detox
Heavy Metal Detox: Safe Chelation Strategies That Actually Work (2026)
Learn evidence-based heavy metal detox strategies including proper testing, natural chelation support with NAC and chlorella, and when medical chelation is needed. Step-by-step guide.
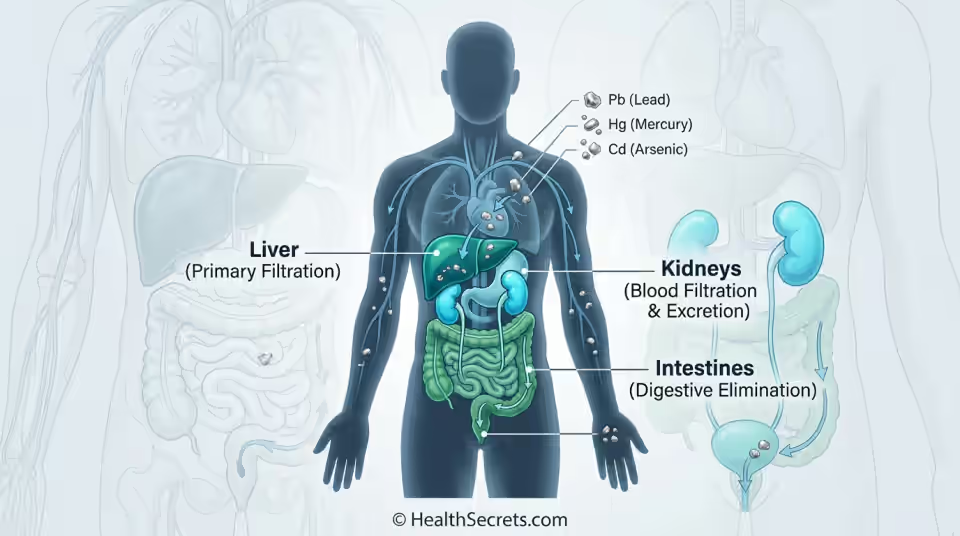
Heavy metals are everywhere — in contaminated water, old paint, dental fillings, certain foods, and industrial pollutants. Over time, chronic low-level exposure to lead, mercury, arsenic, and cadmium can accumulate in tissues and contribute to neurological damage, cardiovascular disease, kidney dysfunction, and even cancer [1]. A 2024 review confirmed that aluminum, cadmium, arsenic, mercury, and lead play significant roles in gastrointestinal, pulmonary, kidney, reproductive, neurodegenerative, and cardiovascular diseases [2].
The good news? Your body already has detoxification pathways designed to handle toxic metals — but they can become overwhelmed. This evidence-based guide walks you through safe chelation strategies, from getting properly tested to supporting your body's natural detox systems and knowing when medical intervention is warranted.
- Heavy metal testing should use validated methods — blood lead, blood mercury, and urine arsenic/cadmium are gold-standard tests, while provoked urine testing remains controversial with a positive predictive value of only 4.3%.
- Removing ongoing exposure sources (old paint, contaminated water, certain fish, occupational hazards) is the single most important first step before any chelation protocol.
- Natural chelation support including NAC, chlorella, modified citrus pectin, and milk thistle can help mobilize and excrete low-level heavy metal burdens when used consistently.
- Medical chelation with DMSA (FDA-approved for lead) or DMPS (effective for mercury) should only be done under physician supervision for confirmed heavy metal poisoning.
- The TACT trial showed EDTA chelation reduced cardiovascular events by 18% in post-MI patients, though the 2024 TACT2 follow-up found no significant cardiovascular benefit despite reducing blood lead by 60%.
- Glutathione — the body's master antioxidant — plays a central role in heavy metal detoxification by binding to metals and facilitating their excretion through bile and urine.
- A phased approach (test → remove exposure → support detox pathways → chelate if needed → retest) is safer and more effective than aggressive protocols.
- The FDA has not approved any over-the-counter chelation products, including supplements, nasal sprays, or clay baths marketed for heavy metal removal.
What Do You Need to Know Before Starting a Heavy Metal Detox?
