gut health
H. Pylori Natural Treatment: Evidence-Based Protocol
Discover evidence-based natural treatments for H. pylori including mastic gum, manuka honey, probiotics, and sulforaphane. Complete protocol with dosages and research.
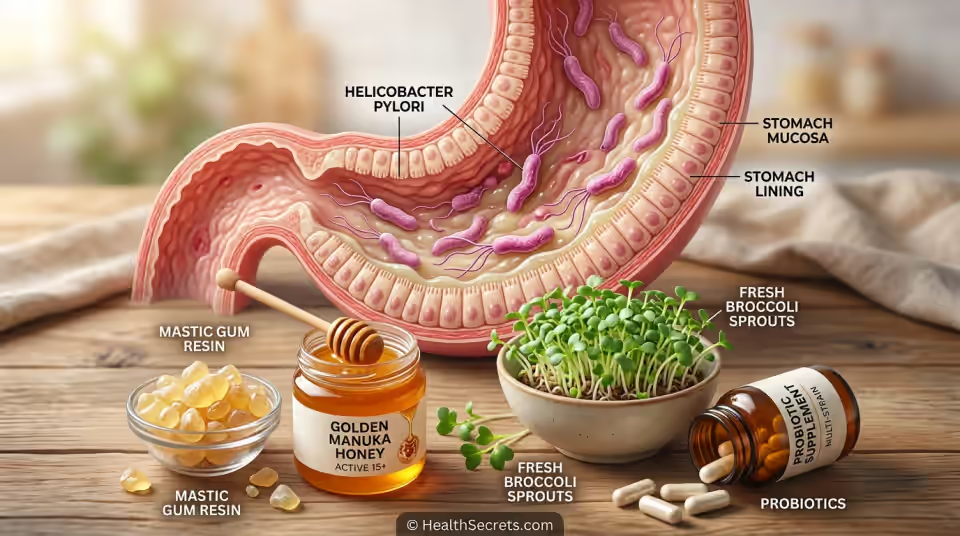
If you've been diagnosed with Helicobacter pylori — or suspect it's behind your chronic stomach discomfort — you're far from alone. This spiral-shaped bacterium quietly inhabits the stomachs of over 4 billion people worldwide, and while many carriers never develop symptoms, those who do can face relentless burning pain, nausea, bloating, and a significantly elevated risk of peptic ulcers and even gastric cancer.
Conventional treatment relies on aggressive antibiotic cocktails known as triple or quadruple therapy. These regimens work — but with rising antibiotic resistance rates and uncomfortable side effects like diarrhea, nausea, and gut dysbiosis, more people are asking whether natural approaches can play a meaningful role. The good news: a growing body of peer-reviewed research says yes.
From mastic gum and manuka honey to sulforaphane from broccoli sprouts, probiotics like Lactobacillus reuteri and Saccharomyces boulardii, and biofilm-disrupting agents like NAC and lactoferrin, natural compounds are showing real promise — both as standalone support and as powerful adjuncts to standard therapy.
If you're new to gut health, start with our complete guide to gut health. For foundational healing strategies, explore gut-healing foods and healing leaky gut syndrome.
- H. pylori infects approximately 50% of the global population and is the leading cause of peptic ulcers and a major risk factor for gastric cancer
- Antibiotic resistance is rising sharply — conventional triple therapy eradication rates have dropped below 80% in many regions, making natural adjuncts increasingly valuable
- Mastic gum (1,000–3,000 mg/day) demonstrates bactericidal activity against H. pylori in multiple clinical studies, with one trial showing a 92.2% eradication rate when combined with standard therapy
- Manuka honey (UMF 15+/MGO 514+) inhibits H. pylori growth through methylglyoxal and suppresses inflammatory pathways including NF-κB
- Sulforaphane from broccoli sprouts (70g fresh daily or 400–800 mcg supplement) reduces H. pylori colonization and gastric inflammation
- Probiotics — especially Lactobacillus reuteri and Saccharomyces boulardii — improve eradication rates above 90% when added to standard therapy and significantly reduce treatment side effects
- Lactoferrin enhances H. pylori eradication by up to 24 percentage points when added to conventional regimens
- Berberine-containing quadruple therapy is non-inferior to bismuth-based quadruple therapy with fewer adverse effects
- A comprehensive natural protocol spans 8–12 weeks across four phases: preparation, active treatment, healing, and maintenance
- Natural approaches work best as complements to conventional treatment — never delay medical care for serious symptoms like vomiting blood or black stools
What Is H. Pylori and Why Is It So Common?
