inflammation
Chronic Inflammation: Causes, Effects and How to Reduce It Naturally
Learn what chronic inflammation is, what causes it, how to test for it, and the evidence-based diet, lifestyle, and supplement strategies proven to reduce it naturally.
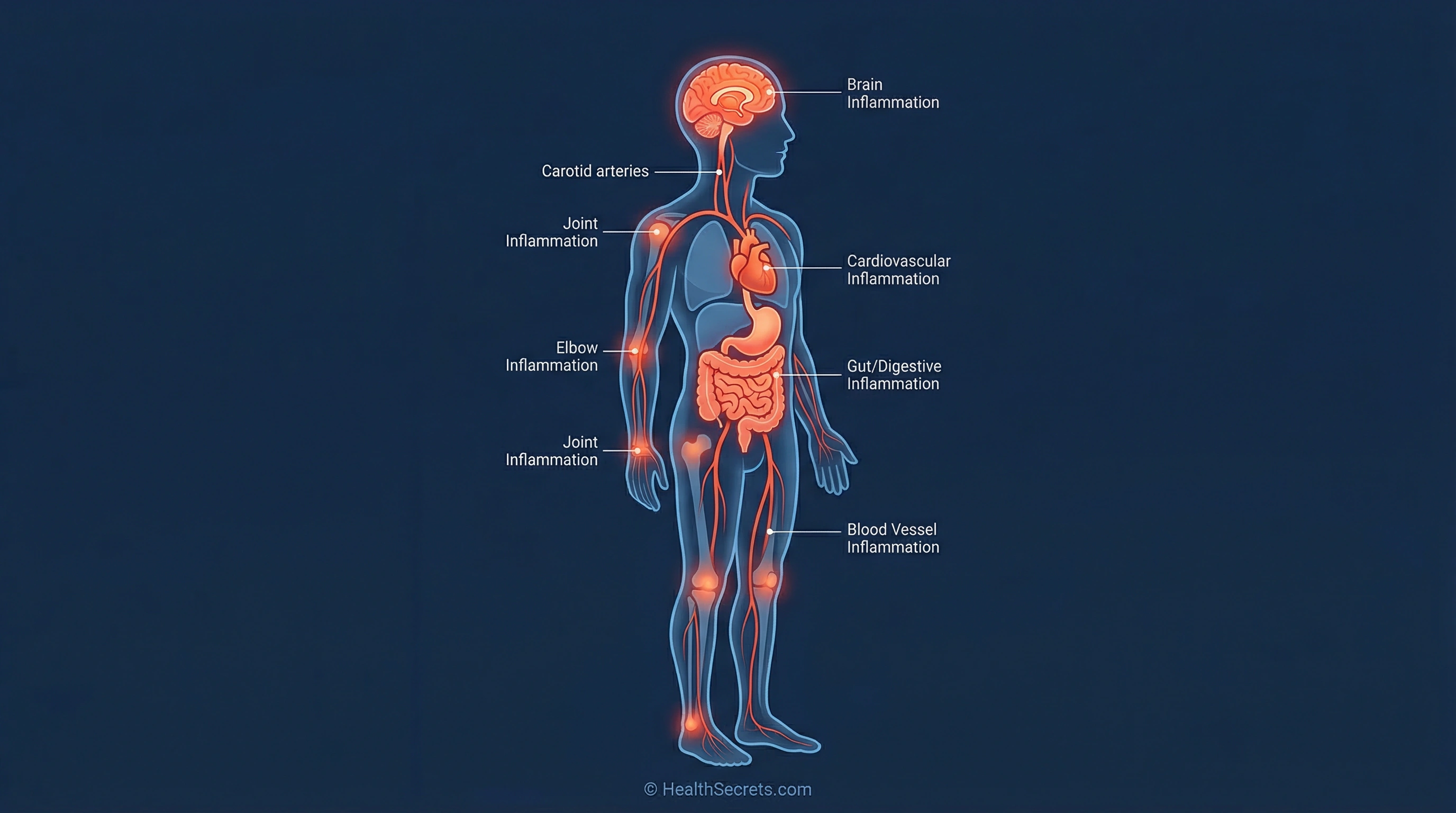
Here's something most people don't realize: the biggest threat to your long-term health probably isn't a dramatic event like a heart attack or a sudden diagnosis. It's something far quieter. Chronic low-grade inflammation — sometimes called "silent inflammation" — operates beneath the surface for months or even years, slowly damaging tissues and driving disease progression before you notice a single symptom.