Before beginning any heavy metal detox protocol, you need a confirmed diagnosis through validated testing, a clear understanding of your exposure sources, and a plan that matches the severity of your burden. Attempting aggressive chelation without proper preparation can redistribute metals to more sensitive tissues, potentially causing more harm than the original exposure.
Heavy metal detoxification is not a one-size-fits-all process. The approach for someone with confirmed lead poisoning from occupational exposure is fundamentally different from someone with low-level accumulated burden from environmental sources. Here's what to consider:
Who should consider heavy metal detox:
- People with confirmed elevated heavy metal levels on validated testing
- Those with known occupational exposure (mining, battery manufacturing, painting, welding)
- Individuals with chronic symptoms consistent with heavy metal toxicity (fatigue, brain fog, neuropathy, GI issues)
- Those living in older homes with lead paint or lead pipes
Expected timeline:
- Mild burden with natural support: 3–6 months
- Moderate burden with medical chelation: 6–12 months with multiple rounds
- Severe poisoning: Ongoing medical management
Prerequisites:
- Adequate kidney and liver function (chelation stresses both organs)
- Sufficient mineral status (zinc, selenium, magnesium) — chelators can deplete essential minerals
- Healthy gut function for proper excretion
Step 1: How Do You Get Properly Tested for Heavy Metals?
The gold standard for heavy metal testing uses blood tests for lead and organic mercury, and urine tests for arsenic and cadmium. These validated methods provide reliable baselines — blood lead levels above 5 µg/dL in adults are considered elevated by the CDC, while mercury levels above 5.8 µg/L warrant further evaluation.
Which tests should you request from your doctor?
Start with these evidence-based tests depending on your suspected exposure:
- Lead: Whole blood lead level (venous draw, not fingerstick). Reference: <5 µg/dL (CDC updated threshold). Levels >25 µg/dL may require chelation [3].
- Mercury: Whole blood mercury for organic/methylmercury exposure (primarily from fish). Reference: <5.8 µg/L. For inorganic mercury (dental amalgams, occupational), urine mercury is more appropriate.
- Arsenic: 24-hour urine collection or spot urine. Avoid seafood for 48 hours before testing (organic arsenic from seafood can cause false elevations).
- Cadmium: Urine cadmium reflects chronic exposure. Blood cadmium reflects recent exposure. Reference: urine <1 µg/L.
What about provoked urine testing?
Provoked urine testing (also called "challenge testing") involves taking a chelating agent and then measuring metal excretion in urine. While some integrative practitioners use this method, it remains controversial. A 2021 study found that provoked urine testing had a positive predictive value of only 4.3% for diagnosing heavy metal poisoning — meaning over 95% of "positive" results were false positives [4]. The American College of Medical Toxicology (ACMT) advises against its use for diagnosis [5].
Step 2: How Do You Identify and Remove Ongoing Exposure Sources?
Removing ongoing heavy metal exposure is the most critical step in any detox protocol — without it, chelation simply creates a revolving door where metals are removed and reabsorbed simultaneously. Identify your primary exposure sources through testing results, occupational history, home environment assessment, and dietary analysis.
Common exposure sources by metal:
Lead:
- Homes built before 1978 (lead paint)
- Old plumbing with lead pipes or lead solder
- Some imported ceramics, toys, and cosmetics
- Occupational: construction, battery recycling, shooting ranges
Mercury:
- High-mercury fish: shark, swordfish, king mackerel, tilefish, bigeye tuna
- Dental amalgam fillings (consult a biological dentist for safe removal — improper removal can spike mercury levels)
- Some skin-lightening creams
- Broken CFL bulbs or old thermometers
Arsenic:
- Well water in certain geographic areas
- Rice and rice products (rice accumulates arsenic from soil)
- Pressure-treated wood (CCA-treated, pre-2004)
Cadmium:
- Cigarette smoke (primary source for most people)
- Contaminated soil (near industrial areas)
- Some shellfish and organ meats
Action steps:
- Test your home water supply (use an NSF-certified lab)
- If you have young children, test for lead paint in pre-1978 homes
- Limit high-mercury fish to 1–2 servings per week; choose low-mercury options (salmon, sardines, anchovies)
- Rinse rice thoroughly and cook in excess water (reduces arsenic by 40–60%)
- If you smoke, quitting is the single most effective way to reduce cadmium exposure
Step 3: How Do You Support Your Body's Natural Detox Pathways?