Helicobacter pylori is a gram-negative, spiral-shaped bacterium uniquely adapted to survive in the harsh acidic environment of the human stomach. It infects approximately 4.4 billion people worldwide — roughly 50% of the global population — making it one of the most prevalent chronic bacterial infections in human history.
H. pylori was famously identified in 1982 by Australian researchers Barry Marshall and Robin Warren, who won the Nobel Prize in Physiology or Medicine in 2005 for their discovery. Marshall famously drank a Petri dish of H. pylori culture to prove the bacterium caused gastritis — and it did.
How Does H. Pylori Survive in Stomach Acid?
H. pylori produces an enzyme called urease that converts urea into ammonia, creating an alkaline microenvironment around the bacterium that neutralizes stomach acid. This allows it to burrow into the protective mucus lining of the stomach wall, where it establishes chronic colonization. Once embedded, H. pylori triggers persistent low-grade inflammation that can last decades if untreated.
Who Does H. Pylori Affect?
Infection rates vary dramatically by geography and socioeconomic factors:
- Developing countries: 70–90% prevalence
- Developed countries: 20–50% prevalence
- Childhood acquisition: Most infections are acquired before age 10 through oral-oral or fecal-oral transmission
- Risk factors: Crowded living conditions, lack of clean water, poor sanitation, close contact with infected family members
Importantly, most H. pylori carriers remain asymptomatic. Only 10–20% develop clinically significant disease, but when problems arise, they can be severe.
What Causes H. Pylori Infection and Who Is Most at Risk?
H. pylori spreads primarily through person-to-person contact via oral-oral or fecal-oral routes, with most infections acquired during childhood. Contaminated water and food are significant transmission vectors, particularly in regions with limited sanitation infrastructure. Understanding the root causes and risk factors helps guide both treatment and prevention.
Transmission Routes
- Oral-oral contact: Sharing utensils, kissing, or exposure to vomit
- Fecal-oral route: Contaminated water supplies, unwashed produce
- Intrafamilial spread: Infected parents or siblings transmitting to children
- Iatrogenic transmission: Inadequately sterilized endoscopic equipment (rare)
Key Risk Factors
| Risk Factor | Impact | Notes |
|---|---|---|
| Crowded living conditions | High | Increases person-to-person transmission |
| Low socioeconomic status | High | Correlates with sanitation access |
| Developing country residence | High | 70–90% prevalence vs. 20–50% in developed nations |
| Childhood exposure | High | Most infections acquired before age 10 |
| Family history of H. pylori | Moderate | Intrafamilial clustering is well-documented |
What Happens When H. Pylori Causes Problems?
When H. pylori triggers active disease, the complications can be serious:
- Peptic ulcers — Stomach and duodenal ulcers (present in 15–20% of infected individuals)
- Chronic gastritis — Persistent stomach lining inflammation
- Gastric cancer — H. pylori is classified as a Group 1 carcinogen by the WHO (3–6x increased risk)
- MALT lymphoma — A rare type of stomach cancer
- Vitamin B12 deficiency — Reduced absorption from chronic inflammation
- Iron deficiency anemia — From chronic low-grade gastric bleeding
What Are the Symptoms of H. Pylori Infection?
Most H. pylori carriers experience no symptoms at all. However, when the infection causes gastritis or peptic ulcers, symptoms range from mild discomfort to severe, potentially life-threatening complications. Recognizing these signs early allows prompt testing and treatment before serious damage occurs.
