natural remedies
Types of Insomnia | Natural Treatments & CBT-I Guide
Learn about sleep onset, maintenance, and early awakening insomnia. Discover CBT-I, sleep restriction, stimulus control, and natural treatments that work.
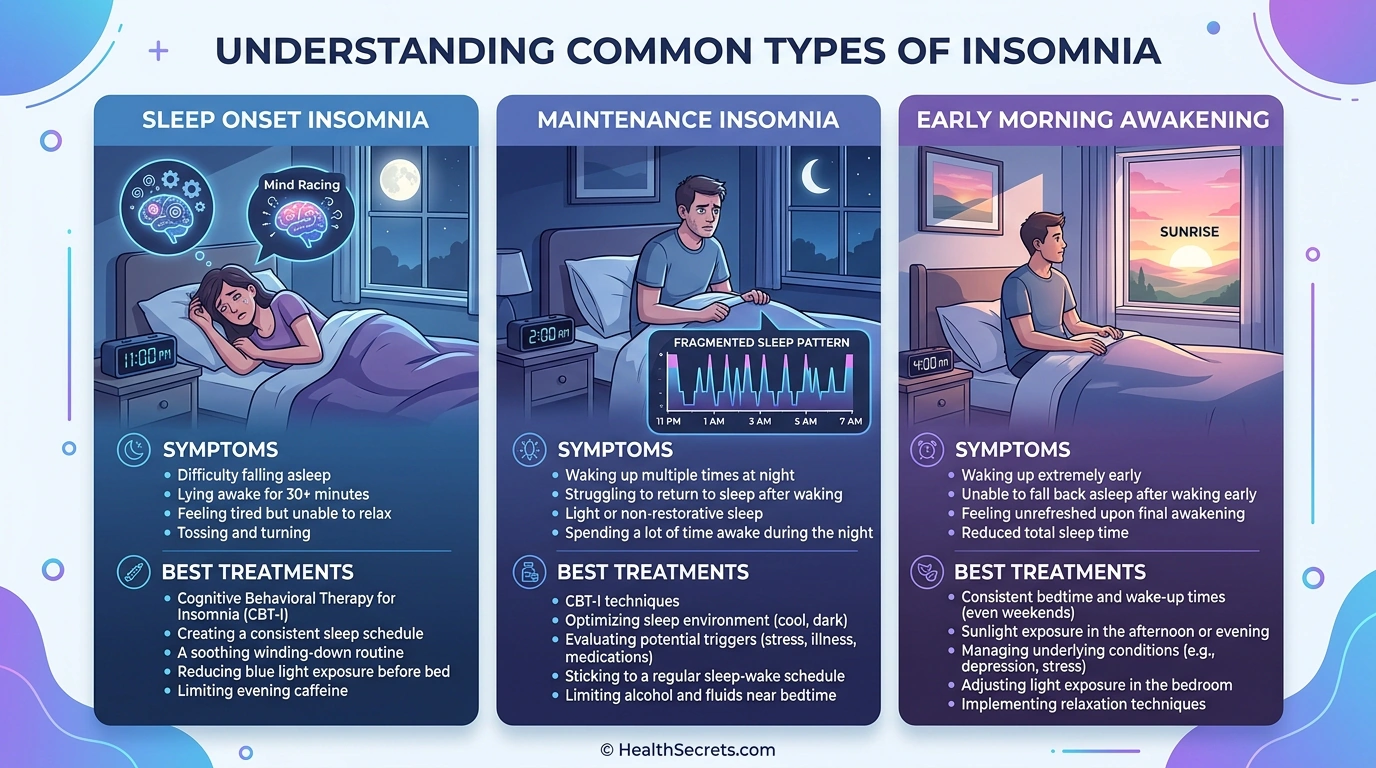
Here's something most people get wrong about insomnia: they treat it like a single problem with a single fix. Pop a melatonin, download a sleep app, hope for the best. But the types of insomnia you're dealing with — sleep onset, maintenance, or early morning awakening — change everything about which treatments will actually help.