Researchers now link chronic inflammation to seven of the ten leading causes of death in the United States. That includes cardiovascular disease, type 2 diabetes, cancer, Alzheimer's disease, and autoimmune conditions. The good news? Chronic inflammation is largely preventable and, in many cases, reversible through targeted changes to your diet, lifestyle, and supplement routine.
In this guide, you'll learn exactly what chronic inflammation is, what triggers it, how to test for it, and — most importantly — the evidence-based strategies that can help you bring it under control.
If you're looking for a comprehensive overview of inflammation science, start with our inflammation guide. For targeted dietary strategies, explore our guide to anti-inflammatory foods.
- Chronic inflammation is a persistent, low-grade immune response that lasts months to years and is linked to cardiovascular disease, diabetes, cancer, Alzheimer's, and autoimmune conditions.
- Unlike acute inflammation (which heals injuries), chronic inflammation damages healthy tissues and often produces no obvious symptoms until disease develops.
- Primary causes include poor diet (processed foods, excess sugar, trans fats), chronic stress, obesity, gut dysbiosis, environmental toxins, lack of sleep, and a sedentary lifestyle.
- High-sensitivity C-reactive protein (hs-CRP) is the most accessible test — optimal levels are below 1.0 mg/L, and levels above 3.0 mg/L indicate high cardiovascular risk.
- The Mediterranean diet is the gold standard for reducing inflammation, with meta-analyses showing significant reductions in hs-CRP and IL-6.
- Weight loss of just 10% in overweight individuals can reduce inflammatory markers by 30–50%, making it one of the most powerful interventions available.
- Key anti-inflammatory supplements include omega-3 fatty acids (2–4g EPA+DHA daily), curcumin (1,000–1,500mg with BioPerine), and vitamin D (optimized to 40–60 ng/mL).
- Lifestyle factors work synergistically — combining diet, stress management, quality sleep (7–9 hours), and regular moderate exercise produces the greatest anti-inflammatory effect.
What Is Chronic Inflammation and How Does It Differ from Acute Inflammation?
Chronic inflammation is a persistent, low-grade immune response that lasts for months or years, silently damaging tissues throughout your body. Unlike acute inflammation — which is a short-term, protective response to injury or infection — chronic inflammation doesn't resolve on its own and is now recognized as a root driver of most modern chronic diseases.
Acute Inflammation: Your Body's Protective Response
When you cut your finger or catch a cold, your immune system launches an acute inflammatory response. White blood cells rush to the site, releasing inflammatory mediators like cytokines, prostaglandins, and histamine. You experience the classic signs — redness, heat, swelling, and pain — as your body fights the threat and repairs the damage. Within hours to days, the process resolves and your body returns to normal. This type of inflammation is essential for survival.
Chronic Inflammation: When the Alarm Never Turns Off
Chronic inflammation is fundamentally different. Instead of a targeted, short-term response, your immune system stays activated at a low level continuously. Pro-inflammatory cytokines like interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-α) circulate through your bloodstream, causing gradual tissue damage that accumulates over time. The process is systemic — affecting your entire body rather than one localized area — and it's often completely asymptomatic until a disease diagnosis reveals the underlying damage.
Researchers sometimes call this "inflammaging" because the same chronic inflammatory process that drives disease also accelerates biological aging. Elevated C-reactive protein (CRP), the most commonly measured inflammatory marker, is found in individuals with cardiovascular disease, diabetes, obesity, depression, and neurodegenerative conditions.
The key distinction is simple: acute inflammation is specific, localized, and resolves — it protects you. Chronic inflammation is diffuse, systemic, and persistent — it destroys you.
What Causes Chronic Inflammation to Develop in Your Body?
Chronic inflammation develops when your immune system encounters persistent triggers — poor diet, chronic stress, excess body fat, gut dysfunction, toxins, and sleep deprivation — that keep inflammatory pathways activated long after they should have shut down. Understanding these root causes is the first step toward reducing your inflammatory burden.