Common Digestive Symptoms
- Burning or gnawing upper abdominal pain — Often described as a dull ache between meals or at night
- Pain that improves with eating or antacids — A hallmark of duodenal ulcers
- Bloating and excessive belching
- Nausea — Especially on an empty stomach
- Loss of appetite and early satiety
- Unintentional weight loss
- Acid reflux or heartburn
Warning Signs Requiring Immediate Medical Attention
- Vomiting blood (hematemesis) — Bright red or coffee-ground appearance
- Black, tarry stools (melena) — Indicates upper GI bleeding
- Severe, sudden abdominal pain — May indicate ulcer perforation
- Persistent vomiting — Could indicate gastric outlet obstruction
- Unexplained anemia — Fatigue, pallor, shortness of breath from chronic bleeding
Silent Carriers
Up to 80–90% of infected individuals remain completely asymptomatic. This makes H. pylori a "silent" infection that can persist for decades, gradually increasing the risk of gastric cancer and other complications without any overt warning signs.
How Is H. Pylori Diagnosed?
Accurate diagnosis is the essential first step before beginning any treatment protocol — natural or conventional. Several reliable testing methods exist, each with specific advantages depending on the clinical situation. A 40–60 word direct answer: H. pylori can be diagnosed through non-invasive tests including the urea breath test and stool antigen test, or through invasive endoscopy with biopsy. The urea breath test and stool antigen test are preferred for initial diagnosis due to their high accuracy and convenience.
Non-Invasive Tests
| Test | Accuracy | Best For | Notes |
|---|---|---|---|
| Urea Breath Test (UBT) | 95–97% | Initial diagnosis and post-treatment confirmation | Gold standard non-invasive test |
| Stool Antigen Test | 92–96% | Initial diagnosis, children, follow-up | Widely available, cost-effective |
| Blood Antibody Test | 80–90% | Screening only | Cannot distinguish past vs. current infection |
Invasive Tests (Endoscopy)
- Rapid urease test (CLO test) — Biopsy placed in urea solution; color change indicates H. pylori
- Histology — Tissue examination under microscope; most definitive
- Culture — Allows antibiotic sensitivity testing; important for resistant cases
When Should You Get Tested?
- Persistent upper abdominal pain or burning
- Family history of stomach cancer
- Unexplained iron deficiency anemia
- Before starting long-term NSAID therapy
- After completing eradication treatment (wait 4–6 weeks post-treatment)
Important: Stop proton pump inhibitors (PPIs) at least 2 weeks and antibiotics at least 4 weeks before breath or stool testing to avoid false negatives.
What Are the Conventional Treatment Options for H. Pylori?
Standard H. pylori treatment involves combination antibiotic regimens designed to overcome the bacterium's ability to resist single-agent therapy. The 2024 American College of Gastroenterology (ACG) guidelines recommend bismuth-based quadruple therapy as the preferred first-line treatment, replacing the previously standard clarithromycin-based triple therapy due to rising resistance.
Current Standard Regimens
First-Line: Bismuth Quadruple Therapy (14 days)
- Proton pump inhibitor (PPI) twice daily
- Bismuth subsalicylate four times daily
- Metronidazole three times daily
- Tetracycline four times daily
- Eradication rate: 85–90%
Alternative: Vonoprazan-Amoxicillin Dual Therapy (14 days)
- Vonoprazan (potassium-competitive acid blocker) twice daily
- Amoxicillin three times daily
- Eradication rate: 84–90%
Alternative: Rifabutin Triple Therapy (14 days)
- PPI twice daily
- Amoxicillin three times daily
- Rifabutin 150 mg daily
- Eradication rate: 78–84%
Limitations of Conventional Treatment
- Antibiotic resistance: Clarithromycin resistance exceeds 15–20% in many regions, dramatically reducing efficacy
- Side effects: Diarrhea (30%), nausea (20%), metallic taste, abdominal pain, gut dysbiosis
- Gut microbiome disruption: Broad-spectrum antibiotics devastate beneficial bacteria
- Treatment failure: 15–25% of patients fail first-line therapy
- Recurrence: 5–10% annual reinfection rate
These limitations create a compelling rationale for integrating natural antimicrobials — either alongside conventional treatment to boost eradication rates and reduce side effects, or as part of a comprehensive natural protocol.
What Natural Approaches Support H. Pylori Treatment?