And the numbers are staggering. Roughly 30–35% of adults experience insomnia symptoms at some point, and 10–15% live with chronic insomnia that disrupts their daily functioning. That's not a minor inconvenience. That's a public health problem hiding in plain sight.
The genuinely good news? Cognitive Behavioral Therapy for Insomnia (CBT-I) is now considered the most effective nonpharmacologic treatment for chronic insomnia, with better overall value than pharmacotherapy. It's a short, structured, evidence-based approach that addresses the root causes of sleeplessness — not just the symptoms. And unlike sleeping pills, the benefits actually persist after treatment ends.
This guide walks you through every major insomnia type, the evidence-based natural treatments for each, and exactly when it's time to call in a specialist. For broader context on how sleep connects to emotional resilience, explore our mental wellness complete guide and sleep optimization guide.
- Insomnia has three main types by timing: sleep onset (can't fall asleep), maintenance (can't stay asleep), and early morning awakening (waking hours too early)
- Acute insomnia lasts under 3 months and often resolves on its own, while chronic insomnia persists 3+ months and requires structured treatment
- CBT-I is the gold standard treatment for chronic insomnia — more effective long-term than sleeping pills with no side effects or dependence
- Sleep restriction therapy paradoxically limits time in bed to consolidate sleep, and stimulus control reassociates the bed with sleep rather than wakefulness
- Sleep hygiene basics — cool dark room (60–67°F), consistent schedule, no screens before bed, no caffeine after noon — form the foundation of every insomnia treatment plan
- Natural supplements like melatonin (0.5–5mg) and magnesium glycinate (200–400mg) can support sleep but are not replacements for CBT-I
- 70–80% of people with chronic insomnia see significant improvement with CBT-I within 4–8 weeks
- Early morning awakening insomnia is frequently linked to depression and may require treatment of the underlying mood disorder
What Are the Different Types of Insomnia and How Do They Differ?
Insomnia is a sleep disorder defined by difficulty falling asleep, staying asleep, or waking too early — combined with daytime impairment like fatigue, mood changes, and concentration problems. The three main types are classified by timing: sleep onset insomnia, maintenance insomnia, and early morning awakening insomnia, each with distinct causes and treatment approaches.
What Is Sleep Onset Insomnia?
Sleep onset insomnia means taking 30 or more minutes to fall asleep, often much longer. Your mind races. Your body feels wired despite exhaustion. This type is driven by hyperarousal — both physiological (racing heart, muscle tension) and cognitive (spiraling thoughts, worry). Over time, your brain starts associating the bed with wakefulness rather than sleep, creating a conditioned arousal pattern that feeds on itself.
Common triggers include anxiety, performance pressure about sleep itself, late caffeine use, screen exposure before bed, and irregular sleep schedules. Stimulus control therapy is particularly effective for this type, as it breaks the bed-wakefulness association.
What Is Maintenance Insomnia?
Maintenance insomnia means waking multiple times during the night with awakenings lasting 20+ minutes. Sleep feels light, fragmented, and easily disrupted. This type often stems from medical conditions (chronic pain, sleep apnea), medications, alcohol use (which disrupts sleep architecture), or stress that activates the mind during natural nighttime awakenings.
Aging also plays a role — sleep architecture naturally shifts with age, producing lighter and more fragmented sleep.
What Is Early Morning Awakening Insomnia?
Early morning awakening insomnia means waking 2+ hours before your desired time with an inability to fall back asleep. This type has a strong association with depression — it's considered a classic symptom. Circadian rhythm shifts (advanced sleep phase) and age-related changes also contribute. Light therapy in the evening can help delay the sleep phase for those with circadian involvement.
How Does Acute Insomnia Differ from Chronic Insomnia?