Your liver, kidneys, and gut are the three primary exit routes for heavy metals, and optimizing their function creates the foundation for effective detoxification. Support these pathways with targeted nutrients — NAC (600–1,200 mg/day) boosts glutathione production, milk thistle (150–300 mg silymarin) protects liver cells, and adequate fiber (30+ g/day) prevents reabsorption through the gut.
How does glutathione help remove heavy metals?
Glutathione is your body's master detoxification molecule and plays a central role in heavy metal excretion. It directly binds to mercury, lead, arsenic, and cadmium, forming conjugates that are excreted through bile and urine. NAC (N-acetyl cysteine) is the most effective way to raise glutathione levels, as it provides the rate-limiting amino acid cysteine [6]. For direct supplementation, liposomal glutathione offers superior absorption compared to standard forms.
Learn more about glutathione's role in detox: Glutathione: The Master Antioxidant for Detox and Cellular Health
Which supplements support liver detox pathways?
- NAC (N-Acetyl Cysteine): 600–1,200 mg/day. Precursor to glutathione. Supports Phase II liver detox. Well-studied for heavy metal protection [6].
- Milk Thistle (Silymarin): 150–300 mg/day standardized to 80% silymarin.
Hepatoprotective — shields liver cells during chelation. Has demonstrated protective effects against lead and mercury-induced liver damage in animal studies [7].
- Alpha-Lipoic Acid (ALA): 300–600 mg/day. Chelates mercury and arsenic. Crosses blood-brain barrier (unique among natural chelators). Use with caution — can redistribute mercury if dental amalgams are still present.
- Selenium: 200 mcg/day. Binds mercury to form inert selenium-mercury complexes. Protective against mercury toxicity [8].
For comprehensive liver support strategies: How to Detox Your Liver Naturally
How does gut health affect heavy metal excretion?
Your gut is the final checkpoint for metal excretion. Metals conjugated by the liver are excreted into bile, enter the intestines, and must be eliminated before they can be reabsorbed (enterohepatic recirculation). Supporting this process requires:
- Fiber: 30+ g/day from vegetables, flaxseed, and psyllium binds metals in the gut
- Chlorella: Binds metals in the GI tract, potentially preventing reabsorption. A human study showed mercury and tin reduction after 90 days of algae supplementation [9], and animal studies demonstrate lead-binding capacity [10]
- Activated charcoal: Can bind metals in the gut when taken away from meals and supplements (2+ hours apart)
- Probiotics: Support gut barrier integrity and may reduce metal absorption
For a complete gut detox protocol: Gut Detox Protocol: Restore Your Digestive Health
Step 4: How Do You Use Natural Chelation Support Safely?
Natural chelation agents like modified citrus pectin, chlorella, and cilantro extract can gently mobilize and bind low-level heavy metal burdens without the aggressive action of pharmaceutical chelators. Modified citrus pectin showed a 74% average decrease in toxic heavy metals across five case studies, while chlorella demonstrated mercury reduction in a 90-day human trial [9][11].
What is modified citrus pectin and how does it chelate metals?
Modified citrus pectin (MCP) is a specially processed form of citrus pectin with smaller molecular weight that allows it to enter the bloodstream. Unlike regular pectin (which only works in the gut), MCP can chelate metals systemically. In a pilot study of five participants, MCP supplementation (15 g/day) produced a 74% average decrease in toxic heavy metals (lead, mercury, cadmium, arsenic) measured in urine excretion [11]. A separate study in children found that MCP significantly increased urinary lead excretion without depleting essential minerals [12].
Dosing: 5–15 g/day, mixed in water, taken between meals.
How effective is chlorella for heavy metal binding?