Research demonstrates that several natural compounds possess genuine anti-H. pylori activity and can significantly improve outcomes when used alongside conventional therapy. The strongest evidence supports mastic gum, manuka honey, sulforaphane, specific probiotic strains, lactoferrin, and berberine — each targeting H. pylori through different mechanisms.
Does Mastic Gum Kill H. Pylori?
Mastic gum (Pistacia lentiscus resin) is one of the most well-studied natural antimicrobials against H. pylori. A landmark letter published in the New England Journal of Medicine demonstrated that even low doses of mastic gum exhibit bactericidal activity against H. pylori in vitro. More recently, a randomized controlled trial of 180 patients found that mastic gum combined with triple therapy achieved a 92.2% eradication rate compared to only 63.3% with antibiotics alone — a statistically significant improvement (p < 0.001).
The active compounds — triterpenic acids including isomasticadienolic acid — disrupt H. pylori cell membranes and reduce gastric inflammation. A pilot study using pure mastic gum at 1,050 mg three times daily for 14 days confirmed in vivo bactericidal activity, though eradication as monotherapy was modest.
- Dosage: 1,000–3,000 mg daily in divided doses
- Duration: 4–8 weeks minimum
- Timing: Between meals on an empty stomach
- Best use: As adjunct to conventional therapy for maximum benefit
Can Manuka Honey Help Fight H. Pylori?
Manuka honey with high methylglyoxal (MGO) content demonstrates direct antibacterial activity against H. pylori. Research published in Molecular Mechanisms of Natural Honey showed that manuka honey inhibits H. pylori-induced NF-κB and AP-1 activation in gastric cells in a dose-dependent manner, while downregulating COX-2 expression — key inflammatory pathways involved in H. pylori pathogenesis.
Earlier research published in the Journal of the Royal Society of Medicine confirmed that all H. pylori isolates tested were sensitive to 20% manuka honey solutions. While manuka honey alone may not eradicate H. pylori, it provides meaningful antimicrobial and anti-inflammatory support.
- Quality: UMF 15+ or MGO 514+ (must be UMFHA-certified)
- Dosage: 1 tablespoon three times daily
- Timing: Before meals on an empty stomach
- Duration: 4–8 weeks
Do Broccoli Sprouts Reduce H. Pylori Colonization?
Sulforaphane, the isothiocyanate compound concentrated in broccoli sprouts, has demonstrated potent anti-H. pylori activity in both laboratory and human studies. Clinical research shows that consuming 70g of fresh broccoli sprouts daily for 8 weeks significantly reduces H. pylori colonization markers and gastric inflammation. Sulforaphane works by directly killing H. pylori and activating the Nrf2 antioxidant pathway, which protects stomach cells from oxidative damage.
- Fresh sprouts: 70g daily (highest sulforaphane content)
- Supplement: 400–800 mcg sulforaphane standardized extract
- Duration: 8 weeks minimum
- Tip: Eat raw for maximum sulforaphane activation; cooking reduces potency
Which Probiotics Help With H. Pylori?
Probiotics represent one of the strongest evidence-based natural adjuncts for H. pylori treatment. A 2024 meta-analysis confirmed that Lactobacillus reuteri supplementation significantly improves eradication rates, reduces overall side effects, and relieves gastrointestinal symptoms during treatment. A 2023 randomized, double-blind trial demonstrated that L. reuteri DSM 17648 as an adjunct boosted eradication rates above 90%.
Saccharomyces boulardii has been extensively studied in multi-center prospective trials, showing significant reduction in antibiotic-associated diarrhea severity and duration during H. pylori eradication therapy. Critically, as a beneficial yeast, S. boulardii is unaffected by antibiotics and can be taken simultaneously.
Key strains for H. pylori:
- Lactobacillus reuteri DSM 17648 — Directly binds to and co-aggregates with H. pylori
- Saccharomyces boulardii — Reduces antibiotic side effects; safe during antibiotic use
- Lactobacillus rhamnosus GG — Enhances eradication, reduces diarrhea
- Bifidobacterium lactis BB-12 — Improves treatment tolerance and gut barrier function
- Dosage: 10–50 billion CFU daily
- Timing: 2 hours away from antimicrobials (except S. boulardii which can be taken with antibiotics)
- Duration: During treatment and 3 months after
Does Lactoferrin Enhance H. Pylori Eradication?
