longevity
Hormone Optimization for Longevity: Complete Guide
Complete guide to hormone optimization and aging. Learn about testosterone, estrogen, HRT benefits and risks, natural strategies, and when hormone replacement helps.
Something shifts in your late thirties or early forties. The energy you used to take for granted just… isn't there anymore. You're sleeping the same hours but waking up tired. Muscle takes longer to build and disappears faster when you skip the gym. Your mood fluctuates for no clear reason. And your doctor says your labs are "normal."
Here's the thing nobody tells you early enough: your hormones are quietly declining every single year after your twenties. Hormone optimization aging isn't some fringe biohacking concept—it's about understanding a universal biological process that affects every single person. Testosterone in men drops about 1% annually after 30. Women face a dramatic estrogen cliff at menopause. Growth hormone, DHEA, thyroid—they all follow the same downward trajectory. And these shifts don't just affect how you feel. They influence how you age at a cellular level.
This isn't about chasing some fountain-of-youth fantasy. It's about understanding which hormones decline, why it matters for longevity, and what you can actually do about it—from lifestyle changes that cost nothing to medical interventions that require careful supervision.
In this guide, you'll learn how hormones change with age, the evidence behind hormone replacement therapy (both the real benefits and the real risks), natural optimization strategies that are proven and free, when replacement might make sense, and how to get tested properly. We'll cover testosterone, estrogen, progesterone, growth hormone, DHEA, and thyroid—the full picture.
If you're interested in the broader science of aging well, check out our longevity and anti-aging complete guide and our sleep optimization guide for one of the most powerful natural hormone boosters available. For understanding how inflammation accelerates hormone decline, see our inflammation and pain relief guide.
- All major hormones—testosterone, estrogen, growth hormone, DHEA, and thyroid—decline progressively with age, starting as early as your late twenties and accelerating after 40.
- Testosterone drops approximately 1% per year in men after age 30, while women experience a dramatic estrogen decline at menopause (average age 51), with up to 30% collagen loss in the first five years.
- Hormone replacement therapy can dramatically improve quality of life when used appropriately, but it is not proven to extend human lifespan and carries real risks including cardiovascular events, blood clots, and cancer concerns.
- The "timing hypothesis" for women's HRT is well-supported: starting estrogen therapy within 10 years of menopause or before age 60 is associated with significantly better outcomes and lower risks.
- Natural optimization strategies—strength training, quality sleep, stress management, and targeted nutrition—should always be the first-line intervention before considering hormone replacement.
- Growth hormone therapy for anti-aging is controversial, expensive ($1,000–$2,000+/month), and may paradoxically accelerate aging through mTOR pathway activation.
- Hormone testing should include morning testosterone (men), comprehensive thyroid panel, DHEA-S, and cortisol—interpreted by a specialist who understands optimal ranges, not just reference ranges.
What Is Hormone Optimization and Why Does It Matter for Aging?
Hormone optimization is the practice of maintaining or restoring hormone levels to support health, vitality, and cellular function as you age. Every major hormone—testosterone, estrogen, progesterone, growth hormone, DHEA, and thyroid—declines progressively after your twenties, contributing to fatigue, muscle loss, cognitive changes, metabolic dysfunction, and accelerated biological aging.