Poor Diet: The Primary Driver
The Western diet — high in processed foods, refined sugars, trans fats, and excess omega-6 fatty acids — is the single largest contributor to chronic inflammation. Refined carbohydrates and added sugars trigger the release of inflammatory cytokines including IL-6 and TNF-α. Trans fats (found in fried and processed foods) directly elevate CRP levels. The typical Western diet delivers an omega-6 to omega-3 ratio of 15–20:1, far above the optimal 4:1 or less, promoting the production of pro-inflammatory eicosanoids.
Chronic Stress and Cortisol Dysregulation
Short-term stress is actually anti-inflammatory — cortisol helps control the immune response. But under chronic stress, your cells develop cortisol resistance, meaning they stop responding to cortisol's anti-inflammatory signals. The result is paradoxical: high cortisol levels alongside rising inflammation. Chronic psychological stress activates NF-κB, a master inflammatory pathway, and disrupts the gut barrier, contributing to endotoxemia.
Obesity: Fat as an Inflammatory Organ
Adipose tissue — especially visceral belly fat — is not just an energy storage depot. It actively produces inflammatory cytokines including IL-6, TNF-α, and pro-inflammatory adipokines. Research consistently shows that obesity is associated with 2–3 times higher CRP levels compared to normal weight. Macrophages infiltrate fat tissue, creating a self-perpetuating inflammatory cycle. Importantly, even modest weight loss of 10% can reduce CRP by 30–50%.
Gut Dysbiosis and Leaky Gut
Your gut microbiome plays a central role in immune regulation. When the balance shifts toward pathogenic bacteria (dysbiosis), the intestinal barrier can weaken — a condition called increased intestinal permeability or "leaky gut." This allows bacterial endotoxins like lipopolysaccharide (LPS) to enter the bloodstream, triggering systemic inflammation. Poor diet, chronic stress, NSAIDs, antibiotics, and excess alcohol all contribute to gut barrier dysfunction. For a deeper dive, see our gut health and inflammation guide.
Environmental Toxins
Air pollution (particularly PM2.5 particulate matter), heavy metals (lead, mercury, cadmium), pesticides, and endocrine-disrupting plastics (BPA, phthalates) all trigger inflammatory pathways. Long-term air pollution exposure is associated with elevated CRP and increased cardiovascular disease risk.
Sleep Deprivation and Sedentary Lifestyle
Sleeping fewer than seven hours per night is consistently associated with elevated CRP, IL-6, and TNF-α — some studies show inflammatory markers rise by 40–60% with chronic sleep restriction. Similarly, sedentary behavior independently increases inflammation. Moderate exercise, by contrast, releases anti-inflammatory myokines (IL-10, IL-1ra), making it one of the most effective anti-inflammatory interventions available.
What Are the Major Health Consequences of Chronic Inflammation?
Chronic inflammation is implicated in the development and progression of virtually every major chronic disease. Research shows it contributes to cardiovascular disease, type 2 diabetes, cancer, Alzheimer's, depression, autoimmune conditions, and accelerated aging — affecting nearly every organ system in the body.
Does Chronic Inflammation Cause Heart Disease?
Yes — chronic inflammation is now recognized as a central driver of atherosclerosis. Inflammation damages the endothelial lining of blood vessels, promotes LDL oxidation (making cholesterol more dangerous), and destabilizes arterial plaques, increasing the risk of heart attack and stroke. Elevated hs-CRP above 3.0 mg/L is associated with a 2–3 times higher cardiovascular risk. The landmark CANTOS trial demonstrated that targeting inflammation with canakinumab (an IL-1β inhibitor) reduced cardiovascular events by 15% — proving inflammation directly causes cardiovascular disease, not just correlates with it.
Can Chronic Inflammation Lead to Type 2 Diabetes?
Inflammatory cytokines — particularly TNF-α and IL-6 — directly impair insulin signaling by activating NF-κB and blocking insulin receptor pathways. This leads to insulin resistance, the hallmark of type 2 diabetes. A major meta-analysis published in Diabetes Care found that elevated IL-6 and CRP are significant, independent predictors of type 2 diabetes development. Inflammation from visceral adipose tissue creates a vicious cycle: obesity causes inflammation, which worsens insulin resistance, which promotes further weight gain.