Lactoferrin, an iron-binding glycoprotein found in milk, demonstrates direct antimicrobial activity against H. pylori — including antibiotic-resistant strains. A randomized controlled trial showed that adding bovine lactoferrin to triple therapy increased eradication rates from 70.3% to 85.6%, while adding it to sequential therapy boosted rates from 82.8% to 94.5%. The mechanism involves iron sequestration (depriving H. pylori of essential iron) plus direct membrane disruption.
- Dosage: 200–400 mg daily
- Duration: 4–8 weeks
- Best combined with: Probiotics and conventional therapy
Can You Prevent H. Pylori Infection and Reinfection?
While no vaccine exists against H. pylori, practical hygiene measures and ongoing gut health maintenance can significantly reduce the risk of initial infection and — importantly — reinfection after successful treatment. Annual reinfection rates range from 2–5% in developed countries but can exceed 10% in high-prevalence regions.
Preventing Initial Infection
- Drink clean, treated water — especially when traveling to high-prevalence regions
- Wash hands thoroughly before eating and after using the bathroom
- Avoid sharing utensils, cups, and toothbrushes with potentially infected individuals
- Wash fruits and vegetables thoroughly before consumption
- Ensure food is properly cooked — especially in areas with questionable food safety
Preventing Reinfection After Treatment
- Test and treat household contacts — Intrafamilial transmission is a major source of reinfection
- Maintain robust gut microbiome health with probiotics and fermented foods
- Support stomach acid production — Adequate stomach acid is a natural defense against pathogens
- Continue anti-inflammatory diet rich in gut-healing foods
- Manage stress — Chronic stress impairs immune surveillance and stomach lining integrity
- Avoid unnecessary NSAIDs — These damage the protective mucus layer
- Confirm eradication — Always retest 4–6 weeks after completing treatment
When Should You See a Doctor for H. Pylori?
While natural approaches can play a valuable complementary role, H. pylori is a serious bacterial infection with potentially life-threatening complications. Certain situations demand immediate medical evaluation. Never delay conventional treatment when warning signs are present, and always work with a healthcare provider when managing H. pylori.
Seek Immediate Medical Care If You Experience:
- Vomiting blood — Bright red or dark, coffee-ground appearance
- Black, tarry stools — Indicates active gastrointestinal bleeding
- Severe, sudden abdominal pain — Possible ulcer perforation (surgical emergency)
- Fainting or lightheadedness with GI symptoms — May indicate significant blood loss
- Rapid, unexplained weight loss
Schedule a Medical Appointment If:
- Burning stomach pain persists for more than 2 weeks
- Over-the-counter antacids provide only temporary relief
- You have a family history of stomach cancer
- You've completed a natural protocol but symptoms persist
- You need confirmation testing (breath test or stool antigen)
- You've failed a previous eradication attempt
Integrative Approach: Best of Both Worlds
The most effective strategy combines conventional medicine with evidence-based natural support:
- Get properly diagnosed (urea breath test or stool antigen)
- Complete recommended antibiotic therapy (bismuth quadruple or as prescribed)
- Add natural adjuncts (S. boulardii during antibiotics, L. reuteri and mastic gum alongside)
- Support gut recovery with probiotics, L-glutamine, and bone broth post-treatment
- Confirm eradication with follow-up testing at 4–6 weeks
- Maintain prevention through diet and lifestyle
For broader natural remedy approaches, explore our natural remedies guide and fighting inflammation naturally.
What Should You Do First If You Suspect H. Pylori?
If you're experiencing symptoms of H. pylori infection, a structured step-by-step approach ensures you address the infection safely and effectively. Start with proper diagnosis, then layer in evidence-based natural support alongside any recommended conventional treatment.