Acute insomnia lasts under 3 months and is typically triggered by a specific stressor — a work deadline, relationship conflict, illness, or major life change. It often resolves when the stressor passes. Chronic insomnia persists 3+ months, occurring 3+ nights per week, and becomes self-perpetuating even after the original trigger disappears. Poor sleep habits formed during acute insomnia (napping, staying in bed awake, irregular schedules) cement the cycle into chronic territory.
What Causes Insomnia and Why Does It Become Chronic?
Insomnia stems from a combination of predisposing factors (genetics, temperament), precipitating events (stress, illness, life changes), and perpetuating behaviors (poor sleep habits, catastrophic thinking about sleep). The transition from acute to chronic insomnia happens when maladaptive coping strategies — spending more time in bed, napping, worrying about sleep — replace the original trigger as the primary driver.
The most common causes include:
- Stress and anxiety — the leading triggers, activating the body's fight-or-flight response at precisely the wrong time
- Depression and mood disorders — particularly linked to early morning awakening patterns
- Poor sleep hygiene — irregular schedules, screens before bed, caffeine and alcohol use
- Medical conditions — chronic pain, thyroid disorders, sleep apnea, restless leg syndrome, acid reflux
- Medications — stimulants, certain antidepressants, corticosteroids, beta-blockers
- Circadian rhythm disruption — shift work, jet lag, inconsistent sleep-wake times
- Aging — natural changes in sleep architecture produce lighter, more fragmented sleep
What makes chronic insomnia so frustrating is the vicious cycle: initial sleep loss creates anxiety about sleep, which triggers hyperarousal at bedtime, which causes more sleep loss, which deepens the anxiety. CBT-I specifically targets this cycle by restructuring the thoughts and behaviors that maintain it.
What Symptoms Indicate You Have Insomnia Rather Than Normal Poor Sleep?
Clinical insomnia goes beyond the occasional rough night. The defining feature is persistent difficulty initiating or maintaining sleep — combined with adequate opportunity to sleep and clinically meaningful daytime impairment. Symptoms must occur despite having enough time and a suitable environment for sleep, ruling out external factors like noise or an infant waking you.
Primary symptoms by type:
- Sleep onset: Lying awake 30+ minutes, racing thoughts, physical tension, dreading bedtime
- Maintenance: Multiple nighttime awakenings, long periods of wakefulness (20+ minutes), light or fragmented sleep
- Early morning awakening: Waking 2+ hours before desired time, inability to return to sleep, feeling unrested
Daytime consequences (required for diagnosis):
- Fatigue and low energy despite adequate time in bed
- Difficulty concentrating, memory lapses, impaired decision-making
- Mood disturbances — irritability, anxiety, depressed mood
- Reduced motivation and performance at work or school
- Increased errors and accidents (including drowsy driving)
- Social withdrawal and relationship strain
A critical distinction: wanting more sleep doesn't equal insomnia. Some people are naturally short sleepers. Insomnia is defined by difficulty sleeping plus functional impairment.
How Is Insomnia Diagnosed and When Do You Need a Sleep Study?
Insomnia is primarily diagnosed through clinical interview and sleep history — not lab tests. Your healthcare provider will ask about sleep patterns, duration of symptoms, daytime impact, medical history, medication use, and mental health. A 2-week sleep diary tracking bedtime, wake time, time to fall asleep, nighttime awakenings, and daytime functioning provides critical diagnostic data.
Key questions to ask your doctor:
- Could an underlying medical condition be causing my insomnia?
- Should I be screened for sleep apnea or restless leg syndrome?
- Are any of my medications contributing to sleep problems?
- Is CBT-I available through your practice or a referral?
:::info[When a sleep study is needed:] Polysomnography (overnight sleep study) isn't routinely required for insomnia diagnosis but is indicated when another sleep disorder is suspected — particularly sleep apnea (snoring, gasping, witnessed breathing pauses), restless leg syndrome, or periodic limb movement disorder. Home sleep tests can screen for sleep apnea in lower-risk patients. :::
Actigraphy — a wrist-worn device tracking movement and rest patterns over 1–2 weeks — can help assess circadian rhythm disorders and validate sleep diary data.