Chlorella (Chlorella vulgaris) has a unique cell wall structure that binds heavy metals in the gastrointestinal tract. While most robust evidence comes from animal studies — including a recent study showing significant lead removal in rats [10] — a human clinical study found that 90 days of chlorella combined with Fucus algae significantly reduced blood mercury and tin levels [9]. Chlorella works best as an ongoing binder during active chelation to prevent gut reabsorption.
Dosing: 3–6 g/day (tablets or powder), with meals.
What role does activated charcoal play in metal detox?
Activated charcoal binds a wide range of toxins including some heavy metals in the GI tract. It is most useful as an adjunct during active detox protocols to prevent reabsorption. However, it also binds medications and supplements, so timing is critical.
Dosing: 560–1,120 mg, taken 2+ hours away from food, supplements, and medications.
For more on activated charcoal protocols: Activated Charcoal: The Complete Detox Guide
Step 5: When Should You Consider Medical Chelation Therapy?
Medical chelation therapy is warranted when blood lead levels exceed 25 µg/dL in adults (or 45 µg/dL in children), when mercury levels remain persistently elevated despite source removal, or when you have documented symptoms of acute heavy metal poisoning. Always pursue medical chelation under the direct supervision of a toxicologist or experienced physician — never self-administer pharmaceutical chelators.
What are the FDA-approved chelation agents?
- DMSA (Succimer/Chemet): FDA-approved for lead poisoning in children. Oral administration makes it the most accessible chelator. A case series of 17 lead-poisoned adults showed DMSA increased lead excretion by a factor of 12 [13]. Also effective for mercury and arsenic.
- DMPS (Unithiol): Not FDA-approved in the US but widely used in Europe. Particularly effective for mercury chelation. Available through compounding pharmacies [13].
- CaNa₂EDTA (Calcium Disodium EDTA): IV administration. Used for severe lead poisoning. The TACT trial demonstrated an 18% relative risk reduction in cardiovascular events in post-MI patients [14]. However, the 2024 TACT2 trial found that while EDTA reduced blood lead by 60%, it showed no significant cardiovascular benefit in diabetic post-MI patients [15].
- D-Penicillamine: Oral chelator for copper (Wilson's disease) and sometimes lead. More side effects than DMSA.
What does a typical medical chelation protocol look like?
Medical chelation follows a cycle-and-rest pattern:
- Chelation round: 3–5 days of chelator administration (oral DMSA or IV EDTA)
- Rest period: 7–14 days off to allow kidney recovery and mineral replenishment
- Mineral supplementation: Zinc, selenium, magnesium between rounds (chelators deplete essential minerals)
- Monitoring: Blood/urine metals and kidney function before each round
- Repeat: Multiple rounds until levels normalize (typically 5–20+ rounds depending on burden)
:::warning[Critical warning] The FDA has not approved any OTC chelation products including supplements marketed as chelators, nasal sprays, suppositories, or clay baths [16]. These unregulated products can be dangerous. :::
Step 6: How Do You Monitor Progress and Know When You're Done?
Monitor your heavy metal detox progress by retesting blood and urine levels every 3–6 months using the same laboratory and collection method as your baseline. Successful detox shows a consistent downward trend in metal levels combined with symptom improvement — a single test is never sufficient to declare completion.
What markers should you track?
- Primary metals: Retest the same metals from your baseline (lead, mercury, arsenic, cadmium)
- Kidney function: BUN, creatinine, GFR — chelation stresses the kidneys
- Liver enzymes: ALT, AST — monitor liver health during the protocol
- Essential minerals: Zinc, selenium, magnesium, copper, iron — chelation can deplete these
- Symptoms journal: Track energy, cognition, GI function, neuropathy, sleep quality monthly
When can you stop the protocol?
Consider your detox protocol complete when:
- Metal levels are within reference ranges on two consecutive tests (3 months apart)
- Symptoms have meaningfully improved or resolved
- Essential mineral levels remain stable
- Your healthcare provider confirms it's safe to discontinue
After completing active detox, transition to a maintenance phase: continue NAC (600 mg/day), eat a mineral-rich diet, maintain gut health, limit ongoing exposures, and retest annually.
