of movement.
- Peristalsis creates wave-like contractions that propel food forward.
- Segmentation mixes contents in the small intestine for better absorption.
- Mass movements are powerful colonic contractions that occur 1–3 times daily, moving waste toward the rectum.
The most important motility mechanism you have probably never heard of is the migrating motor complex (MMC). This cyclical pattern of electrical activity occurs only during fasting and sweeps undigested food, bacteria, and debris through your intestines every 90–120 minutes. Research published in the Journal of Smooth Muscle Research confirmed that the MMC cycle is mediated through the interaction between motilin and serotonin (5-HT) via a positive feedback mechanism [1]. When the MMC is disrupted — by frequent snacking, stress, or certain medications — bacterial overgrowth and bloating often follow. In fact, one study found that 86% of people with an abnormal MMC also had bacterial overgrowth [2] in the duodenum [2].
- Signs of poor gut motility include: chronic constipation (fewer than 3 bowel movements per week), bloating after meals, early satiety, nausea, belching, and undigested food in stool. Conditions like gastroparesis, SIBO, and IBS-C are all linked to impaired motility.
- Who this guide is for: Anyone experiencing sluggish digestion, chronic constipation, or post-meal bloating who wants to improve transit naturally before or alongside medical treatment. If you have IBS with constipation, these strategies can complement your existing plan.
- Expected timeline: Hydration and exercise improvements can show results within days. Dietary and supplement changes typically take 1–2 weeks. Full lifestyle optimization takes 4–8 weeks of consistent effort.
Step 1: How Do You Optimize Meal Spacing to Support the MMC?
Space your meals 4–5 hours apart and aim for a 12–14 hour overnight fast. The MMC only activates during fasting — every time you eat, even a small snack, the cleaning cycle resets. Protecting these fasting windows is the single most impactful habit for preventing bacterial buildup and improving intestinal transit.
The MMC completes a full cycle every 90–120 minutes and includes four phases. Phase 3 — the intense, rhythmic "sweep" lasting 5–15 minutes — is the critical housekeeping phase that clears debris from the small intestine [1]. Eating interrupts this cycle immediately.
How should you structure your daily eating schedule?
Aim for three meals per day with no snacking between them. A sample schedule might be breakfast at 8 AM, lunch at 12:30 PM, and dinner at 6 PM — giving your MMC ample fasting windows to complete its cleaning cycles. Finish dinner at least 3 hours before bed so your overnight fast reaches 12–14 hours, a period when MMC activity peaks [3].
What disrupts the MMC: Frequent eating or grazing, chronic stress, opioid medications, anticholinergics, gut infections, diabetes (nerve damage), and hypothyroidism.
Step 2: How Do You Build a Motility-Boosting Diet?
Focus on three pillars: adequate fiber (25–35 g daily), prokinetic foods like ginger and prunes, and proper hydration (at least 8 glasses of water per day). Fiber adds bulk and stimulates intestinal contractions, prokinetic foods directly accelerate transit, and water is essential for fiber to work effectively.
Which high-fiber foods improve digestive transit?
Both soluble fiber (oats, beans, apples, psyllium) and insoluble fiber (whole grains, vegetables, wheat bran) support motility. Soluble fiber softens stool while insoluble fiber adds bulk. Increase intake gradually — jumping from 10 g to 35 g overnight will cause gas and bloating. Add 5 g per week until you reach your target. For more on fiber's role, see our prebiotic foods guide.
Which prokinetic foods naturally stimulate gut motility?
| Food | Mechanism | Amount | Evidence |
|---|---|---|---|
| Ginger | Stimulates gastric emptying, antral contractions | 1–2 g fresh or supplement daily | Strong — multiple RCTs |
| Coffee | Stimulates colonic contractions via chlorogenic acid and caffeine | 1–2 cups morning | Moderate |
| Prunes | High fiber + sorbitol (natural osmotic laxative) | 3–6 prunes daily | Strong |
| Kiwi | Actinidin enzyme + fiber improves bowel frequency | 2 kiwis daily | Strong — RCTs |
| Fermented foods | Support SCFA-producing bacteria that stimulate motility | 1 serving daily | Moderate |
Healthy fats from olive oil, avocados, and fatty fish stimulate gallbladder contraction and bile release, which acts as a natural laxative. Aim for 1–2 tablespoons of extra virgin olive oil daily. For a deeper dive into gut-supportive eating, explore our gut-healing foods guide.