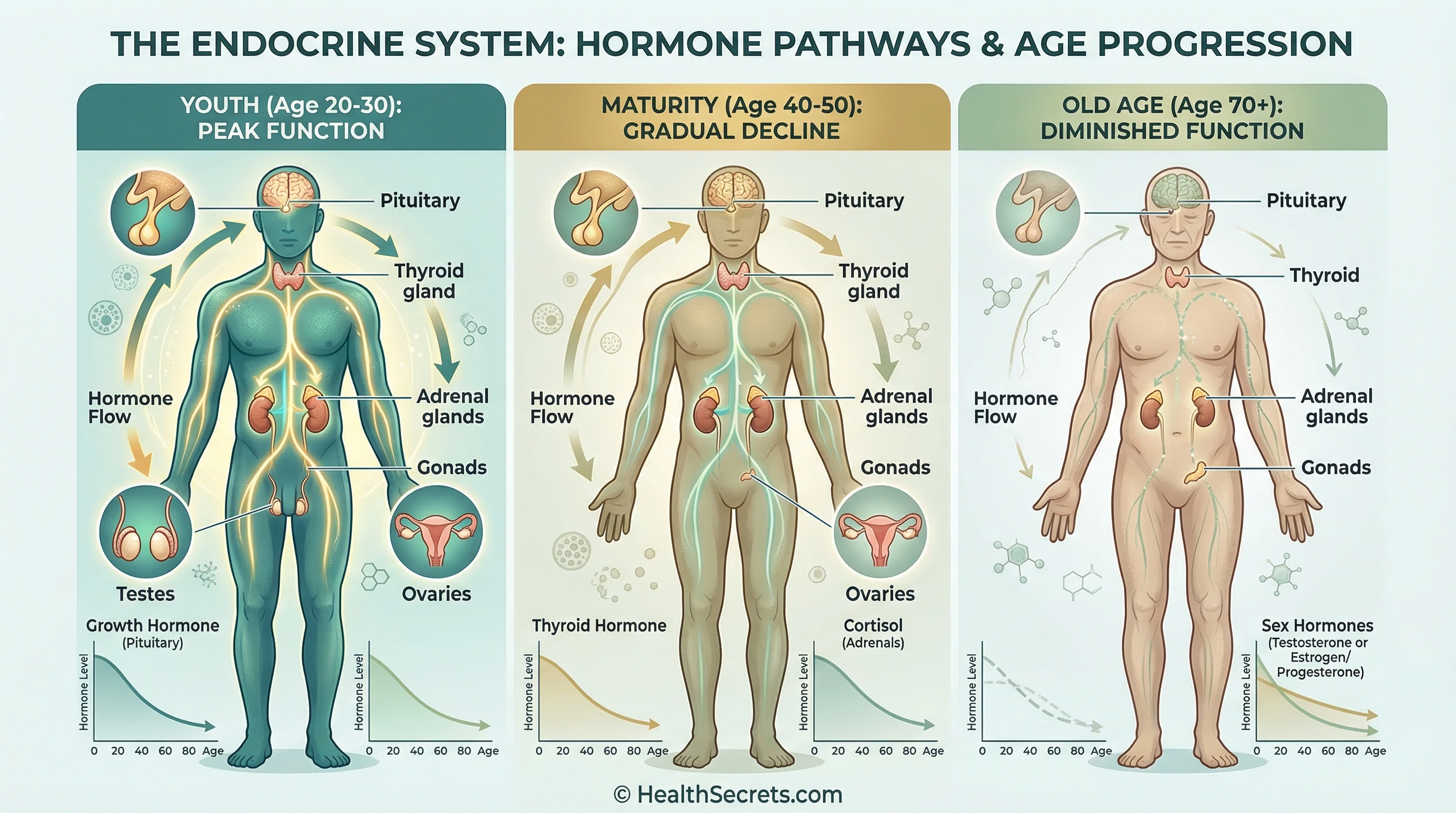
Your endocrine system is essentially the body's chemical messaging network. Glands—including the pituitary, thyroid, adrenals, and gonads—produce hormones that regulate metabolism, growth, reproduction, mood, energy, and cellular repair. When these signals weaken with age, the downstream effects touch virtually every system in your body.
The decline isn't dramatic overnight. Testosterone in men drops roughly 1% per year after age 30, meaning by 70, many men have half the testosterone they had at 25 ([1]). Women face a different pattern—relatively stable estrogen through their reproductive years, then a sharp decline at menopause that accelerates bone loss, cardiovascular risk, and cognitive changes.
What makes this relevant to longevity? Hormones don't just affect how you feel—they regulate cellular repair, inflammation, mitochondrial function, and metabolic health. Research suggests that testosterone replacement therapy increased survival rate by 9–10% over five years in men with late-onset hypogonadism ([2]). For women, hormone therapy initiated early in menopause has been associated with a 39% reduction in all-cause mortality ([3]).
But—and this is critical—hormone optimization isn't just about replacement therapy. Lifestyle factors profoundly influence hormone levels. Obesity suppresses testosterone. Poor sleep crushes growth hormone production. Chronic stress elevates cortisol, which actively breaks down the hormones you need most. For many people, addressing these factors first can restore hormone function without medication.
How Do Hormones Decline and Affect Your Body as You Age?
Hormones decline through multiple mechanisms: reduced glandular production, decreased receptor sensitivity, increased binding proteins that trap hormones in inactive forms, and hypothalamic-pituitary axis dysfunction. The result is a progressive loss of cellular signaling that drives virtually every symptom we associate with aging—from energy loss and muscle wasting to cognitive decline and metabolic dysfunction.