How Does Chronic Inflammation Contribute to Cancer?
The National Cancer Institute states that chronic inflammation accounts for approximately 15–20% of all cancers. Inflammatory free radicals cause DNA mutations, while inflammatory signaling promotes angiogenesis (blood vessel growth to tumors), suppresses anti-tumor immunity, and facilitates metastasis. Well-established examples include inflammatory bowel disease leading to colon cancer, chronic hepatitis leading to liver cancer, and H. pylori infection leading to stomach cancer.
Does Chronic Inflammation Affect Brain Health and Alzheimer's Risk?
Neuroinflammation — driven by chronically activated microglia (the brain's immune cells) — promotes amyloid and tau protein accumulation, disrupts the blood-brain barrier, and damages neurons. Elevated inflammatory markers including CRP and IL-6 are associated with a 2–3 times higher risk of developing Alzheimer's disease. Chronic inflammation also impairs amyloid clearance, accelerating the neurodegenerative process.
Can Chronic Inflammation Cause Depression and Mental Health Issues?
Emerging research shows that inflammatory cytokines cross the blood-brain barrier and disrupt neurotransmitter metabolism. Specifically, inflammation shifts tryptophan metabolism away from serotonin production through the kynurenine pathway, depleting mood-regulating neurotransmitters. Elevated CRP and IL-6 are associated with 50–100% higher depression risk. Some studies show that anti-inflammatory interventions, including omega-3 fatty acids, improve depressive symptoms.
How Does Chronic Inflammation Accelerate Aging?
"Inflammaging" — the age-related increase in chronic low-grade inflammation — accelerates telomere shortening, promotes cellular senescence ("zombie cells" that secrete inflammatory factors), and drives muscle loss (sarcopenia), cognitive decline, and frailty. Elevated inflammatory markers are consistently associated with shorter lifespan and accelerated biological aging. For more on the aging and inflammation connection, understanding inflammaging is critical.
What Are the Risks of Ignoring Chronic Inflammation and How Do You Test for It?
The greatest risk of chronic inflammation is that it often produces no obvious symptoms until significant disease has developed. Testing inflammatory markers — particularly hs-CRP — is the most practical way to detect and monitor chronic inflammation before it causes irreversible damage.
High-Sensitivity C-Reactive Protein (hs-CRP)
hs-CRP is the most widely available and clinically validated test for chronic inflammation. CRP is an acute-phase protein produced by the liver in response to inflammatory signaling.
Optimal ranges:
- Below 1.0 mg/L: Low risk (optimal for health)
- 1.0–3.0 mg/L: Moderate risk
- Above 3.0 mg/L: High risk (elevated cardiovascular and chronic disease risk)
- Above 10 mg/L: Likely acute inflammation (infection, injury — not chronic)
Important: Test hs-CRP twice, two weeks apart, to confirm chronic versus acute elevation. A single reading above 10 mg/L may reflect a temporary infection.
Additional Inflammatory Markers
- Interleukin-6 (IL-6): A key pro-inflammatory cytokine and more specific than CRP, but not routinely tested clinically.
- TNF-α: Master regulator of inflammation and target of biologic drugs for autoimmune diseases.
- ESR (Erythrocyte Sedimentation Rate): Less specific than CRP but sometimes used alongside it.
- Fibrinogen: Elevated in inflammation and increases clotting risk.
- Homocysteine: Elevated in inflammation and B-vitamin deficiency; optimal levels are below 10 μmol/L.
When to Test
- Baseline: If you have risk factors including obesity, poor diet, family history of chronic disease, or chronic stress.
- Monitoring: Every 6–12 months while implementing anti-inflammatory lifestyle changes.
- Cardiovascular risk: hs-CRP is increasingly included in standard cardiovascular risk assessments.
For more on inflammation markers and testing, see our dedicated guide.
How Can You Reduce Chronic Inflammation with Supplements and Protocols?