Step 3: Which Prokinetic Supplements Improve Gut Motility?
The most evidence-based natural prokinetics are ginger extract (1–2 g daily), artichoke leaf extract (300–640 mg three times daily), magnesium citrate (300–500 mg daily), and the herbal formula Iberogast (20 drops three times daily). Each targets different motility mechanisms, and they can be combined under practitioner guidance for stronger effects.
- Ginger (Zingiber officinale) is the standout performer. A clinical trial found that ginger reduced gastric half-emptying time from 26.7 minutes (placebo) to 13.1 minutes — nearly a 50% acceleration — while significantly increasing the frequency of antral contractions [4]. A 2023 study in patients with functional dyspepsia confirmed that ginger supplementation significantly improved gastric emptying and gastrointestinal motility [5].
- Artichoke leaf extract stimulates bile production and supports MMC activity. Clinical evidence shows it improves symptoms of IBS and functional dyspepsia by enhancing upper GI motility [6].
- 5-HTP (5-Hydroxytryptophan) at 50–200 mg daily is a serotonin precursor — and roughly 90% of your body's serotonin resides in the gut, where it plays a central role in MMC regulation [1]. The serotonin-gut health connection explains this mechanism in detail.
- Caution: Do not combine 5-HTP with SSRIs or other serotonergic medications.
- Magnesium citrate (300–500 mg daily) draws water into the intestines through osmotic action, softens stool, and relaxes smooth muscle. A randomized, double-blind, placebo-controlled trial demonstrated that magnesium significantly improved defecation status and shortened colonic transit time in patients with chronic constipation [7].
- Iberogast (STW 5) is a nine-herb formula with over 50 years of clinical use. Multiple controlled trials show it improves GI symptoms by 70–80%, with region-specific effects — relaxing the fundus while increasing antral contractions [8][9]. A 2024 meta-analysis confirmed STW 5-II significantly improves functional dyspepsia symptoms after 4 and 8 weeks of treatment [10].
- Triphala (500–1,000 mg before bed) is an Ayurvedic formula with gentle laxative and motility-supporting properties, best suited for long-term maintenance.
Step 4: How Does Exercise Improve Digestive Transit?
Moderate aerobic exercise for 30 minutes most days directly stimulates colonic contractions, increases blood flow to digestive organs, and activates the parasympathetic nervous system. A 10–15 minute walk after meals is one of the simplest and most effective motility interventions — it reduces post-meal bloating and accelerates gastric emptying.
What are the best exercises for gut motility?
- Aerobic exercise (walking, jogging, cycling, swimming) — 30 minutes most days at moderate intensity. This is the most well-studied exercise type for stimulating colonic motility.
- Yoga — twists compress and massage abdominal organs, forward folds compress the abdomen, and specific poses like Cat-Cow, Seated Twist, and Wind-Relieving Pose target digestion directly.
- Abdominal self-massage — 5–10 minutes daily in a clockwise direction (following the path of the colon) mechanically stimulates peristalsis.
- Deep diaphragmatic breathing — 5–10 minutes, 2–3 times daily. The diaphragm physically massages internal organs while activating vagal tone.
Step 5: How Do You Stimulate the Vagus Nerve for Better Gut Motility?
The vagus nerve is the longest cranial nerve and the primary controller of your parasympathetic "rest and digest" response. A 2026 systematic review confirmed that transcutaneous vagus nerve stimulation relieves abdominal pain, improves GI symptoms, and accelerates GI motility by enhancing vagal activity [11]. You can activate your vagus nerve at home with simple daily techniques.
Research using real-time MRI demonstrated that high-frequency transcutaneous auricular vagus nerve stimulation significantly increased gastric motility — specifically the amplitude of peristaltic waves — compared to low-frequency stimulation [12]. While clinical devices deliver precise frequencies, these at-home techniques activate the same nerve:
- Deep breathing: Slow diaphragmatic breathing using the 4-7-8 technique (inhale 4 seconds, hold 7, exhale 8) directly activates the parasympathetic response.