Phase 1: Diagnosis and Preparation (Week 1)
- [ ] Schedule H. pylori testing (urea breath test or stool antigen preferred)
- [ ] Stop PPIs 2 weeks before testing and antibiotics 4 weeks before
- [ ] Begin anti-inflammatory diet — remove processed foods, sugar, alcohol, NSAIDs
- [ ] Start probiotics (Saccharomyces boulardii 5–10 billion CFU daily)
- [ ] Begin zinc carnosine (75 mg twice daily) for stomach lining protection
Phase 2: Active Treatment (Weeks 2–9)
- [ ] Follow prescribed conventional therapy if recommended by your doctor
- [ ] Add primary natural antimicrobials: mastic gum (1g three times daily), broccoli sprouts (70g daily), manuka honey (1 tbsp three times daily before meals)
- [ ] Add supporting agents: berberine (500 mg twice daily), lactoferrin (200 mg twice daily), NAC (600 mg twice daily)
- [ ] Continue probiotics: L. reuteri and S. boulardii (2 hours from antibiotics, except S. boulardii)
- [ ] Follow the H. pylori-friendly diet strictly
Phase 3: Gut Healing (Weeks 10–12)
- [ ] Taper antimicrobials gradually
- [ ] Increase probiotic diversity — add multi-strain formula
- [ ] Focus on gut-healing nutrients: L-glutamine, bone broth, zinc carnosine
- [ ] Slowly reintroduce previously restricted foods one at a time
- [ ] Continue anti-inflammatory diet as baseline
Phase 4: Confirmation and Maintenance (Week 13+)
- [ ] Retest for H. pylori (urea breath test or stool antigen) at 4–6 weeks post-treatment
- [ ] Continue probiotics for at least 3 months total
- [ ] Maintain anti-inflammatory diet and lifestyle habits
- [ ] Test and treat household contacts if positive
- [ ] Monitor for symptom recurrence
References
- Al Somal, N., et al. "Susceptibility of Helicobacter pylori to the Antibacterial Activity of Manuka Honey." Journal of the Royal Society of Medicine, 87(1), 1994. Source
- Huwez, F.U., et al. "Mastic Gum Kills Helicobacter pylori." New England Journal of Medicine, 339(26), 1998. Source
- Dabos, K.J., et al. "The effect of mastic gum on Helicobacter pylori: A randomized pilot study." Phytomedicine, 17(3-4), 2010. Source
- Kottakis, F., et al. "In Vitro and In Vivo Activities of Chios Mastic Gum Extracts against Helicobacter pylori." Antimicrobial Agents and Chemotherapy, 50(5), 2006. Source
- El-Hashash, M., et al. "Assessing the Efficacy of a Modified Triple Drug Regimen Supplemented with Mastic Gum in the Eradication of Helicobacter pylori." American Journal of Clinical Pathology, 160(S1), 2023. Source
- Mahalanobish, S., et al. "Molecular Mechanisms of Natural Honey Against H. pylori Infection." Archives of Medical Research, 47(3), 2016. Source
- Nair, M., et al. "The Antibacterial Activity of Honey on Helicobacter pylori." Sultan Qaboos University Medical Journal, 11(1), 2011. Source
- Zhang, L., et al. "The effects and mechanisms of natural products on Helicobacter pylori eradication." Frontiers in Cellular and Infection Microbiology, 14, 2024. Source
- Ismail, N.I., et al. "Probiotic containing Lactobacillus reuteri DSM 17648 as an adjunct treatment for Helicobacter pylori infection." Helicobacter, 28(1), 2023. Source
- Emara, M.H., et al. "Lactobacillus reuteri in management of Helicobacter pylori infection in dyspeptic patients." Therapeutic Advances in Gastroenterology, 7(1), 2014. Source
- Zhu, X., et al. "Lactobacillus reuteri compared with placebo as an adjuvant in Helicobacter pylori eradication therapy: A meta-analysis of randomized controlled trials." Frontiers in Nutrition, 11, 2024. Source
- Poonyam, P., et al. "Investigating the effect of quadruple therapy with Saccharomyces boulardii or Lactobacillus reuteri." BMC Gastroenterology, 22(1), 2022. Source
Frequently asked questions
Can you cure H. pylori without antibiotics using only natural remedies?