How Does Testosterone Change in Men After 30?
Testosterone decline in men is driven by both primary factors (testicular function decreasing) and secondary factors (hypothalamic-pituitary changes). Modern lifestyle compounds the problem—obesity, poor sleep, chronic stress, and endocrine disruptors may be accelerating testosterone decline beyond what's historically normal ([1]).
Symptoms include reduced energy and motivation, loss of muscle mass, increased abdominal fat, decreased libido, mood changes, cognitive fog, reduced bone density, and sleep disturbances. Not every man with declining levels is symptomatic—individual variation is enormous.
What Happens to Estrogen and Progesterone During Menopause?
Unlike the gradual decline in men, women experience a dramatic drop in estrogen and progesterone at menopause (average age 51). Perimenopause can begin in the early 40s with fluctuating hormones causing symptoms years before periods stop. In the first five years post-menopause, women lose approximately 30% of their collagen, bone density loss accelerates, and cardiovascular risk increases significantly.
The 2002 Women's Health Initiative study created widespread fear about HRT by showing increased breast cancer and cardiovascular risk. But subsequent analysis revealed critical limitations: the study used synthetic hormones, enrolled mostly older women (average age 63), and used oral administration. The "timing hypothesis" has since reshaped understanding—women who start HRT within 10 years of menopause show reduced cardiovascular disease, reduced mortality, and minimal breast cancer risk increase ([4]; [3]).
Why Is Growth Hormone Therapy Controversial for Anti-Aging?
Growth hormone declines dramatically with age—a process called somatopause. By 60, GH secretion is roughly 50% of youthful levels. While GH therapy can increase muscle mass and reduce body fat, it also causes insulin resistance, joint pain, and may promote cancer cell growth. Perhaps most concerning: lower GH and IGF-1 levels are actually associated with longevity in some studies. Centenarians often have low IGF-1 ([5]; [14]).
Does DHEA Supplementation Actually Work?
DHEA, produced by the adrenal glands and a precursor to sex hormones, declines to about 20% of peak levels by age 70. Despite being available over-the-counter, clinical trials using 50–100 mg daily in elderly individuals have shown no clear benefits for body composition, strength, or insulin sensitivity ([6]; Harvard Health. DHEA Supplements).
Thyroid hormones (T3 and T4) can also decline with age. Subclinical hypothyroidism becomes more common, causing fatigue, weight gain, cold intolerance, hair loss, and cognitive fog. When genuinely deficient, thyroid replacement is life-changing—but overtreatment carries serious risks.
What Are the Key Benefits of Hormone Optimization for Longevity?
When done appropriately and under medical supervision, hormone optimization can dramatically improve quality of life and may support healthspan—the years you live in good health. The evidence is strongest for symptom relief and metabolic improvement, while lifespan extension remains unproven. Natural optimization through lifestyle provides benefits with virtually no risk.
Can Testosterone Replacement Improve Quality of Life in Men?
For men with clinically low testosterone (below 300 ng/dL) and symptoms, TRT can increase muscle mass and strength, reduce body fat, improve energy and mood, enhance libido, and support bone density. Research supports meaningful benefits for men with genuine deficiency ([2]). The key distinction: TRT benefits men with true deficiency far more than men with age-related decline still within "normal" ranges.
Does Hormone Therapy Benefit Women During Menopause?
For women with moderate-to-severe menopausal symptoms, HRT can eliminate hot flashes and night sweats (90% reduction), improve sleep quality, preserve bone density, maintain vaginal and urinary health, and potentially protect cardiovascular health when started early. Transdermal estrogen (patches, gels) combined with micronized progesterone appears to carry lower risk than oral synthetic formulations ([9]; Menopause Society. When Women Initiate Estrogen Therapy Matters).
How Does Natural Hormone Optimization Support Longevity?
Strength training boosts testosterone and growth hormone significantly. Sleep is when most hormone production occurs—chronic sleep deprivation drops testosterone 10–15% in young men. Stress management lowers cortisol, which otherwise suppresses virtually every beneficial hormone. These strategies are free, proven, and carry essentially zero risk ([16]).
Can Thyroid Optimization Impact Energy and Metabolism?
For people with genuine thyroid deficiency—elevated TSH, low Free T3/T4—replacement therapy can be transformative. Energy returns, weight management improves, mood stabilizes, and cognitive function sharpens. The key is accurate diagnosis and careful dosing, since overtreatment causes heart palpitations, bone loss, and anxiety.