- Cold exposure: Splash cold water on your face or hold a cold pack to your neck for 1–2 minutes. Sudden cold stimulates the vagus nerve, slows heart rate, and can trigger digestive enzyme release.
- Singing, humming, and gargling: Vibrations from vocalization stimulate the vagus nerve through the laryngeal branches. Gargle water vigorously for 30 seconds, or hum for several minutes daily.
- Meditation and mindfulness: 10–20 minutes daily increases vagal tone and reduces the stress response that inhibits motility. Research shows tai chi and moderate interval training also enhance vagal modulation [13].
For a comprehensive look at how the brain and gut communicate, see our gut-brain axis guide.
Step 6: What Lifestyle Changes Support Healthy Digestive Transit?
Stress management, quality sleep (7–9 hours nightly), a consistent daily routine, and proper toilet posture create the foundation that makes every other motility strategy more effective. Chronic stress inhibits the parasympathetic nervous system and directly suppresses MMC activity, making it one of the most overlooked causes of sluggish digestion.
- Stress management is non-negotiable. Meditation, yoga, therapy, and journaling all activate the parasympathetic nervous system. Even 10 minutes of daily breathwork can shift your autonomic balance.
- Sleep optimization: The MMC is most active during sleep. Poor sleep disrupts motility and lowers your pain threshold, worsening symptoms. Aim for 7–9 hours on a consistent schedule.
- Establish a routine: Regular meal times and a consistent morning bathroom time train your digestive system. Never ignore the urge to defecate — doing so trains the colon to become less responsive over time.
- Proper toilet posture: Elevate your feet on a stool to approximate a squatting position. This straightens the anorectal angle and allows easier, strain-free elimination.
- Avoid motility inhibitors: Discuss with your doctor if you take opioids, anticholinergics, or excessive antacids — all of which significantly slow gut motility.
What Are the Most Common Mistakes That Slow Gut Motility?
The biggest mistakes people make are constant snacking (which prevents the MMC from ever completing a cleaning cycle), increasing fiber too quickly without enough water, and relying solely on supplements without addressing stress and meal timing. Fixing these three errors often produces more improvement than any single supplement.
- Snacking between meals: Even a handful of nuts resets your MMC cycle. Commit to defined meals only.
- Too much fiber too fast: Adding 20 g of fiber overnight causes gas, bloating, and can actually worsen constipation. Increase by 5 g per week.
- Dehydration: Fiber without water creates a concrete-like mass in your colon. Drink at least 8 glasses daily — more if you are increasing fiber.
- Ignoring stress: No amount of ginger capsules will overcome a chronically activated sympathetic nervous system. Address stress first.
- Expecting overnight results: Natural motility strategies take 1–4 weeks. Track progress with a symptom diary rather than giving up after 3 days.
- Combining 5-HTP with SSRIs: This combination risks serotonin syndrome. Always consult your prescriber before adding serotonergic supplements.
Is It Safe to Use Natural Prokinetics? When Should You Stop?
Most natural prokinetic supplements — ginger, artichoke, magnesium, triphala — have strong safety profiles at recommended doses. However, chronic or worsening motility issues can signal serious conditions like gastroparesis, hypothyroidism, diabetes-related neuropathy, or even intestinal obstruction, which require medical evaluation rather than self-treatment.
- See a doctor if you experience: constipation lasting more than 3 weeks despite interventions, severe abdominal pain, blood in stool, unexplained weight loss, vomiting, inability to pass gas, or symptoms that interfere with daily life.
- Medical conditions to rule out: hypothyroidism (check thyroid function), diabetes (can damage enteric nerves), Parkinson's disease, scleroderma, and SIBO. Common diagnostic tests include gastric emptying studies, colonic transit studies, anorectal manometry, and SIBO breath tests [14].
- Supplement safety notes: 5-HTP should never be combined with SSRIs or MAOIs. High-dose magnesium can cause diarrhea and should be avoided in kidney disease. Artichoke extract should be avoided with gallstones or bile duct obstruction. Always start one supplement at a time to identify what works and monitor for side effects.
What Should You Do First to Improve Gut Motility?