Natural remedies alone can reduce H. pylori colonization but complete eradication without antibiotics is less reliable, with natural-only protocols achieving roughly 30–50% eradication compared to 85–90% with conventional quadruple therapy. Research shows natural compounds work best as adjuncts — mastic gum combined with triple therapy achieved 92.2% eradication versus 63.3% with antibiotics alone. For confirmed H. pylori infection, the safest approach combines conventional treatment with natural support.
How long does it take to get rid of H. pylori naturally?
A comprehensive natural protocol typically spans 8–12 weeks across four phases. Symptom improvement often begins within 2–3 weeks, but complete eradication requires sustained treatment. Conventional antibiotic therapy takes 10–14 days but is followed by weeks of gut recovery. When combining natural and conventional approaches, plan for the full 12-week protocol including the healing and maintenance phases.
Does mastic gum actually kill H. pylori?
Yes, mastic gum has demonstrated bactericidal activity against H. pylori both in vitro and in vivo. A New England Journal of Medicine study confirmed mastic gum's anti-H. pylori properties, and a subsequent randomized controlled trial showed mastic gum combined with triple therapy achieved a 92.2% eradication rate. As monotherapy, mastic gum reduces H. pylori loads but typically doesn't achieve complete eradication.
What type of manuka honey kills H. pylori?
Manuka honey with a UMF rating of 15+ (corresponding to MGO 514+) has demonstrated antibacterial activity against H. pylori in laboratory studies. The active compound methylglyoxal (MGO) is responsible for the antimicrobial effect. Lower-grade manuka or regular honey lacks sufficient MGO concentration. Always verify UMF certification from the Unique Manuka Factor Honey Association to ensure authenticity.
Which probiotic is best for H. pylori treatment?
Lactobacillus reuteri DSM 17648 and Saccharomyces boulardii have the strongest clinical evidence for H. pylori support. A 2024 meta-analysis confirmed L. reuteri improves eradication rates and reduces side effects. S. boulardii is uniquely valuable because it can be taken during antibiotic therapy without being killed. Together, they provide complementary benefits — enhanced eradication and reduced adverse effects.
Can H. pylori come back after successful treatment?
Yes, reinfection occurs in approximately 2–5% of cases per year in developed countries and up to 10%+ in high-prevalence regions. The primary source of reinfection is untreated household contacts. To minimize recurrence, test and treat family members, maintain good hygiene practices, support ongoing gut health with probiotics and anti-inflammatory diet, and confirm eradication with follow-up testing.
Is it safe to take berberine for H. pylori alongside antibiotics?
Clinical research supports berberine as safe and effective alongside standard H. pylori therapy. A meta-analysis of 13 randomized trials found berberine-containing quadruple therapy significantly improved eradication rates and reduced side effects compared to standard triple therapy alone. However, berberine can interact with certain medications including metformin and cyclosporine, so always consult your healthcare provider before combining.
How do you know if H. pylori treatment worked?
Confirm eradication with a urea breath test or stool antigen test at least 4 weeks after completing antibiotic therapy. Stop PPIs 2 weeks before testing to avoid false negatives. Blood antibody tests are unreliable for confirming eradication because antibodies can remain positive for months after successful treatment. Symptom resolution alone is insufficient — asymptomatic infection is common.
What foods should you avoid with H. pylori infection?
Avoid foods that irritate the stomach lining or promote inflammation: spicy foods, acidic foods (citrus, tomatoes), coffee, alcohol, carbonated beverages, refined sugar, processed meats, fried foods, and NSAIDs like ibuprofen. Focus instead on anti-inflammatory foods, broccoli sprouts, fermented foods, bone broth, and manuka honey. Eating smaller, more frequent meals also reduces stomach irritation.
Does lactoferrin help with antibiotic-resistant H. pylori?
Yes, research demonstrates that bovine lactoferrin has direct antimicrobial activity against antibiotic-resistant H. pylori strains, with minimum inhibitory concentrations of 1.25–5 mg/mL. In clinical trials, adding lactoferrin to standard therapy improved eradication rates by up to 24 percentage points. Lactoferrin works through iron sequestration and membrane disruption — mechanisms unrelated to antibiotic resistance pathways.