Reducing chronic inflammation requires a multi-pronged approach combining targeted supplements with foundational diet and lifestyle changes. The most evidence-backed supplements — omega-3 fatty acids, curcumin, vitamin D, probiotics, and ashwagandha — can significantly lower inflammatory markers when used consistently alongside dietary improvements.
Omega-3 Fatty Acids (EPA + DHA)
Take 2–4g of combined EPA and DHA daily, ideally with a higher EPA ratio (2:1 EPA:DHA). Research shows omega-3 supplementation reduces CRP and IL-6 by 20–30%. Choose triglyceride-form fish oil for better absorption. For more on omega-3 for inflammation, see our supplement guide.
Curcumin (Turmeric Extract)
Take 1,000–1,500mg daily of curcumin standardized to 95% curcuminoids, always with BioPerine (piperine) for absorption. Studies show curcumin can reduce inflammatory markers by 30–40%. Learn more in our guide to turmeric for inflammation.
Vitamin D3
Optimize levels to 40–60 ng/mL with 2,000–5,000 IU daily. Vitamin D supplementation significantly reduces CRP in deficient individuals. Test your levels before supplementing.
Probiotics
Take 10–50 billion CFU daily of a multi-strain formula containing Lactobacillus and Bifidobacterium species. Research shows probiotics reduce CRP and support the gut-immune axis.
Ashwagandha (KSM-66)
Take 600mg daily of KSM-66 ashwagandha root extract. Clinical studies show it reduces cortisol and inflammatory markers, addressing the stress-inflammation connection.
Quercetin
Take 500–1,000mg daily. This flavonoid antioxidant acts as a mast cell stabilizer and has been shown to significantly decrease total cholesterol, LDL, and CRP in meta-analyses.
Supplement Protocol Timeline
- Weeks 1–2: Start omega-3 and vitamin D3.
- Weeks 2–4: Add curcumin and probiotics.
- Week 4+: Add ashwagandha and quercetin if needed.
- Week 12: Retest hs-CRP to measure progress.
What Diet and Lifestyle Changes Help Fight Chronic Inflammation?
The Mediterranean diet is the gold standard anti-inflammatory eating pattern, with meta-analyses of randomized controlled trials showing significant reductions in hs-CRP and IL-6. Combined with stress management, quality sleep, regular exercise, and toxin reduction, lifestyle changes provide the foundation that makes supplement protocols effective.
The Anti-Inflammatory Diet
Prioritize these foods daily:
- Fatty fish (salmon, sardines, mackerel) — 2–3 servings weekly for omega-3
- Colorful vegetables and leafy greens — 5–9 servings daily for polyphenols and antioxidants
- Berries (blueberries, strawberries) — daily for anthocyanins
- Extra virgin olive oil — 2–3 tablespoons daily (contains oleocanthal, a natural COX-2 inhibitor)
- Nuts and seeds (walnuts, flaxseeds) — 1–2 oz daily
- Spices — turmeric, ginger, cinnamon, garlic daily
- Green tea — 2–3 cups daily for EGCG
Eliminate or minimize:
- Processed foods, fast food, and refined carbohydrates
- Added sugars and sugary beverages
- Trans fats (fried foods, margarine, baked goods)
- Excess omega-6 vegetable oils (soybean, corn, sunflower) — replace with olive or avocado oil
- Excess alcohol (more than 1–2 drinks per day)
Explore our complete anti-inflammatory foods guide for detailed meal planning.
Stress Management
- Meditation: 10–20 minutes daily reduces cortisol and inflammatory markers by 15–25%.
- Yoga or tai chi: 2–3 times weekly combines movement, breathing, and stress reduction.
- Nature exposure: Weekly time in nature measurably reduces stress hormones.
- Adaptogenic herbs: Ashwagandha and rhodiola support the stress-cortisol-inflammation axis.
Sleep Optimization
- Target 7–9 hours nightly — sleep deprivation directly elevates CRP and IL-6.
- Maintain a consistent sleep-wake schedule.
- Keep your bedroom dark (blackout curtains) and cool (65–68°F).
- Get morning light exposure within 1–2 hours of waking to set circadian rhythm.
- Limit screens 2–3 hours before bed.
Regular Exercise
- 150 minutes weekly of moderate aerobic exercise (walking, cycling, swimming) reduces CRP by 20–30%.