Start with the highest-impact, lowest-effort changes in Week 1, then layer in supplements and advanced techniques over the following weeks. This phased approach prevents overwhelm and lets you identify which strategies work best for your body.
Phase 1 — Foundation (Week 1):
- [ ] Space meals 4–5 hours apart — eliminate all snacking
- [ ] Increase water intake to 8+ glasses daily
- [ ] Take a 10–15 minute walk after each meal
- [ ] Begin 5 minutes of deep diaphragmatic breathing twice daily
- [ ] Establish a consistent morning bathroom routine
Phase 2 — Diet Optimization (Weeks 2–3):
- [ ] Gradually increase fiber to 25–35 g daily (add 5 g per week)
- [ ] Add prokinetic foods: ginger tea with meals, 3–6 prunes daily, 2 kiwis daily
- [ ] Include 1–2 tablespoons extra virgin olive oil daily
- [ ] Start overnight fast of 12–14 hours
Phase 3 — Targeted Supplements (Weeks 3–4):
- [ ] Add ginger extract (1–2 g daily) or Iberogast (20 drops 3x daily)
- [ ] Consider magnesium citrate (300–500 mg) in the evening
- [ ] Add artichoke extract if bile flow is a concern
- [ ] Start daily vagus nerve exercises (cold water splash, humming, gargling)
Phase 4 — Advanced Optimization (Weeks 4–8):
- [ ] Add 30 minutes of moderate aerobic exercise most days
- [ ] Incorporate yoga for digestion 2–3 times weekly
- [ ] Begin daily abdominal self-massage (5–10 minutes, clockwise)
- [ ] Address stress with meditation, therapy, or journaling
- [ ] Optimize sleep to 7–9 hours nightly
References
- Takahashi T. Mechanism of interdigestive migrating motor complex. J Neurogastroenterol Motil. 2012;18(3):246-257. Source
- Vantrappen G, Janssens J, Hellemans J, Ghoos Y. The interdigestive motor complex of normal subjects and patients with bacterial overgrowth of the small intestine. J Clin Invest. 1977;59(6):1158-1166. Source
- National Institute of Diabetes and Digestive and Kidney Diseases. Constipation. Source
- Wu KL, Rayner CK, Chuah SK, et al. Effects of ginger on gastric emptying and motility in healthy humans. Eur J Gastroenterol Hepatol. 2008;20(5):436-440. Source
- Alizadeh-Navaei R, et al. The effect of ginger supplementation on the improvement of dyspeptic symptoms in patients with functional dyspepsia. Caspian J Intern Med. 2023;14(4):644-652. Source
- Malfertheiner P. STW 5 (Iberogast) therapy in gastrointestinal functional disorders. Dig Dis. 2017;35(Suppl 1):25-29. Source
- Mori S, et al. A randomized double-blind placebo-controlled trial on the effect of magnesium oxide in patients with chronic constipation. J Neurogastroenterol Motil. 2019;25(4):563-575. Source
- Melzer J, et al. STW 5 (Iberogast) — a safe and effective standard in the treatment of functional gastrointestinal disorders. Wien Med Wochenschr. 2004;154(21-22):528-534. Source
- Raedsch R, et al. Early onset of efficacy in patients with functional and motility-related gastrointestinal disorders: a noninterventional study with Iberogast. Wien Med Wochenschr. 2018;168(4):89-98. Source
- Müller M, et al. Efficacy and safety of STW 5-II for functional dyspepsia treatment: a patient data-based meta-analysis. BMC Gastroenterol. 2024;24:191. Source
- Chen Y, et al. Transcutaneous vagal nerve stimulation for gastrointestinal disorders. J Clin Med. 2025. Source
- Teckentrup V, et al. Transcutaneous auricular vagus nerve stimulation influences gastric motility: a randomized, double-blind trial in healthy individuals. Brain Stimul. 2021;14(5):1126-1132. Source
Frequently asked questions
What is the migrating motor complex and why does it matter for gut motility?
The migrating motor complex (MMC) is a cyclical pattern of electrical activity that sweeps undigested food, bacteria, and debris through your intestines during fasting. It completes a full cycle every 90–120 minutes and is often called the "intestinal housekeeper." When the MMC is disrupted — by frequent snacking, stress, or certain medications — bacteria can accumulate in the small intestine, leading to SIBO, bloating, and constipation. Supporting your MMC by spacing meals 4–5 hours apart and fasting 12–14 hours overnight is one of the most effective strategies for improving digestive transit.