Are There Any Risks or Side Effects of Hormone Replacement Therapy?
Hormone replacement therapy carries real risks that must be weighed against benefits on an individual basis. For testosterone in men, concerns include potential cardiovascular effects, increased red blood cell production (blood clot risk), possible acceleration of existing prostate cancer, worsened sleep apnea, and suppressed fertility. For women, risks include a small increase in breast cancer with combined estrogen-progestin therapy, blood clots, and stroke.
The cardiovascular picture for testosterone remains contested. Some studies suggest increased risk, others show neutral or protective effects. What's clearer: TRT increases hematocrit (red blood cell count), requiring monitoring to prevent clotting complications. It does not appear to cause prostate cancer but may accelerate existing, undiagnosed disease.
For women, the breast cancer risk with combined estrogen-progestin therapy is approximately 1 extra case per 1,000 women per year—meaningful but small. Estrogen-only therapy (for women without a uterus) shows even lower risk. The route of administration matters: transdermal estrogen avoids first-pass liver metabolism and carries lower clot risk than oral forms ([12]).
Regarding the bioidentical vs. synthetic debate: "bioidentical" means chemically identical to human hormones. Both compounded and pharmaceutical versions exist. Compounded bioidenticals lack FDA oversight, raising quality concerns. FDA-approved bioidenticals (estradiol patches, micronized progesterone) offer standardized dosing. The route and timing may matter more than bioidentical vs. synthetic classification (Harvard Health. Bioidentical Hormones; [8]).
Growth hormone therapy for anti-aging is expensive ($1,000–$2,000+/month) and carries risks including insulin resistance, joint pain, fluid retention, and potential cancer promotion. Lower GH/IGF-1 levels are paradoxically associated with longevity ([19]).
Absolute contraindications for HRT include active breast or prostate cancer, history of blood clots or clotting disorders, active liver disease, pregnancy, and uncontrolled cardiovascular disease.
How Do You Optimize Your Hormones Safely?
The safest approach follows a clear hierarchy: optimize lifestyle first, test hormones if symptomatic, consider replacement only for documented deficiency with no contraindications, and commit to ongoing monitoring. This sequence is not optional—skipping straight to replacement without lifestyle optimization is medically irresponsible and less effective.
Step 1: Optimize lifestyle (everyone should do this). Before any testing or treatment, address the fundamentals. Strength train 2–3 times per week with compound movements. Get 7–9 hours of quality sleep consistently. Manage chronic stress through meditation, nature exposure, or therapy. Maintain a healthy body weight—obesity alone can suppress testosterone by 30% or more.
Step 2: Get tested if symptomatic. Don't guess—test. For men over 40 with symptoms: morning total and free testosterone, SHBG, estradiol, LH/FSH, thyroid panel (TSH, Free T3, Free T4), DHEA-S, and morning cortisol. For women in perimenopause or menopause: estradiol, progesterone, testosterone, FSH/LH, thyroid panel, DHEA-S, and cortisol. Timing matters—testosterone and cortisol peak in the morning and should be drawn before 10 AM.
Reference ranges are broad. A 55-year-old man with testosterone at 350 ng/dL is technically "normal" but may be symptomatic. Work with a doctor who understands optimal ranges and treats the whole picture—symptoms plus labs.
Step 3: Consider replacement for documented deficiency. Good candidates for TRT: clinically low testosterone (below 300 ng/dL) with symptoms, after failed natural optimization, with no contraindications. Good candidates for women's
HRT: moderate-to-severe menopausal symptoms, within 10 years of menopause or under 60, no contraindications.
Step 4: Monitor continuously. TRT requires checking hormone levels, hematocrit, PSA, and lipids every 3–6 months initially, then annually. Women's HRT requires annual breast exams, mammograms, and ongoing symptom assessment. Thyroid replacement needs TSH and Free T3/T4 every 6–12 weeks initially.
Seek endocrinologists, reproductive medicine specialists, certified menopause practitioners, or functional medicine doctors with hormone expertise. Avoid anti-aging clinics promising miracles without proper testing and monitoring.
What Diet and Lifestyle Changes Support Healthy Hormone Levels?
A nutrient-dense, anti-inflammatory diet combined with regular exercise, quality sleep, and stress management forms the foundation of natural hormone optimization. These interventions are free, evidence-based, and can meaningfully improve hormone levels without any medical risk—often restoring function enough to avoid replacement therapy entirely.