- Add resistance training 2–3 times weekly.
- Avoid overtraining — excessive exercise increases inflammation.
- Recovery and rest days are essential.
Weight Management
If overweight, target a 10% reduction in body weight through a 500–750 calorie daily deficit. This single intervention can reduce inflammation by 30–50% — more than most supplements.
Reduce Toxin Exposure
- Filter your drinking water (removes heavy metals and chlorine).
- Use a HEPA air filter indoors.
- Choose organic produce when possible (prioritize the Dirty Dozen).
- Use glass or stainless steel food containers instead of plastic.
Address Oral Health
Periodontal disease is a common and overlooked source of systemic inflammation. Regular dental cleanings and good oral hygiene can reduce inflammatory markers.
What Is the Best Step-by-Step Plan to Reduce Chronic Inflammation?
The most effective approach to reducing chronic inflammation follows a phased timeline — starting with testing and dietary changes, then layering in lifestyle modifications and targeted supplements. Most people see measurable improvements in inflammatory markers within 8–12 weeks of consistent effort.
Phase 1 — Test and Eliminate (Weeks 1–2):
- [ ] Get baseline hs-CRP, lipid panel, fasting glucose, HbA1c, and vitamin D levels
- [ ] Remove processed foods, added sugars, trans fats, and excess omega-6 oils
- [ ] Begin Mediterranean-style eating with emphasis on vegetables, fatty fish, olive oil, and berries
- [ ] Start omega-3 (2–4g EPA+DHA) and vitamin D3 (2,000–5,000 IU)
Phase 2 — Build the Foundation (Weeks 3–4):
- [ ] Add curcumin (1,000–1,500mg with BioPerine) and probiotics (10–50 billion CFU)
- [ ] Establish daily stress management practice (10–20 min meditation or deep breathing)
- [ ] Optimize sleep environment and commit to 7–9 hours nightly
- [ ] Begin moderate exercise routine (30 min, 5 times per week)
Phase 3 — Optimize and Monitor (Weeks 5–12):
- [ ] Add ashwagandha (600mg KSM-66) and quercetin (500–1,000mg) if needed
- [ ] Add resistance training 2–3 times per week
- [ ] Address gut health with prebiotic-rich foods (onions, garlic, asparagus, oats)
- [ ] Reduce toxin exposure (water filter, HEPA filter, glass containers)
Phase 4 — Retest and Maintain (Week 12+):
- [ ] Retest hs-CRP (goal: below 1.0 mg/L)
- [ ] Retest vitamin D (goal: 40–60 ng/mL)
- [ ] Assess body composition and symptom improvements
- [ ] Continue anti-inflammatory lifestyle as long-term maintenance
- [ ] Retest annually and adjust as needed
Expected timeline: Initial energy and digestive improvements in weeks 1–4. Measurable CRP reductions typically appear by weeks 8–12. Long-term disease risk reduction builds over months to years of consistent practice.
References
- Pahwa R, Goyal A, Jialal I. Chronic Inflammation. StatPearls. 2023. Source
- Furman D, et al. Chronic inflammation in the etiology of disease across the life span. Nature Medicine. 2019;25(12):1822-1832. Source
- National Cancer Institute. Chronic Inflammation. Source
- Ridker PM, et al. Antiinflammatory Therapy with Canakinumab for Atherosclerotic Disease. N Engl J Med. 2017;377(12):1119-1131. Source
- Wang X, et al. Inflammatory Markers and Risk of Type 2 Diabetes: A Systematic Review and Meta-analysis. Diabetes Care. 2013;36(1):166-175. Source
- Coussens LM, Werb Z. Inflammation and cancer. Nature. 2002;420(6917):860-867. Source
- Heneka MT, et al. Neuroinflammation in Alzheimer's disease. Lancet Neurol. 2015;14(4):388-405. Source
- Irwin MR, et al. Sleep Disturbance, Sleep Duration, and Inflammation: A Systematic Review and Meta-Analysis. Biol Psychiatry. 2016;80(1):40-52. Source
- Pedersen BK. Anti-inflammatory effects of exercise: role in diabetes and cardiovascular disease. Eur J Clin Invest. 2017;47(8):600-611. Source
- Estruch R, et al. Primary Prevention of Cardiovascular Disease with a Mediterranean Diet Supplemented with Extra-Virgin Olive Oil or Nuts. N Engl J Med. 2018;378(25):e34. Source
- Kheirouri S, et al. Mediterranean Diet Reduces Inflammation in Adults: A Systematic Review and Meta-analysis of Randomized Controlled Trials. 2025. Source
- Black DS, Slavich GM. Mindfulness meditation and the immune system: a systematic review. Ann N Y Acad Sci. 2016;1373(1):13-24. Source
Frequently asked questions
What is chronic inflammation in simple terms?