Why Is CBT-I the Gold Standard Treatment for Chronic Insomnia?
Cognitive Behavioral Therapy for Insomnia (CBT-I) is the most effective nonpharmacological treatment for chronic insomnia because it addresses the root behavioral and cognitive patterns that perpetuate sleeplessness, rather than masking symptoms. Research consistently shows CBT-I produces better long-term outcomes than pharmacotherapy, with a 70–80% response rate and benefits that persist well after treatment ends.
CBT-I focuses on restructuring the thoughts, feelings, and behaviors contributing to insomnia using several core components:
How Does Sleep Restriction Therapy Work?
Sleep restriction paradoxically limits your time in bed to match your actual sleep time. If you're sleeping 5 hours but spending 8 hours in bed, your sleep window shrinks to 5 hours. This builds homeostatic sleep pressure, consolidates fragmented sleep, and improves sleep efficiency. Time in bed gradually increases as sleep quality improves. Sleep restriction therapy and stimulus control therapy show promise as highly effective interventions for chronic insomnia.
It's initially challenging — expect temporary daytime fatigue during the first 1–2 weeks. But the payoff is substantial.
How Does Stimulus Control Therapy Treat All Types of Insomnia?
Stimulus control reassociates the bed with sleep instead of wakefulness. The rules are straightforward: go to bed only when sleepy, use the bed only for sleep and intimacy, leave the bedroom if you haven't fallen asleep within 15–20 minutes, return only when sleepy, wake at the same time every morning regardless of sleep quality, and avoid napping. Research confirms stimulus control therapy is effective for the treatment of all types of insomnia.
What Role Does Cognitive Therapy Play?
Cognitive therapy targets the dysfunctional beliefs that fuel insomnia — catastrophic thinking ("I'll never function tomorrow"), unrealistic expectations ("I need exactly 8 hours"), and performance anxiety about sleep itself. Cognitive restructuring helps you challenge these patterns, reducing the hyperarousal that keeps you awake.
CBT-I vs. sleeping pills:
- Benefits persist after treatment ends (pills only work while taking them)
- No side effects, no tolerance, no dependence
- Addresses root causes rather than masking symptoms
- 70–80% see significant improvement within 4–8 weeks
CBT-I is available through sleep specialists, online programs (digital CBT-I), self-help books, and dedicated apps.
What Natural Treatments Help Different Types of Insomnia?
The most effective natural treatments for insomnia combine sleep hygiene optimization, relaxation techniques, strategic exercise timing, and targeted supplementation. The specific combination depends on your insomnia type — sleep onset responds best to arousal-reduction techniques, maintenance insomnia to sleep consolidation strategies, and early morning awakening to circadian rhythm interventions.
How Does Sleep Hygiene Optimization Improve Sleep Quality?
Sleep hygiene forms the foundation of every insomnia treatment plan:
- Temperature: Keep your bedroom cool — 60–67°F (15–19°C) is optimal, as core body temperature naturally drops during sleep
- Darkness: Use blackout curtains or an eye mask; darkness signals melatonin production
- Noise: A white noise machine masks disruptive sounds; consistent background noise beats intermittent silence
- Schedule consistency: Same wake time every day (including weekends) anchors your circadian rhythm
- Screen curfew: No screens 1 hour before bed — blue light suppresses melatonin and stimulating content activates the brain
- Caffeine cutoff: No caffeine after noon (half-life is 5–6 hours; hidden sources include tea, chocolate, some medications)
- Alcohol avoidance: Alcohol disrupts sleep architecture, reduces REM sleep, and causes middle-of-night awakenings
- Meal timing: No heavy meals 2–3 hours before bed
Which Relaxation Techniques Reduce Sleep Onset Time?