- For testosterone support: Zinc from oysters, red meat, and pumpkin seeds—deficiency directly lowers testosterone. Vitamin D from sunlight, fatty fish, or supplementation (2,000–5,000 IU daily). Healthy fats from olive oil, avocados, and nuts—cholesterol is the raw material for testosterone synthesis. Adequate protein at 0.7–1g per pound of bodyweight supports both muscle mass and hormone production. Magnesium from leafy greens, nuts, and seeds supports 300+ enzymatic reactions including hormone production.
- For thyroid support: Iodine from seafood and iodized salt—essential building block for thyroid hormones. Selenium from Brazil nuts (2–3 daily) and fish—converts T4 to active T3.
- General hormone health: Follow an anti-inflammatory diet (Mediterranean pattern) rich in vegetables, fruits, fish, olive oil, and nuts. Avoid processed foods and excess sugar—insulin resistance disrupts virtually all hormone pathways. Eat adequate calories—chronic under-eating suppresses thyroid, testosterone, and reproductive hormones. Omega-3 fatty acids from salmon, sardines, and walnuts reduce inflammation that impairs hormone signaling.
- Avoid endocrine disruptors: BPA in plastics and can linings, phthalates in personal care products, pesticides (choose organic when possible), and parabens in cosmetics. Use glass or stainless steel containers. Read labels on personal care products.
- Intermittent fasting (16:8 pattern) may boost growth hormone secretion during fasting windows and improve insulin sensitivity, supporting overall hormonal balance. And maintaining a healthy weight is perhaps the single most impactful change—obesity suppresses testosterone and increases estrogen through aromatization in fat tissue. Losing excess weight often normalizes hormone levels without any replacement therapy.
What Should You Do First to Optimize Your Hormones for Longevity?
Start with the lifestyle fundamentals that cost nothing and carry zero risk—strength training, sleep optimization, stress management, and targeted nutrition. These changes alone can meaningfully improve hormone levels within weeks. If symptoms persist after 3–6 months of consistent lifestyle optimization, get comprehensive hormone testing through a qualified specialist before considering any replacement therapy.
Phase 1 — Foundation (Weeks 1–4):
- [ ] Begin strength training 2–3x per week (compound movements: squats, deadlifts, presses)
- [ ] Prioritize 7–9 hours of sleep with consistent schedule
- [ ] Add 10–20 minutes daily stress management (meditation, deep breathing, nature walks)
- [ ] Eliminate processed foods and excess sugar; increase vegetables, healthy fats, quality protein
- [ ] Start vitamin D (2,000–5,000 IU) and zinc (15–30 mg) supplementation if not already
Phase 2 — Assessment (Weeks 4–12):
- [ ] Track symptoms weekly (energy, mood, libido, sleep quality, body composition)
- [ ] If symptomatic, schedule comprehensive hormone panel with a knowledgeable doctor
- [ ] Address any sleep disorders (sleep apnea screening if relevant)
- [ ] Achieve and maintain healthy body weight
- [ ] Reduce exposure to endocrine disruptors (switch to glass containers, clean personal care products)
Phase 3 — Targeted Intervention (Months 3–6+):
- [ ] Review lab results with specialist—compare to optimal ranges, not just reference ranges
- [ ] If deficient: discuss replacement options, risks, and monitoring requirements
- [ ] If starting HRT: commit to regular monitoring schedule (every 3–6 months initially)
- [ ] Continue lifestyle optimization alongside any medical intervention
- [ ] Set realistic expectations: symptom relief in 2–8 weeks, body composition changes in 3–6 months
References
- Travison, T.G. et al., 2024. Age-related testosterone decline: mechanisms and intervention strategies. PMC Source
- Fink, J. et al., 2015. Hormone replacement therapy and longevity. PubMed Source
- Hodis, H.N. & Mack, W.J., 2022. Menopausal Hormone Replacement Therapy and Reduction of All-Cause Mortality and Cardiovascular Disease. PubMed Source
- JAMA Network Open, 2024. Hormone Therapy and Biological Aging in Postmenopausal Women Source
- Aguiar-Oliveira, M.H. & Bartke, A., 2019. Growth Hormone and Aging: Updated Review. PMC Source
- Rutkowski, K. et al., 2022. Dehydroepiandrosterone, Cancer, and Aging. PMC Source
- Seftel, A., 2005. Off-label use of hormones as an antiaging strategy: a review. PMC Source
- Holtorf, K., 2009. The bioidentical hormone debate. PubMed Source
- Boardman, H.M. et al., 2018. AJP: Update on hormone therapy in postmenopausal women Source
- Salpeter, S.R. et al., 2016. The timing hypothesis: Do coronary risks of menopausal HT vary by age. PMC Source
- Harman, S.M., 2011. Timing and Duration of Menopausal Hormone Treatment May Affect Cardiovascular Outcomes. PMC Source
- Collaborative Group on Hormonal Factors, 2019. Type and timing of MHT and breast cancer risk. The Lancet Source
Frequently asked questions
At what age do hormones start declining?