What Are the Most Common Heavy Metal Detox Mistakes to Avoid?
The most dangerous mistake is attempting aggressive chelation without proper testing or medical supervision — this can redistribute metals from tissues to the brain, kidneys, or other sensitive organs. Other common errors include chelating while dental amalgams are still present, neglecting mineral replacement, and expecting overnight results from a process that takes months.
Top mistakes and how to avoid them:
- Chelating without testing first. You need a baseline to know what you're dealing with and to measure progress. Random supplement protocols based on symptoms alone are inefficient at best and dangerous at worst.
- Ignoring ongoing exposure. Chelation while you're still being exposed is like bailing water from a sinking boat without plugging the hole. Address sources first.
- Using alpha-lipoic acid with amalgam fillings. ALA crosses the blood-brain barrier and can redistribute mercury from fillings directly into brain tissue. Remove amalgams first (by a qualified biological dentist), wait 3 months, then consider ALA.
- Neglecting mineral replacement. All chelators — natural and pharmaceutical — bind some essential minerals along with toxic metals. Supplement zinc (30 mg), selenium (200 mcg), and magnesium (400 mg) between chelation rounds.
- Expecting fast results. Heavy metals accumulate in bones and deep tissues over decades. Safe removal takes months to years. Aggressive protocols that promise rapid detox often cause redistribution injuries.
- Ignoring gut health. If your gut is compromised (constipation, leaky gut, dysbiosis), mobilized metals can be reabsorbed instead of excreted. Fix gut function before intensive chelation.
- Falling for unproven products. Detox foot pads, ionic foot baths, zeolite sprays, and infrared sauna "metal detox" have no reliable evidence for heavy metal removal. Stick to evidence-based approaches.
For a comprehensive foundation: The Complete Guide to Detox and Cleansing
Is Heavy Metal Chelation Safe? When Should You Stop?
Heavy metal chelation is generally safe when performed under medical supervision with proper monitoring, but all chelation carries risks including mineral depletion, kidney stress, and potential metal redistribution. Stop immediately and contact your doctor if you experience worsening symptoms, signs of kidney problems (reduced urination, swelling), severe GI distress, or neurological changes.
What are the main risks of chelation?
- Mineral depletion: Chelators bind essential minerals (zinc, copper, iron, calcium). Without replacement, this can cause deficiencies with serious consequences.
- Kidney stress: Metals bound to chelators are excreted through the kidneys. Pre-existing kidney disease increases risk.
- Metal redistribution: Improper chelation can move metals from less harmful storage sites (bone, fat) to more sensitive organs (brain, kidneys).
- Herxheimer-like reactions: Mobilizing stored metals can temporarily worsen symptoms — fatigue, headaches, GI upset. Mild reactions are expected; severe reactions mean the protocol is too aggressive.
Who should NOT attempt chelation?
- People with kidney disease or impaired kidney function
- Pregnant or breastfeeding women (mobilized metals can cross the placenta and enter breast milk)
- People with severe liver disease
- Anyone taking medications with known chelator interactions (consult your pharmacist)
- Children (must be under pediatric toxicology supervision)
What Should You Do First to Start a Safe Heavy Metal Detox?
Start with validated testing to establish your baseline, then systematically remove exposure sources before adding any chelation support. This phased approach prevents the common mistake of chelating metals that are still actively entering your body, which reduces effectiveness and increases side effects.