Relaxation techniques directly target the hyperarousal driving sleep onset insomnia:
- Progressive muscle relaxation (PMR): Systematically tense and release muscle groups from head to toe, reducing physical tension and redirecting mental focus away from worries
- 4-7-8 breathing: Exhale fully, inhale through the nose for 4 counts, hold for 7, exhale through the mouth for 8. Repeat 4 times. Activates the parasympathetic nervous system
- Body scan meditation: Mentally scan from head to feet, noticing sensations without judgment — quiets both body and mind
- Guided imagery: Visualize a peaceful scene engaging all senses; distracts from worry and promotes relaxation
How Do Exercise and Stress Management Affect Sleep?
Regular aerobic exercise improves both sleep quality and duration. Timing matters: morning or afternoon exercise is best, as vigorous activity within 3 hours of bedtime can be stimulating. Consistency matters more than intensity — even moderate daily walking shows sleep benefits.
Stress management through journaling, therapy, time management, and setting boundaries addresses one of insomnia's most common root causes.
Which Natural Supplements Support Better Sleep?
Supplements can be supportive tools but are not replacements for CBT-I:
- Melatonin (0.5–5mg): Most effective for circadian rhythm issues (jet lag, shift work). Start low at 0.5–1mg; more is not better. Take 30–60 minutes before bed
- Magnesium glycinate (200–400mg): Supports muscle relaxation and sleep quality. Glycinate form is best absorbed and most calming
- L-theanine (200mg): Amino acid from tea that promotes relaxation without sedation
- Valerian root: Mixed evidence — some studies show modest benefit, others show none
Important: Avoid long-term use of over-the-counter sleeping pills. Tolerance develops, dependence forms, side effects accumulate, and they don't address underlying causes.
How Can You Prevent Acute Insomnia from Becoming Chronic?
Preventing the acute-to-chronic transition requires catching poor sleep habits before they calcify into patterns. The single most important prevention strategy is maintaining consistent sleep-wake times — especially wake time — even during stressful periods when sleep quality drops. Resist the urge to compensate with late mornings, daytime naps, or extended time in bed.
Long-term prevention habits:
- Maintain a consistent wake time 7 days a week (the most powerful circadian anchor)
- Follow stimulus control principles even during good sleep periods
- Manage stress proactively — don't wait until it disrupts sleep
- Limit caffeine to morning hours and alcohol to moderate, early-evening consumption
- Exercise regularly (morning or afternoon preferred)
- Keep your bedroom reserved for sleep and intimacy only
- Address anxiety or depression early — both are strong insomnia risk factors
- Avoid building a dependency on sleep aids during acute episodes
If a stressful period does disrupt your sleep, apply CBT-I principles immediately rather than developing compensatory habits. The faster you respond, the less likely acute insomnia will take root.
When Should You See a Sleep Specialist for Insomnia?
Consult a healthcare provider or sleep specialist if insomnia persists for 3 or more months despite consistent self-help measures, significantly impairs daytime functioning, or is accompanied by symptoms suggesting another sleep disorder. Early intervention prevents the entrenchment of chronic patterns and rules out treatable medical causes.
See a specialist immediately if you experience:
- Suspected sleep apnea: Loud snoring, gasping or choking during sleep, witnessed breathing pauses, morning headaches, excessive daytime sleepiness
- Restless leg syndrome: Uncomfortable crawling or tingling sensations in legs, irresistible urge to move, symptoms worse at night
- Excessive daytime sleepiness: Falling asleep during activities, conversations, or driving
- Insomnia with depression or anxiety: Persistent mood changes, loss of interest, hopelessness — treating the underlying condition often resolves the insomnia
- Medication-related insomnia: Sleep problems began after starting a new medication
- Shift work sleep disorder: Chronic sleep problems tied to night or rotating shifts
A sleep study (polysomnography) isn't typically needed for insomnia diagnosis but rules out sleep apnea, periodic limb movements, and other disorders. Home sleep tests offer a convenient screening option for sleep apnea.
What Is a Step-by-Step Action Plan for Treating Your Insomnia Naturally?