How long does it take for natural prokinetic supplements to improve gut motility?
Most natural prokinetic supplements take 1–4 weeks of consistent daily use to produce noticeable improvements. Ginger and magnesium citrate tend to show effects within the first week, while herbal formulas like Iberogast and Triphala typically require 2–4 weeks. Lifestyle changes like meal spacing and exercise can produce improvements within days. The key is consistency — track your symptoms with a diary and give each intervention at least 3–4 weeks before evaluating its effectiveness.
Can you take ginger and Iberogast together for gut motility?
Yes, ginger and Iberogast can generally be taken together because they work through complementary mechanisms. Ginger primarily accelerates gastric emptying through antral contractions, while Iberogast has region-specific effects across the entire upper GI tract. However, it is always best to introduce one supplement at a time so you can identify what works for you and monitor for any side effects. Consult your healthcare provider if you are on medications.
Does exercise really help with constipation and slow digestion?
Yes, moderate aerobic exercise is one of the most well-established interventions for improving gut motility. Walking, jogging, cycling, and swimming for 30 minutes most days directly stimulate colonic contractions and reduce transit time. Even a short 10–15 minute walk after meals can significantly reduce post-meal bloating and accelerate gastric emptying. The effect is partly mechanical (abdominal movement) and partly neurological (exercise activates the parasympathetic nervous system).
Is it safe to take 5-HTP for gut motility if you are on antidepressants?
No, you should not combine 5-HTP with SSRIs, SNRIs, MAOIs, or other serotonergic medications without medical supervision. This combination can cause serotonin syndrome, a potentially dangerous condition. Since 5-HTP increases serotonin production in the gut and brain, it can interact with medications that also raise serotonin levels. If you take antidepressants and want to support your MMC, consider ginger or Iberogast instead, which work through non-serotonergic mechanisms.
How much water should you drink to improve gut motility?
Aim for at least 8 glasses (64 ounces) of water per day, and more if you are increasing your fiber intake, exercising, or in a hot climate. Water is essential for fiber to work effectively — without adequate hydration, fiber can actually worsen constipation by creating bulky, hard-to-pass stool. Sip water throughout the day rather than drinking large amounts only at meals.
What is the best time of day to take magnesium for constipation?
Taking magnesium in the evening, about 1–2 hours before bedtime, is often the most effective timing for constipation relief. Magnesium's muscle-relaxing properties also support sleep quality, and the overnight period allows the osmotic effect to draw water into the intestines. This typically produces a bowel movement in the morning. Start with 300 mg and increase to 500 mg if needed, but reduce the dose if you experience diarrhea.
Can stress really cause constipation and slow gut motility?
Absolutely. Chronic stress activates the sympathetic "fight or flight" nervous system, which directly suppresses the parasympathetic "rest and digest" response needed for normal gut motility and MMC function. Stress also increases inflammatory cytokines in the gut and can alter the microbiome. This is why stress management — through meditation, deep breathing, yoga, or therapy — is not optional when addressing motility issues. It is a foundational intervention.
How do you stimulate the vagus nerve at home for better digestion?
The simplest home vagus nerve stimulation techniques include deep diaphragmatic breathing (the 4-7-8 technique), splashing cold water on your face, gargling water vigorously for 30 seconds, humming or singing, and practicing meditation for 10–20 minutes daily. These techniques activate the parasympathetic nervous system, which controls gut motility. Research confirms that vagus nerve stimulation accelerates GI motility by enhancing parasympathetic activity.
When should you see a doctor about slow gut motility?
See a doctor if constipation lasts more than 3 weeks despite interventions, if you experience severe abdominal pain, blood in stool, unexplained weight loss, vomiting, inability to pass gas, or symptoms that interfere with daily life. These can signal serious conditions like gastroparesis, intestinal obstruction, thyroid disorders, or neurological diseases. Your doctor may order gastric emptying studies, colonic transit tests, or SIBO breath tests to identify the underlying cause.