Phase 1 — Test and Assess (Weeks 1–2):
- [ ] Request blood lead and blood mercury tests from your doctor
- [ ] Request 24-hour urine arsenic and cadmium tests
- [ ] Complete an exposure assessment (home, work, diet, dental history)
- [ ] Test your home water supply for heavy metals
- [ ] Get baseline kidney function (BUN, creatinine) and liver enzymes (ALT, AST)
Phase 2 — Remove Exposure (Weeks 2–6):
- [ ] Address identified exposure sources (water filter, diet changes, occupational protection)
- [ ] Switch to low-mercury fish (salmon, sardines, anchovies)
- [ ] If dental amalgams are a concern, consult a biological dentist for evaluation
- [ ] Begin mineral optimization: zinc 30 mg, selenium 200 mcg, magnesium 400 mg daily
Phase 3 — Support Detox Pathways (Weeks 4–12):
- [ ] Start NAC 600 mg twice daily to boost glutathione
- [ ] Add milk thistle 150 mg (standardized to 80% silymarin) twice daily
- [ ] Increase dietary fiber to 30+ g/day
- [ ] Add chlorella 3 g/day with meals as a gut binder
- [ ] Consider modified citrus pectin 5–15 g/day between meals
Phase 4 — Retest and Evaluate (Month 3–4):
- [ ] Retest all baseline metals using the same lab and method
- [ ] Review symptom journal for improvements
- [ ] If levels remain significantly elevated, consult a toxicologist about medical chelation
- [ ] If levels are trending down, continue natural support for another 3 months
Phase 5 — Maintenance (Ongoing):
- [ ] Continue NAC 600 mg/day and mineral supplementation
- [ ] Maintain clean diet with adequate fiber
- [ ] Retest annually or as recommended by your doctor
- [ ] Stay vigilant about new exposure sources
References
- Tchounwou PB, Yedjou CG, Patlolla AK, Sutton DJ. Heavy metal toxicity and the environment. Molecular, Clinical and Environmental Toxicology. 2012;101:133-164. Source
- Khan S, et al. Heavy metals (Al, Cd, As, Hg, Pb) toxicity and their role in diseases: A comprehensive review (2024). Environmental Science and Pollution Research. Source
- CDC. Blood Lead Reference Value. Centers for Disease Control and Prevention. Source
- Ruha AM, et al. Provoked urine testing in patients with suspected heavy metal poisoning: Positive predictive value of 4.3%. Journal of Medical Toxicology. 2021;17(4):358-362. Source
- American College of Medical Toxicology. Position Statement on Post-Chelator Challenge Urinary Metal Testing. Source
- Mokhtari V, et al. A review on various uses of N-acetyl cysteine. Cell Journal. 2017;19(1):11-17. Source
- Abenavoli L, et al. Milk thistle in liver diseases: past, present, future. Phytotherapy Research. 2010;24(10):1423-1432. Source
- Ralston NVC, Raymond LJ. Dietary selenium's protective effects against methylmercury toxicity. Toxicology. 2010;278(1):112-123. Source
- Merino JJ, et al. Effects of chlorella and Fucus algae supplementation on mercury and tin levels in humans: A 90-day pilot study. Nutrients. 2019;11(12):3032. Source
- Al-Asmari AK, et al. Chlorella vulgaris supplementation on lead toxicity in rats. Biological Trace Element Research. 2025. Source
- Eliaz I, et al. The effect of modified citrus pectin on urinary excretion of toxic elements. Phytotherapy Research. 2006;20(10):859-864. Source
- Zhao ZY, et al. The role of modified citrus pectin as an effective chelator of lead in children hospitalized with toxic lead levels. Alternative Therapies in Health and Medicine. 2008;14(4):34-38. Source
Frequently asked questions
How long does it take to detox heavy metals from your body?
A typical heavy metal detox takes 3–12 months depending on the severity of your burden and the methods used. Mild environmental accumulation may respond to natural support (NAC, chlorella, MCP) in 3–6 months, while confirmed heavy metal poisoning requiring medical chelation often takes 6–12 months with multiple chelation rounds. Metals stored in bone (like lead) can take even longer, as bone turnover is slow. Regular retesting every 3 months helps track your progress.
Can you remove heavy metals from your body naturally without chelation drugs?
Yes, mild to moderate heavy metal burdens can often be addressed with natural approaches including NAC, chlorella, modified citrus pectin, and dietary strategies. These work by supporting glutathione production, binding metals in the GI tract, and optimizing liver and kidney excretion. However, confirmed heavy metal poisoning with significantly elevated levels typically requires pharmaceutical chelators like DMSA or CaNa₂EDTA under medical supervision. The key distinction is severity — natural approaches support the body's existing detox pathways, while pharmaceutical chelators actively pull metals from tissues.