A structured action plan targeting your specific insomnia type produces the fastest results. Start with sleep hygiene and stimulus control foundations, then layer in type-specific strategies over 4–8 weeks. Most people notice meaningful improvement by week 3–4 if they remain consistent.
Phase 1 — Foundation (Weeks 1–2):
- [ ] Identify your insomnia type (sleep onset, maintenance, early awakening, or mixed)
- [ ] Set a consistent wake time and stick to it 7 days a week
- [ ] Optimize bedroom: cool (60–67°F), dark (blackout curtains), quiet (white noise machine)
- [ ] Cut caffeine after noon and alcohol 3+ hours before bed
- [ ] No screens 1 hour before bed
- [ ] Start a sleep diary tracking bedtime, wake time, time to fall asleep, awakenings
Phase 2 — Active Treatment (Weeks 3–6):
- [ ] Implement stimulus control: bed for sleep only, leave if awake 15–20 minutes, return when sleepy
- [ ] Begin sleep restriction: limit time in bed to actual sleep time, increase gradually as efficiency improves
- [ ] Practice relaxation technique nightly (PMR, 4-7-8 breathing, or body scan)
- [ ] Add targeted supplements if desired: magnesium glycinate (200–400mg evening), melatonin (0.5–1mg if circadian issues)
- [ ] Challenge catastrophic sleep thoughts ("I'll never function" → "I've managed before on less sleep")
Phase 3 — Maintenance (Weeks 7–8+):
- [ ] Review sleep diary: calculate sleep efficiency (time asleep ÷ time in bed × 100)
- [ ] Gradually extend sleep window as efficiency exceeds 85%
- [ ] Maintain consistent wake time and stimulus control rules
- [ ] If chronic insomnia persists, seek CBT-I with a trained specialist
- [ ] Address underlying conditions (depression, anxiety, medical issues) with professional support
Frequently asked questions
How long does CBT-I take to work for chronic insomnia?
Most people see meaningful improvement within 4–8 weeks of consistent CBT-I practice. The first 1–2 weeks of sleep restriction may actually feel worse as temporary sleep deprivation builds sleep pressure. By weeks 3–4, sleep typically begins consolidating. Full benefits emerge by weeks 6–8, with 70–80% of people with chronic insomnia reporting significant improvement. Unlike sleeping pills, CBT-I benefits persist long after treatment ends because the underlying behavioral and cognitive patterns have been restructured.
Can you have more than one type of insomnia at the same time?
Yes, mixed insomnia — having difficulty both falling asleep and staying asleep, or combining any of the three types — is common. Many people with chronic insomnia experience overlapping patterns. The treatment approach for mixed insomnia typically combines stimulus control (for sleep onset) with sleep restriction (for consolidation) and addresses any cognitive distortions maintaining the cycle.
Is melatonin effective for all types of insomnia?
No, melatonin is most effective for circadian rhythm-related insomnia — jet lag, shift work, and delayed sleep phase syndrome. It is less effective for chronic insomnia caused by behavioral patterns, anxiety, or medical conditions. For chronic insomnia, CBT-I is significantly more effective. If you use melatonin, start with a low dose (0.5–1mg) taken 30–60 minutes before bed.
Why does sleep restriction therapy make you feel worse before better?
Sleep restriction limits your time in bed to match actual sleep time, which initially reduces total sleep and increases daytime fatigue. This is intentional — the temporary sleep deprivation builds homeostatic sleep pressure, which consolidates fragmented sleep and improves sleep efficiency. Within 2–3 weeks, most people begin sleeping more deeply during their restricted window, and time in bed is gradually extended.
When does insomnia require medication rather than natural treatments?
Medication may be appropriate for severe acute insomnia causing safety concerns (e.g., drowsy driving), insomnia accompanying acute psychiatric crisis, or as a short-term bridge while CBT-I takes effect. However, current guidelines recommend CBT-I as the first-line treatment for chronic insomnia. Sleeping pills should generally be used short-term (2–4 weeks) due to risks of tolerance, dependence, and side effects. Always discuss medication decisions with your healthcare provider.