Most hormones begin declining in your late twenties to early thirties. Testosterone in men drops about 1% per year after age 30. Growth hormone and DHEA decline progressively from the mid-twenties. Women experience relatively stable estrogen until perimenopause (typically mid-40s), followed by a dramatic decline at menopause (average age 51). The rate varies significantly based on genetics, lifestyle, body composition, and overall health.
Is hormone replacement therapy safe for long-term use?
Long-term safety depends on the type of hormone, dosage, route of administration, timing of initiation, and individual risk factors. For women, estrogen therapy started within 10 years of menopause appears relatively safe and may reduce all-cause mortality. For men, TRT requires ongoing monitoring of hematocrit, PSA, and cardiovascular markers. All HRT carries some risk and requires medical supervision with regular follow-up.
Can you boost testosterone naturally without medication?
Yes, lifestyle interventions can meaningfully increase testosterone. Strength training (especially compound movements), achieving a healthy weight, getting 7–9 hours of quality sleep, managing chronic stress, and correcting zinc and vitamin D deficiencies have all been shown to improve testosterone levels. Weight loss alone can boost testosterone up to 30% in overweight men.
What is the timing hypothesis for women's hormone therapy?
The timing hypothesis states that hormone therapy is safer and more beneficial when started within 10 years of menopause or before age 60. Meta-analyses show that early initiation reduces all-cause mortality by up to 39% and coronary heart disease by 32%, while late initiation (10+ years post-menopause) increases cardiovascular risk. This explains why the WHI study found negative results—it enrolled mostly older women.
Are bioidentical hormones safer than synthetic hormones?
Despite marketing claims, bioidentical hormones are not conclusively safer than synthetic versions. Both carry similar risks. The route of administration (transdermal vs. oral) and timing of initiation likely matter more than whether hormones are bioidentical or synthetic. FDA-approved bioidenticals offer standardized dosing, while compounded versions lack regulatory oversight and may have inconsistent quality.
Should you take growth hormone for anti-aging?
For most people, no. Growth hormone therapy is expensive ($1,000–$2,000+/month), carries significant risks (insulin resistance, joint pain, potential cancer promotion), and paradoxically, lower GH/IGF-1 levels are associated with longevity in some studies. Unless you have diagnosed GH deficiency from pituitary disease, natural optimization through sleep, exercise, and intermittent fasting is safer and more practical.
How do you test your hormone levels properly?
Request a comprehensive panel including morning testosterone (total and free for men), estradiol, progesterone, FSH/LH, thyroid panel (TSH, Free T3, Free T4), DHEA-S, and morning cortisol. Timing matters—testosterone and cortisol peak in the morning and should be drawn before 10 AM. Work with a specialist who interprets optimal ranges, not just reference ranges.
Does DHEA supplementation help with aging?
Evidence for DHEA supplementation is weak. While DHEA declines dramatically with age, clinical trials using 50–100 mg daily in elderly individuals have shown no clear benefits for body composition, strength, or insulin sensitivity. Some modest improvements in mood and bone density have been reported in women. Given potential risks, DHEA should only be considered after testing and with medical supervision.
What are the signs of low thyroid function with aging?
Common signs include persistent fatigue despite adequate sleep, unexplained weight gain, cold intolerance, hair loss, dry skin, constipation, brain fog, depression, and slow heart rate. Subclinical hypothyroidism becomes more common with aging and may be missed with only TSH testing. A complete thyroid panel including Free T3 and Free T4 provides a fuller picture.
Can exercise really affect hormone levels?
Yes, substantially. Resistance training acutely boosts testosterone and growth hormone, especially compound movements at moderate-to-high intensity. Regular exercise improves insulin sensitivity (supporting all hormones), reduces cortisol chronically, and supports healthy body composition. Both aerobic and resistance training contribute, but strength training has the most pronounced hormonal effects.