What are the symptoms of heavy metal toxicity?
Common symptoms include chronic fatigue, brain fog, memory problems, headaches, digestive issues, joint and muscle pain, and numbness or tingling in the extremities. More specific symptoms depend on the metal — lead primarily affects the nervous system and blood (anemia, neuropathy), mercury targets the brain and kidneys (tremors, mood changes), arsenic affects skin and GI tract (skin lesions, abdominal pain), and cadmium damages kidneys and lungs. These symptoms overlap with many other conditions, which is why testing is essential.
Is chelation therapy dangerous?
Chelation therapy is generally safe when performed under medical supervision with proper monitoring, but it does carry risks. The main concerns are essential mineral depletion (zinc, copper, iron, calcium), kidney stress from excreting metal-chelator complexes, and potential metal redistribution if protocols are too aggressive. Rare but serious complications include kidney failure and severe mineral imbalances. IV chelation carries more risk than oral chelation. The key to safety is proper pre-screening (kidney function, mineral status), supervised dosing, and regular monitoring between rounds.
Does cilantro really remove heavy metals?
Cilantro has shown some metal-mobilizing properties in laboratory and animal studies, but human clinical evidence is limited and inconclusive. The concern with cilantro is that it may mobilize metals without adequately binding them for excretion, potentially causing redistribution. If you want to include cilantro, always pair it with a binding agent like chlorella or activated charcoal to catch mobilized metals in the gut. It should never be relied upon as a primary chelation strategy.
Which foods help remove heavy metals from the body?
Foods rich in sulfur compounds, fiber, and specific minerals support heavy metal excretion. Top choices include garlic and onions (sulfur compounds support glutathione), cruciferous vegetables like broccoli and Brussels sprouts (sulforaphane activates detox enzymes), cilantro (mild mobilizer), flaxseed and chia seeds (fiber binds metals in the gut), blueberries (antioxidant protection), and selenium-rich Brazil nuts (forms protective selenium-mercury complexes). Wild-caught salmon provides selenium and omega-3s that protect against mercury damage.
How do you test for heavy metals at home?
While home test kits exist for water and some claim to test hair or urine for heavy metals, they are not reliable for clinical decision-making. For accurate results, request venous blood tests for lead and mercury and a 24-hour urine collection for arsenic and cadmium through your doctor or a direct-to-consumer lab that uses certified reference laboratories. Home water testing kits from NSF-certified labs are reliable for testing your water supply specifically.
Can heavy metals cause autoimmune disease?
Research suggests that heavy metal exposure may contribute to autoimmune conditions by disrupting immune regulation, though the relationship is complex. Mercury has the strongest association, with studies linking dental amalgam exposure and occupational mercury exposure to increased risk of autoimmune thyroiditis, lupus, and other conditions. Lead and cadmium can also dysregulate immune function. However, heavy metals are likely one factor among many (genetics, infections, gut health) that contribute to autoimmune development rather than a sole cause.
Should you take chlorella before or after meals for heavy metal detox?
Take chlorella with meals for heavy metal detox purposes. When taken with food, chlorella's cell wall binds metals present in your meal and metals excreted into the GI tract via bile, preventing reabsorption through enterohepatic recirculation. If you're using chlorella during an active chelation protocol, take it with each main meal (1 g, three times daily) to maintain consistent binding throughout the day. Take it at least 2 hours away from any pharmaceutical chelators to avoid binding the chelator itself.
Is infrared sauna effective for heavy metal detox?
Infrared saunas may support detoxification through increased sweating, and some studies have detected small amounts of heavy metals in sweat. However, sweat is a minor excretion route compared to urine and bile/stool — the amounts of metals removed through sweating are minimal relative to what chelation achieves. Infrared saunas can be a helpful adjunct for general wellness and may support circulation and relaxation during a detox protocol, but they should not be relied upon as a primary heavy metal removal strategy.