Chronic inflammation is a persistent, low-grade activation of your immune system that lasts for months or years. Unlike the short-term inflammation you get from a cut or cold, chronic inflammation doesn't resolve on its own and gradually damages healthy tissues throughout your body, contributing to diseases like heart disease, diabetes, and cancer.
What are the early warning signs of chronic inflammation?
Early signs can be subtle and include persistent fatigue, unexplained body aches, frequent infections, digestive issues (bloating, constipation, diarrhea), brain fog, weight gain (especially around the midsection), skin problems, and mood changes like anxiety or depression. Many people have no noticeable symptoms at all, which is why testing hs-CRP is valuable.
How do you test for chronic inflammation?
The most practical test is a high-sensitivity C-reactive protein (hs-CRP) blood test, which your doctor can order. Optimal levels are below 1.0 mg/L. Test twice, two weeks apart, to confirm chronic versus acute elevation. Additional markers like IL-6, ESR, and homocysteine may provide further insight.
What is a normal CRP level and what level is dangerous?
Optimal hs-CRP is below 1.0 mg/L. Levels between 1.0 and 3.0 mg/L indicate moderate inflammation and cardiovascular risk. Levels above 3.0 mg/L indicate high risk and warrant lifestyle intervention. Levels above 10 mg/L typically suggest acute infection or injury rather than chronic inflammation.
What foods cause the most inflammation?
The most inflammatory foods include processed and ultra-processed foods, refined sugars and high-fructose corn syrup, trans fats (fried foods, margarine), excess omega-6 vegetable oils (soybean, corn, sunflower oil), refined carbohydrates (white bread, pastries), processed meats, and excessive alcohol. These foods trigger inflammatory cytokine release and elevate CRP.
What is the best diet to reduce chronic inflammation?
The Mediterranean diet is the most studied and effective anti-inflammatory eating pattern. It emphasizes vegetables, fruits, fatty fish, olive oil, nuts, seeds, and whole grains while limiting processed foods, sugar, and unhealthy fats. Meta-analyses of randomized controlled trials show it significantly reduces hs-CRP and IL-6.
How long does it take to reduce chronic inflammation?
Most people begin feeling improvements in energy and digestion within 2–4 weeks of consistent dietary and lifestyle changes. Measurable reductions in inflammatory markers like CRP typically appear within 8–12 weeks. Full optimization of inflammatory status may take 3–6 months of sustained effort.
Can chronic inflammation be reversed?
Yes, in most cases chronic inflammation can be significantly reduced and even reversed through lifestyle changes. Anti-inflammatory diet, regular moderate exercise, stress management, quality sleep, weight loss (if overweight), and targeted supplements can lower inflammatory markers to optimal levels. The earlier you intervene, the more reversible the damage.
What supplements are best for reducing inflammation?
The most evidence-backed anti-inflammatory supplements are omega-3 fatty acids (2–4g EPA+DHA daily), curcumin with BioPerine (1,000–1,500mg daily), vitamin D3 (optimized to 40–60 ng/mL), probiotics (10–50 billion CFU multi-strain), and ashwagandha (600mg KSM-66). Quercetin and magnesium glycinate provide additional support.
Does chronic inflammation cause weight gain?
Yes, chronic inflammation and weight gain create a vicious cycle. Inflammatory cytokines impair insulin signaling, promoting fat storage — especially visceral belly fat. That fat tissue then produces more inflammatory cytokines, worsening the problem. Breaking this cycle through anti-inflammatory diet and exercise addresses both issues simultaneously.